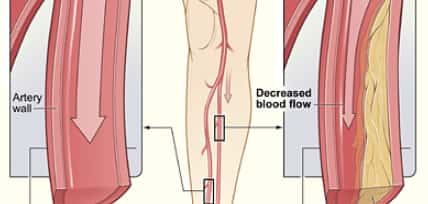
Definition
Peripheral vascular disease (PVD) is a blood flow disorder that causes the capillary beyond your heart and brain to narrow, block, or spasm. This can happen in your arteries or veins. PVD normally causes pain and tiredness, frequently in your legs, and especially during workout. The pain typically enhances with rest.
It can also affect the vessels that supply blood and oxygen to your arms, stomach and intestines, kidneys.
In PVD, blood vessels end up being narrowed and blood flow decreases. This can be due to arteriosclerosis, or “hardening of the arteries,” or it can be triggered by blood vessel spasms. In arteriosclerosis, plaques develop in a vessel and limit the flow of blood and oxygen to your organs and limbs.
As plaque growth advances, embolisms might establish and entirely obstruct the artery. This can result in organ damage and loss of fingers, toes, or limbs, if left neglected.
Health Support: This Vitamin K2 + D3 Complex is essential for bone density, cardiovascular health, and immune function. It’s a highly-rated formula for those looking to maintain optimal nutrient levels. You can find it on Amazon.
Peripheral arterial disease (PAD) develops just in the arteries, which carry oxygen-rich blood away from the heart. According to the CDC, approximately 12 to 20 percent of people over age 60 establish PAD, about 8.5 million people in the United States. PAD is the most common kind of PVD, so the terms are often used to suggest the exact same condition.
PVD is also known as:
- arteriosclerosis obliterans
- arterial deficiency of the legs
- claudication
- periodic claudication
Types
The two primary types of PVD are practical and organic PVD.
Functional PVD indicates there’s no physical damage to your blood vessels’ structure. Rather, your vessels broaden and narrow in response other elements like brain signals and temperature changes. The constricting causes blood flow to reduce.
Health Support: This high-absorption Magnesium Glycinate (200 mg) is gentle on the stomach and supports muscle relaxation, better sleep, and metabolic health. You can find this trusted formula on Amazon.
Organic PVD involves changes in blood vessel structure like inflammation, plaques, and tissue damage.
What Causes Peripheral Vascular Disease?
1. Functional PVD
Your vessels naturally broaden and narrow in response to your environment. But in practical PVD, your vessels overemphasize their action. Raynaud’s disease, when stress and temperature levels impact your blood circulation, is an example of functional PVD.
The most common causes of functional PVD are:
- emotional stress
- cold temperature levels
- running vibrating equipment or tools
- drugs
2. Organic PVD
Organic PVD means there’s change in the structure of your blood vessels. For example, the plaque buildup from arteriosclerosis can cause your capillary to narrow. The main causes of organic PVD are:
- cigarette smoking
- high blood pressure
- diabetes
- high cholesterol
Additional causes of natural PVD consist of extreme injuries, muscles or ligaments with irregular structures, blood vessel inflammation, and infection.
Risk Factors
There are numerous risk factors for PVD. You’re at greater risk for PVD if you:
- are over age 50
- are overweight
- have unusual cholesterol
- have a history of cerebrovascular disease or stroke
- have heart disease
- have diabetes
- have a family history of high cholesterol, hypertension, or PVD
- have hypertension
- have kidney disease on hemodialysis
Lifestyle options that can increase your risk of developing PVD consist of not participating in workout, poor eating routines, smoking or drug use.
Symptoms of Peripheral Vascular Disease
For lots of people, the first signs of PVD begin slowly and irregularly. You may feel pain like fatigue and cramping in your legs and feet that worsens with physical activity due to the absence of blood flow. Other symptoms of PVD include:
| Area of pain | Symptoms |
|---|---|
| legs | reduced hair growth, cramps when lying in bed |
| legs and arms | turn reddish blue or pale |
| legs and feet | thin or pale skin, weak pulses, wounds, or ulcers that won’t heal |
| toes | blue color, severe burning, or thick and opaque toe nails |
| muscles | feel numb or heavy |
Inform your doctor if you’re experiencing any symptoms of PVD. These symptoms are commonly dismissed as the results of aging, but postponed diagnosis and treatment can cause more complications. In extreme cases of blood loss, gangrene, or dead tissue, can happen. If you all of a sudden establish a cold, painful, pale limb with weak or no pulses, this is a medical emergency. You will need treatment as soon as possible in order to avoid severe complications and amputation.
Claudication
The most common symptom of PVD and PAD is claudication. Claudication is lower limb muscle pain when walking. You might discover the pain when you are walking quicker or for fars away. It normally goes away after some rest. When the pain returns, it may take the exact same quantity of time to go away.
Claudication happens when there’s inadequate blood circulation to the muscles you’re using. In PVD, the narrowed vessels can just provide a limited amount of blood. This causes more problems during activity than at rest.
As your PAD advances, symptoms will take place more regularly and worsen. Eventually, you may even experience pain and fatigue during rest. Ask your doctor about treatments to help improve blood circulation and reduce pain.
Complications
Complications from undiagnosed and without treatment PVD can be major and even deadly. Restricted blood flow of PVD can be a warning sign of other types of vascular disease.
Complications of PVD can include:
- tissue death, which can cause limb amputation.
- impotence.
- pale skin.
- pain at rest and with movement.
- severe pain that limits mobility.
- injuries that don’t heal.
- dangerous infections of the bones and blood stream.
The most severe complications involve the arteries bringing blood to the heart and brain. When these ended up being stopped up, it can lead to heart attack, stroke, or death.
Treatment for Peripheral Vascular Disease
The two primary objectives of PVD treatment is to stop the disease from progressing and to help you manage your pain and symptoms so you can stay active. The treatments will likewise decrease your risk for severe complications.
First-line treatment generally involves lifestyle modifications. Your doctor will recommend a regular exercise program that includes walking, a balanced diet, and dropping weight.
If you smoke, you must give up. Smoking directly causes reduced blood flow in vessels. It likewise causes PVD to get worse, along with increasing your risk of cardiovascular disease and stroke.
If lifestyle modifications alone aren’t enough, you might need medication. Medications for Peripheral Vascular Disease consist of:
- cilostazol or pentoxifylline to increase blood flow and relieve symptoms of claudication.
- clopidogrel or daily aspirin to minimize blood clotting.
- atorvastatin, simvastatin, or other statins to lower high cholesterol.
- angiotensin-converting enzyme (ACE) inhibitors to lower hypertension.
- diabetes medication to control blood sugar, if you have diabetes.
Substantial artery clogs may require surgery like angioplasty or vascular surgery. Angioplasty is when your doctor inserts a catheter or long tube into your artery. A balloon on the pointer of the catheter inflates and opens up the artery. In many cases, your doctor will place a small wire tube in the artery, called a stent, to keep it open.
Vascular surgery enables blood to bypass the narrow area through vein grafting.
Peripheral Vascular Disease Piagnosis
If identified early, lots of cases of Peripheral Vascular Disease will react to lifestyle treatments. One method to determine enhancement is to determine how far you can walk without pain. With effective treatment, you need to be able to slowly increase the distance.
Contact your doctor if your symptoms worsen or you experience any of the following:
- legs look pale or blue.
- legs become cold.
- chest pain accompanies leg pain.
- legs end up being red, swollen, or hot.
- new sores or ulcers establish and do no recover.
- fever, chills, weakness, or other signs of infection.
How to Prevent PVD
You can reduce your risk of establishing Peripheral Vascular Disease through a healthy lifestyle. This includes:
- preventing smoking.
- managing your blood sugar, if you have diabetes.
- setting an exercise goal of 30 minutes a day, 5 times a week.
- working to lower cholesterol and high blood pressure.
- consuming a healthy diet that’s low in hydrogenated fat.
- keeping your weight at a healthy level.
Talk to your doctor if you experience symptoms of PVD. Early diagnosis can assist you and your doctor discover ways to minimize your symptoms and increase the efficiency of your treatment.