Mammography is a specific type of breast imaging that uses low-dose x-rays to identify cancer early – prior to women experience symptoms – when it is most treatable.
Inform your doctor about any breast symptoms or issues, prior surgeries, hormone use, whether you have a household or personal history of breast cancer, and if there’s a possibility you are pregnant. If possible, acquire copies of your previous mammograms and make them readily available to your radiologist on the day of your exam. Leave jewelry at home and use loose, comfortable clothes. You might be asked to use a gown. Do not use deodorant, talc or cream under your arms or on your breasts as these might appear on the mammogram and hinder correct medical diagnosis.
What is Mammography?
Mammography is specialized medical imaging that uses a low-dose x-ray system to see inside the breasts. A mammography test, called a mammogram, helps in the early detection and medical diagnosis of breast diseases in women.
Health Support: This Vitamin K2 + D3 Complex is essential for bone density, cardiovascular health, and immune function. It’s a highly-rated formula for those looking to maintain optimal nutrient levels. You can find it on Amazon.
An x-ray (radiograph) is a noninvasive medical test that helps doctors detect and treat medical conditions. Imaging with x-rays involves exposing a part of the body to a small dosage of ionizing radiation to produce photos of the within the body. X-rays are the oldest and most often used kind of medical imaging.
3 recent advances in mammography include digital mammography, computer-aided detection and breast tomosynthesis.
Digital mammography, also called full-field digital mammography (FFDM), is a mammography system where the x-ray film is replaced by electronic devices that transform x-rays into mammographic pictures of the breast. These systems resemble those discovered in digital electronic cameras and their effectiveness allows much better pictures with a lower radiation dose. These pictures of the breast are moved to a computer for evaluation by the radiologist and for long term storage. The patient’s experience during a digital mammogram is similar to having a traditional movie mammogram.
Computer-aided detection (CAD) systems search digitized mammographic images for abnormal areas of density, mass, or calcification that may indicate the existence of cancer. The CAD system highlights these areas on the images, signaling the radiologist to thoroughly assess this area.
Health Support: This high-absorption Magnesium Glycinate (200 mg) is gentle on the stomach and supports muscle relaxation, better sleep, and metabolic health. You can find this trusted formula on Amazon.
Breast tomosynthesis, likewise called three-dimensional (3-D) mammography and digital breast tomosynthesis (DBT), is an advanced form of breast imaging where numerous images of the breast from different angles are recorded and reconstructed (” manufactured”) into a three-dimensional image set. In this way, 3-D breast imaging resembles computed tomography (CT) imaging where a series of thin “pieces” are assembled together to produce a 3-D reconstruction of the body.
Although the radiation dose for some breast tomosynthesis systems is slightly greater than the dose used in basic mammography, it remains within the FDA-approved safe levels for radiation from mammograms. Some systems have doses really similar to traditional mammography.
Large population research studies have actually revealed that screening with breast tomosynthesis results in enhanced breast cancer detection rates and less “call-backs,” instances where women are recalled from evaluating for additional testing because of a possibly unusual finding.
Breast tomosynthesis might also result in:
- earlier detection of small breast cancers that might be concealed on a standard mammogram
- higher accuracy in identifying the size, shape and place of breast problems
- less unnecessary biopsies or extra tests
- greater possibility of discovering numerous breast tumors
- clearer pictures of irregularities within thick breast tissue
What Are Some Common Uses of the Procedure?
Mammograms are used as a screening tool to spot early breast cancer in women experiencing no symptoms. They can also be used to detect and identify breast disease in women experiencing symptoms such as a lump, pain, skin dimpling or nipple discharge.
Screening Mammography
Mammography plays a main part in early detection of breast cancers because it can show changes in the breast as much as two years prior to a patient or physician can feel them. Present standards from the U.S. Department of Health and Human Services (HHS) and the American College of Radiology (ACR) advise screening mammography every year for women, starting at age 40. Research has actually shown that annual mammograms result in early detection of breast cancers, when they are most curable and breast-conservation therapies are available.
The National Cancer Institute (NCI) adds that women who have had breast cancer, and those who are at increased risk due to a household history of breast or ovarian cancer, need to seek skilled medical guidance about whether they ought to begin evaluating before age 40 and the need for other types of screening. If you are at high risk for breast cancer, you might need to obtain a breast MRI in addition to your annual mammogram.
Diagnostic Mammography
Diagnostic mammography is used to evaluate a patient with unusual scientific findings – such as a breast lump or nipple discharge – that have actually been discovered by the lady or her doctor. Diagnostic mammography might also be done after an abnormal screening mammogram in order to evaluate the area of concern on the screening examination.
How should I prepare?
Prior to arranging a mammogram, the American Cancer Society (ACS) and other specialized organizations recommend that you talk about any brand-new findings or problems in your breasts with your doctor. In addition, notify your doctor of any prior surgical treatments, hormone use, and household or personal history of breast cancer.
Do not arrange your mammogram for the week prior to your menstrual duration if your breasts are usually tender during this time. The best time for a mammogram is one week following your period. Always inform your doctor or x-ray technologist if there is any possibility that you are pregnant.
The ACS likewise recommends you:
- Do not wear deodorant, talc or lotion under your arms or on your breasts on the day of the exam. These can appear on the mammogram as calcium spots.
- Explain any breast symptoms or problems to the technologist performing the examination.
- Get your previous mammograms and make them available to the radiologist if they were done at a various area.
- This is required for contrast with your existing exam and can typically be acquired on a CD.
- Ask when your outcomes will be available; do not assume the outcomes are normal if you do not speak with your doctor or the mammography facility.
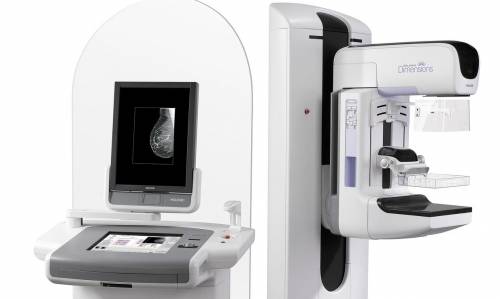
What Does a Mammography Equipment Look Like?
A mammography system is a rectangular box that houses the tube where x-rays are produced. The unit is used exclusively for x-ray exams of the breast, with unique devices that allow just the breast to be exposed to the x-rays. Attached to the unit is a device that holds and compresses the breast and positions it so images can be acquired at different angles.
Breast tomosynthesis is carried out using digital mammography units, but not all digital mammography devices are equipped to perform tomosynthesis imaging.
How Does the Procedure Work?
X-rays are a type of radiation like light or radio waves. X-rays travel through many items, including the body. Once it is thoroughly targeted at the part of the body being analyzed, an x-ray maker produces a little burst of radiation that passes through the body, recording an image on photographic film or a special detector.
Various parts of the body take in the x-rays in varying degrees. Dense bone absorbs much of the radiation while soft tissue, such as muscle, fat and organs, enable more of the x-rays to travel through them. As an outcome, bones appear white on the x-ray, soft tissue appears in shades of gray and air appears black.
Until recently, x-ray images were kept on large movie sheets (much like a big photographic negative). Today, most images are digital files that are saved digitally. These stored images are quickly accessible and are regularly compared with current x-ray images for diagnosis and disease management.
In standard film and digital mammography, a stationery x-ray tube captures an image from the side and an image from above the compressed breast. In breast tomosynthesis, the x-ray tube moves in an arc over the breast, recording several images from different angles.
How Is the Procedure Performed?
Mammography is carried out on an outpatient basis.
During mammography, a specially certified radiologic technologist will position your breast in the mammography unit. Your breast will be put on an unique platform and compressed with a clear plastic paddle. The technologist will gradually compress your breast.
Breast compression is essential in order to:
- Level the breast thickness so that all of the tissue can be visualized.
- Spread out the tissue so that small problems are less likely to be hidden by overlying breast tissue.
- Enable the use of a lower x-ray dose considering that a thinner quantity of breast tissue is being imaged.
- Hold the breast still in order to reduce blurring of the image caused by motion.
- Minimize x-ray scatter to increase sharpness of photo.
You will be asked to alter positions between images. The regular views are a top-to-bottom view and an angled side view. The process will be duplicated for the other breast. Compression is still needed for tomosynthesis imaging in order to lessen motion, which deteriorates the images. During screening breast tomosynthesis, two-dimensional images are also obtained or created from the synthesized 3-D images.
You must hold really still and may be asked to keep from breathing for a few seconds while the x-ray picture is required to reduce the possibility of a blurred image. The technologist will walk behind a wall or into the next room to trigger the x-ray maker.
When the assessment is complete, you may be asked to wait until the radiologist figures out that the necessary images have actually been obtained.
The examination procedure should take about 30 minutes.
What Does Mammography Procedure Feel Like?
You will feel pressure on your breast as it is squeezed by the compression paddle. Some women with delicate breasts may experience discomfort. If this is the case, schedule the procedure when your breasts are least tender. Make certain to inform the technologist if pain happens as compression is increased. If pain is considerable, less compression will be used. Always keep in mind compression permits better quality mammograms.
Who Interprets the Results and How Do I Get Them?
A radiologist, a physician specifically trained to supervise and interpret radiology examinations, will examine the images and send a signed report to your primary care or referring physician, who will go over the results with you.
You will also be notified of the results by the mammography facility.
Follow-up examinations may be needed. Your doctor will discuss the precise reason another examination is asked for. Sometimes a follow-up exam is done because a potential problem requires more assessment with extra views or a special imaging strategy. A follow-up examination may likewise be required so that any modification in a known abnormality can be monitored in time. Follow-up examinations are in some cases the best method to see if treatment is working or if a finding is steady or altered in time.
Benefits and Side Effects of Mammography
Benefits
- Imaging of the breast enhances a physician’s ability to identify little tumors. When cancers are little, the lady has more treatment alternatives.
- Making use of evaluating mammography increases the detection of little irregular tissue developments confined to the milk ducts in the breast, called ductal carcinoma in situ (DCIS). These early tumors can not hurt patients if they are eliminated at this stage and mammography is an exceptional way to find these tumors. It is likewise useful for finding all types of breast cancer, consisting of invasive ductal and invasive lobular cancer.
- No radiation stays in a patient’s body after an x-ray evaluation.
- X-rays generally have no side effects in the common diagnostic variety for this examination.
Side Effects and Risks
- There is constantly a minor possibility of cancer from excessive exposure to radiation. However, the advantage of an accurate diagnosis far surpasses the risk.
- The effective radiation dosage for this procedure varies. See the Safety page to find out more about radiation dose.
- Incorrect Positive Mammograms. 5 percent to 15 percent of screening mammograms need more testing such as extra mammograms or ultrasound. Most of these tests turn out to be normal. If there is an irregular finding, a follow-up or biopsy might need to be performed. Most of the biopsies verify that no cancer existed. It is approximated that a woman who has annual mammograms in between ages 40 and 49 has about a 30 percent possibility of having a false-positive mammogram at some point in that years and about a 7 percent to 8 percent opportunity of having a breast biopsy within the 10-year duration.
- Women need to constantly notify their doctor or x-ray technologist if there is any possibility that they are pregnant. See the Safety page for more information about pregnancy and x-rays.
How to Minimize Radiation Exposure
Special care is taken during x-ray assessments to use the most affordable radiation dose possible while producing the best images for examination. National and international radiology defense companies constantly evaluate and update the technique requirements used by radiology experts.
Modern x-ray systems have really regulated x-ray beams and dose control methods to minimize stray (scatter) radiation. This guarantees that those parts of a patient’s body not being imaged receive very little radiation exposure.
What Are the Limitations of Mammography?
Initial mammographic images themselves are not typically adequate to figure out the existence of a benign or deadly disease with certainty. If a finding or spot seems suspicious, your radiologist might advise additional diagnostic research studies.
Analyses of mammograms can be tough due to the fact that a normal breast looks different for each woman. Also, the look of an image may be jeopardized if there is powder or salve on the breasts or if you have gone through breast surgery. Because some breast cancers are difficult to envision, a radiologist might want to compare the image to views from previous examinations. It is very important to recognize that not all breast cancers can be seen on mammography.
Increased breast density has attracted attention from a variety of state legislatures for numerous reasons, including:
- Increased breast density makes it tough to see a cancer on mammography.
- Increased breast density may increase the risk of getting breast cancer.
The radiologist reading your mammogram determines your breast density and reports it to your doctor. Some states also require the center to inform you if you have thick breasts.
Breast augmentation can likewise hamper precise mammogram readings since both silicone and saline implants are not transparent on x-rays and can obstruct a clear view of the tissues behind them, particularly if the implant has actually been put in front of, instead of beneath, the chest muscles. Experienced technologists and radiologists know how to carefully compress the breasts to improve the view without rupturing the implant.
When making an appointment for a mammogram, women with implants need to ask if the facility uses special strategies designed to accommodate them. Prior to the mammogram is taken, they must make certain the technologist is experienced in carrying out mammography on patients with breast augmentation.
While mammography is the best screening tool for breast cancer offered today, mammograms do not detect all breast cancers. This is called an incorrect unfavorable outcome. On the other hand, when a mammogram looks abnormal and no cancer exists, this is called a false-positive result.
Research is being done on a range of breast imaging techniques that can contribute to the early detection of breast cancer and improve the accuracy in differentiating non-cancerous breast conditions from breast cancers.