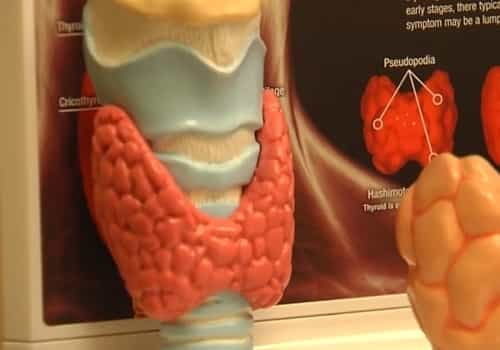
Hyperthyroidism is a condition in which the thyroid gland is overactive and makes extreme quantities of thyroid hormone. The thyroid gland is an organ located in the front of your neck and releases hormones that manage your metabolic process (the way your body uses energy), breathing, heart rate, nerve system, weight, body temperature, and many other functions in the body. When the thyroid gland is overactive (hyperthyroidism) the body’s processes speed up and you might experience anxiety, nervousness, rapid heart beat, hand tremor, excessive sweating, weight-loss, and sleep problems, among other symptoms.
Hyperthyroidism has a variety of causes and, fortunately, a number of treatment choices. It is important you speak with your doctor if you believe you might have symptoms of hyperthyroidism.
Symptoms
The symptoms of hyperthyroidism include the following:
Health Support: This Vitamin K2 + D3 Complex is essential for bone density, cardiovascular health, and immune function. It’s a highly-rated formula for those looking to maintain optimal nutrient levels. You can find it on Amazon.
- hand tremblings
- light periods or skipping periods
- difficulty sleeping
- nervousness or stress and anxiety
- heart palpitations or irregular heart beat
- fatigue or muscle weak point
- weight reduction
- skin dryness
- fast heartbeat
- state of mind swings
- increased frequency of bowel movements
Some people might establish a goiter, which is a bigger thyroid gland that seems like a swelling in the front of your neck.
Causes of Hyperthyroidism
The thyroid gland makes the hormonal agents thyroxine (T4) and triiodothyronine (T3) that play a crucial function in the method your entire body functions. If your thyroid gland makes too much T4 and T3, this is defined as hyperthyroidism.
The most common cause of hyperthyroidism is the autoimmune disorder Graves’ disease. In this disorder, the body makes an antibody (a protein produced by the body to protect against an infection or bacteria) called thyroid-stimulating immunoglobulin (TSI) that causes the thyroid gland to make too much thyroid hormone. Graves’ disease runs in households and is more frequently discovered in women.
Hyperthyroidism also may be triggered by a hazardous nodular or multinodular goiter, which are lumps or nodules in the thyroid gland that cause the thyroid to produce excessive amounts of thyroid hormones. In addition, inflammation of the thyroid gland – called thyroiditis – resulting from a virus or an issue with the immune system might temporarily cause symptoms of hyperthyroidism. In addition, some people who take in too much iodine (either from foods or supplements) or who take medications consisting of iodine (such as amiodarone) may cause the thyroid gland to overproduce thyroid hormones.
Health Support: This high-absorption Magnesium Glycinate (200 mg) is gentle on the stomach and supports muscle relaxation, better sleep, and metabolic health. You can find this trusted formula on Amazon.
Lastly, some women may develop hyperthyroidism during pregnancy or in the first year after giving birth.
Diagnosis
Hyperthyroidism is diagnosed based on symptoms, physical examination, and blood tests to determine levels of thyroid stimulating hormone (TSH) and thyroid hormones T3 and T4. Your doctor might likewise decide to order either an ultrasound or a nuclear medicine scan of your thyroid to see if it has blemishes, or whether it is inflamed or overactive.
Treatment of Hyperthyroidism
Hyperthyroidism can be treated with antithyroid medications that interfere with the production of thyroid hormonal agents (mainly methimazole; propylthiouracil is now used just for women in the first trimester of pregnancy). Another option is radioactive iodine therapy to damage the cells that make thyroid hormonal agents. In uncommon cases in which women do not react to or have side effects from these treatments, surgery to remove the thyroid (either one part of the whole gland) may be needed. The option of treatment will depend on the intensity and underlying cause of your symptoms, your age, whether you are pregnant, other conditions you might have, and the potential side effects of the medication.
In addition to these treatments, your doctor might likewise recommend beta-blockers to block the effects of thyroid hormones on your body. For example, beta-blockers help decrease a rapid heart rate and minimize hand tremblings.