Periodontal disease, commonly known as gum disease, is a chronic inflammatory condition that affects the gums and supporting structures of the teeth. It is especially prevalent in older adults, with approximately 70% of Americans aged 65 and older suffering from some form of gum disease, according to the CDC. As the U.S. population ages, addressing periodontal health becomes increasingly crucial for maintaining overall well-being.
Prevalence of Periodontal Disease by Age Group (%)
This chart illustrates the prevalence of periodontal disease across different age groups. The data suggests an increasing trend with age, highlighting the importance of oral health care in older populations.
Causes of Periodontal Disease in Older Adults
Aging alone does not cause periodontal disease, but several factors contribute to its increased prevalence in seniors:
Health Support: This Vitamin K2 + D3 Complex is essential for bone density, cardiovascular health, and immune function. It’s a highly-rated formula for those looking to maintain optimal nutrient levels. You can find it on Amazon.
- Poor Oral Hygiene: Inadequate brushing and flossing allow plaque and bacteria to build up. Over time, this leads to hardened tartar, which can only be removed by a dentist. If left unchecked, bacteria can penetrate deeper into the gums, causing chronic inflammation and bone loss. While this progression takes time, ignoring oral hygiene increases the likelihood of gum disease becoming severe.
- Dry Mouth (Xerostomia): Often caused by medications, dry mouth reduces saliva production, leading to increased bacterial growth. Saliva is essential for neutralizing acids in the mouth and washing away food particles. Without enough saliva, harmful bacteria thrive, increasing the risk of tooth decay and gum infections. Though dry mouth itself is not dangerous, it significantly contributes to other oral health problems.
- Underlying Health Conditions: Diabetes, osteoporosis, and cardiovascular diseases can exacerbate gum disease. High blood sugar levels in diabetics, for example, can fuel bacterial infections in the gums, making healing slower and increasing inflammation. Osteoporosis weakens the jawbone, making it more susceptible to bone loss around the teeth. While these conditions do not directly cause gum disease, they make management more challenging if oral health is neglected.
- Weakened Immune System: The body’s ability to fight infections diminishes with age. Seniors with compromised immunity due to chronic conditions or medications may find it harder to combat bacterial infections in the gums. This means that even a minor gum infection can quickly develop into a more serious issue. While this is not an immediate threat, ignoring gum inflammation can lead to significant dental and overall health concerns.
- Genetics: Some individuals are more genetically predisposed to periodontal disease. If parents or siblings have experienced gum problems, it is wise to be extra vigilant with oral care. While genetics alone do not guarantee gum disease, they can make a person more vulnerable, meaning proactive prevention is essential.
Risk Factors for Periodontal Disease in Seniors (% Contribution)
| Risk Factor | Contribution (%) |
|---|---|
| Smoking | 35% |
| Poor Oral Hygiene | 25% |
| Diabetes | 20% |
| Genetics | 10% |
| Medications | 10% |
This chart illustrates the primary risk factors contributing to periodontal disease in seniors. Smoking and poor oral hygiene are the most significant factors, while genetics and medications play smaller roles.
Recognizing Symptoms Early
Identifying periodontal disease in its early stages can prevent severe complications. Common symptoms include:
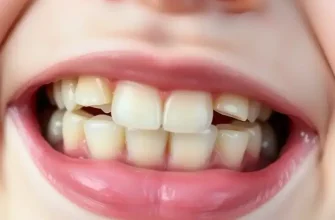
- Persistent bad breath (halitosis): A foul odor that does not go away even after brushing and using mouthwash. This often signals an excess of bacteria in the mouth, which can also leave a bad taste.
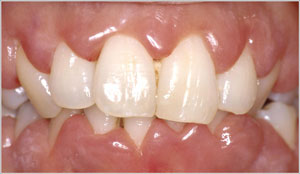
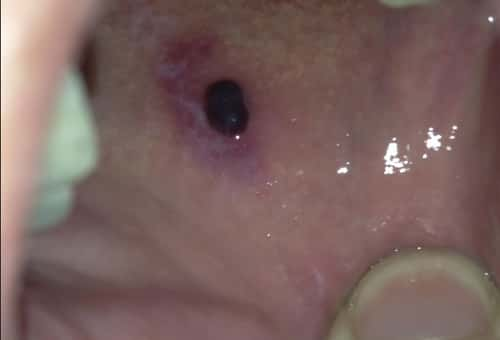
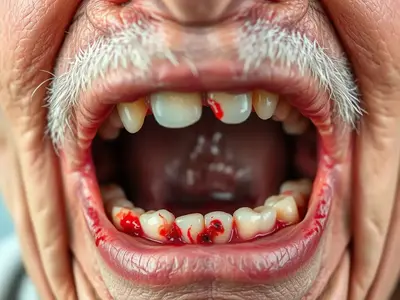
- Red, swollen, or bleeding gums: Gums that look puffy, feel tender to the touch, or bleed during brushing and flossing. Some people may also notice a constant soreness or a tingling sensation in the gums.
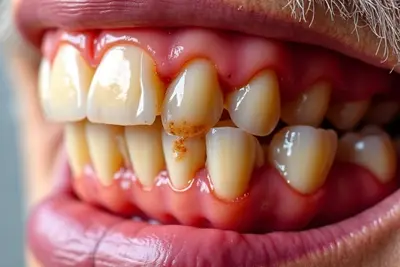
- Receding gum line exposing more of the tooth: Teeth appear “longer” due to gums pulling away, sometimes revealing sensitive root surfaces that make eating hot or cold foods uncomfortable.
- Loose or shifting teeth: A feeling that teeth do not fit together properly when biting, or visible gaps forming where there were none before. This can make it harder to chew certain foods.
- Painful chewing: A dull ache or sharp pain when eating, especially harder foods like apples or nuts. Some individuals also report a sensation of pressure or discomfort in their jaw.
Advanced Diagnostic Methods
Modern dentistry has made diagnosing periodontal disease more accurate and efficient. Here are some key diagnostic tools:
Health Support: This high-absorption Magnesium Glycinate (200 mg) is gentle on the stomach and supports muscle relaxation, better sleep, and metabolic health. You can find this trusted formula on Amazon.
| Diagnostic Method | Accuracy | Average Cost (U.S.) |
|---|---|---|
| Periodontal Probing | 7/10 | $50 – $100 |
| Digital X-Rays | 8.5/10 | $100 – $250 |
| 3D CBCT Imaging | 9/10 | $250 – $500 |
| Salivary Biomarker Tests | 9/10 | $150 – $300 |
Salivary biomarker testing is an emerging technology that detects inflammatory markers, offering a non-invasive and highly precise diagnosis.
Modern Treatment Approaches
Laser Therapy
Laser therapy is a cutting-edge treatment that reduces bacteria and inflammation while promoting faster healing. Unlike traditional surgery, lasers precisely target infected areas without damaging healthy tissue. This method is ideal for seniors because it minimizes pain, shortens recovery time, and reduces the risk of infection.
Scaling and Root Planing
This deep-cleaning procedure removes plaque and tartar from below the gum line. It is often the first step in managing periodontal disease and preventing further damage. Many older adults find it helpful to use a numbing gel before the procedure to reduce discomfort. Regular follow-ups every three to six months can ensure long-term success.
Topical Antibiotics (Arestin, PerioChip)
For those who prefer non-invasive treatments, dentists can apply antibiotics directly to infected gum pockets. These medications, such as Arestin and PerioChip, help eliminate bacteria and reduce inflammation over several weeks. This option is particularly beneficial for seniors with mild to moderate gum disease who may not require surgery.
Guided Tissue Regeneration (GTR)
Severe periodontal disease can lead to bone loss around the teeth. Guided tissue regeneration is a procedure that encourages bone regrowth by placing a small membrane between the gum and bone. This treatment is highly effective for preventing tooth loss and strengthening the jawbone. Seniors with osteoporosis may find this particularly beneficial.
Minimally Invasive Surgery (LANAP – Laser-Assisted New Attachment Procedure)
LANAP is a revolutionary laser treatment that treats advanced gum disease with minimal discomfort. Unlike traditional surgery, LANAP preserves more of the natural gum tissue while promoting regeneration. Many seniors opt for this procedure due to its quick recovery time and reduced risk of complications.
Costs of Periodontal Disease Treatment in Seniors (Average Cost in USD per Procedure)
| Treatment Type | Average Cost (USD) |
|---|---|
| Deep Cleaning | $200 |
| Medication | $150 |
| Gum Surgery | $1000 |
| Dental Implants | $3000 |
This chart displays the average costs of periodontal disease treatments for seniors. While deep cleaning and medication are more affordable, surgical procedures and dental implants require significantly higher expenses.
Real-Life Cases from the U.S.
- Case 1: 72-Year-Old Male from Florida – Struggled with chronic gum inflammation despite regular dental visits. After undergoing LANAP, he experienced a 60% reduction in pocket depth and improved gum health within six months.
- Case 2: 68-Year-Old Female from California – Diagnosed with severe periodontitis linked to her diabetes. A combination of scaling, antibiotics, and guided tissue regeneration restored her oral health, improving her blood sugar control.
Editorial Advice
Reyus Mammadli, healthcare advisor, recommends: “Older adults should prioritize gum health not only for their smiles but for their overall systemic health. Research has linked periodontal disease to heart disease, Alzheimer’s, and respiratory infections. With modern treatments like laser therapy and salivary biomarker testing, managing gum disease is more effective than ever. Seniors should not hesitate to seek specialized periodontal care to maintain their quality of life.”
Investing in oral health means investing in overall well-being—healthy gums, healthy life!
References
- CDC – Periodontal Disease and Older Adults
https://www.cdc.gov/oralhealth/conditions/periodontal-disease.html - American Academy of Periodontology (AAP)
https://www.perio.org/ - National Institute on Aging (NIA) – Oral Health
https://www.nia.nih.gov/ - American Dental Association (ADA)
https://www.ada.org/ - Harvard Health – Gum Disease & Health Links
https://www.health.harvard.edu/ - Mayo Clinic – Periodontitis Guide
https://www.mayoclinic.org/