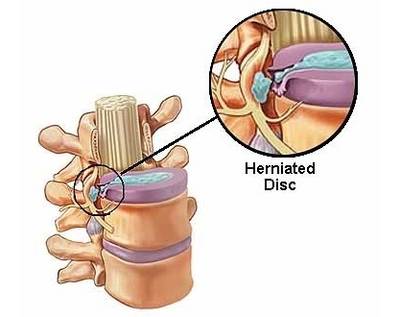
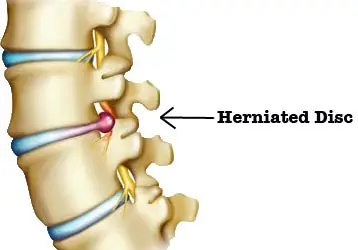
A herniated disk refers to a problem with among the rubbery cushions (disks) between the individual bones (vertebrae) that accumulate to make your spine.
A spinal disk is a little like a jelly donut, with a softer center enclosed within a harder outside. In some cases called a slipped disk or a burst disk, a herniated disk happens when a few of the softer “jelly” pushes out through a crack in the harder exterior.
A herniated disk can irritate nearby nerves and result in pain, tingling or weak point in an arm or leg. On the other hand, many individuals experience no symptoms from a herniated disk. The majority of people who have actually a herniated disk do not require surgery to correct the problem.
Health Support: This Vitamin K2 + D3 Complex is essential for bone density, cardiovascular health, and immune function. It’s a highly-rated formula for those looking to maintain optimal nutrient levels. You can find it on Amazon.
Herniated Disk Symptoms
You can have a herniated disk without understanding it – herniated disks in some cases show up on spinal images of people who have no symptoms of a disk problem. But some herniated disks can be agonizing. Most herniated disks happen in your lower back (lumbar spine), although they can likewise take place in your neck (cervical spinal column).
The most common signs and symptoms of a herniated disk are:
- Arm or leg pain. If your herniated disk remains in your lower back, you’ll generally feel the most intense pain in your butts, thigh and calf. It might also include part of the foot. If your herniated disk remains in your neck, the pain will usually be most extreme in the shoulder and arm.
- This pain may shoot into your arm or leg when you cough, sneeze or move your spine into particular positions.
- Tingling or tingling. People who have a herniated disk commonly experience pins and needles or tingling in the body part served by the afflicted nerves.
- Weakness. Muscles served by the afflicted nerves tend to weaken. This might trigger you to stumble, or harm your capability to raise or hold items.
When to see a doctor
Seek medical interest if your neck or back pain travels down your arm or leg, or if it’s accompanied by pins and needles, tingling or weakness.
Health Support: This high-absorption Magnesium Glycinate (200 mg) is gentle on the stomach and supports muscle relaxation, better sleep, and metabolic health. You can find this trusted formula on Amazon.

Causes of a herniated disk
Disk herniation is most often the outcome of a gradual, aging-related wear and tear called disk degeneration. As you age, your spinal disks lose a few of their water material. That makes them less versatile and more prone to tearing or rupturing with even a small strain or twist.
The majority of people can’t pinpoint the specific reason for their herniated disk. Often, using your back muscles instead of your leg and thigh muscles to raise large, heavy objects can result in a herniated disk, as can weaving while lifting. Hardly ever, a traumatic event such as a fall or a blow to the back can cause a herniated disk.
Risk factors
Elements that enhance your threat of a herniated disk may consist of:
- Weight. Excess body weight causes additional stress on the disks in your lower back.
- Profession. Individuals with physically demanding jobs have a higher danger of back issues. Recurring lifting, pulling, pushing, bending laterally and twisting also might enhance your threat of a herniated disk.
- Genes. Some people inherit a predisposition to establishing a herniated disk.
Complications
 Your spine does not extend into the lower part of your spinal canal. Just below your waist, the spine separates into a group of long nerve roots (cauda equina) that look like a horse’s tail. Rarely, disk herniation can compress the whole cauda equina. Emergency situation surgery may be needed to prevent irreversible weak point or paralysis.
Your spine does not extend into the lower part of your spinal canal. Just below your waist, the spine separates into a group of long nerve roots (cauda equina) that look like a horse’s tail. Rarely, disk herniation can compress the whole cauda equina. Emergency situation surgery may be needed to prevent irreversible weak point or paralysis.
Seek emergency medical interest if you have:
- Worsening symptoms. Pain, tingling or weak point may enhance to the point that you can’t perform your usual everyday activities.
- Bladder or bowel dysfunction. People who have the cauda equina syndrome may become incontinent or have trouble urinating even with a complete bladder.
- Saddle anesthesia. This progressive loss of feeling impacts the areas that would touch a saddle– the inner thighs, back of legs and the area around the anus.
Getting ready for your consultation
You’re likely to initially bring your symptoms to the interest of your family doctor. He or she may refer you to a doctor specializing in physical medication and rehabilitation, orthopedic surgery, neurology, or neurosurgery.
Exactly what you can do
Prior to your visit, write a list that responds to the following questions:
- When did you initially begin experiencing symptoms?
- Were you lifting, pressing or pulling anything at the time you initially felt symptoms? Were you twisting your back?
- Has the pain kept you from taking part in activities you wished to do?
- What, if anything, seems to enhance your symptoms?
- What, if anything, appears to intensify your symptoms?
- What medications or supplements do you take?
What to anticipate from your doctor
Your doctor might ask some of the following questions:
- Do you have any pain that takes a trip into your arms or legs?
- Do you feel any weakness or tingling in your arms or legs?
- Have you discovered any changes in your bowel or bladder routines?
- Does coughing or sneezing intensify your leg pain?
- Is the pain interfering with sleep or work?
Tests and diagnosis
Multimedia
- MRI of herniated disk MRI of herniated disk
During the physical examination, your doctor will examine your back for inflammation. He or she might ask you to lie flat and move your legs into various positions to assist identify the reason for your pain. Your doctor may also perform a neurological test, to inspect your:
- Reflexes
- Muscle strength
- Walking ability
- Capability to feel light touches, pinpricks or vibration
In many cases of herniated disk, a physical exam and a medical history are all that’s needed to make a medical diagnosis. If your doctor believes another condition or has to see which nerves are impacted, she or he may order several of the following tests
Imaging tests
- X-rays. Plain X-rays don’t find herniated disks, but they may be carried out to rule out other causes of back pain, such as an infection, tumor, back positioning problems or a broken bone.
- Computerized tomography (CT scan). A CT scanner takes a series of X-rays from many different instructions and after that integrates them to develop cross-sectional pictures of your spinal column and the structures around it.
- Magnetic resonance imaging (MRI). Radio waves and a strong magnetic field are made use of to develop pictures of your body’s internal structures. This test can be utilized to verify the location of the herniated disk and to see which nerves are impacted.
- Myelogram. A color is injected into the spine fluid, and then X-rays are taken. This test can show pressure on your spinal cord or nerves due to several herniated disks or other conditions.
- Nerve tests.
Electromyograms and nerve conduction studies determine how well electrical impulses are moving along nerve tissue. This can help identify the place of the nerve damage.

Treatments and drugs
- Multimedia
- Illustration revealing removal of herniated part of spinal disk
- Conservative treatment – primarily avoiding agonizing positions and following a planned exercise and pain-medication programs– eases symptoms in 9 from 10 individuals with a herniated disk.
Medications
- Over the counter pain medications. If your pain is mild to moderate, your doctor may tell you to take a non-prescription pain medication, such as ibuprofen (Advil, Motrin IB, others) or naproxen (Aleve, others).
- Narcotics. If your pain doesn’t enhance with over the counter medications, your doctor might recommend narcotics, such as codeine or an oxycodone-acetaminophen mix (Percocet, Oxycontin, others), for a brief time. Sedation, nausea, confusion and constipation are possible negative effects from these drugs.
- Nerve pain medications. Drugs such as gabapentin (Neurontin, Gralise, Horizant), pregabalin (Lyrica), duloxetine (Cymbalta), tramadol (Ultram) and amitriptyline commonly help relieve nerve-damage pain. Because these drugs have a milder set of side effects than do narcotic medications, they’re progressively being used as first line prescription medications for individuals who have herniated disks.
- Muscle relaxers. Muscle relaxants may be prescribed if you have muscle spasms. Sedation and lightheadedness prevail negative effects of these medications.
- Cortisone injections. Inflammation-suppressing corticosteroids may be given by injection directly into the area around the spine nerves. Spine imaging can assist guide the needle more securely. Occasionally a course of oral steroids might be attempted to lower swelling and inflammation.
Therapy
Physical therapists can show you positions and exercises designed to reduce the pain of a herniated disk. A physical therapist may likewise advise:
- Heat or ice
- Traction
- Ultrasound
- Electrical stimulation
- Short-term bracing for the neck or lower back
Surgery solution for herniated disk
A very small number of individuals with herniated disks ultimately need surgery. Your doctor might suggest surgery if conservative treatments fail to enhance your symptoms after six weeks, especially if you continue to experience:
- Tingling or weak point
- Trouble standing or walking
- Loss of bladder or bowel control
In a lot of cases, cosmetic surgeons can get rid of just the extending part of the disk. Hardly ever, however, the whole disk has to be eliminated. In these cases, the vertebrae may need to be merged together with metal hardware to supply spinal stability. Hardly ever, your surgeon might suggest the implantation of a synthetic disk.
Way of life and home treatments
- Take painkiller. Over the counter medications – such as ibuprofen (Advil, Motrin IB, others) or naproxen (Aleve, others) – might help in reducing the pain connected with a herniated disk.
- Use heat or cold. At first, cold packs can be made use of to ease pain and inflammation. After a few days, you might switch to gentle heat to give relief and comfort.
- Avoid overwhelming bed rest. Overwhelming bed rest can result in stiff joints and weak muscles – which can complicate your recovery. Instead, rest in a position of comfort for 30 minutes, then opt for a short walk or do some work. Try to avoid activities that aggravate your pain throughout the recovery process.
Herniated Disk Prevention
To help avoid a herniated disk:
- Workout. Reinforcing the trunk muscles helps stabilize and support the spinal column.
- Maintain excellent posture. Excellent posture reduces the pressure on your spine and disks. Keep your back straight and aligned, especially when sitting for long periods. Lift heavy things appropriately, making your legs – not your back – do the majority of the work.
- Keep a healthy weight. Excess weight puts more pressure on the spinal column and disks, making them more vulnerable to herniation.