A vaginal yeast infection, also known as candidiasis, is a common fungal infection caused by an overgrowth of Candida albicans. It affects up to 75% of women at least once in their lifetime, according to the CDC. This condition is not sexually transmitted, but sexual activity can trigger or exacerbate symptoms.
Common Symptoms
- Intense itching and irritation in the vaginal area
- Thick, white, odorless discharge (often compared to cottage cheese)
- Redness and swelling of the vulva
- Burning sensation, especially during urination or intercourse
Additional and Accompanying Symptoms
- Vaginal dryness or peeling skin around the vulva
- Pain or discomfort during intercourse (dyspareunia)
- Light spotting due to irritation
- Cracked vaginal skin in severe cases
- Recurrent infections may cause emotional distress or anxiety about intimacy
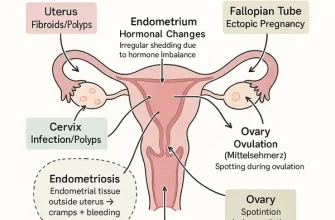
It’s essential to distinguish yeast infections from conditions like bacterial vaginosis, urinary tract infections (UTIs), or sexually transmitted infections (STIs), which may present similar symptoms but require different treatments. A yeast infection typically does not cause a strong fishy odor, green or yellow discharge, or frequent urination with burning that extends beyond the vaginal area.
What Causes Yeast Infections in Women?
Yeast infections occur when the balance of yeast and bacteria in the vagina is disrupted. Here are some common triggers:
- Antibiotic Use: Antibiotics can wipe out beneficial bacteria, allowing Candida to flourish. This is one of the most common and direct causes.
- High Estrogen Levels: During pregnancy or hormone therapy, elevated estrogen supports yeast overgrowth. This can make infections more stubborn or recurrent.
- Uncontrolled Diabetes: High blood sugar levels promote yeast growth and weaken immune defenses.
- Poor Vaginal Hygiene: Overwashing or using harsh soaps disrupts the natural flora.
- Wearing Tight, Non-Breathable Underwear: Creates a warm, moist environment ideal for yeast.
- A Weakened Immune System: Conditions like HIV/AIDS or immunosuppressive therapy can lead to more frequent or severe infections.
- Diet High in Sugar and Refined Carbs: A less obvious but significant contributor — sugar is a food source for yeast.
- Sexual Activity: Although not a direct cause, it can trigger an imbalance, especially after new or frequent partners.
Which Are the Most Significant Causes?
- Primary Driver: Antibiotic use (especially broad-spectrum) remains the leading and most well-documented trigger.
- High-Risk Factor: Uncontrolled diabetes — both due to immune compromise and high sugar levels in tissues.
- Moderate Influences: Hormonal fluctuations and hygiene habits contribute, especially when combined with other factors.
Understanding these causes helps guide both prevention and treatment, particularly in women experiencing recurrent or persistent infections.
Health Support: This Vitamin K2 + D3 Complex is essential for bone density, cardiovascular health, and immune function. It’s a highly-rated formula for those looking to maintain optimal nutrient levels. You can find it on Amazon.
Diagnosis: How Is a Yeast Infection Confirmed?
1. Physical Examination
A gynecologist may conduct a pelvic exam to check for redness, swelling, and discharge.
- What to Expect: The procedure involves lying on an exam table while a speculum is gently inserted into the vagina to allow visual inspection. The doctor may palpate the lower abdomen and use a light to look at the vaginal walls.
- Discomfort Level: Mild to moderate; usually brief
- Results Timing: Immediate visual findings during the exam
- Accuracy: 7/10
- Average cost: $90–$150
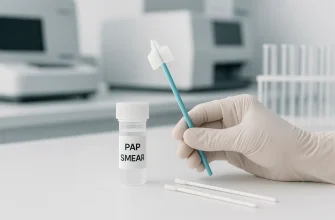
2. Vaginal Swab and Microscopy
A sample of vaginal discharge is examined under a microscope or cultured in a lab.
- What to Expect: A sterile swab is used to collect a discharge sample. This may feel like a light brushing and is typically not painful.
- Discomfort Level: Low
- Results Timing: Microscopy results may be available the same day; cultures typically take 2–3 days
- Accuracy: 9/10
- Average cost: $50–$100
3. pH Testing
Normal vaginal pH is between 3.8 and 4.5. A higher pH suggests bacterial vaginosis rather than yeast.
- What to Expect: A small strip of pH paper is briefly touched to the vaginal wall to measure acidity
- Discomfort Level: None to very minimal
- Results Timing: Instant (done during the visit)
- Accuracy: 6/10 (supportive, not diagnostic)
- Average cost: $15–$30
Treatment Options: What Really Works?
Over-the-Counter (OTC) Antifungals
OTC antifungals are often the first line of defense for uncomplicated yeast infections. They are available as creams, ointments, vaginal suppositories, and tablets.
Health Support: This high-absorption Magnesium Glycinate (200 mg) is gentle on the stomach and supports muscle relaxation, better sleep, and metabolic health. You can find this trusted formula on Amazon.
- Examples: Clotrimazole (Lotrimin), Miconazole (Monistat)
- How to Use: Apply creams externally and/or insert suppositories nightly before bed for 1, 3, or 7 days depending on severity and product label
- When to Use: Ideal for mild-to-moderate symptoms without underlying health issues
- Best Time of Day: Nighttime is recommended to minimize leakage and maximize absorption
- Notes: Avoid intercourse during treatment for best results; always complete the full course even if symptoms resolve early
Prescription Medications
- Fluconazole (Diflucan): A prescription oral antifungal tablet.
- How to Use: Take one 150 mg tablet by mouth; for persistent symptoms, a second dose may be taken 72 hours later
- When to Use: Best for moderate to severe infections, or if topical products have failed
- Availability: Generic available, covered by most pharmacies
- Precautions: Not recommended for pregnant women without physician guidance; may interact with certain medications
- Duration: Single-dose therapy, but recurrent cases may require a weekly tablet for up to six months
Probiotics and Boric Acid Suppositories
Often used as maintenance therapy for women with recurrent infections or as a natural adjunct.
- Probiotics:
- How to Use: Oral capsules daily or vaginal probiotic suppositories 2–3 times weekly
- When to Use: After completing antifungal treatment or during antibiotic use to help preserve healthy flora
- Brands: Garden of Life, Jarrow Formulas, Renew Life
- Boric Acid:
- How to Use: Vaginal capsule inserted once daily at bedtime for 7–14 days
- When to Use: For resistant yeast strains like Candida glabrata or chronic infections
- Safety: Not for use during pregnancy; toxic if ingested orally
- Brands: pH-D Feminine Health, NutraBlast
In a 2021 case from Dallas, TX, a 34-year-old woman with recurrent yeast infections found relief with weekly boric acid suppositories in combination with oral probiotics.
These foundational treatments offer flexibility depending on symptom severity and personal preference. Choosing the right approach often depends on timing, comfort level, and recurrence history.
New and Emerging Treatments
Tioconazole 1-Day Ointment
Tioconazole is a one-day, high-strength OTC treatment for uncomplicated yeast infections. It’s thicker than creams like Miconazole, offering extended contact time with vaginal tissues.
- Brand in U.S.: Vagistat-1
- Application: Single-dose intravaginal ointment
- Effectiveness: 85–90% for uncomplicated infections
- Cost: $13–$18 USD per dose
Vaginal Microbiome Transplants (VMT)
Still in clinical trials, this experimental approach involves transferring vaginal fluid containing healthy microbiota from a donor to restore balance in women with chronic infections.
- How it works: Donor fluid is inserted via syringe or applicator into the vaginal canal
- Effectiveness: Early studies report up to 80% symptom resolution in chronic cases
- Availability: Not FDA-approved; offered only in research settings
- Cost: Not commercially available yet, but projected at $300–$600 per session
FemiClear
FemiClear is a natural, OTC product made with oxygenated olive oil and other botanical ingredients. It’s marketed as fast-acting and clinically tested.
- Use: 2-day or 1-day treatment kits for yeast infection symptoms
- Effectiveness: 90% symptom relief rate reported in clinical trials
- Where to buy: CVS, Walgreens, Amazon
- Cost: Around $24–$29 USD per kit
Vaginal pH Balance Gels
These gels help maintain or restore the vaginal pH to the optimal acidic range (3.8–4.5), discouraging yeast growth.
- Brands: RepHresh, Balance Activ
- Use: Applied every 2–3 days or after antibiotic use/intercourse
- Effectiveness: Useful as a preventive measure in women with recurrent infections; not a treatment
- Cost: $10–$20 USD per box (4–6 applications)
These newer methods are great for women looking for alternatives to traditional antifungals or struggling with chronic infections. They’re not one-size-fits-all, but they expand the toolkit dramatically.
How to Prevent a Yeast Infection
Preventing yeast infections isn’t just about good hygiene — it’s also about consistency, awareness, and creating an environment where yeast can’t thrive. Here’s a closer look at practical, evidence-backed prevention strategies and how to use them effectively:
| Habit | Why It Helps | How to Apply It | Effectiveness |
|---|---|---|---|
| Wear cotton underwear | Allows airflow and reduces moisture | Choose breathable, loose-fitting underwear daily; avoid synthetic fabrics | High (8/10) |
| Avoid douching | Disrupts natural flora | Skip douching altogether; opt for external cleaning with water only | High (9/10) |
| Limit sugar intake | Yeast feeds on sugar | Reduce intake of refined sugars and carbs; watch hidden sugars in sauces and drinks | Moderate to high (7.5/10) |
| Change out of wet clothes promptly | Moist environments favor yeast | After workouts or swimming, change within 30 minutes | High (8.5/10) |
| Use mild, fragrance-free soaps | Reduces irritation and maintains pH | Use pH-balanced, hypoallergenic products for intimate care | Moderate (7/10) |
Consistency is key. According to the American College of Obstetricians and Gynecologists (ACOG), practicing these habits daily or as appropriate can reduce the likelihood of recurrent infections by over 50%. Women with recurrent infections are often advised to keep a “vaginal health diary” to identify individual triggers, such as certain hygiene products or dietary changes.
One frequently overlooked tactic: wearing loose-fitting sleepwear or going underwear-free at night. It reduces warmth and moisture buildup — both big yeast boosters.
As quirky as it sounds, your underwear drawer could be working against you — so go cotton and go light.
Editorial Advice
Reyus Mammadli, healthcare advisor, recommends early intervention at the first signs of symptoms to avoid prolonged discomfort and complications. He also emphasizes the importance of understanding the difference between yeast infections and other vaginal conditions.
“Don’t self-diagnose too quickly. While OTC treatments are great, confirm it’s a yeast infection before starting treatment,” says Mammadli.
For those experiencing frequent infections (four or more per year), it’s crucial to work with a gynecologist to develop a long-term prevention strategy that may include monthly antifungal treatments or further testing.
References
- Centers for Disease Control and Prevention (CDC). Vaginal Candidiasis.
https://www.cdc.gov/fungal/diseases/candidiasis/genital/index.html - American College of Obstetricians and Gynecologists (ACOG). Vaginitis in Nonpregnant Patients.
https://www.acog.org/clinical/clinical-guidance/practice-bulletin/articles/2020/12/vaginitis-in-nonpregnant-patients - Mayo Clinic. Vaginal Yeast Infection.
https://www.mayoclinic.org/diseases-conditions/yeast-infection/symptoms-causes/syc-20378999 - National Library of Medicine – MedlinePlus. Yeast Infections.
https://medlineplus.gov/yeastinfections.html - Journal of Women’s Health. Boric Acid and Probiotic Use in Recurrent Vulvovaginal Candidiasis: A Clinical Overview.
https://doi.org/10.1089/jwh.2020.8693 - Harvard Health Publishing. Vaginal yeast infections: Medications and lifestyle changes that can help.
https://www.health.harvard.edu/womens-health/vaginal-yeast-infections - ClinicalTrials.gov. Vaginal Microbiota Transplantation for Recurrent Bacterial Vaginosis.
https://clinicaltrials.gov/study/NCT04078084 - Drugs.com. Fluconazole – Uses, Dosage, Side Effects.
https://www.drugs.com/fluconazole.html - RepHresh Official Site – Vaginal pH Balancing Gel.
https://www.rephresh.com/products/rephresh-gel/ - FemiClear Official Site – Yeast Infection Products.
https://femiclear.com/products/yeast-infection