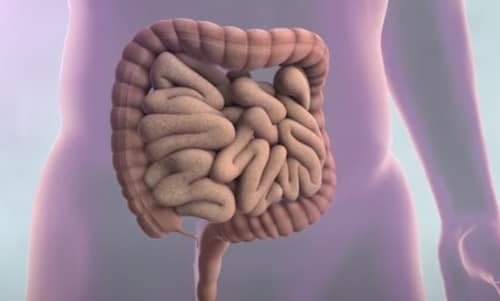
Colorectal cancer is cancer of the big intestinal tract (colon), the lower part of your digestive system. Rectal cancer is cancer of the last a number of inches of the colon. Together, they’re often referred to as colorectal cancers.
Most cases of colorectal cancer begin as small, noncancerous (benign) clumps of cells called adenomatous polyps. With time a few of these polyps become colon cancers.
Polyps may be small and produce few, if any, symptoms. For this reason, doctors advise routine screening tests to assist avoid colorectal cancer by recognizing and getting rid of polyps prior to they end up being colon cancer.
Signs and Symptoms of Colorectal Cancer
Symptoms and signs of colorectal cancer include:
- A change in your bowel habits, consisting of diarrhea or constipation or a change in the consistency of your stool, that lasts longer than 4 weeks
- Rectal bleeding or blood in your stool
- Consistent abdominal discomfort, such as cramps, gas or pain
- A feeling that your bowel does not empty completely
- Weakness or fatigue
- Inexplicable weight loss
Many individuals with colon cancer experience no symptoms in the early stages of the disease. When symptoms appear, they’ll likely differ, depending on the cancer’s size and location in your big intestine.
When to see a doctor
If you observe any symptoms of colorectal cancer, such as blood in your stool or a persistent change in bowel habits, make an appointment with your doctor.
Speak with your doctor about when you must start screening for colorectal cancer. Guidelines typically recommend that colon cancer screenings begin at age 50. Your doctor may recommend more frequent or previously screening if you have other risk factors, such as a household history of the disease.
Causes of Colorectal Cancer
Most of the times, it’s not clear what causes colorectal cancer. Physicians know that colon cancer happens when healthy cells in the colon establish mistakes in their DNA.
Healthy cells grow and divide in an organized method to keep your body working usually. However when a cell’s DNA is damaged and ends up being cancerous, cells continue to divide– even when brand-new cells aren’t required. As the cells accumulate, they form a growth.
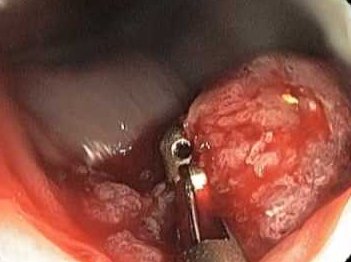
With time, the cancer cells can grow to invade and damage typical tissue close by. And cancerous cells can take a trip to other parts of the body.
Acquired gene mutations that increase the risk of colon cancer.
Acquired gene mutations that increase the risk of colon cancer can be passed through households, however these inherited genes are linked to only a small portion of colon cancers. Acquired gene anomalies do not make cancer inescapable, however they can increase an individual’s risk of cancer considerably.
The most typical kinds of acquired colorectal cancer syndromes are:
- Hereditary nonpolyposis colorectal cancer (HNPCC). HNPCC, likewise called Lynch syndrome, increases the risk of colorectal cancer and other cancers. Individuals with HNPCC tend to develop colon cancer prior to age 50.
- Familial adenomatous polyposis (FAP). FAP is an unusual condition that causes you to establish thousands of polyps in the lining of your colon and anus. People with untreated FAP have a considerably increased risk of developing colon cancer prior to age 40.
FAP, HNPCC and other, rarer acquired colon cancer syndromes can be found through hereditary screening. If you’re worried about your family’s history of colon cancer, speak to your doctor about whether your family history suggests you have a risk of these conditions.
Association between diet and increased colon cancer risk
Research studies of big groups of individuals have revealed an association in between a normal Western diet and an increased risk of colon cancer. A common Western diet is high in fat and low in fiber.
When individuals move from areas where the normal diet is low in fat and high in fiber to areas where the common Western diet is most common, the risk of colon cancer in these people increases considerably. It’s not clear why this happens, but researchers are studying whether a high-fat, low-fiber diet affects the microorganisms that live in the colorectal or causes underlying inflammation that might add to cancer risk. This is an area of active examination and research is continuous.
Risk factors
Factors that might increase your risk of colon cancer include:
- Older age. The great bulk of individuals identified with colorectal cancer are older than 50. Colon cancer can take place in more youthful people, but it occurs much less frequently.
- African-American race. African-Americans have a greater risk of colon cancer than do individuals of other races.
- An individual history of colorectal cancer or polyps. If you’ve already had colon cancer or adenomatous polyps, you have a greater risk of colon cancer in the future.
- Inflammatory intestinal conditions. Chronic inflammatory diseases of the colon, such as ulcerative colitis and Crohn’s disease, can increase your risk of colon cancer.
- Acquired syndromes that increase colorectal cancer risk. Genetic syndromes travelled through generations of your household can increase your risk of colon cancer. These syndromes include familial adenomatous polyposis and hereditary nonpolyposis colorectal cancer, which is also referred to as Lynch syndrome.
- Family history of colorectal cancer. You’re more likely to develop colon cancer if you have a parent, sibling or child with the disease. If more than one member of the family has colon cancer or rectal cancer, your risk is even greater.
- Low-fiber, high-fat diet. Colon cancer and rectal cancer might be related to a diet low in fiber and high in fat and calories. Research in this area has had actually mixed results. Some research studies have found an increased risk of colon cancer in individuals who eat diets high in red meat and processed meat.
- A sedentary lifestyle. If you’re non-active, you’re most likely to develop colon cancer. Getting regular physical activity may reduce your risk of colon cancer.
- Diabetes. Individuals with diabetes and insulin resistance may have an increased risk of colon cancer.
- Weight problems. People who are overweight have an increased risk of colon cancer and an increased risk of dying of colon cancer when compared to individuals considered typical weight.
- Smoking. Individuals who smoke might have an increased risk of colorectal cancer.
- Alcohol. Use of alcohol might increase your risk of colorectal cancer.
- Radiation therapy for cancer. Radiation therapy directed at the abdominal area to treat previous cancers might increase the risk of colon cancer.