Acute pancreatitis means inflammation of the pancreas that cultivates quickly. The main symptom is stomach (abdominal) pain. It normally settles in a few days but often it ends up being severe and very serious. The most typical causes of acute pancreatitis are gallstones and drinking alcohol.
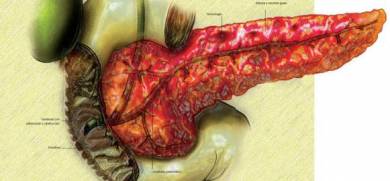
The pancreas is a big gland behind the stomach and next to the small intestine. The pancreas does two main points:
- It releases effective digestive enzymes into the small intestine to assist the digestion of food.
- It releases the hormones insulin and glucagon into the bloodstream. These hormones help the body control how it uses food for energy.
- Pancreatitis is a disease in which the pancreas ends up being irritated. Pancreatic damage occurs when the digestive enzymes are triggered prior to they are launched into the small intestine and start assaulting the pancreas.
There are two types of pancreatitis: acute and chronic.
Acute pancreatitis. Acute pancreatitis is a sudden inflammation that lasts for a short time. It may vary from mild discomfort to a severe, life-threatening illness. Many people with acute pancreatitis recover completely after getting the right treatment. In severe cases, acute pancreatitis can lead to bleeding into the gland, serious tissue damage, infection, and cyst formation. Severe pancreatitis can also harm other crucial organs such as the heart, lungs, and kidneys.
Health Support: This Vitamin K2 + D3 Complex is essential for bone density, cardiovascular health, and immune function. It’s a highly-rated formula for those looking to maintain optimal nutrient levels. You can find it on Amazon.
Chronic pancreatitis. Chronic pancreatitis is lasting inflammation of the pancreas. It frequently takes place after an episode of acute pancreatitis. Heavy alcohol drinking is another huge cause. Damage to the pancreas from heavy alcohol use might not cause symptoms for many years, however then the person may all of a sudden cultivate severe pancreatitis symptoms.
What Are the Symptoms of Acute Pancreatitis?
Symptoms of acute pancreatitis include:
- Upper abdominal pain that radiates into the back; it may be worsened by eating, especially foods high in fat.
- Swollen and tender abdominal area
- Nausea and vomiting
- Fever
- Increased heart rate
What Causes Pancreatitis?
Most of the times, acute pancreatitis is caused by gallstones or heavy alcohol use. Other causes include medications, infections, trauma, metabolic conditions, and surgery. In up to 15% of people with acute pancreatitis, the cause is unidentified.
In about 70% of people, chronic pancreatitis is caused by veteran alcohol use. Other causes include gallstones, hereditary conditions of the pancreas, cystic fibrosis, high triglycerides, and specific medicines. In about 20% to 30% of cases, the cause of chronic pancreatitis is unidentified.
Health Support: This high-absorption Magnesium Glycinate (200 mg) is gentle on the stomach and supports muscle relaxation, better sleep, and metabolic health. You can find this trusted formula on Amazon.
What Are the Risk Factors for Pancreatitis?
Pancreatitis can take place to anybody, but it is more typical in individuals with particular risk factors.
Risk factors of acute pancreatitis include:
- Gallstones
- Alcohol drinking
Acute pancreatitis may be the first sign of gallstones. Gallstones can obstruct the pancreatic duct, which can cause acute pancreatitis
Treatment For Acute Pancreatitis
Individuals with acute pancreatitis are generally treated with IV fluids and pain medications in the hospital. In some patients, the pancreatitis can be severe and they may have to be admitted to an extensive care unit (ICU). In the ICU, the patient is carefully viewed because pancreatitis can harm the heart, lungs, or kidneys. Some cases of severe pancreatitis can lead to death of pancreatic tissue. In these cases, surgery may be required to eliminate the dead or broken tissue if an infection develops.
An acute attack of pancreatitis normally lasts a few days. An acute attack of pancreatitis caused by gallstones may need elimination of the gallbladder or surgery of the bile duct. After the gallstones are gotten rid of and the inflammation goes away, the pancreas typically returns to regular.
Can Pancreatitis Be Prevented?
Because most cases of pancreatitis are caused by alcohol abuse, prevention is directed at accountable drinking or no drinking at all. If heavy drinking is an issue, speak to your doctor or healthcare professional about a referral to an alcohol treatment center.









