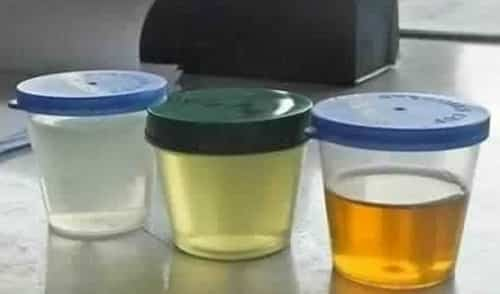
A change in urine color can be stressful for patients and doctors alike. A lot of the reasons for abnormal urine color are benign impacts of medications and foods; nevertheless, a modification in urine color may be a sign of an underlying pathological condition. The good news is that in many cases the diagnosis can be identified from a thorough history and urinalysis. This post provides a lot of the conditions physicians might encounter and will help them form a slim differential diagnosis and treatment plan.
Understanding Urine Color Change
Ubnormal urine color can be upsetting to patients, their relative, and clinicians alike. Patients anticipate a description for any modifications in the color of their urine, and truly so. Unfortunately, little initial research exists relating to urine staining. Much of the info comes from case credit reports. Additional complicating the issue is that there is no goal, standardized way to explain urine color, according to iytmed.com. One person may use the term “dark” to explain findings without fully defining the term to imply either a bolder shade of yellow, muddy brown, orange, and even a crimson red (check out urine color chart below).
More than 20 years earlier, the Southern Medical Journal published a review article on the differential diagnosis of numerous urine colors. Although beneficial at that time, clinicians are not likely to perform benchtop chemistry tests such as adding hypochlorite bleach to urine samples to determine the existence of aminosalicylic acid. The present review efforts to list a number of the conditions physicians may encounter and help them form a narrow differential medical diagnosis and treatment plan.
Health Support: This Vitamin K2 + D3 Complex is essential for bone density, cardiovascular health, and immune function. It’s a highly-rated formula for those looking to maintain optimal nutrient levels. You can find it on Amazon.
Urine Color Meaning Chart
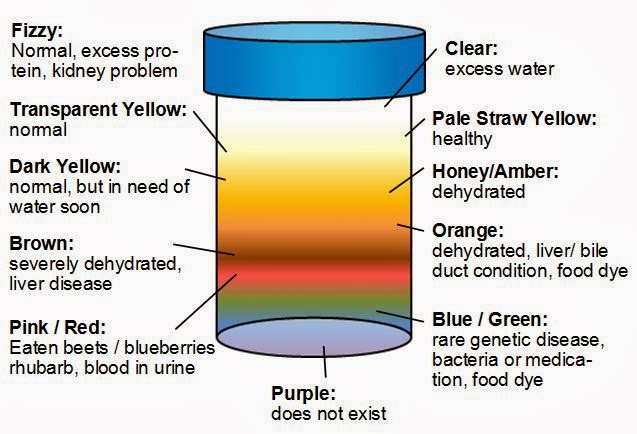
Urine Color Meaning
Red Urine
The first issue we encounter with word “red” is that the term is broad enough to incorporate the colors pink, tones of red, orange, brown, or black, depending on which clinician views the sample. Whenever a patient establishes red urine, the doctor needs always to order a urine dipstick and urinalysis to look for the existence of red blood cells or hemoglobin. If blood is genuinely present, then the differential is broad and consists of conditions of the kidney gathering system and hematologic system, and contamination from menstrual blood. Added workup will be guided depending on the patient’s history and physical examination. A computed tomography scan may illuminate an anatomical problem such as entrapment of the left renal vein between the exceptional mesenteric artery and the aorta, typically called Nutcracker syndrome. A transfusion reaction, glucose-6 -phosphate dehydrogenase shortage, sickle cell anemia, or thalassemia can result in hemolytic anemia and darken the urine to a deep reddish color.
Even without the presence of blood, dark red urine might be an ominous sign. The classification of illness collectively referred to as porphyria can provide dark urine, abdominal pain, photosensitive rashes, or neuropsychiatric complaints. The disease is difficult to identify since it is rare. Also, lots of medical facility laboratories are ill geared up to perform porphyrin analysis on urine, further delaying treatment.
A fairly brand-new development in US toxicology practice is the use of hydroxocobalamin for cyanide poisoning. The traditional treatments for cyanide poisoning– amyl nitrite, salt nitrite, and sodium thiosulfate– can induce methemoglobinemia, additional minimizing the oxygen-carrying ability of red cell. Hydroxocobalamin works by integrating with cyanide to form cyanocobalamin (vitamin B). An unintended yet benign effect of its administration is to color the skin and urine red. The results usually wear away after a few days.
Other medications related to red urine development include warfarin, phenazopyridine, rifampin, ibuprofen, and deferoxamine. Specific foods such as carrots (carotene), blackberries, and beets can sometimes cause red urine. Curiously, beeturia appears to be connected to the co-ingestion of oxalate-containing foods such as rhubarb, spinach, and oysters.
Health Support: This high-absorption Magnesium Glycinate (200 mg) is gentle on the stomach and supports muscle relaxation, better sleep, and metabolic health. You can find this trusted formula on Amazon.
Finally, a patient with factitious disorder might provide with red urine from including blood or another red-colored material straight to his or her sample. These patients may provide with otherwise nonspecific complaints and will go through an extensive however useless workup. Malingering is hard to diagnose and may require repeat urine samples gotten under direct observation to discover the condition lastly.
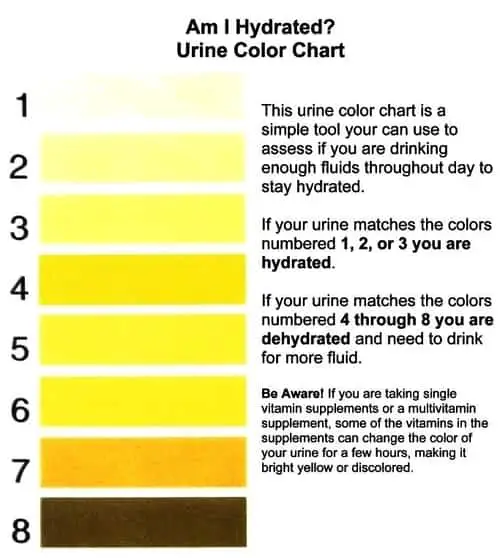
Orange Urine
Continuing along the spectrum of red conditions, orange urine might be a manifestation of one of the above-named conditions or ingested drugs such as high-dose riboflavin, phenazopyridine, and isoniazid. According to one study, 50% of isoniazid users will notice staining, making the finding common but insensitive when checking for compliance. The discovery is harmless and requires no further workup if there are no extra problems.
Oddly, one case credit report points out an infant with orange urine caused by a urinary tract infection. The apparent cause was a Gram-negative bacillus that produces indole from tryptophan. The conclusion reached by the authors is strange because indole reactions typically produce blue, green, or purple urine.
Brown Urine
As red urine ends up being darker, some clinicians might analyze the color as brown. As an outcome, any of the conditions or ingestions listed above ought to be thought about whenever a sample is thought to be brown. In the 1980s, a case series on acetaminophen overdose demonstrated that in addition to hepatorenal failure, three patients established brown urine since of the accumulation of the metabolite p-aminophenol.
Brown urine might be a sign of melanocytes in the urinary system. Metastatic melanoma can cause an uncommon condition called diffuse melanosis, triggering dark skin, remote sores to the internal organs, and brown or black urine. One case credit report points out a patient with severe kidney injury from melanin build-up in the tubular system. The diagnosis is poor at this moment.
Black Urine
Black urine rounds out the discussion of reasons for reddish urine discoloration. A lot of the conditions noted above can provide with black urine if the discoloration is dark enough; nevertheless, several of the conditions listed below are unsafe sufficient that the existence of black urine requires additional workup. Example causes include metronidazole, nitrofurantoin, cascara or senna laxatives, methocarbamol, sorbitol, and the phenol acquired cresol, a common disinfectant consumed by problem drinkers, which typically is devastating and causes severe systemic toxicity. Intramuscular iron injections are commonly associated with black urine as a good impact of the medication.
Patients, in this case, require peace of mind. The presence of melanin in the urine can cause brown discoloration, as talked about above, or with a black tint. Methyldopa and L-dopa can induce urinary melanin in alkalotic urine, which is a known adverse impact of these medications. Alcaptonuria is an uncommon hereditary disease in which the body has a damaged ability to catabolize tyrosine, leading to a build-up of homogentisic acid in the body. It presents clinically with arthritis and darkening of the skin and urine. The medical diagnosis is made by determining homogentisic acid in the urine. There is no cure, nevertheless, and treatment consists of high-dose vitamin C and restricting protein intake.
Blue and Green Urine
Blue urine most typically appears to be caused by ingestion of methylene blue. This compound is made use of in the United States for diagnostic tests, treatment of methemoglobinemia, or as a treatment for refractory hypotension. Outside the country, nevertheless, oral methylene blue might be discovered in medications and home solutions because it has antimicrobial homes. Real blue urine seems to be exceedingly uncommon, potentially since blue pigments integrate with urochrome, the significant contributor to urine’s normal yellow tone, to develop a green color before urine’s elimination. In that regard, there are lots of case files where methylene blue turns urine green.
Other medications related to green urine might consist of phenol groups and include promethazine, thymol, cimetidine, and propofol. The system of action seems caused by phenol’s conjugation by the liver and subsequent excretion by the kidneys. The stamina of the green appears to be dose associated. Strangely enough, propofol also is associated with pink and white urine.
Some nonphenol drugs kept in mind to produce green urine are metoclopramide, amitriptyline, and indomethacin. In any event, the urinary findings of all of the above medications are good effects and do not get further workup as soon as urinalysis results are typical.
There are separated case files of parenteral absorption of tetrahydronaphthalene (Cuprex), a pesticide that was made use of in the 1980s as a non-prescription treatment for lice, and consumptions of the herbicides mefenaceta and imazosulfuro producing green urine. A patient who has actually can be found in contact with these compounds must be dealt with as if he or she were poisoned and deserved full toxicology workup, stabilization, and possible admission to the excellent care device.
In the necessary care setting, patients receiving enteral tube feeds have on event been noted to produce green urine. The belief is that the food coloring additive Food Dye and Color Blue Number 1 (FD&C Blue No. 1) is taken in from the gastrointestinal (GI) system in sufficiently high concentrations to cause dark green urine. In animal designs, > 1 % of FD&C Blue No. 1 is discovered in rat urine. This finding is harmless and vanishes with changes in tube feeds.
Not all reasons for green urine are innocuous, however. Pseudomonas-causing bacteremia and urinary system infections can provide with green urine. In this case, the patient’s history and physical exam ought to indicate an infectious condition and urine and blood cultures may make the diagnosis. Treatment is centered on clearing the infection instead of on urine color.
Bile pigments in the urine represent a rare but worrisome cause of staining. Upon finding biliverdin, clinicians have to take a careful and thorough history to identify the area of the leak. Radiographs or invasive imaging may even be required. A case credit report of an enterovesical fistula triggered by pelvic radiation treatment offers one such source of bile. Other rarer causes of blue and green urine consist of conditions that impair amino acid absorption from the GI system.
Blue diaper syndrome and Hartnup illness are autosomal recessive disorders in which tryptophan develops in the GI tract, triggering germs to metabolize it to indole, resulting in a buildup of indican in the urine. The blue coloring by itself is not dangerous; however it does indicate another underlying condition that needs investigation.
Purple Urine
The just known cause of purple urine is purple urine bag syndrome. This usually benign condition is believed to arise from a series of actions in which tryptophan in the GI system is transformed to indole, the liver then metabolizes the indole and excreted by the kidneys, and the end product goes through change by bacteria in the urine to develop indigo (a blue pigment) and indirubin (a red pigment). These pigments combine to form purple urine that then stains the polyvinylchloride of a Foley catheter. Purple urine is connected with Gram-negative bacteriuria and usually fixes after treatment with prescription antibiotics and changing the catheter.
White Urine (Albinuria)
Albinuria has an extensive differential diagnosis and requires a more comprehensive investigation beyond an easy urinalysis. Sediment from minerals in the urine such as hypercalciuria, phosphaturia, or hyperoxaluria occasionally can be discovered after centrifugation and analysis. Consultation with a nephrologist is recommended at this moment since modifications in dietary intake, and medication initiation may be needed. Severe urinary tract infection is one possible cause of white urine because purulent fluid might get in the bladder. Also, caseous material from urinary tuberculosis commonly must be amused. Mindful urine culture is required, followed by antibiotic therapy.
Chyluria is another possible diagnosis. It emerges from irregular communication between the lymphatics to the urinary tract, a lot of frequently as an outcome of filariasis, however typically can be the outcome of a lymphatic fistula. Antiparasitic drugs are of no benefit since this point usually sterilizes the urine. Recommendation to a urologist is required because the patient might need intervention to close the communication.
Urine and Urination Facts
- Kidneys: In your lifetime, your kidneys filter more than one million gallons of water, enough to fill a pond. Remarkably, one kidney can handle the task perfectly well. In truth, if you lose a kidney, your staying kidney can increase in size by 50 percent within two months, to take control of the job of both.
- Consistency: About 91-96% of urine consists of water. Urine likewise contains a variety of inorganic salts and organic compounds, including proteins, hormones, and a wide range of metabolites, varying by what is introduced into the body.
- Urine Production: The typical urine production in adult humans is around 1.4 L of urine per individual daily with a standard variety of 0.6 to 2.6 L per individual each day, produced in about 6 to 8 urinations daily depending on state of hydration, activity level, ecological elements, weight, and the person’s health. Producing excessive or insufficient urine requires medical attention.
- Density: Human urine has a particular gravity of 1.003 – 1.035. Variances may be associated with urinary disorders.
- Urine pH Levels: The pH level of human urine is generally within the range of 5.5 to 7 with an average of 6.2.
- Urinalysis: A urinalysis (UA), also referred to like routine and microscopy (R&M), is an array of tests carried out on urine, and one of the most typical techniques of medical diagnosis. A part of a urinalysis can be carried out by utilizing home urine test strips, in which the test results can be read as their color changes. A urinalysis checks appearance, concentration and material of urine and is used to discover and/or manage an extensive range of medical conditions, such as urinary tract infections (UTI’s), kidney disease and diabetes and if specific compounds are present, or if certain levels are above, or below, normal which can indicate the presence of compounds like proteins, ketones, hemoglobin, and nitrites, as well as hazardous pathogens.
- Compounds: In a study, scientists discovered that a minimum of 3,079 compounds could be found in urine. 72 of these compounds are made by germs, while 1,453 come from the body itself. Another 2,282 originated from a diet, drugs, cosmetics or direct environmental exposure (some substances come from more than one group).
Conclusions
A change in urine color can be upsetting for patients, their relative, and clinicians alike. You can ask reasonable question as ‘what is my pee color meaning?” This article presented a lot of the possible causes of urine staining. Fortunately, many of these causes are benign results and can be clarified from a comprehensive history. At a minimum, nevertheless, physicians should order a urinalysis when confronted with an irregular urine color due to the fact that potential pathologies do exist.