Ah, the Achilles tendon. The strongest, thickest tendon in the human body. It’s like the Hulk of tendons, responsible for everything from walking to sprinting, jumping, and even standing on your tiptoes to reach that top shelf. But just like the mighty Greek hero it’s named after, the Achilles tendon has one fatal flaw: it can snap. And when it does, it’s not subtle. Achilles tendon rupture is the kind of injury that takes you from hero to zero in a split second.
What Exactly Happens During an Achilles Tendon Rupture?
Imagine this: you’re feeling good, mid-stride, when suddenly, it feels like someone kicked you in the back of the ankle. Except, no one’s around. That’s your Achilles tendon giving out. A rupture occurs when the tendon that connects your calf muscles to your heel bone tears, either partially or completely. The result? Pain, swelling, and the sudden inability to push off your foot or stand on your toes. In other words, you’re down for the count.
Causes: Why Does It Happen?
Achilles tendon rupture doesn’t play favorites, but it does have a thing for athletes, weekend warriors, and anyone who’s a bit too overconfident in their physical prowess. It usually happens during activities that involve sudden starts, stops, or pivots—think basketball, tennis, or that moment when you decide to sprint across the street because the light’s about to change. Age is also a factor. The older you get, the more brittle that once-mighty tendon becomes. And if you’re taking certain medications, like corticosteroids, your risk goes up even more.
Symptoms: How Do You Know It’s Ruptured?
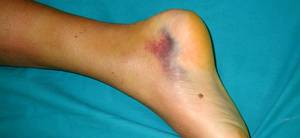
The symptoms of an Achilles tendon rupture are hard to ignore—mainly because you’ll probably be on the ground. That telltale ‘pop’ sound is often the first sign, followed by sharp pain in the back of your ankle and calf. You might notice swelling or bruising, and walking becomes a challenge, if not impossible. If you can’t point your toes downward or push off the ground with your foot, it’s time to call the doctor.
Health Support: This Vitamin K2 + D3 Complex is essential for bone density, cardiovascular health, and immune function. It’s a highly-rated formula for those looking to maintain optimal nutrient levels. You can find it on Amazon.
Diagnosis: What Will Your Doctor Do?
Diagnosis typically involves a physical exam where the doctor will gently squeeze your calf to see if your foot moves—this is known as the Thompson test. If your foot doesn’t respond, it’s likely you’ve ruptured your Achilles tendon. To confirm the extent of the damage, imaging tests like an MRI or ultrasound might be ordered. This will help determine whether the rupture is partial or complete, which is crucial for deciding on treatment.
Treatment: Surgery or No Surgery?
Here’s where things get interesting. The treatment for an Achilles tendon rupture depends on several factors, including your age, activity level, and the severity of the rupture. Traditionally, surgery has been the go-to treatment, especially for athletes or active individuals, as it lowers the risk of re-rupture and often leads to a quicker return to full activity. During surgery, the torn ends of the tendon are stitched back together, and you’re put in a cast or boot to keep your foot immobilized.
Non-surgical treatment is also an option, particularly for older or less active individuals. This approach involves wearing a cast, brace, or walking boot for several weeks, allowing the tendon to heal naturally. The downside? A higher chance of re-rupture and a potentially longer recovery time. But, with the right physical therapy, many people recover just as well without going under the knife.
Recovery: Getting Back on Your Feet
Whether you opt for surgery or not, recovery from an Achilles tendon rupture is a marathon, not a sprint. Expect to be in a cast or boot for 6 to 12 weeks, with physical therapy starting as soon as your doctor gives the green light. The goal is to gradually restore your range of motion, strength, and flexibility. It can take 6 months to a year to fully recover, and even then, you might need to ease back into high-impact activities.
Health Support: This high-absorption Magnesium Glycinate (200 mg) is gentle on the stomach and supports muscle relaxation, better sleep, and metabolic health. You can find this trusted formula on Amazon.
The key to a successful recovery? Patience. Rushing back too soon can lead to setbacks or, worse, another rupture. Listen to your body, follow your physical therapist’s advice, and remember: it’s a long road, but one that leads back to full strength.
Conclusion: The Achilles Heel
An Achilles tendon rupture is no joke. It’s a serious injury that requires serious treatment and an even more serious commitment to recovery. But with the right approach, you can come back from it, possibly even stronger than before. Just don’t forget to stretch before that next pickup game. Achilles’ pride was his downfall—don’t let it be yours too.