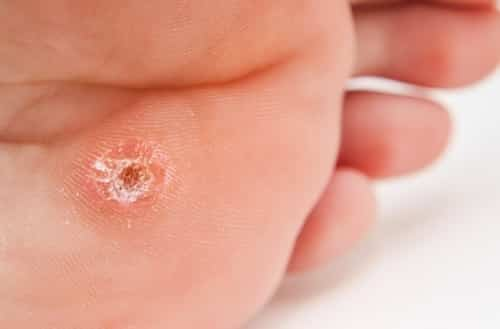
What Are Plantar Warts?
Warts are triggered by an infection of the skin by human papillomavirus (HPV), which is the most common viral infection of the skin. Plantar warts grow on the plantar surface or the sole. They can be found throughout this area but tend to produce symptoms in areas of pressure and friction. The virus that triggers warts, the human papillomavirus, contaminates just the shallow layer of skin, producing a thickened callus-like growth that, is located in an area subjected to pressure, can end up being quite tender.
Although warts characteristically resolve spontaneously, it is sometimes required to deal with painful plantar warts. The incubation duration (the period between infection and the production of the noticeable skin sore) is unknown however estimates differ from months to years. Historical proof is of little advantage in trying to figure out how one’s wart was acquired. There are at least 120 different types of human papillomavirus (HPV), and specific types tend to infect particular anatomical areas, like the plantar surface area of the foot. Other HPV types that contaminate oral or genital mucous membranes are linked in the development of cervical cancer and other malignancies of the oral or anal lining tissues. HPV infections are ubiquitous infections, with least one-half of adults contaminated throughout their lifetime. The actual occurrence of plantar warts in adults is unidentified, but it is a fraction of the approximated 7% -10% of adults with all types of wart infection infections.
What Are Causes and Risk Factors of Plantar Warts?
The HPV types 57, 27, and 1a account for the majority of plantar warts. The infection gains access to the skin through direct contact. It is presumed that shot of the skin takes place in locations most likely to be contaminated by others with plantar warts, like common showers. Once contaminated by HPV, the spontaneous resolution appears to depend on the advancement of immune lymphocytes that damage the virus-infected cells. Vaccines are available to protect versus specific types of genital viral infections; however, there are no vaccines for the HPV types that cause plantar warts.
Health Support: This Vitamin K2 + D3 Complex is essential for bone density, cardiovascular health, and immune function. It’s a highly-rated formula for those looking to maintain optimal nutrient levels. You can find it on Amazon.
- Plantar warts are seen in all age groups, however, are particularly typical amongst children 12-16 years of age and uncommon in the senior.
- Danger aspects for the advancement of plantar warts consist of usage of public showers,
- skin injury, and
- weakened immune system because of specific medications used or illness.
Are Plantar Warts Contagious?
Yes, because a viral infection causes plantar warts (see above) it is possible to spread the infection and the condition from person to person. For instance, locations such as communal showers are areas where the HPV infection can spread.
What Are Plantar Wart Symptoms and Signs?
- Foot pain localized to a thickened area on the sole
- Firm, warty (rough, rough, and spongy, some appear thick and scaly) sores with small pinpoint dark spots in the body of the wart (not always evident): These dark spots are minute, thrombosed (consisting of blood clots) blood vessels in the much deeper layers of the skin.
- Smooth surface with a gray-yellow or brown color
- Often located over areas of pressure or bony point such as the heel and ball of the foot
- A usually flat sense of pressure
- Some warts might fuse to form “mosaic” warts.
What Specialists Treat Plantar Warts?
Generally, a medical care doctor can adequately deal with plantar warts. If treatment under a family physician’s care fails to work sufficiently, a recommendation to a skin doctor (a skin specialist) might be essential.
When Should Someone Seek Medical Care for Plantar Warts?
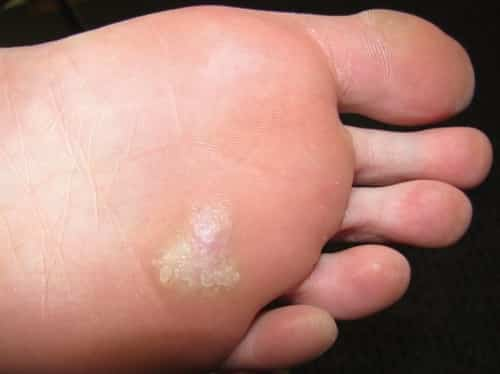
Call a medical professional if natural home treatment fails to deal with the problem.
Health Support: This high-absorption Magnesium Glycinate (200 mg) is gentle on the stomach and supports muscle relaxation, better sleep, and metabolic health. You can find this trusted formula on Amazon.
Corns and calluses, which can resemble warts, typically develop very slowly over several years. It is a good idea to seek advice from a doctor when one is not able to differentiate a plantar wart from corn, callus, nevus (mole), or another type of skin lesion.
Many such growths are safe; however, some may position a considerable health danger. It is also possible for a variety of more primary lesions to appear on foot, including malignant lesions such as cancers and cancer malignancies. Although unusual, these conditions can sometimes be misidentified as a wart.
Seek medical attention for these conditions when
- you or your kid have warts and desire them eliminated;
- acute pain, soreness, swelling, bleeding, or large lesions develop;
- elimination by a doctor by freezing or burning is preferred;
- warts do not disappear entirely after treatment; or
- other warts appear after treatment.
Plantar warts are seldom an emergency; nevertheless, the complications of aggressive treatment can be bleeding, extreme pain, inability to walk, redness, swelling, scarring, and infection.
How Do Doctors Diagnose Plantar Warts?
The medical diagnosis is usually made by observing the wart. If in doubt, the physician might send out a tissue sample of the wart to a pathologist for assessment.
The medical professional might think about other problems that may trigger a similar appearance, such as corns, calluses, or black heel (ruptured capillaries).
Home Remedies for Plantar Warts
Since warts usually go away on their own within months or years and leave no scar, treatment should be conservative, with damaging methods being reserved after all else fails.
- For the momentary relief of pain, place a doughnut-shaped piece of moleskin around the wart. This can be purchased at a drugstore.
- Since the source of discomfort in a lot of symptomatic plantar warts is the thickened layer of hard skin between the nerve-bearing tissues and the ground, simple nontraumatic elimination of this product is a good option.
- This can be achieved with a pumice stone or some other type of abrasive material after the sole has been soaked in water for 20 minutes to soften the wart. Given that the thickened surface area keratin is identical to the keratin found in any callus, it is painless. Bloodless removal by mindful paring with a corn or callus trimmer is a reasonable option. Recently, a battery-powered abrasive wheeled device (Amope) has become available, which should work in eliminating excess keratin. Individuals with diabetes or peripheral artery disease or people who have felt numb due to peripheral neuropathy need to prevent paring.
- Salicylic acid
- Another technique to get rid of the excess keratin is a non-prescription salicylic acid preparation, readily available at the pharmacy in liquid, gel, pad, or lotion kind. Some familiar trademark name is Dr. Scholl’s Wart
- Remover, Compound W, Freezone, DuoFilm, and Wart-Off. Make sure to follow plan instructions because over-application of these items can aggravate the skin. Regularly sand and retreat the wart. It can take numerous months to eliminate a large one utilizing these treatments. Warts can spread, so monitor your feet carefully and treat warts when they are little.
- Soak the afflicted area in warm water for five minutes before using the salicylic acid. This will boost the impacts of the medication.
- Remove any loose tissue with a brush, washcloth, or emery board and dry thoroughly. It is also crucial to submit away as much of the overlying callus tissue as possible so that the medication can permeate the wart appropriately.
- In basic, one must see enhancement in one to two weeks. If such treatment does not yield results after several weeks, see a physician for more aggressive methods of wart elimination.
- The extended use of this medication is not suggested, particularly in babies, people with diabetes, and others with impaired flow.
- Salicylic acid ought to only be used on warts or calluses and not on other types of skin problem or sores.
- A commercial preparation containing about 17% salicylic acid and 17% lactic acid in a fast-drying option (for example, DuoFilm or Dermatech Wart Treatment) can be applied daily after showering. The preparation is permitted to dry and the wart covered with waterproof tape, which is removed after the next shower or bath.
- An individual can pare the wart as soon as a week with a sharp blade (or a relative can do it). It may take many months to clear the wart with this approach.
- The application of “duct tape” is a safe and potentially efficient treatment approach worth trying. Any color duct tape is applied to the wart, which is kept covered 24 hours a day, six out of 7 days a week, for six weeks.
What Are Treatments for Plantar Warts?
Doctors may choose from many different methods for getting rid of plantar warts.
- Acid: One of the most common methods is to burn warts off with a moderate acid used topically to the wart. Lots of applications might be required throughout several weeks to achieve this; however the strategy is extremely successful. Salicylic acid and dichloroacetic (or trichloroacetic) acid work.
- Other acid approaches might be used.
- Upton’s paste: Upton’s paste includes six parts salicylic acid and one part trichloroacetic acid in glycerin, blended to a stiff paste (ordered by prescription).
- A piece of thick adhesive tape (such as Leukoplast), with a hole cut in the middle for the wart, is applied to the sole to isolate the wart. Upton’s paste is applied to the wart, and the whole area is covered with the 2nd piece of tape. This is kept dry and undamaged for one week. The wart is then pared (shaved down) and the paste reapplied till clearance occurs.
- Salicylic acid in soft white paraffin: A mixture of 40% -60% salicylic acid in soft white paraffin is applied daily after showering and covered with waterproof tape. Pare the wart once a week with a sharp blade.
- Efudex (5-fluorouracil), utilized off-label, is another topical lotion that has been utilized to deal with warts.
- Laser treatment: New technology has allowed doctors to use lasers to ruin the wart. The treatment, performed in the physician’s office, is pricey and is likely to result in some scarring. It is efficacy in comparison to other harmful methods in unverified.
- Cryotherapy: Freezing warts with liquid nitrogen is frequently sufficient. This triggers the wart to turn black and eventually fall off within a few days. If used appropriately, there must be no scarring.
- Curettage and desiccation: After injecting an anesthetic, the doctor utilizes an electrical or ultrasonic gadget to destroy the wart, the remainder of which is removed with a curette. This method is likely to cause a scar. (Note:
- The excision of warts is not advised since the surgery may leave a painful scar, and it prevails for warts to return in the scar tissue.)
- Oral medication: No oral medication has proven reliable in the treatment of warts.
- Immunotherapy: For plantar warts that are resistant to treatment, one may be described as a dermatologist for immunotherapy, which develops an immune reaction versus foreign compounds. Physicians might topically apply dinitrochlorobenzene (DNCB) to the warts of patients formerly sensitized to it. Sometimes, the injection of Candida skin test antigen into warts works if the patient is skin test positive to this product.
- Seldom, certain chemotherapeutic representatives (like bleomycin [Blenoxane] are injected directly into the wart.
- There are numerous other treatments available for the treatment of plantar warts. No single treatment is so efficient that it has eliminated using all others. Ultimately, all treatments rely on the client’s body immune system to acknowledge the wart virus proteins and to produce an immune response that will rid the body of this annoying problem.
Follow-up for Plantar Warts
Follow the doctor’s directions. Overuse of recommended medications can result in damaging results.
Is It Possible to Prevent Plantar Warts?
- Avoid strolling barefoot, except on sandy beaches. Usage shower thongs or shoes, especially in public bathroom.
- Change shoes and socks daily.
- Keep feet clean and dry.
- Check children’s feet periodically.
- Prevent direct contact with warts from other individuals or other parts of the body. Don’t touch warts on other people. To keep from spreading out warts, don’t scratch them. Warts spread out ready to little cuts and scratches.
- Do not ignore growths on, or changes in, the skin.
- Prevent sharing socks, shoes, and showering centers.
- Protect the skin from injury, and clean hands frequently. Warts should be covered with water-resistant tape in damp environments such as showers and swimming pools to avoid contaminating oneself or others.
What Is the Prognosis of Plantar Warts?
No matter the home treatment or medical treatment utilized, treatment is not ensured. Warts may come back at any time. Most therapies need several treatments and strict adherence to them. Deal with a physician or skin specialist to figure out which therapy is best.
- In as much as 60% of cases, plantar warts show “spontaneous remission.” This disappearance of the wart is since the action of the body’s immune system.
- Unattended, plantar warts may mature to 1 inch throughout and spread into clusters. Since specific HPV types are oncogenic (able to produce intrusive malignant cancers), it is possible that plantar warts can seldom end up being invasive malignancies. Any wart-like lesion on the sole that does not deal with after proper therapy and continues to increase the size of the need to be biopsied and analyzed by a pathologist.
- An agonizing scar on the sole can pose a lot more serious issue, which is why excisional surgery is not a desirable treatment option.
- Much of these warts solve within one to 2 years. While they last, though, the warts are ugly, annoying, and often agonizing. For these factors, numerous podiatrists (foot specialists) recommend having plantar warts dealt with.
- Warts can grow back. This shows a virus is still in the body and growing. Nevertheless, this is not causing for undue alarm. The type of HPV that causes plantar warts is relatively safe and triggers a couple of problems.
- Warts can spread to other parts of the body, mainly if scratching a wart triggers it to bleed. Blood from a wart consists of the infection and can trigger a new wart to grow in an area that it touches.
- Infection, pain, and scarring might result from extremely aggressive home treatment permeating below the skin surface area. Pain can spread to other websites, and warts can be transmitted to others because of inefficient treatment.