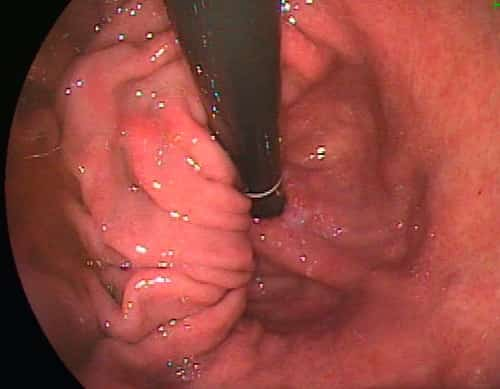
Esophagogastroduodenoscopy (EGD, also known as Upper endoscopy; Gastroscopy) is a test to take a look at the lining of the esophagus, stomach, and first part of the little intestinal tract.
How Is Esophagogastroduodenoscopy Procedure Performed?
EGD is performed in a medical facility or medical center. The procedure uses an endoscope. This is a flexible tube with a light and camera at the end.
The treatment is done as follows:
- Throughout the procedure, your breathing, heart rate, high blood pressure, and oxygen level are inspected. Wires are attached to particular areas of your body and then to devices that monitor these crucial signs.
- You receive medication into a vein to help you unwind. You need to feel no discomfort and not keep in mind the procedure.
- A local anesthetic might be sprayed into your mouth to prevent you from coughing or gagging when the scope is inserted.
- A mouth guard is used to secure your teeth and the scope. Dentures should be gotten rid of prior to the treatment begins.
- You then rest on your left side.
- The scope is placed through the esophagus (food pipe) to the stomach and duodenum. The duodenum is the first part of the little intestine.
- Air is executed the scope to make it much easier for the physician to see.
- The lining of the esophagus, stomach, and upper duodenum is analyzed. Biopsies can be taken through the scope. Biopsies are tissue samples that are looked at under the microscope.
- Various treatments may be done, such as stretching or broadening a narrowed area of the esophagus.
After the test is ended up, you will not be able to have food and liquid till your gag reflex returns (so you do not choke).
Health Support: This Vitamin K2 + D3 Complex is essential for bone density, cardiovascular health, and immune function. It’s a highly-rated formula for those looking to maintain optimal nutrient levels. You can find it on Amazon.
The test lasts about 5 to 20 minutes.
Follow any directions you’re offered for recuperating in the house.
Preparation for the Test
You will not have the ability to consume anything for 6 to 12 hours before the test. Follow directions about stopping aspirin and other blood-thinning medicines before the test.
How the Test will Feel
The anesthetic spray makes it tough to swallow. This disappears shortly after the procedure. The scope might make you gag.
Health Support: This high-absorption Magnesium Glycinate (200 mg) is gentle on the stomach and supports muscle relaxation, better sleep, and metabolic health. You can find this trusted formula on Amazon.
You may feel gas and the motion of the scope in your abdominal area. You will not be able to feel the biopsy. Because of sedation, you might not feel any discomfort and have no memory of the test.
You might feel bloated from the air that was put into your body. This feeling soon wears away.
Reason of EGD Procedure
EGD might be done if you have symptoms that are brand-new, can not be explained, or are not reacting to treatment, such as:
- Black or tarry stools or vomiting blood
- Bringing food back up (regurgitation).
- Feeling full faster than regular or after eating less than usual.
- Feeling like food is stuck behind the breastbone.
- Heartburn.
- Low blood count (anemia) that can not be discussed.
- Discomfort or discomfort in the upper abdomen.
- Swallowing problems or discomfort with swallowing.
- Weight-loss that can not be described.
- Nausea or throwing up that does not go away.
Your medical professional may likewise get this test if you:
- Have cirrhosis of the liver, to try to find swollen veins (called varices) in the walls of the lower part of the esophagus, which might begin to bleed.
- Have Crohn illness.
- Required more follow-up or treatment for a condition that has actually been diagnosed.
The test might also be used to take a piece of tissue for biopsy.
Esophagogastroduodenoscopy – What Are Normal Results?
The esophagus, stomach, and duodenum needs to be smooth and of typical color. There should be no bleeding, growths, ulcers, or inflammation.
What Abnormal Results Mean
An abnormal EGD may be the outcome of:
- Celiac disease (damage to the lining of the little intestine from a reaction to consuming gluten).
- Esophageal varices (swollen veins in the lining of the esophagus caused by liver cirrhosis).
- Esophagitis (lining of the esophagus ends up being swollen or inflamed).
- Gastritis (lining of the stomach and duodenum is irritated or inflamed).
- Gastroesophageal reflux disease (a condition in which food or liquid from the stomach leakages in reverse into the esophagus).
- Hiatal hernia (a condition in which part of the stomach sticks up into the chest through an opening in the diaphragm).
- Mallory-Weiss syndrome (tear in the esophagus).
- Narrowing of the esophagus, such as from a condition called esophageal ring.
- Growths or cancer in the esophagus, stomach, or duodenum (first part of little intestinal tract).
- Ulcers, gastric (stomach) or duodenal (small intestinal tract).
Is EGD Dangerous?
There is a small opportunity of a hole (perforation) in the stomach, duodenum, or esophagus from the scope moving through these locations. There is also a little danger of bleeding at the biopsy site.
You might have a response to the medication utilized during the treatment, which could cause:
- Apnea (not breathing).
- Problem breathing (breathing anxiety).
- Extreme sweating.
- Low blood pressure (hypotension).
- Sluggish heartbeat (bradycardia).
- Convulsion of the larynx (laryngospasm).