Deep vein thrombosis (DVT) happens when a blood clot (thrombus) forms in several of the deep veins in your body, generally in your legs. Deep vein thrombosis can cause leg pain or swelling, however may occur with no symptoms. Keep reading the article for better understanding blood clots in your legs.
Deep vein thrombosis can establish if you have particular medical conditions that affect how your blood clots. Deep vein thrombosis can likewise occur if you do not move for a long time, such as after surgery, following an accident, or when you are confined to a medical facility or retirement home bed.
Deep vein thrombosis is a serious condition since blood clots in your veins can break out, travel through your blood stream and lodge in your lungs, blocking blood flow (pulmonary embolism).
Health Support: This Vitamin K2 + D3 Complex is essential for bone density, cardiovascular health, and immune function. It’s a highly-rated formula for those looking to maintain optimal nutrient levels. You can find it on Amazon.
Symptoms and signs of blood clots in legs
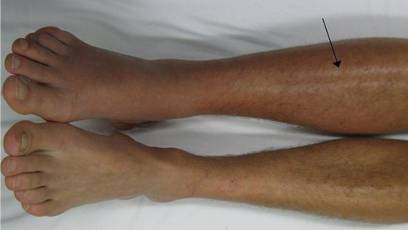
Deep vein thrombosis symptoms and signs can include:
- Swelling in the affected leg. Rarely, there might be swelling in both legs.
- Pain in your leg. The pain typically starts in your calf and can feel like cramping or a pain.
Deep vein thrombosis may often take place with no visible symptoms.
When to see a doctor
If you establish signs or symptoms of deep vein thrombosis, call your doctor for support.
Health Support: This high-absorption Magnesium Glycinate (200 mg) is gentle on the stomach and supports muscle relaxation, better sleep, and metabolic health. You can find this trusted formula on Amazon.
If you develop signs or symptoms of a pulmonary embolism– a deadly problem of deep vein thrombosis– seek medical attention right away.
The indication of a lung embolism include:
- Unusual sudden start of shortness of breath
- Chest pain or discomfort that aggravates when you take a deep breath or when you cough
- Feeling lightheaded or woozy, or fainting
- Rapid pulse
- Spending blood
Causes of blood clots in legs
Deep vein thrombosis occurs when a blood clot forms in the veins that are deep in your body, frequently in your legs. Blood clots can be caused by anything that prevents your blood from circulating normally or clotting effectively.
Complications
A concerning complication related to deep vein thrombosis is lung embolism
Lung embolism
A pulmonary embolism happens when a blood vessel in your lung becomes obstructed by a blood clot (thrombus) that takes a trip to your lungs from another part of your body, generally your leg.
A pulmonary embolism can be deadly. So, it’s crucial to be on the lookout for symptoms and signs of a lung embolism and seek medical attention if they take place. Symptoms and signs of a lung embolism include:
- Unusual abrupt onset of shortness of breath
- Chest pain or discomfort that gets worse when you take a deep breath or when you cough
- Feeling lightheaded or lightheaded, or fainting
- Quick pulse
- Spending blood
Postphlebitic syndrome
A typical issue that can occur after deep vein thrombosis is a condition called postphlebitic syndrome, also called postthrombotic syndrome. This syndrome is used to describe a collection of signs and symptoms, consisting of:
- Swelling of your legs (edema).
- Leg pain.
- Skin discoloration.
- Skin sores.
This syndrome is caused by issue to your veins from the blood clot. This damage reduces blood circulation in the affected areas. The symptoms of postphlebitic syndrome might not happen until a few years after the DVT.

Treatments for blood clots in legs
Deep vein thrombosis treatment is aimed at preventing the embolisms from getting any larger, as well as preventing the embolisms from breaking out and triggering a lung embolism. After that, the goal ends up being decreasing your chances of deep vein thrombosis happening once again.
Deep vein thrombosis treatment choices include:.
Blood thinners. Medications used to treat deep vein thrombosis include the use of anticoagulants, likewise in some cases called blood thinners, whenever possible. These are drugs that decrease your blood’s capability to embolisms. While they do not separate existing blood clots, they can avoid clots from growing or reduce your risk of establishing added embolisms.
Usually, you’ll first be given a shot or infusion of the blood thinner heparin for a few days. After starting heparin injections, your treatment might be followed by another injectable blood thinner, such as enoxaparin (Lovenox), dalteparin (Fragmin) or fondaparinux (Arixtra). Other blood thinners can be given in pill form, such as warfarin (Coumadin, Jantoven) or rivaroxaban (Xarelto). More recent blood thinners also might provide extra alternatives in the near future.
You might need to take blood thinners for three months or longer. If you’re recommended any of these blood thinners, it’s key to take your medication precisely as your doctor advises. Blood-thinning medications can have serious side effects if you take excessive or insufficient.
You might need periodic blood tests to inspect how much time it takes your blood to clot. Pregnant women should not take particular blood-thinning medications.
Clotbusters. If you have a more serious type of deep vein thrombosis or pulmonary embolism, or if other medications aren’t working, your doctor might prescribe different medications.
One group of medications is called thrombolytics. These drugs, called tissue plasminogen activators (TPA), are provided through an IV line to break up blood clots or might be provided through a catheter positioned directly into the embolisms. These drugs can cause serious bleeding and are normally used only in dangerous situations. For these factors, thrombolytic medications are only given in an extensive care ward of a hospital.
Filters. If you cannot take medicines to thin your blood, a filter might be inserted into a large vein– the vena cava– in your abdomen. A vena cava filter prevents embolisms that break out from lodging in your lungs.
Compression stockings. These help prevent swelling related to deep vein thrombosis. These stockings are endured your legs from your feet to about the level of your knees.
This pressure helps reduce the chances that your blood will pool and embolisms, according to iytmed.com. You ought to use these stockings during the day for at least 2 to 3 years if possible. Compression stockings can help avoid postphlebitic syndrome.
Lifestyle and home remedies
When you get treatment for deep vein thrombosis you have to watch your diet and try to find signs of extreme bleeding, in addition to take actions to help avoid another DVT. Some things you can do include:.
- Examine in with your doctor routinely to see if your medication or treatments need to be customized. If you’re taking warfarin (Coumadin, Jantoven), you’ll need a blood test to see how well your blood is thickening.
- Take your blood thinners as directed. If you’ve had DVT, you’ll gone on blood thinners for at least three to six months.
- Watch how much vitamin K you’re eating if you are taking warfarin. Vitamin K can impact how warfarin works. Green leafy vegetables are high in vitamin K. Check with your doctor or a dietitian about your diet if you’re taking warfarin.
- Be on the lookout for extreme bleeding, which can be a side effect of taking medications such as blood thinners. Speak with your doctor about activities that might cause you to bruise or get cut, as even a minor injury could become serious if you’re taking blood thinners.
- Move. If you’ve been on bed rest, due to the fact that of surgery or other aspects, the earlier you get moving, the less likely blood clots will establish.
- Wear compression stockings to assist avoid blood clots in the legs if your doctor suggests them.








