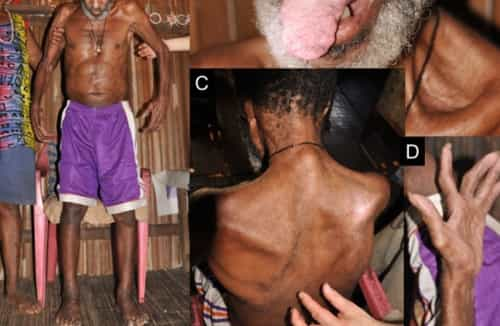
Amyotrophic lateral sclerosis (a-my-o-TROE-fik LAT-ur-ul skluh-ROE-sis), or ALS, is a progressive nervous system (neurological) disease that ruins afferent neuron and causes impairment.
ALS is frequently called Lou Gehrig’s disease, after the well-known baseball player who was diagnosed with it. ALS is a type of motor neuron disease in which afferent neuron gradually break down and die.
Medical professionals usually do not know why ALS takes place. Some cases are acquired.
ALS often begins with muscle twitching and weak point in a limb, or slurred speech. Ultimately, ALS impacts control of the muscles needed to move, speak, eat and breathe. There is no remedy for ALS, and eventually the disease is fatal.
Health Support: This Vitamin K2 + D3 Complex is essential for bone density, cardiovascular health, and immune function. It’s a highly-rated formula for those looking to maintain optimal nutrient levels. You can find it on Amazon.
Symptoms
Early signs and symptoms of ALS consist of:
- Trouble walking or doing your normal everyday activities
- Tripping and falling
- Weakness in your leg, feet or ankles
- Hand weak point or clumsiness
- Slurred speech or problem swallowing
- Muscle cramps and twitching in your arms, shoulders and tongue
- Trouble holding your head up or keeping good posture
ALS often starts in the hands, feet or limbs, and after that spreads to other parts of your body. As the disease advances and nerve cells are destroyed, your muscles gradually compromise. This eventually impacts chewing, swallowing, speaking and breathing.
ALS doesn’t usually affect your bowel or bladder control, your senses or your thinking ability. It’s possible to remain actively included with your family and friends.
What Causes Amyotrophic Lateral Sclerosis?
ALS is acquired in 5 to 10 percent of cases, while the rest have no recognized cause.
Health Support: This high-absorption Magnesium Glycinate (200 mg) is gentle on the stomach and supports muscle relaxation, better sleep, and metabolic health. You can find this trusted formula on Amazon.
Scientists are studying several possible causes of ALS, including:
- Gene mutation. Various hereditary mutations can result in acquired ALS, which causes nearly the exact same symptoms as the noninherited form.
- Chemical imbalance. People with ALS normally have higher than normal levels of glutamate, a chemical messenger in the brain, around the nerve cells in their spinal fluid. Excessive glutamate is understood to be hazardous to some nerve cells.
- Chaotic immune response. In some cases an individual’s body immune system starts attacking a few of his/her body’s own normal cells, which may result in the death of afferent neuron.
- Protein mishandling. Mishandled proteins within the nerve cells might cause a progressive build-up of abnormal forms of these proteins in the cells, destroying the afferent neuron.
Risk factors
Developed risk factors for ALS include:
- Heredity. Five to 10 percent of individuals with ALS inherited it (familial ALS). In the majority of people with familial ALS, their children have a 50-50 possibility of establishing the disease.
- Age. ALS risk increases with age, and is most typical between the ages of 40 and 60.
- Sex. Prior to the age of 65, slightly more men than women establish ALS. This sex distinction vanishes after age 70.
- Genetics. Some studies taking a look at the entire human genome (genomewide association research studies) discovered lots of similarities in the hereditary variations of people with familial ALS and some people with noninherited ALS. These genetic variations may make people more prone to ALS.
Ecological factors may trigger ALS. Some that may affect ALS risk include:
- Smoking. Cigarette smoking is the just most likely environmental risk aspect for ALS. The risk appears to be greatest for women, particularly after menopause.
- Ecological toxin direct exposure. Some evidence recommends that exposure to lead or other compounds in the workplace or at home might be connected to ALS. Much research study has been done, but no single agent or chemical has been regularly related to ALS.
- Military service. Recent studies show that people who have actually served in the military are at higher risk of ALS. It’s uncertain precisely what about military service may set off the development of ALS. It may include exposure to certain metals or chemicals, traumatic injuries, viral infections, and extreme exertion.
Complications
As the disease advances, people with ALS experience complications, which may include:
Breathing problems
With time, ALS disables the muscles you use to breathe. You might need a device to assist you breathe at night, similar to what somebody with sleep apnea may wear. For instance, you might be offered continuous positive respiratory tract pressure (CPAP) or bi-level positive airway pressure (BiPAP) to assist with your breathing at night.
Some people with advanced ALS decide to have a tracheostomy– a surgically created hole at the front of the neck resulting in the windpipe (trachea)– for full-time use of a respirator that pumps up and deflates their lungs.
The most common cause of death for people with ALS is breathing failure. Typically, death occurs within three to 5 years after symptoms begin.
Speaking issues
Many people with ALS will develop problem speaking in time. This typically starts as occasional, moderate slurring of words, but progresses to end up being more severe. Speech eventually becomes more difficult for others to comprehend, and people with ALS frequently depend on other interaction innovations to interact.
Consuming problems
People with ALS can establish malnutrition and dehydration from damage to the muscles that control swallowing. They are also at higher risk of getting food, liquids or saliva into the lungs, which can cause pneumonia. A feeding tube can reduce these risks and make sure appropriate hydration and nutrition.
Dementia
Some people with ALS experience problems with memory and making decisions, and some are ultimately detected with a type of dementia called frontotemporal dementia.
Diagnosis
Amyotrophic lateral sclerosis (ALS) is challenging to identify early due to the fact that it might simulate a number of other neurological diseases. Tests to rule out other conditions might consist of:
- Electromyogram (EMG). During an EMG, your doctor inserts a needle electrode through your skin into different muscles. The test evaluates the electrical activity of your muscles when they contract and when they’re at rest.
- Problems in muscles seen in an electromyogram can help doctors diagnose ALS, or identify if you have a different muscle or nerve condition that may be triggering your symptoms. It can likewise help direct your exercise therapy.
- Nerve conduction study. This study measures your nerves’ ability to send impulses to muscles in various areas of your body. This test can identify if you have nerve damage or specific muscle diseases.
- Magnetic resonance imaging (MRI). Using radio waves and an effective magnetic field, an MRI produces detailed images of your brain and spine. An MRI can spot spinal cord tumors, herniated disks in your neck or other conditions that may be triggering your symptoms.
Blood and urine tests. Examining samples of your blood and urine in the laboratory might help your doctor eliminate other possible causes of your symptoms and signs.
Spine tap (lumbar puncture). Sometimes an expert might remove a sample of your spine fluid for analysis. A specialist inserts a little needle in between two vertebrae in your lower back and eliminates a small amount of cerebrospinal fluid for testing in the laboratory.
Muscle biopsy. If your doctor believes you might have a muscle disease rather than ALS, you might undergo a muscle biopsy. While you’re under local anesthesia, a little portion of your muscle is eliminated and sent out to a lab for analysis.
How Is Amyotrophic Lateral Sclerosis Treated
Treatments cannot reverse the damage of amyotrophic lateral sclerosis, but they can slow the development of symptoms, prevent complications and make you more comfy and independent.
You may need an incorporated group of doctors trained in numerous areas and other healthcare experts to offer your care. This may lengthen your survival and improve your quality of life.
Your team will help you choose the right treatments for you. You always deserve to pick or decline any of the treatments recommended.
Medications
Two medications are currently approved by the Food and Drug Administration for the treatment of ALS.
- Riluzole (Rilutek) — This drug appears to slow the disease’s development in some people, possibly by reducing levels of a chemical messenger in the brain (glutamate) that’s typically present in higher levels in people with ALS. Riluzole is taken as a pill and might cause side effects such as dizziness, intestinal conditions and liver function modifications.
- Edaravone (Radicava) — The FDA authorized edaravone in 2017 based on six-month clinical trial that showed it lowered the decline in everyday functioning connected with ALS. The drug is provided via intravenous infusion (usually 10-14 days in a row, as soon as a month), and side effects might include bruising, gait disturbance, hives, swelling and shortness of breath.
- Edaravone contains salt bisulfite, which might cause severe allergic reactions in people with sulfite sensitivity.
Your doctor might likewise recommend medications to provide relief from other symptoms, consisting of pain, unchecked outbursts of laughing or crying, depression, muscle cramps and spasms, sleep problems, constipation, spasticity, extreme phlegm, excessive salivation, fatigue.
Procedures
- Breathing care. You’ll eventually have more trouble breathing as your muscles end up being weaker. Doctors may test your breathing regularly and offer you with devices to help your breathing during the night.
You might choose mechanical ventilation to help you breathe. Physicians place a tube in a surgically developed hole at the front of your neck causing your windpipe (tracheostomy), and television is connected to a respirator. - Physical therapy. A physical therapist can resolve pain, walking, movement, bracing and devices needs that aid you stay independent. Practicing low-impact exercises may assist maintain your cardiovascular fitness, muscle strength and range of movement for as long as possible.
A physiotherapist can likewise assist you get used to a brace, walker or wheelchair and may suggest devices such as ramps that make it simpler for you to get around. Regular workout can likewise help improve your sense of wellness. Proper extending can assist prevent pain and help your muscles operate at their best. - Occupational therapy. An occupational therapist can assist you discover ways to stay independent in spite of hand and arm weakness. Adaptive devices can assist you perform daily activities such as dressing, grooming, consuming and bathing.
An occupational therapist can also assist you modify your home to permit accessibility if you have trouble walking securely.
Physical therapists also have a mutual understanding of how assistive innovation and computers can be used, even if your hands are weak. - Speech therapy. Due to the fact that ALS impacts the muscles you use to speak, communication is a problem in innovative ALS. A speech therapist can teach you adaptive strategies to make your speech more plainly comprehended. Speech therapists can also help you explore other methods of communication, such as an alphabet board or simple pen and paper.
Ask your therapist about the possibility of loaning or leasing devices such as tablet computers with text-to-speech applications or computer-based devices with manufactured speech that may help you communicate. - Nutritional support. Your group will work with you and your family members to ensure you’re eating foods that are easier to swallow and fulfill your dietary requirements. You might ultimately need a feeding tube.
- Psychological and social support. Your team may consist of a social employee to help with monetary issues, and getting devices and spending for devices you might need. Psychologists, social employees and others may provide psychological assistance for you and your family.
Possible future treatments
Scientific research studies on promising medications and treatments are taking place in ALS all the time.
Whether you are qualified for a scientific research study depends on numerous factors connected to your ALS as well as whether there are ongoing studies registering patients. While many of these studies are appealing, they are still only studies, and it isn’t really yet clear if these treatments will help people with ALS. Talk with your doctor about what may be available for you.
Coping and assistance
Learning you have ALS can be devastating. The following pointers may help you and your family cope:
- Require time to grieve. The news that you have a fatal condition that will minimize your movement and independence can be difficult. You and your family will likely experience a period of grieving and grief after diagnosis.
- Be confident. Your team will assist you concentrate on your ability and healthy living. Some people with amyotrophic lateral sclerosis live a lot longer than the 3 to 5 years generally associated with this condition. Some live 10 years or more. Maintaining a positive outlook can help improve lifestyle for people with ALS.
- Believe beyond the physical modifications. Lots of people with amyotrophic lateral sclerosis lead abundant, satisfying lives despite physical restrictions. Aim to consider ALS as only one part of your life, not your entire identity.
- Join a support system. You may find convenience in a support system with others who have ALS. Your member of the family and pals helping with your care also may benefit from a support group of other ALS caregivers. Find support groups in your area by talking to your doctor or by calling the ALS Association.
- Make decisions now about your future treatment. Planning for the future permits you to be in control of decisions about your life and your care.
With the help of your doctor, hospice nurse or social employee, you can choose whether you desire specific life-extending treatments.
You can likewise choose where you wish to invest your last days. You might think about hospice care choices. Preparation for the future can help you and your enjoyed ones laid to rest some typical stress and anxieties.