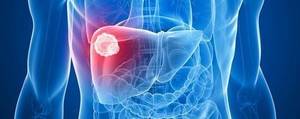
A benign tumor called a hepatic hemangioma may develop on the liver. It’s regarded as one of the most prevalent kinds of liver tumors. Liver hemangioma is frequently found by accident during an ultrasound or CT scan, and it seldom causes any symptoms.
A non-cancerous growth of the liver is called a hepatic hemangioma. It is made up of a collection of blood-filled blood vessels. Although the size and quantity of these tumors might vary, their diameter usually ranges from a few millimeters to several centimeters. Liver hemangiomas are more common in middle-aged women who have had estrogen treatment.
Liver Hemangioma Types
Liver hemangiomas are considered the most common type of liver mass and are typically asymptomatic, often discovered incidentally during imaging tests for other conditions. There are few types that vary based on their physical characteristics and imaging findings:
Capillary Hemangioma:
Health Support: This Vitamin K2 + D3 Complex is essential for bone density, cardiovascular health, and immune function. It’s a highly-rated formula for those looking to maintain optimal nutrient levels. You can find it on Amazon.
- This is the most common subtype.
- Composed of small capillaries.
- Usually small in size and less likely to cause symptoms.
Cavernous Hemangioma:
- Made of larger, blood-filled vascular spaces.
- They can grow to a significant size, occasionally causing symptoms due to mass effect on adjacent structures.
- Sometimes, they require monitoring or treatment if symptomatic.
Giant Hemangioma:
- These are larger versions of cavernous hemangiomas, typically greater than 4-5 cm in diameter.
- Have a higher propensity to cause symptoms due to their size.
- There is a slight increase in the risk of complications, such as rupture or intralesional bleeding.
Flash-Filling Hemangioma:
- Characterized by rapid contrast enhancement during imaging.
- They fill in more quickly than typical cavernous hemangiomas.
- Can sometimes be mistaken for malignant lesions on certain imaging modalities.
Pedunculated Hemangioma:
Health Support: This high-absorption Magnesium Glycinate (200 mg) is gentle on the stomach and supports muscle relaxation, better sleep, and metabolic health. You can find this trusted formula on Amazon.
- A pedunculated hemangioma is attached to the liver surface by a stalk.
- They can be mistaken for other abdominal masses when they extend beyond the liver’s edge.
- These can be particularly challenging to diagnose due to atypical appearance.
Sclerosed / Hyalinized Hemangioma:
- These hemangiomas have undergone degenerative changes, often appearing as scar-like tissue.
- Less vascular than other types and may exhibit calcifications.
- Less characteristic appearance on imaging, which can make them appear similar to more worrying lesions.
Atypical Hemangioma:
- Exhibits non-classic imaging features.
- Can be difficult to distinguish from malignant liver lesions without further testing, such as MRI with contrast or biopsy.
For most patients with liver hemangiomas, no treatment is necessary unless symptoms arise or there is uncertainty about the diagnosis. Regular monitoring may be recommended, especially for the larger or atypical variants. It’s essential to consult with health care professionals when managing liver hemangiomas to ensure proper diagnosis and care.
Liver Hemangioma Causes
It is unknown what specifically causes hepatic hemangiomas. Nonetheless, scientists think that a few elements, including heredity, could contribute to the illness’s onset.
It is thought that blood vessels that grow in the liver during fetal development are the source of hepatic hemangiomas. The tumor forms as a result of these blood vessels’ improper operation. Hemangiomas in the liver, however, do not seem to run in families and are not usually present at birth.
According to some research, female hormones may potentially have a role in the development of hepatic hemangiomas. Liver hemangiomas are more common in women than in males. Additionally, when hormone levels are high during pregnancy and fall after delivery, liver hemangiomas have a tendency to proliferate.
Taking birth control pills or hormone replacement therapy, having a history of pregnancy-related problems, and having a history of liver illness are other variables that may raise the chance of developing hepatic hemangiomas. But it’s crucial to remember that hepatic hemangiomas often occur spontaneously and may not even be linked to any risk factors.
Hemangioma in the Liver Symptoms
Liver hemangiomas may have no symptoms at all. Indeed, unless their liver hemangioma is detected by medical tests or imaging scans performed for other purposes, the majority of individuals with this problem are entirely ignorant of their hepatic hemangioma.
Liver hemangiomas may, however, sometimes result in symptoms. These might consist of:
- stomach ache, which might be really painful
- vomiting and nausea
- appetite decrease combined with weight loss
- abdominal distension or swelling
- Weakness and exhaustion
Liver hemangiomas may sometimes burst or bleed, resulting in abrupt, excruciating stomach pain, vomiting, and shock. This is an emergency that has to be treated right away by medical professionals.
Because the symptoms of liver hemangiomas and other liver disorders sometimes overlap, it is important to remember that liver hemangiomas are frequently misdiagnosed as liver cysts, liver tumors, or liver abscesses. Therefore, if you have a family history of liver illness or encounter any persistent symptoms, you should definitely see a doctor.
Liver hemangioma: is it dangerous?
Liver hemangiomas are liver-specific blood vessel tumors that are not malignant. Some instances may be harmful, although they are usually innocuous and seldom show any symptoms. It’s critical to comprehend the possible dangers and issues associated with hepatic hemangiomas.
The first thing to note is that liver hemangiomas often do not create any discernible symptoms. They may, however, in rare instances result in symptoms including nausea, vomiting, lack of appetite, weight loss, and stomach pain.
Rarely, hepatic hemangiomas may burst or bleed, sending patients into shock, experiencing excruciating stomach pain, and vomiting. This has to be treated medically right away since it might be fatal.
Furthermore, liver hemangiomas have the potential to enlarge to the point where they impair the liver’s regular function. Complications include portal hypertension, liver failure, and hepatic dysfunction may result from this.
Consequently, it’s critical to closely monitor hepatic hemangiomas to make sure problems don’t arise. To track the size and progress of the hemangioma, doctors may advise routine imaging tests like magnetic resonance imaging (MRI), computed tomography (CT) scans, or ultrasounds.
How to Diagnose Liver Hemangioma
Making the diagnosis of hepatic hemangiomas is essential to guaranteeing their early identification and appropriate treatment. Various diagnostic methods may be used by doctors, depending on the symptoms and presentation of the patient.
Diagnostic imaging techniques including CT, MRI, and ultrasounds are the most often utilized methods to find hepatic hemangiomas. The doctor can see the liver’s blood vessels and any unusual growths, including hemangiomas, thanks to these tests.
In order to assess the extent of the problem, the doctor may also suggest further testing if a liver hemangioma is found. Blood testing may assist in determining if the hemangioma is connected to any bleeding issues or liver failure.
In rare instances, a biopsy can be necessary to provide conclusive evidence of the diagnosis. This entails taking a little sample of liver tissue, which is then inspected under a microscope to check for aberrant blood vessels or cells.
Treatment for the Liver Hemangioma
The doctor’s treatment strategy for hepatic hemangiomas will be determined by the growth’s size, location, and accompanying symptoms. Because hepatic hemangiomas are often benign and asymptomatic, therapy is not necessary in the majority of instances. However, therapy could be required for more substantial hemangiomas or those that are uncomfortable.
The three main treatments for hepatic hemangiomas are medication, surgery, and monitoring. Periodic monitoring is frequently the sole advised line of therapy for tiny, asymptomatic hemangiomas. This is due to the fact that hepatic hemangiomas often do not expand or result in problems. However, the doctor could advise further therapy if the hemangioma starts to alter in size or form or if symptoms appear.
Medication may be recommended in some circumstances to assist control the symptoms brought on by hepatic hemangiomas. For instance, a doctor can provide painkillers to deal with any discomfort a hemangioma may cause.
Surgery could be suggested if the hepatic hemangioma is bigger or producing serious symptoms. Partial hepatectomy, which entails removing the portion of the liver containing the hemangioma, is the most popular surgical technique. Minimally invasive techniques like embolization or ablation could be advised in certain circumstances.
Prevention
Since hepatic hemangiomas occur spontaneously and lack a known cause, prevention is often not an option. To lower the chance of difficulties or future growth, there are a few actions that may be performed. Maintaining a healthy lifestyle is advised, which includes abstaining from alcohol and tobacco, exercising often, and eating a balanced diet.
Additionally, routine examinations are crucial, particularly for those with a family history of hemangiomas or liver illness. Ultrasounds and CT scans are two imaging techniques that may identify any abnormal growths in the liver early. Timely care after early discovery may help avoid further problems and the need for lengthy therapy.
It is important to remember that most people with hepatic hemangiomas do not have any symptoms or consequences, and the disease is often benign. However, if symptoms like pain, nausea, or discomfort in the abdomen appear, it is imperative that you see a doctor. Liver hemangiomas have the potential to burst in extreme situations, which might result in bleeding or other problems that need medical care.
FAQ
Q: What is good for liver hemangioma?
A: There is no specific medication or treatment that can cure liver hemangioma. However, doctors may recommend regular monitoring to ensure the tumor is not growing and causing any complications.
Q: Can you live a normal life with liver hemangioma?
A: Yes, in most cases, liver hemangiomas are benign and do not cause any symptoms or health problems. Many people live their entire lives without ever knowing they have a liver hemangioma.
Q: Can you exercise with a liver hemangioma?
A: Yes, exercise is generally safe for people with liver hemangioma. However, it is important to consult with a doctor to ensure that there are no restrictions or limitations.
Q: Do liver hemangiomas ever go away?
A: Liver hemangiomas typically do not go away on their own. However, they may stop growing or even shrink over time.
Q: How do you stop a liver hemangioma from growing?
A: There is no guaranteed way to stop a liver hemangioma from growing. However, regular monitoring and imaging can help detect any changes in size or behavior, which can then be addressed with appropriate medical management.
Q: What size liver hemangioma needs surgery?
A: In general, liver hemangiomas that are larger than 2″ (5 cm) in diameter or causing symptoms may need to be surgically removed.
Q: How big can a liver hemangioma grow?
A: Liver hemangiomas can vary significantly in size, from just a few millimeters to several centimeters in diameter. While larger hemangiomas may pose a greater risk of complications, the size of the tumor alone is not always a reliable indicator of its severity or impact on overall health.
Interesting fact: the largest liver hemangioma
Surgeons have encountered some of the most significant liver hemangiomas, with the largest recorded cases presenting remarkable challenges for surgical intervention. A notable instance involves a massive liver hemangioma, which reached an extraordinary size of 11″ x 8.6″ (28 cm by 22 cm), located in the patient’s right hepatic lobe. This voluminous mass necessitated a right hepatectomy, showcasing not only the potential enormity of such lesions but also the surgical expertise required to successfully treat them.
The continuous growth of this hemangioma was documented through radiological records, expanding from a diameter of 5″ (13 cm) in 2015 to ~10″ (25 cm) in 2018. Surgical and medical teams dedicating their expertise to these cases do so with the understanding that such procedures are essential for alleviating the patient’s symptoms and complications associated with these gigantic growths.