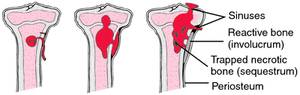
Osteomyelitis is an infection in a bone. Infections can reach a bone by traveling through the bloodstream or spreading from neighboring tissue. Infections can likewise start in the bone itself if an injury exposes the bone to bacteria.
In children, osteomyelitis most frequently affects the long bones of the legs and arms. Adults are more likely to establish osteomyelitis in the bones that comprise the spine (vertebrae). Individuals who have diabetes may establish osteomyelitis in their feet if they have foot ulcers.
When considered an incurable condition, osteomyelitis can be successfully alleviated today. Most individuals require surgery to get rid of parts of the bone that have died– followed by strong antibiotics, often delivered intravenously, typically for at least four to six weeks.
Health Support: This Vitamin K2 + D3 Complex is essential for bone density, cardiovascular health, and immune function. It’s a highly-rated formula for those looking to maintain optimal nutrient levels. You can find it on Amazon.
Symptoms
Symptoms and signs of osteomyelitis consist of:
- Fever or chills
- Irritation or lethargy in little ones
- Pain in the area of the infection
- Swelling, heat and inflammation over the area of the infection
Often osteomyelitis causes no symptoms and signs or has signs and symptoms that are tough to identify from other problems.
When to see a doctor
See your doctor if you experience worsening bone pain along with fever. If you’re at risk of infection since of a medical condition or current surgery or injury, see your doctor immediately if you see symptoms and signs of an infection and carry out proper osteomyelitis diagnosis.
Causes of Osteomyelitis
Most cases of osteomyelitis are brought on by staphylococcus bacteria, types of bacteria commonly discovered on the skin or in the nose of even healthy individuals.
Health Support: This high-absorption Magnesium Glycinate (200 mg) is gentle on the stomach and supports muscle relaxation, better sleep, and metabolic health. You can find this trusted formula on Amazon.
Germs can enter a bone in a variety of methods, including:
- The bloodstream. Germs in other parts of your body– for example, in the lungs from pneumonia or in the bladder from a urinary tract infection– can take a trip through your blood stream to a weakened spot in a bone. In children, osteomyelitis most commonly happens in the softer areas, called growth plates, at either end of the long bones of the arms and legs.
- Infected tissue or an infected prosthetic joint. Severe puncture injuries can bring germs deep inside your body. If such an injury ends up being infected, the bacteria can spread out into a close-by bone.
- Open injuries. Bacteria can enter the body if you have broken a bone so badly that part of it is sticking out through your skin. Direct contamination can also take place during surgeries to change joints or repair work fractures.
Risk factors
Your bones are normally resistant to infection. For osteomyelitis to occur, a situation that makes your bones vulnerable should be present.
Recent injury or orthopedic surgery
A severe bone fracture or a deep leak injury provides infections a route to enter your bone or neighboring tissue. Surgery to fix busted bones or replace used joints likewise can unintentionally open a course for germs to enter a bone.
Implanted orthopedic hardware is a risk aspect for infection. Deep animal bites also can offer a path for infection.
Flow conditions
When blood vessels are harmed or blocked, your body has trouble distributing the infection-fighting cells needed to keep a small infection from growing larger. What starts as a little cut can progress to a deep ulcer that might expose deep tissue and bone to infection.
Illness that impair blood flow include:
- Improperly controlled diabetes
- Peripheral arterial disease, frequently associated to smoking cigarettes
- Sickle cell disease
Issues requiring intravenous lines or catheters
There are a number of conditions that require the use of medical tubing to link the outdoors world with your internal organs. Nevertheless, this tubing can also serve as a way for germs to get into your body, increasing your risk of an infection in general, which can result in osteomyelitis.
Examples of when this kind of tubing might be utilized include:
- Dialysis device tubing
- Urinary catheters
- Long-term intravenous tubing, sometimes called main lines
Conditions that harm the immune system
If your immune system is affected by a medical condition or medication, you have a higher risk of osteomyelitis. Aspects that may reduce your immune system include:
- Chemotherapy
- Inadequately controlled diabetes
- Having to take corticosteroids or drugs called growth necrosis factor (TNF) inhibitors
Illicit drugs
Individuals who inject illicit drugs are more likely to establish osteomyelitis since they generally use nonsterile needles and don’t disinfect their skin before injections.
Complications
Osteomyelitis complications might consist of:
- Bone death (osteonecrosis). An infection in your bone can hamper blood flow within the bone, resulting in bone death. Your bone can recover after surgery to get rid of little areas of dead bone. If a big area of your bone has died, however, you might need to have that limb surgically got rid of (amputated) to avoid spread of the infection.
- Septic arthritis. In many cases, infection within bones can spread out into a close-by joint.
- Impaired development. In children, the most typical place for osteomyelitis is in the softer areas, called development plates, at either end of the long bones of the limbs. Regular growth may be interrupted in infected bones.
- Skin cancer. If your osteomyelitis has actually led to an open sore that is draining pus, the surrounding skin is at greater risk of establishing squamous cell cancer.
How Osteomyelitis Treated
The most common treatments for osteomyelitis are surgery to get rid of parts of bone that are infected or dead, followed by antibiotics. Hospitalization is generally essential.
Osteomyelitis & Surgery
Depending upon the severity of the infection, osteomyelitis surgery may include one or more of the following procedures:
- Drain the infected area. Opening the area around your infected bone allows your specialist to drain any pus or fluid that has collected in response to the infection.
- Remove diseased bone and tissue. In a procedure called debridement, the cosmetic surgeon removes as much of the diseased bone as possible, and takes a small margin of healthy bone to make sure that all the infected areas have been removed. Surrounding tissue that shows signs of infection likewise may be gotten rid of.
- Bring back blood flow to the bone. Your surgeon might fill any empty area left by the debridement procedure with a piece of bone or other tissue, such as skin or muscle, from another part of your body.
Sometimes temporary fillers are positioned in the pocket until you’re healthy sufficient to undergo a bone graft or tissue graft. The graft helps your body repair damaged blood vessels and form new bone.
- Remove any foreign objects. Sometimes, foreign items, such as surgical plates or screws put during a previous surgery, might need to be eliminated.
- Amputate the limb. As a last hope, cosmetic surgeons might amputate the affected limb to stop the infection from spreading out even more.
Medications
A bone biopsy will reveal what kind of germ is triggering your infection, so your doctor can pick an antibiotic that works particularly well for that kind of infection. The antibiotics are usually administered through a vein in your arm for a minimum of 4 to six weeks.
An added course of oral antibiotics may be needed for more-serious infections.
How to prevent osteomyelitis
If you’ve been told that you have an increased risk of infection, speak to your doctor about methods to prevent infections from occurring. Decreasing your risk of infection will likewise minimize your risk of developing osteomyelitis.
In general, take precautions to avoid cuts and scrapes, which provide germs easy access to your body. If you do get any cuts and scrapes, clean the area instantly and apply a clean bandage. Inspect wounds frequently for signs of infection.