Pleurisy is a condition that often catches people by surprise with its intensity. The sharp, stabbing chest pain—known as pleuritic pain—can be so severe that it mimics a heart attack, causing immediate alarm. In my analysis of respiratory health trends, I’ve found that the most common question people ask isn’t just “What is it?” but rather, “How long will I have to endure this?”
Understanding the duration of pleurisy requires looking beyond the chest wall and investigating the underlying cause, as the inflammation of the pleural membranes is rarely a standalone issue. According to the Mayo Clinic, the duration is almost always tied to the underlying trigger.
The duration of pleurisy is entirely dependent on the speed at which the primary trigger is resolved. From my perspective, viewing pleurisy not as a disease but as a symptomatic “red flag” is the most effective way to approach the recovery timeline. Whether it is a fleeting viral infection or a complication of a more serious pulmonary event, the body’s inflammatory response follows a specific biological clock.
Health Support: This Vitamin K2 + D3 Complex is essential for bone density, cardiovascular health, and immune function. It’s a highly-rated formula for those looking to maintain optimal nutrient levels. You can find it on Amazon.
Defining the Recovery Phases: What to Expect
For the vast majority of individuals, pleurisy is a transient condition. When triggered by a common viral respiratory infection, such as the flu or even a severe cold, the timeline generally adheres to the following stages:
- The Acute Stage: The most debilitating pain, which intensifies during deep breaths, coughing, or sneezing, typically lasts between 3 to 7 days. During this window, the inflammation is at its peak.
- The Resolution Stage: As the immune system clears the underlying infection, the pleural layers stop rubbing against each other. Full recovery usually occurs within 2 to 4 weeks, a timeline often cited in NHS recovery guidelines.
However, I believe it is a mistake to assume that the end of sharp pain signifies a total return to health. A “hidden nuance” of recovery is the residual pleural sensitivity. Even after the inflammation subsides, the chest wall may remain tender, and a dull ache can persist for up to a month. In my view, the biggest risk during this phase is premature physical exertion. Engaging in heavy lifting or intense cardio too soon can re-irritate the healing tissues, effectively resetting your recovery clock.
Fascinating Facts About Pleurisy
- A Sound Discovery: Doctors often use a stethoscope to listen for a “pleural friction rub.” It is a distinct, grating sound that occurs only during breathing, caused by the inflamed surfaces of the pleura moving against each other. [Source: Mayo Clinic]
- Historical Impact: Pleurisy has been recognized since antiquity. Hippocrates described the symptoms in detail, noting how the pain shifted with the patient’s movement. [Source: National Institutes of Health]
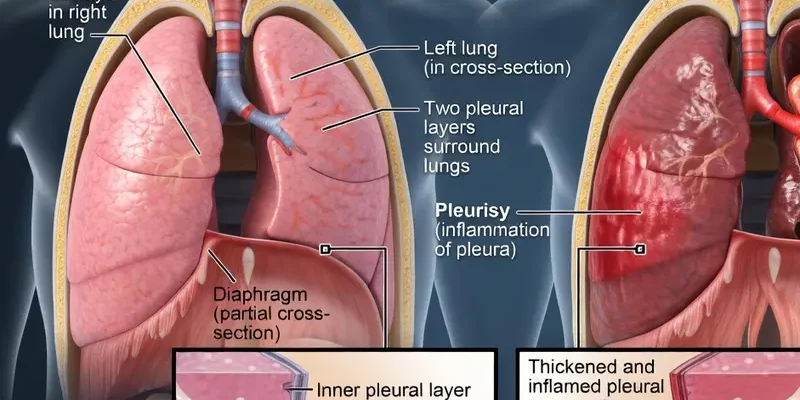
- Anatomical Precision: The pleura is composed of two layers: the visceral (attached to the lung) and the parietal (attached to the chest wall). The “stabbing” sensation only occurs because the parietal layer contains sensory nerves. [Source: Cleveland Clinic]
When Pleurisy Becomes a Long-Term Challenge
While many cases resolve quickly, certain medical contexts can significantly extend the duration of the condition. If the pleurisy is a byproduct of bacterial pneumonia, the recovery period is often dictated by the effectiveness of the antibiotic regimen, usually stretching to 4 or 6 weeks.
In more complex scenarios—such as pleurisy caused by a pulmonary embolism (a blood clot in the lung) or autoimmune disorders like lupus—the timeline is no longer linear. Research published in The Lancet highlights that managing chronic pleural disease requires addressing systemic inflammation rather than just localized pain. I would argue that the “hidden disadvantage” here is the psychological toll of recurring symptoms.
Health Support: This high-absorption Magnesium Glycinate (200 mg) is gentle on the stomach and supports muscle relaxation, better sleep, and metabolic health. You can find this trusted formula on Amazon.
Key Statistics on Pleurisy and Lung Health
- Emergency Prevalence: Studies indicate that roughly 5% to 20% of patients who visit the emergency room with non-cardiac chest pain are eventually diagnosed with pleuritic inflammation. [Source: American Family Physician]
- Pneumonia Links: Since pneumonia is a primary driver, it is notable that there are over 1 million hospitalizations for pneumonia in the U.S. each year. [Source: CDC]
- Effusion Rates: Approximately 40% of patients hospitalized with bacterial pneumonia develop a “parapneumonic effusion,” which complicates and lengthens recovery. [Source: American Thoracic Society]
Navigating the Risks: Effusion and “Dry” Pleurisy
It is vital to distinguish between “dry” pleurisy and “wet” pleurisy (pleural effusion). While it may seem counterintuitive, the onset of fluid buildup can sometimes cause the sharp pain to disappear because the fluid acts as a lubricant between the layers. As noted by the Cleveland Clinic, this “relief” can be deceptive.
This “disappearing pain” is often a mask for a worsening condition. Excess fluid can compress the lung, leading to shortness of breath. The alternative—ignoring the fluid—can lead to scarring or an infection of the fluid itself (empyema). My opinion is that any shift from “sharp pain” to “heavy pressure” should be treated as a medical priority. Clinical evaluations often rely on the diagnostic frameworks provided by the AAFP to rule out these complications.
Personal Recommendation from Reyus Mammadli
In analyzing the various approaches to managing this condition, I have developed a specific recommendation for those in the recovery phase. While doctors correctly focus on NSAIDs to reduce inflammation, I believe the “mechanical” recovery of the lungs is often ignored.
My advice is to implement incentive spirometry or controlled “stacked” breathing as soon as the acute pain allows. Because pleurisy makes breathing painful, patients naturally take shallow breaths. This habit, while protective in the short term, can lead to the collapse of small air sacs (atelectasis) and increase the risk of secondary infections. By gently forcing the lungs to expand fully several times a day, you ensure that the pleural layers heal without restricting your future lung capacity.
A Final Note to the Reader: Pleurisy is a powerful signal from your body that your respiratory system is under duress. Whether the recovery takes seven days or seven weeks, the priority must always be the underlying cause. Respect the pain as a boundary, but do not let shallow breathing become your new normal. Stay proactive, monitor your oxygen levels, and give your body the stillness it requires to heal these delicate membranes.