These subtypes of breast cancer are normally diagnosed based upon the presence, or absence of, three “receptors” known to sustain most breast cancers: estrogen receptors, progesterone receptors and human epidermal development factor receptor 2 (HER2). The most successful treatments for breast cancer target these receptors.
Regrettably, none of these receptors are found in women with triple negative breast cancer. Simply puts, a triple unfavorable breast cancer diagnosis means that the offending growth is estrogen receptor-negative, progesterone receptor-negative and HER2-negative, thus triggering the name “triple unfavorable breast cancer.” On a favorable note, this type of breast cancer is typically responsive to chemotherapy. Because of its triple negative status, nevertheless, triple negative growths typically do not react to receptor targeted treatments. Depending on the stage of its diagnosis, triple unfavorable breast cancer can be particularly aggressive, and more likely to recur than other subtypes of breast cancer.
Triple-negative Breast Cancer Symptoms
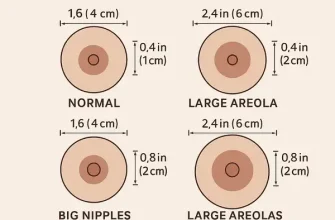
Although triple-negative breast cancer does not look different from other breast cancer, it has a number of distinct characteristics, consisting of:
- Receptor status: Tests that discover receptors for estrogen, progesterone and HER2 will be unfavorable, which implies hormone therapy, a standard breast cancer treatment, is ineffective. Rather, triple-negative breast cancer treatment alternatives consist of chemotherapy, targeted therapy and radiation.
- More aggressive: A greater tendency to spread out and recur after treatment compared to other breast cancer types. This risk reduces after the first couple of years following therapy.
- Cell type and grade: Triple-negative breast cancer cells tend to be “basal-like,” meaning that they look like the basal cells lining the breast ducts. The cells might likewise be greater grade, which means that they not resemble normal, healthy cells.
Stages of Triple Negative Breast Cancer
The stages of triple negative breast cancer are based on the size and area of the growth, in addition to whether the cancer has spread out beyond the part of the breast in which it came from. To stage cancer, physicians use a scale of Stage 0 to Stage 4.
Health Support: This Vitamin K2 + D3 Complex is essential for bone density, cardiovascular health, and immune function. It’s a highly-rated formula for those looking to maintain optimal nutrient levels. You can find it on Amazon.
Stage 0 breast cancers are isolated in one part of the breast, such as duct or lobule, and show no sign of spreading into other tissue. Stage 1 triple negative breast cancer likewise often means that the cancer hasn’t spread beyond the breast. Stage 1 is normally localized, although further local spread may cause the cancer to move into stage 2.
In stage 3, the cancer has attacked the body’s lymph system. Stage 4 cancer is the most serious. Stage 4 cancer has actually spread beyond the breast and nearby lymph nodes, and into other organs and tissue of the body.
In addition to stages, breast cancers are provided grades based on the size, shape, and activity of the cells in the tumor. A higher-grade cancer implies a higher percentage of cells look and act unhealthy, or they no longer resemble normal, healthy cells. On a scale of one to 3, with the three being the most severe condition, TNBC is typically identified Grade 3.
Triple Negative Breast Cancer Survival Rate
If you’ve been identified with triple negative breast cancer (TNBC), you might wonder how your diagnosis will impact your life. Some concerns you might have are:
Health Support: This high-absorption Magnesium Glycinate (200 mg) is gentle on the stomach and supports muscle relaxation, better sleep, and metabolic health. You can find this trusted formula on Amazon.
- What is triple unfavorable breast cancer?
- Is it treatable?
- What will treatment be like?
- What’s my long-lasting outlook?
The answer to those and other questions you have will depend upon a great deal of factors, such as the stage of your cancer and how well you react to treatment. Keep checking out for more information about TNBC and your outlook.
Facts About Triple Negative Breast Cancer
- About 15-20 percent of people with breast cancer have triple negative breast cancer (TNBC).
- TNBC is often more aggressive than other types of cancers. That can make treatment more difficult.
- Hormone therapy isn’t normally an effective treatment for TNBC. Instead, treatment often involves chemotherapy, radiation, and surgery.
Life Expectancy
The outlook for breast cancer is frequently explained in terms of five-year survival rates. This survival rate represents the portion of people who are still alive a minimum of 5 years after their medical diagnosis. Five-year survival rates have the tendency to be lower for triple negative breast cancer (TNBC) than for other forms of breast cancer.
A 2007 study of more than 50,000 women with all stages of breast cancer discovered that 77 percent of women with TNBC survived at least 5 years. Ninety-three percent of women with other types of breast cancer were found to endure a minimum of 5 years. A 2009 study, nevertheless, found that the five-year survival rate for women with TNBC resembled the survival rates for women with other cancers of similar stages. The 2009 research study only consisted of 296 women, so the research study size was a lot smaller than the 2007 study hall.
A separate research study released in 2007 found that after 5 years of their diagnosis, women with TNBC not had a greater risk of death.
These survival rates should not be used to anticipate your outlook. Your doctor will be able to provide you a more exact outlook based on the stage of your TNBC, your age, and your total health. How well you react to treatment will also determine your outlook.
Treatment for Triple-Negative Breast Cancer
Triple-negative breast cancer is generally treated with a mix of treatments such as surgery, radiation therapy, and chemotherapy. Numerous women are stressed when they find out that extra treatments such as hormone therapy and Herceptin aren’t most likely to treat triple-negative breast cancer. But new treatments are being studied, and there is motivating news about chemotherapy for triple-negative breast cancer.
Some research has shown that hormone-receptor-negative breast cancers – which triple-negative breast cancers are – in fact respond much better to chemotherapy than breast cancers that are hormone-receptor-positive. If you follow the treatment plan that makes one of the most sense for your specific scenario, while doing your best to make healthy lifestyle options such as eating a healthy low-fat diet, exercising routinely, and quitting alcohol, you’re doing everything you can to treat the cancer.
You likewise may wonder whether you should have more aggressive treatment, such as mastectomy rather than lumpectomy, or more chemotherapy treatments or higher dosages of chemotherapy. It’s logical to assume that, given that triple-negative breast cancer has the tendency to be more aggressive, it should get more aggressive treatment. At this time, nevertheless, there is no standard recommendation that people with triple-negative breast cancer ought to have more treatment.
Some studies have looked at whether offering chemotherapy before surgery – called neoadjuvant therapy – might be a good choice for women with triple-negative breast cancer. A little research study of women with locally advanced triple-negative breast cancer discovered that for two-thirds of them, chemotherapy medications provided before surgery resulted in no living cancer cells in the tumor when it was gotten rid of. Another study, released in 2008 by researchers at M.D. Anderson Cancer Center, found that chemotherapy before surgery benefited some women with triple-negative breast cancer, causing all proof of disease to disappear. For these women, survival rates resembled those of women with breast cancer that was not triple-negative. Another 2007 research study of more than 100 women found that neoadjuvant chemotherapy did benefit some individuals with hormone-receptor-negative and triple-negative breast cancer. These women had a total reaction to chemotherapy (no evidence of disease) and after that went on to have surgery. More research study on neoadjuvant chemotherapy for triple-negative breast cancer is needed.
Due to the fact that doctors are still establishing their understanding of triple-negative breast cancer, they might differ in their treatment suggestions. You might discover it useful to get a few various viewpoints.