Aortobifemoral bypass surgery is a significant vascular procedure, and if you are facing it, I understand the weight of that decision. This surgery is typically recommended when the iliac arteries—the main vessels supplying blood to your legs—become severely blocked due to Atherosclerotic Occlusive Disease. In my experience, while the prospect of such an invasive procedure is daunting, the restoration of mobility and the prevention of limb loss make it a cornerstone of modern vascular intervention.
Understanding the Procedure: Why It Is Necessary
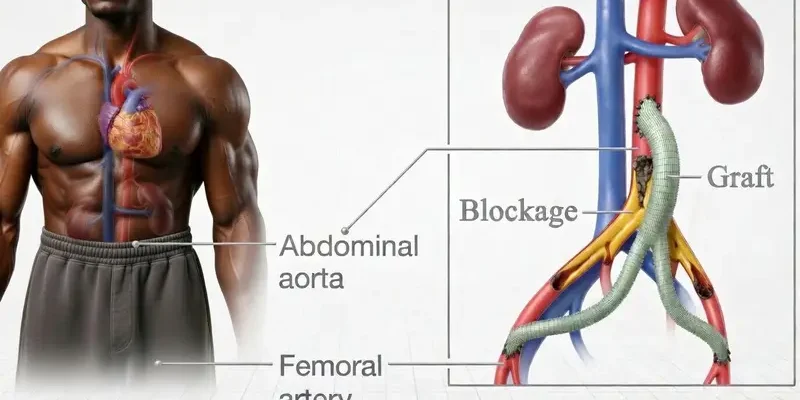
In this operation, a Y-shaped synthetic graft is used to reroute blood flow. I find that many patients are surprised to learn that we don’t actually remove the blocked arteries. Instead, we create a “detour.” One end of the graft is attached to the aorta (the body’s main artery), and the two branched ends are attached to the femoral arteries in each groin. According to the Society for Vascular Surgery, this bypass remains the most effective long-term treatment for extensive blockages that cannot be managed by simpler methods.
While some might argue that endovascular stenting is a less invasive alternative, I believe the “open” aortobifemoral bypass remains the gold standard for complex cases. The durability of a surgical graft often far outlasts that of a stent in younger, active patients.
Key Statistics in Vascular Health
- Success Rate: The five-year patency rate (the likelihood of the graft remaining open) for aortobifemoral bypass is approximately 85% to 90%.
- Prevalence: Peripheral Artery Disease (PAD) affects over 8.5 million Americans aged 40 and older, as reported by the American Heart Association.
- Risk Reduction: Smoking cessation after surgery reduces the risk of graft failure by over 3-fold compared to patients who continue to smoke.
Preparation and the Surgical Nuance
Preparing for this surgery isn’t just about fasting before the procedure. It’s about optimizing your cardiovascular health. From my perspective, the hidden challenge here isn’t the surgery itself, but the underlying systemic nature of atherosclerosis. If your leg arteries are blocked, there is a high probability your coronary arteries need attention too.
Health Support: This Vitamin K2 + D3 Complex is essential for bone density, cardiovascular health, and immune function. It’s a highly-rated formula for those looking to maintain optimal nutrient levels. You can find it on Amazon.
I always recommend a rigorous cardiac clearance. The nuance here is that “being fit for surgery” is different from “being healthy.” We focus on ensuring your heart can handle the stress of clamping the aorta, which is a critical moment during the operation. As detailed by the Mayo Clinic, preoperative testing often includes EKGs and stress tests to minimize the risk of cardiac complications during the bypass phase.
Fascinating Facts About Vascular Surgery
- Synthetic Durability: The grafts used (usually Dacron or PTFE) are designed to last for the rest of a patient’s life and are biocompatible, meaning the body does not reject them like an organ transplant.
- Blood Flow Volume: The aorta is roughly the diameter of a garden hose, and during this surgery, we are redirecting the highest volume of blood flow in the human body.
- Temperature Control: During the procedure, surgeons often keep the operating room cooler and monitor the patient’s core temperature strictly to protect vital organs.
- Ancient Roots: While modern grafts are high-tech, the concept of vascular suturing dates back to the late 19th century, pioneered by Nobel laureate Alexis Carrel.
The Recovery Journey: What to Truly Expect
Recovery from an aortobifemoral bypass is a marathon, not a sprint. You will likely spend 4 to 7 days in the hospital. I often observe that the “hidden disadvantage” of this surgery is the abdominal discomfort. Because we must access the aorta through the abdomen, your digestive system may “go to sleep” (a condition called ileus) for a few days. The Cleveland Clinic emphasizes that managing post-operative pain and gradual reintroduction of food are key to overcoming this temporary hurdle.
- Week 1-2: Focus on light movement. Walking is your best friend, even if it’s just to the end of the hallway.
- Week 4-6: Most patients begin to feel like themselves again, but heavy lifting remains strictly off-limits.
In my opinion, the most overlooked aspect of recovery is mental health. Dealing with a major surgery and the lifestyle changes required can be taxing. Don’t underestimate the power of a support system during these weeks.
Risks, Benefits, and Alternatives
No surgery is without risk. For aortobifemoral bypass, these include infection of the graft, blood clots, and potential kidney issues. However, the alternative—leaving severe blockages untreated—often leads to critical limb ischemia, non-healing ulcers, and eventually, amputation. Research published by the Journal of Vascular Surgery indicates that for patients with extensive TASC II D lesions, the long-term limb salvage rate of surgical bypass is significantly higher than endovascular attempts.
Health Support: This high-absorption Magnesium Glycinate (200 mg) is gentle on the stomach and supports muscle relaxation, better sleep, and metabolic health. You can find this trusted formula on Amazon.
I believe the benefit of “claudication relief” (ending the pain while walking) is the most immediate reward. Patients often tell me they feel like they’ve been given new legs. But remember, the graft is a tool, not a cure. You must still manage your blood pressure and cholesterol to protect the rest of your vascular system.
Personal Recommendation from Reyus Mammadli
When considering an aortobifemoral bypass, my primary recommendation is to prioritize vascular pre-habilitation. This means working with your doctor at least 3-4 weeks before the surgery to optimize your nutrition and respiratory function. Many people focus only on the post-op, but the stronger you are going in, the faster you will recover.
Additionally, I strongly suggest a consultation regarding Endovascular-First options. While I stand by the bypass as a superior long-term solution for many, technology is advancing rapidly. In some specific cases, a hybrid approach (combining minor surgery with stenting) might offer a shorter recovery time with acceptable results. Always ask your surgeon: “Why is the open bypass better for my specific anatomy than a minimally invasive stent?”
Final Advice to the Reader: The road to vascular health is paved with daily choices. Surgery can open the pipes, but only you can keep them clean. My unique advice? Watch your hydration levels religiously post-surgery. Proper hydration keeps your blood viscosity at an optimal level, reducing the stress on your new graft and helping your kidneys process the medications used during your hospital stay. You’ve been given a second chance at mobility—walk it with pride and care.