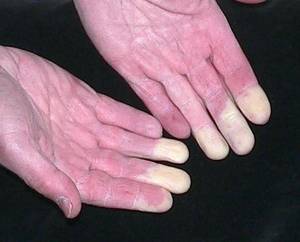
Raynaud’s (ray-NOHZ) Phenomenon causes some areas of your body – such as your fingers and toes – to feel numb and cold in reaction to cold temperatures or stress. In Raynaud’s disease, smaller arteries that supply blood to your skin slim, limiting blood flow to impacted areas (vasospasm).
Women are more likely than men to have Raynaud’s disease, likewise known as Raynaud or Raynaud’s phenomenon or syndrome. It seems more common in people who live in colder climates.
Treatment of Raynaud’s Phenomenon depends on its severity and whether you have other health conditions. For many people, Raynaud’s Phenomenon isn’t disabling, but can impact quality of life.
Symptoms of Raynaud’s Phenomenon
Signs and symptoms of Raynaud’s depend on the frequency, period and severity of the blood vessel spasms that underlie the disorder. Raynaud’s Phenomenon signs and symptoms consist of:
- Cold fingers or toes
- Color modifications in your skin in reaction to cold or stress
- Numb, prickly feeling or stinging pain upon warming or stress relief
- During an attack of Raynaud’s, affected areas of your skin usually first turn white. Then, the affected areas typically turn blue and feel cold and numb. As you warm and circulation enhances, the influenced areas may turn red, throb, tingle or swell. The order of the color modifications isn’t the same for everybody, and not everybody experiences all 3 colors.
Although Raynaud’s Phenomenon most frequently impacts your fingers and toes, the condition can likewise influence other areas of your body, such as your nose, lips, ears as well as nipples. After warming, it might take 15 minutes for regular blood circulation to return to the area.
When to see a doctor
See your doctor right away if you have a history of severe Raynaud’s and establish a sore or infection in one of your afflicted fingers or toes.
Causes of Raynaud’s Phenomenon
Medical professionals don’t entirely understand the cause of Raynaud’s attacks, however blood vessels in the hands and feet appear to overreact to cold temperatures or stress.
Blood vessels in spasm
With Raynaud’s, arteries to your fingers and toes go into vasospasm when exposed to cold or stress, narrowing your vessels and briefly limiting blood supply. With time, these little arteries may thicken slightly, additional limiting blood circulation.
Cold temperature levels are more than likely to activate an attack. Direct exposure to cold, such as putting your hands in cold water, taking something from a freezer or coming across cold air, is the most likely trigger. For some people, psychological stress can cause an episode of Raynaud’s.
Raynaud’s Phenomenon Types
There are two primary types of the condition.
- Main Raynaud’s. Also called Raynaud’s Phenomenon, this most common type isn’t the result of a hidden connected medical condition that might provoke vasospasm.
- Secondary Raynaud’s. Likewise called Raynaud’s phenomenon, this form is brought on by an underlying issue.
Although secondary Raynaud’s is less common than the main type, it tends to be more severe. Symptoms and signs of secondary Raynaud’s typically appear later on in life– around age 40– than they provide for primary Raynaud’s.
Causes of secondary Raynaud’s include:
- Connective tissue illness. Most people who have an uncommon Phenomenon that leads to hardening and scarring of the skin (scleroderma) have Raynaud’s. Other illness that enhance the risk of Raynaud’s include lupus, rheumatoid arthritis and Sjogren’s syndrome.
- Illness of the arteries. Raynaud’s phenomenon can be connected with different illness that influence arteries, such as the buildup of plaques in blood vessels that feed the heart (atherosclerosis) or a condition in which the blood vessels of the hands and feet end up being inflamed (Buerger’s disease). A type of hypertension that impacts the arteries of the lungs (primary pulmonary hypertension) can be linked to Raynaud’s.
- Carpal tunnel syndrome. This condition includes pressure on a significant nerve to your hand (typical nerve) producing numbness and pain in the affected hand. The hand may end up being more susceptible to cold temperatures and episodes of Raynaud’s.
- Recurring action or vibration. Typing, playing piano or doing similar movements for extended periods and running vibrating tools, such as jackhammers, can enhance your risk of developing Raynaud’s.
- Cigarette smoking. Cigarette smoking constricts capillary and is a possible reason for Raynaud’s.
Injuries. Injuries to the hands or feet, such as wrist fracture, surgery or frostbite, can lead to Raynaud’s phenomenon. - Particular medications. Some drugs– consisting of beta blockers, which are used to treat high blood pressure; migraine headache medications that contain ergotamine or sumatriptan; attention-deficit/hyperactivity condition medications; particular chemotherapy agents; and drugs that cause capillary to slim, such as some over-the-counter cold medications– have actually been linked to Raynaud’s.
Risk factors for Raynaud’s Phenomenon
Risk aspects for primary Raynaud’s consist of:
- Sex. Primary Raynaud’s influences women more than men.
- Age. Although anybody can develop the condition, primary Raynaud’s typically starts between the ages of 15 and 30.
- Climate. The disorder is also more typical in people who live in cooler climates.
- Family history. A family history appears to enhance your risk of primary Raynaud’s. About one-third of people with main Raynaud’s have a first-degree relative – a parent, sibling or child – with the condition.
Risk aspects for secondary Raynaud’s consist of:
- Associated illness. These include conditions such as scleroderma and lupus.
- Particular occupations. People in professions that cause repeated trauma, such as operating tools that vibrate, might be more vulnerable to secondary Raynaud’s.
- Direct exposure to certain drugs. Smoking, medications that impact the blood vessels, and direct exposure to particular chemicals, such as vinyl chloride, are associated with an increased risk of Raynaud’s.
Raynaud’s Phenomenon Complications
If Raynaud’s is severe – which is unusual– blood flow to your fingers or toes could completely lessen, triggering defects of your fingers or toes.
If an artery to an afflicted area ends up being blocked totally, sores (skin ulcers) or dead tissue (gangrene) may establish. Ulcers and gangrene can be hard to treat. In extreme untreated cases, your doctor may have to eliminate the afflicted part of your body (amputation).
Tests and medical diagnosis
Your doctor will ask about your symptoms and medical history and carry out a physical exam. Your doctor might also run tests to eliminate other medical problems that may cause comparable signs and symptoms, such as a pinched nerve.
Difference Between Primary and Secondary Raynaud’s Phenomenon
To compare primary and secondary Raynaud’s, your doctor may perform an in-office test called nail fold capillaroscopy. During the test, the doctor examines your nail fold– the skin at the base of your fingernail– under a microscopic lense. Tiny capillary (blood vessels) near the nail fold that are enlarged or warped might indicate a hidden disease. Nevertheless, some secondary diseases can’t be found by this test.
If your doctor suspects that another condition, such as an autoimmune or connective tissue disease, underlies Raynaud’s, she or he might purchase blood tests, such as:
- Antinuclear antibodies test. A positive test for the presence of these antibodies– produced by your body immune system– may show a promoted immune system and prevails in people who have connective tissue diseases or other autoimmune disorders.
- Erythrocyte sedimentation rate. This test figures out the rate at which red cell settle to the bottom of a tube. A faster than regular rate might signal a hidden inflammatory or autoimmune disease.
There’s no single blood test to identify Raynaud’s. Your doctor may purchase other tests, such as those that rule out illness of the arteries, to help determine a disease or condition that might be connected with Raynaud’s.
Raynaud’s Phenomenon and Breastfeeding
Breastfeeding women with Raynaud’s phenomenon experience debilitating nipple pain that typically follows the feeding (although it can take place during the feeding) and might last for hours. When the warm mouth of the baby comes off the breast, the face of the nipple, or part of the nipple, will blanch white and burning pain starts. The nipple can go through numerous color changes (white, blue, red) and the whole breast might pulsate. Poor positioning and bad lock may cause nipple damage, nipple blanching and pain, and are thought by some to activate the problem. Nevertheless, the symptoms of Raynaud’s phenomenon can take place even without inappropriate breastfeeding techniques and nipple damage. Not all nipple vasospasm is Raynaud’s Phenomenon and may completely deal with if the lock can be improved and the damage recovered. Direct exposure to cold is also a known trigger in Raynaud’s phenomenon.
What Women with Raynaud’s Phenomenon Can Do During Breastfeeding
If your nipples are sore and broken, make a visit to see a lactation specialist who can evaluate your latch strategy and assist you to improve it.
- Avoid or decrease any cold exposure to your breasts. Heat will typically stop the vasospasm, which will increase blood circulation to the nipples and help reduce the pain.
- Cover breasts and keep them warm. Even your warm hands can help.
- While nursing, keep the opposite breast covered and warm.
- Wear hand warmers inside your bra when going out into cold air.
- Use dry heat when experiencing pain. Try a hair dryer or heating pad to warm breasts. Wet, warm compresses will help during use, however when gotten rid of, evaporation will occur causing cooling, and the pain can start once again.
- Massage olive oil, warmed between your fingers, into the nipple when it is burning. Press forward from the base of the nipple which helps blood circulation forward into the nipple.
- Quit smoking. Nicotine is a vasoconstrictor and can increase episodes.
Prevent caffeine and other stimulants. Inspect labels to make sure soft drinks don’t include caffeine. - Prevent vibration. Use a good quality breast pump that has a smooth, comfy action.
How Is Raynaud’s Phenomenon Treated
Dressing for the cold in layers and using gloves or heavy socks normally are effective in dealing with mild symptoms of Raynaud’s. Medications are available to deal with more-severe kinds of the condition. The objectives of treatment are to:
- Decrease the number and seriousness of attacks.
- Prevent tissue damage.
- Get rid of the underlying disease or condition.
Medications for Raynaud’s Phenomenon
Depending upon the cause of your symptoms, medications may assist get rid of Raynaud’s. To widen (dilate) capillary and promote circulation, your doctor might recommend:
- Calcium channel blockers. These drugs relax and open small blood vessels in your hands and feet, reducing the frequency and seriousness of attacks in most people with Raynaud’s. These drugs can also help recover skin ulcers on your fingers or toes. Examples consist of nifedipine (Afeditab CR, Procardia), amlodipine (Norvasc) and felodipine (Plendil).
- Alpha blockers. Some people discover relief with drugs called alpha blockers, which combat the actions of norepinephrine, a hormonal agent that constricts capillary. Examples include prazosin (Minipress) and doxazosin (Cardura).
- Vasodilators. Some medical professionals prescribe a drug that relaxes capillary (vasodilator), such as nitroglycerin cream applied to the base of your fingers in order to help heal skin ulcers. Some vasodilators typically utilized to alleviate other conditions, including the hypertension drug losartan (Cozaar), the erectile dysfunction medication sildenafil (Viagra, Revatio), the antidepressant medication fluoxetine (Prozac, Sarafem, others), and a class of medications called prostaglandins, may eliminate the symptoms of Raynaud’s.
Work with your doctor to find what works best for you. Inform your doctor if a drug loses efficiency or causes worrisome side effects.
Some medications can intensify Raynaud’s by causing enhanced blood vessel spasm. Your doctor may recommend that you prevent taking:
- Certain non-prescription (OTC) cold drugs. Examples include drugs which contain pseudoephedrine (Chlor-Trimeton, Sudafed, others).
- Beta blockers. This class of drugs, utilized to get rid of hypertension and heart disease, includes metoprolol (Lopressor, Toprol-XL), nadolol (Corgard) and propranolol (Inderal, InnoPran XL).
Surgical Treatments and Medical Treatments for Raynaud’s
For some cases of severe Raynaud’s, approaches other than medications might be a treatment choice:.
Nerve surgery. Nerves called sympathetic nerves in your hands and feet control the opening and constricting of capillary in your skin. Cutting these nerves interrupts their overstated reaction.
Through little cuts in the affected hands or feet, a doctor strips away these tiny nerves around the blood vessels. This surgery (sympathectomy) might decrease the frequency and duration of attacks, but it’s not constantly successful.
Chemical injection. Doctors can inject chemicals such as local anesthetics or onabotulinumtoxin type A (Botox) to block considerate nerves in impacted hands or feet. You may have to have actually the procedure repeated if symptoms return or continue.
Home Remedies for Raynaud’s Phenomenon
A range of actions can decrease Raynaud’s attacks and assist you feel much better.
- Do not smoke. Smoking cigarettes causes skin temperature to stop by constricting blood vessels, which may cause an attack. Breathing in previously owned smoke also can exacerbate Raynaud’s.
- Exercise. Workout can increase flow, among other health benefits. If you have secondary Raynaud’s, speak with your doctor prior to working out outdoors in the cold.
- Control stress. Learning to acknowledge and avoid difficult circumstances might assist manage the variety of attacks.
- Avoid quickly changing temperatures. Try not to move from a hot environment to an air-conditioned space. If possible, prevent frozen-food sections of supermarket.
Raynaud’s Phenomenon Attack
First, warm your hands, feet or other affected areas. To gently warm your fingers and toes:.
- Get indoors or to a warmer area.
- Wiggle your fingers and toes.
- Place hands under armpits.
- Make broad circles (windmills) with your arms.
- Run warm – not hot – water over your fingers and toes.
- Massage your hands and feet.
If stress triggers an attack, get out of the stressful circumstance and unwind. Practice a stress-reduction method that works for you, and warm your hands or feet in water to help lessen the attack.
Alternative Medicine for Raynaud’s Phenomenon
Lifestyle modifications and supplements that encourage better flow might help you manage Raynaud’s. Nevertheless, more research is required. If you’re interested, talk to your doctor about:.
- Fish oil. Taking fish oil supplements could help enhance your tolerance to cold and postpone the narrowing of your blood vessels that triggers Raynaud’s attacks.
- Ginkgo. Ginkgo supplements could help reduce the number of Raynaud’s attacks you have.
Speak to your doctor before taking supplements. Your doctor can warn you if there are prospective drug interactions or side effects of alternative treatments.
Managing Raynaud’s takes patience and effort. Deal with your doctor to manage your condition and keep a positive mindset. The majority of individuals with Raynaud’s respond to treatment.