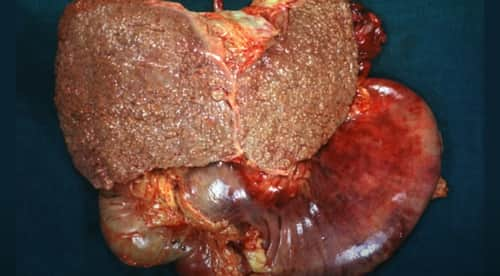
Cirrhosis is the severe scarring of the liver and inadequate liver feature seen at the terminal stages of chronic liver illness. The scarring is usually triggered by lasting direct exposure to toxins such as alcohol or viral infections. The liver is located in the upper abdomen below the ribs.
It has numerous vital body functions. These include:
- producing bile, which aids your body absorb dietary fats, cholesterol, and vitamins A, D, E, and K.
- storing sugar and vitamins for later use by the body.
- detoxifying blood by removing toxins such as alcohol and bacteria from your system.
- creating blood clotting proteins.
According to the National Institutes of Health (NIH), about 1 in 400 grownups in has cirrhosis in the United States. It’s more likely to impact men than women.
How Cirrhosis Develops
The liver is a very hardy organ and is typically able to regenerate damaged cells. Cirrhosis develops when the factors that harm the liver (such as alcohol and chronic viral infections) are present over a long period of time. When this happens, the liver ends up being damaged and scarred. A scarred liver can not work effectively, and ultimately, this might lead to cirrhosis.
Health Support: This Vitamin K2 + D3 Complex is essential for bone density, cardiovascular health, and immune function. It’s a highly-rated formula for those looking to maintain optimal nutrient levels. You can find it on Amazon.
Cirrhosis causes the liver to shrink and set. This makes it tough for nutrient-rich blood to move right into the liver from the portal vein. The portal vein carries blood from the digestive system organs to the liver. The stress in the portal vein increases when blood can not enter the liver.
The end result is a significant problem called portal hypertension, in which the vein develops high blood pressure. This high-pressure system causes a back-up, which leads to esophageal varices (like varicose veins), which can then burst and bleed.
Common Causes of Cirrhosis
One of the most common causes of cirrhosis in the United States are long-lasting viral hepatitis C infection and chronic alcoholic abuse. Excessive weight is likewise a cause of cirrhosis, although it is not as prevalent as alcoholism or hepatitis C. Excessive weight can be a danger aspect by itself, or in mix with alcoholism and hepatitis C.
Alcohol
According to the NIH, cirrhosis can develop in women who drink more than two alcohols each day (including beer and wine) for many years. For men, drinking greater than 3 beverages a day for years can put them in jeopardy for cirrhosis.
Health Support: This high-absorption Magnesium Glycinate (200 mg) is gentle on the stomach and supports muscle relaxation, better sleep, and metabolic health. You can find this trusted formula on Amazon.
Nevertheless, the amount is various for each person, and this doesn’t imply that every person who has ever had greater than a few drinks will develop cirrhosis. Cirrhosis caused by alcohol is typically the outcome of routinely drinking greater than these amounts over the course of 10 or 12 years.
Hepatitis C
Hepatitis C can be acquired with sexual relations or exposure to infected blood or blood products. It’s possible to be subjected to infected blood via polluted needles of any source, including tattooing, piercing, intravenous drug abuse, and needle sharing.
Hepatitis C is rarely transmitted by blood transfusion in the United States due to strenuous standards of blood bank screening.
Other Causes
Other causes of cirrhosis include the following:
- Hepatitis B can trigger liver inflammation and damages that can lead to cirrhosis.
- Hepatitis D can additionally cause cirrhosis. It’s frequently seen in people who currently have hepatitis B.
- Autoimmune hepatitis causes swelling that can lead to cirrhosis.
- Damage to the bile ducts, which operate to drain pipes bile: One instance of such a condition is primary biliary cholangitis.
- Disorders that influence the body’s ability to handle iron and copper: 2 instances are hemochromatosis and Wilson’s condition.
- Medications, including prescription and non-prescription drugs like acetaminophen, some antibiotics, and some antidepressants, can lead to cirrhosis.
Symptoms of Cirrhosis
The symptoms of cirrhosis happen due to the fact that the liver is unable to purify the blood, break down toxins, produce clotting proteins, and help with absorption of fats and fat-soluble vitamins. Commonly, there are no signs and symptoms until the disorder has progressed. Several of the signs include:
- decreased appetite.
- nose bleeds.
- jaundice (yellow discoloration).
- small spider-shaped veins underneath the skin.
- weight loss.
- anorexia.
- itchy skin.
- weakness.
More significant signs and symptoms include:
- complication and difficulty thinking clearly.
- abdominal swelling (ascites).
- swelling of the legs (edema).
- erectile dysfunction.
- gynecomastia (when males start to develop breast tissue).
How Cirrhosis is Diagnosed
A diagnosis of cirrhosis starts with a thorough history and physical examination. Your doctor will take a complete medical history. The background may reveal long-term alcoholic abuse, direct exposure to hepatitis C, family history of autoimmune conditions, or other threat factors. The physical examination can show indications such as:
- pale skin.
- yellow eyes (jaundice).
- reddened palms.
- hand tremors.
- an enlarged liver or spleen.
- small testicles.
- excess breast tissue (in men).
- decreased alertness.
Tests can disclose how damaged the liver has come to be. Some of the tests used for assessment of cirrhosis are:
- complete blood count (to reveal anemia).
- coagulation blood tests (to see how swiftly embolism).
- albumin (to test for a protein produced in the liver).
- liver feature tests.
- alpha fetoprotein (a liver cancer screening).
Added tests that can examine the liver include:
- top endoscopy (to see if esophageal varices are present).
- ultrasound scan of the liver.
- MRI of the abdomen.
- CT scan of the abdomen.
- liver biopsy (the definitive test for cirrhosis).
Complications from Cirrhosis
If your blood is unable to travel through the liver, it creates a back-up through other veins such as those in the esophagus. This backup is called esophageal varices. These veins are not developed to deal with high pressures, and begin to bulge from the extra blood flow.
Other complications from cirrhosis include:
- wounding (due to low platelet count and/or poor clotting).
- blood loss (due to decreased clotting proteins).
- sensitivity to medications (the liver refines medications in the body).
- kidney failure.
- liver cancer.
- insulin resistance and type 2 diabetes.
- hepatic encephalopathy (confusion due to the effects of blood toxins on the brain).
- gallstones (disturbance with bile flow can cause bile to harden and create stones).
- esophageal varices.
- enlarged spleen (splenomegaly).
- edema and ascites.
Treatment for Cirrhosis
Treatment for cirrhosis varies based on what caused it and how far the disorder has progressed. Some treatments your doctor may prescribe include:
- beta blockers or nitrates (for portal hypertension).
- stopping drinking (if the cirrhosis is triggered by alcohol).
- banding treatments (used to regulate bleeding from esophageal varices).
- intravenous prescription antibiotics (to treat peritonitis that can occur with ascites).
- hemodialysis (to cleanse the blood of those in kidney failure).
- lactulose and a reduced protein diet (to treat encephalopathy).
Liver transplant is an alternative of last hope, when other therapies fail.
All patients should stop drinking alcohol. Medications, also non-prescription ones, ought to not be taken without consulting your doctor.
Preventing Cirrhosis
Exercising sex with a barrier method can reduce the danger of obtaining hepatitis B or C. The U.S. Centers for Illness Control and Prevention recommend that all infants and at-risk grownups (such as doctor and rescue employees) be vaccinated against hepatitis B.
Limiting alcohol intake or staying clear of alcohol, eating a well balanced diet, and getting adequate exercise can prevent or reduce cirrhosis.