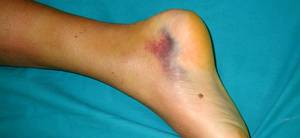
Achilles tendon ruptures can be devastating, sidelining athletes and impacting the quality of life for everyday individuals alike. The road to recovery is long and nuanced, requiring dedication, the right approach, and sometimes a dose of patience. This rehabilitation protocol delves into the latest trends in Achilles tendon recovery, balancing traditional approaches with modern research to help you navigate this challenging but ultimately rewarding journey.
How Common Is Achilles Tendon Rupture? A Statistical Perspective
Achilles tendon ruptures are not as rare as you might think. Recent data indicates that roughly 18 in 100,000 people will suffer from this injury each year. It’s particularly common among men aged 30-50, often occurring during sports activities like basketball, tennis, or even simple running. Interestingly, the rupture rate is growing as more adults embrace active lifestyles later in life, with a 20% increase in Achilles tendon injuries reported over the last decade.
The Achilles tendon, the strongest tendon in the body, is responsible for the explosive strength needed for running, jumping, and pushing off the ground. However, this strength can also make it vulnerable to injury, particularly in those who make sudden, high-intensity movements without proper preparation.
A Week-by-Week Approach: From Injury to Recovery
Weeks 1-2: Protection and Immobilization
The initial phase focuses on immobilization to prevent further injury and allow the tendon to start healing. Typically, this means wearing a splint, cast, or a walking boot to keep the foot in a plantarflexed position. During these first two weeks, the tendon begins its journey of healing, and no weight-bearing is recommended for most patients.
Health Support: This Vitamin K2 + D3 Complex is essential for bone density, cardiovascular health, and immune function. It’s a highly-rated formula for those looking to maintain optimal nutrient levels. You can find it on Amazon.
Many patients report frustration during this period, as the complete lack of mobility can feel counterintuitive. However, Dr. Robert Harrison, an orthopedic surgeon, explains that this immobilization is crucial: “The Achilles tendon needs to begin reattaching, and any undue stress during this phase can delay progress or even cause re-rupture.”
Weeks 3-6: Gradual Weight-Bearing
After the initial healing, patients gradually transition to partial weight-bearing with the help of crutches or a walking boot. Controlled mobility exercises are introduced to prevent stiffness and muscle atrophy. Physical therapy usually begins during this time, emphasizing gentle range-of-motion (ROM) exercises. The patient will often start with seated exercises that promote ankle mobility without stressing the tendon.
A 2019 study highlighted the effectiveness of early mobilization, showing that patients who began ROM exercises within the first six weeks had a 15% faster return to activities compared to those who remained fully immobilized.
Weeks 7-12: Strength and Balance Training
This phase is where active rehabilitation takes center stage. Patients transition to full weight-bearing without crutches, typically around week 8. Physical therapy now includes exercises that focus on calf strengthening, balance, and proprioception. Here’s where the groundwork for a return to everyday activities is laid down.
Health Support: This high-absorption Magnesium Glycinate (200 mg) is gentle on the stomach and supports muscle relaxation, better sleep, and metabolic health. You can find this trusted formula on Amazon.
Table 1: Key Exercises During Weeks 7-12
| Exercise | Purpose |
|---|---|
| Seated Heel Raises | Strengthening calf muscles |
| Single-leg Stance | Improving balance |
| Resistance Band Work | Increasing ankle stability |
| Toe-to-Heel Rocking | Restoring normal gait |
Patients are often eager to push their limits during this phase, but overdoing it can lead to setbacks. Dr. Linda Parker, a renowned physiotherapist, advises, “Patients need to remember that strength is built gradually. Increasing intensity too quickly is one of the most common causes of re-injury.”
Weeks 13-20: Advanced Strengthening and Functional Training
At this stage, the tendon is significantly healed, and the focus shifts to high-level strengthening and preparing for a return to sports or vigorous activities. Plyometric exercises, such as box jumps and skipping, help restore the explosive power needed for dynamic sports. It’s also crucial to regain full flexibility of the calf muscle and tendon, which will ultimately improve performance and reduce the risk of future injuries.
The return-to-sport rate after an Achilles tendon rupture varies, with about 65-80% of patients able to resume pre-injury activities within 8-12 months. However, this can differ significantly based on age, overall health, and adherence to the rehabilitation protocol.
Table 2: Rehabilitation Progression Chart
| Week Range | Key Focus | Expected Outcome |
|---|---|---|
| 1-2 | Immobilization | Tendon protection |
| 3-6 | Gradual Weight-Bearing | Initial tendon flexibility |
| 7-12 | Strength and Balance | Improved gait and stability |
| 13-20 | Advanced Strengthening | Ready for advanced movement |
Modern Approaches: Surgical vs. Conservative Treatment
One of the most debated topics in Achilles tendon rupture rehabilitation is surgical vs. non-surgical intervention. Surgical repair was once considered the gold standard, especially for active individuals, but recent research suggests that conservative treatment, with early functional rehabilitation, can provide comparable outcomes for many patients.
A 2021 meta-analysis comparing surgical and conservative treatments showed that re-rupture rates were similar, around 3-5%, provided patients adhered to early mobilization protocols. Surgical intervention tends to lead to a slightly faster recovery, but also carries a higher risk of complications like infection.
Dr. Joseph Carter, a sports medicine specialist, advises, “The choice between surgical and non-surgical treatment depends heavily on the patient’s activity level, age, and overall health. Surgery may be the best option for an athlete aiming to return to competition, whereas conservative treatment might be better for someone with a less physically demanding lifestyle.”
Lifestyle Changes: Setting the Stage for Recovery
Recovery from an Achilles rupture isn’t just about exercises—it’s about lifestyle. Completely avoiding smoking and alcohol is paramount, as both can impede tendon healing. Smoking, in particular, is linked to delayed healing and higher rates of complications. Proper nutrition, rich in protein and Vitamin C, is essential to provide the building blocks for tendon repair.
Many experts stress the importance of rest and stress management. Overtraining or attempting to accelerate recovery against medical advice often leads to setbacks, sometimes requiring more intensive treatment or delaying progress by several weeks.
Our Editorial Team’s Recovery Tips
Recovering from an Achilles tendon rupture requires patience, discipline, and a willingness to accept setbacks along the way. Our advice: follow the plan laid out by your healthcare professionals and communicate openly with your physical therapist about your progress and any discomfort you feel. Remember, this is a marathon, not a sprint.
Consider every phase as a building block for the next. Start slow, build consistency, and trust the process. When in doubt, always err on the side of caution—your long-term mobility and quality of life depend on it. Your body has an incredible ability to heal, given the time and right conditions, so stick with it, and you’ll be back on your feet stronger than ever.