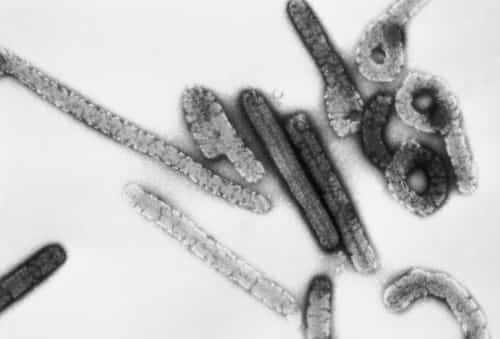
Marburg hemorrhagic fever (Marburg virus) is a rare, severe type of hemorrhagic fever which impacts both humans and non-human primates. Triggered by a genetically special zoonotic (that is, animal-borne) RNA virus of the filovirus family, its recognition led to the development of this virus family. The four species of Ebola virus are the just other known members of the filovirus family.
Marburg virus was first acknowledged in 1967, when outbreaks of hemorrhagic fever occurred simultaneously in laboratories in Marburg and Frankfurt, Germany and in Belgrade, Yugoslavia (now Serbia). A total of 37 people ended up being ill; they consisted of lab employees along with several medical personnel and relative who had cared for them. The first people infected had been exposed to African green monkeys or their tissues. In Marburg, the monkeys had actually been imported for research study and to prepare polio vaccine.
Where Does Marburg Hemorrhagic Fever Occur?
Taped cases of the disease are unusual, and have actually appeared in just a few locations. While the 1967 break out happened in Europe, the disease representative had gotten here with imported monkeys from Uganda. No other case was taped up until 1975, when a traveler most likely exposed in Zimbabwe ended up being ill in Johannesburg, South Africa – and passed the virus to his travelling companion and a nurse. 1980 saw two other cases, one in Western Kenya not far from the Ugandan source of the monkeys linked in the 1967 break out. This patient’s participating in physician in Nairobi ended up being the second case. Another human Marburg infection was recognized in 1987 when a young man who had taken a trip extensively in Kenya, including western Kenya, became ill and later on died.
Health Support: This Vitamin K2 + D3 Complex is essential for bone density, cardiovascular health, and immune function. It’s a highly-rated formula for those looking to maintain optimal nutrient levels. You can find it on Amazon.
Transmission
Simply how the animal host first sends Marburg virus to people is unknown. Nevertheless, just like some other viruses which cause viral hemorrhagic fever, human beings who end up being ill with Marburg hemorrhagic fever may spread the virus to other individuals. This may occur in several ways. Individuals dealing with infected monkeys who enter into direct contact with them or their fluids or cell cultures, have actually ended up being infected. Spread of the virus between human beings has actually taken place in a setting of close contact, often in a hospital. Beads of body fluids, or direct contact with persons, devices, or other objects infected with contagious blood or tissues are all extremely suspect as sources of disease.
Symptoms of Marburg Hemorrhagic Fever
After an incubation period of 5-10 days, the beginning of the disease is unexpected and is marked by fever, chills, headache, and myalgia. Around the 5th day after the start of symptoms, a maculopapular rash, most prominent on the trunk (chest, back, stomach), might take place. Nausea, vomiting, chest pain, a sore throat, abdominal pain, and diarrhea then might appear. Symptoms become increasingly severe and might include jaundice, inflammation of the pancreas, severe weight-loss, delirium, shock, liver failure, huge hemorrhaging, and multi-organ dysfunction.
Due to the fact that a lot of the symptoms and signs of Marburg hemorrhagic fever resemble those of other transmittable diseases, such as malaria or typhoid fever, medical diagnosis of the disease can be tough, particularly if just a single case is included.
Health Support: This high-absorption Magnesium Glycinate (200 mg) is gentle on the stomach and supports muscle relaxation, better sleep, and metabolic health. You can find this trusted formula on Amazon.
Diagnosis
Antigen-capture enzyme-linked immunosorbent assay (ELISA) screening, IgM-capture ELISA, polymerase chain reaction (PCR), and virus isolation can be used to confirm a case of Marburg hemorrhagic fever within a few days of the beginning of symptoms. The IgG-capture ELISA is proper for testing persons later in the course of disease or after recovery. The disease is easily identified by immunohistochemistry, virus seclusion, or PCR of blood or tissue specimens from departed patients.
Known Recovery Complications
Recovery from Marburg hemorrhagic fever might be prolonged and accompanied by orchititis, persistent hepatitis, transverse myelitis or uvetis. Other possible complications include inflammation of the testis, spinal cord, eye, parotid gland, or by prolonged hepatitis.
Is the disease ever deadly?
Yes. The case-fatality rate for Marburg hemorrhagic fever is between 23-25%.
Marburg Hemorrhagic Fever Treatment
A particular treatment for this disease is unidentified. However, helpful healthcare facility therapy must be made use of. This includes balancing the patient’s fluids and electrolytes, maintaining their oxygen status and blood pressure, changing lost blood and clotting aspects and treating them for any complicating infections.
In some cases treatment also has used transfusion of fresh-frozen plasma and other preparations to replace the blood proteins essential in clotting. One controversial treatment is the use of heparin (which blocks clotting) to prevent the usage of clotting elements. Some scientists think the intake of clotting aspects belongs to the disease procedure.
Who Is at Risk for the Disease?
People who have close contact with a human or non-human primate infected with the virus are at risk. Such persons consist of lab or quarantine center workers who deal with non-human primates that have actually been associated with the disease. In addition, health center personnel and relative who take care of patients with the disease are at risk if they do not use appropriate barrier nursing methods.
Prevention
Due to our restricted understanding of the disease, preventive measures against transmission from the original animal host have actually not yet been developed. Measures for prevention of secondary transmission are similar to those used for other hemorrhagic fevers. If a patient is either suspected or confirmed to have Marburg hemorrhagic fever, barrier nursing strategies need to be used to prevent direct physical contact with the patient. These preventative measures consist of using of protective dress, gloves, and masks; positioning the infected individual in stringent seclusion; and sterilization or proper disposal of needles, equipment, and patient excretions.
In conjunction with the World Health Organization, CDC has actually established useful, hospital-based guidelines, titled “Infection Control for Viral Haemorrhagic Fevers In the African Health Care Setting.” The manual can help health-care centers recognize cases and prevent further hospital-based disease transmission using in your area available products and few funds.
Dealing with the Danger
Marburg hemorrhagic fever is a really rare human disease. Nevertheless, when it does happen, it has the possible to spread to other people, specifically healthcare personnel and family members who look after the patient. Therefore, increasing awareness among health-care companies of clinical symptoms in patients that suggest Marburg hemorrhagic fever is critical. Better awareness can assist result in taking safety measures versus the spread of virus infection to relative or health-care companies. Improving using diagnostic tools is another top priority. With modern ways of transportation that admit even to remote areas, it is possible to acquire fast screening of samples in disease control centers equipped with Biosafety Level 4 labs in order to confirm or eliminate Marburg virus infection.
A fuller understanding of Marburg hemorrhagic fever will not be possible up until the ecology and identity of the virus reservoir are established. In addition, the impact of the disease will remain unidentified until the actual incidence of the disease and its endemic areas are determined.