For decades, the medical community viewed menopause as an absolute physiological finish line—a one-way street where the depletion of ovarian follicles signaled the end of reproductive vitality. However, as I analyze the current trajectory of regenerative medicine, the conversation is shifting from “managing symptoms” to the provocative question: Can we actually reverse the biological clock? While the short answer remains complex, the emerging science of ovarian rejuvenation suggests that the “permanent” nature of menopause may eventually be challenged.
The Biological Reality of Ovarian Aging
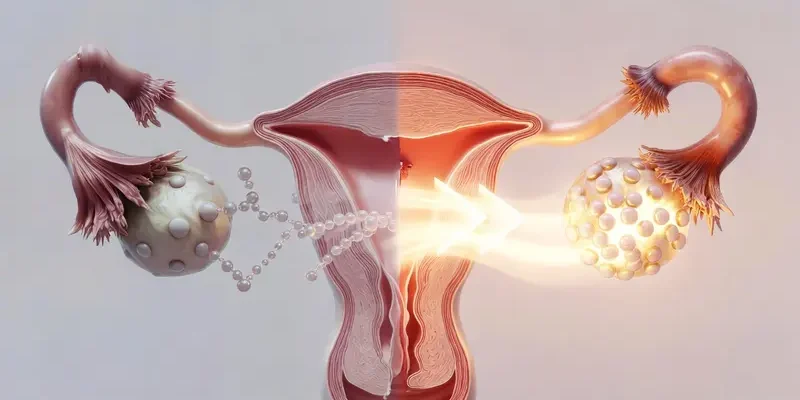
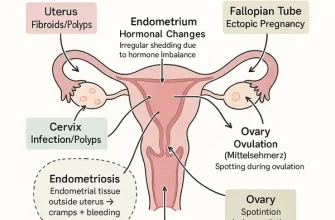
To understand the possibility of reversal, I believe it is crucial to first define what we are fighting against. Menopause is clinically confirmed after 12 consecutive months without a menstrual period, driven by the exhaustion of the ovarian reserve. In my view, the nuance often missed is that even after menopause, the ovaries are not “dead”; they contain thousands of residual primordial follicles that have simply fallen into a state of dormancy.
The challenge lies in “awakening” these follicles. Conventional Hormone Replacement Therapy (HRT) effectively manages the fallout—hot flashes, bone density loss, and mood shifts—but it does not restore ovarian function. From a clinical perspective, HRT is a bypass, not a reversal. True reversal would require the restoration of endogenous estrogen production and, potentially, the release of viable oocytes.
Interesting Facts About Ovarian Biology
- The Dormant Reserve: A person is born with approximately 1 to 2 million eggs, but by menopause, while active cycles stop, nearly 1,000 to 2,000 dormant follicles may still remain in the ovarian stroma. [Source: National Institutes of Health (NIH)]
- The “Grandmother Hypothesis”: Evolutionary biologists suggest menopause evolved to allow older females to help raise grandchildren, increasing the survival rate of the lineage. [Source: Smithsonian Magazine]
- Epigenetic Clocks: Ovaries age up to two times faster than any other organ in the human body, making them a primary target for anti-aging research. [Source: Buck Institute for Research on Aging]
PRP and Stem Cell Therapy: Emerging Frontiers
When I describe the current “reversal” landscape, the most discussed intervention is Platelet-Rich Plasma (PRP) therapy. This involves injecting a concentrated dose of the patient’s own growth factors directly into the ovaries. The theory is that these factors can stimulate the “niche” environment, potentially prompting dormant follicles to develop.
Health Support: This Vitamin K2 + D3 Complex is essential for bone density, cardiovascular health, and immune function. It’s a highly-rated formula for those looking to maintain optimal nutrient levels. You can find it on Amazon.
I find the data on PRP encouraging but inconsistent. Some clinical trials, such as those discussed by the American Society for Reproductive Medicine (ASRM), show that a small percentage of postmenopausal women resume menstruation and even achieve spontaneous pregnancy. However, the hidden disadvantage is the lack of long-term standardization. We do not yet know the “ideal” concentration of platelets or the longevity of the effect. It is a promising alternative for those who have failed traditional IVF, but it is not yet a guaranteed “cure” for menopause.
Statistical Realities of Reproductive Longevity
- Pregnancy Rates: For women over 45, the chance of natural conception is less than 1%, emphasizing the steep decline in egg quality even before menopause. [Source: Centers for Disease Control and Prevention (CDC)]
- PRP Success: Small-scale studies have indicated that up to 40% of perimenopausal women experienced a temporary restoration of hormonal markers after ovarian PRP. [Source: Journal of Clinical Medicine]
- The Age Factor: The average age of menopause in the United States is 51, a figure that has remained relatively stable despite increases in overall life expectancy. [Source: North American Menopause Society (NAMS)]
The Role of Lifestyle and Epigenetics
I often argue that while we wait for high-tech “reversals,” we underestimate the power of delaying the transition through epigenetic management. Factors such as oxidative stress, chronic inflammation (inflammaging), and environmental toxins accelerate follicular depletion. As highlighted by the Endocrine Society, endocrine-disrupting chemicals found in plastics and pesticides can trigger early ovarian failure.
In my experience, a lifestyle focused on mitochondrial support—utilizing coenzyme Q10, NAD+ precursors, and a high-antioxidant Mediterranean-style diet—can extend the perimenopausal window. While this isn’t “reversing” menopause once it has occurred, it is a form of proactive preservation. The nuance here is that lifestyle cannot create new eggs, but it can significantly improve the quality and functional lifespan of the remaining ones. Research published through the National Library of Medicine (PMC) suggests that mitochondrial health is the “engine” of ovarian longevity.
Breakthroughs in Genetic Engineering and Bio-Islets
Looking toward the future, I am closely watching the development of “bio-artificial ovaries.” This involves seeding a 3D-printed scaffold with a patient’s cells to mimic natural hormonal cycles. Unlike HRT, which provides a steady, artificial dose, these bio-islets respond to the body’s feedback loops.
Health Support: This high-absorption Magnesium Glycinate (200 mg) is gentle on the stomach and supports muscle relaxation, better sleep, and metabolic health. You can find this trusted formula on Amazon.
Research published through Harvard Medical School explores how CRISPR and genetic reprogramming might one day allow us to “reset” the aging markers in ovarian tissue. This is the only path that could truly be called a “reversal.” The drawback, of course, is that these technologies are currently in the experimental stages. We must be careful not to mistake laboratory progress for immediate clinical availability.
Personal Recommendation from Reyus Mammadli
If you are seeking to navigate the possibility of ovarian rejuvenation, my strongest recommendation is to shift your focus from “reversing the past” to “optimizing the present.” Do not be swayed by clinics promising a “fountain of youth” through unverified stem cell injections without rigorous data.
My unique advice: Prioritize mitochondrial health at least two years before you expect the menopausal transition to begin. The energy centers of your cells (mitochondria) are the first to fail in the ovaries. By utilizing targeted supplementation like Ubiquinol and practicing intermittent fasting—which triggers autophagy and cellular cleanup—you are effectively giving your ovaries the best environment to function longer.
In closing, while science is inching closer to “turning back the clock,” your best strategy is to maintain the biological “machinery” you currently have. Reversal is a fascinating scientific frontier, but prevention and optimization remain your most reliable tools.