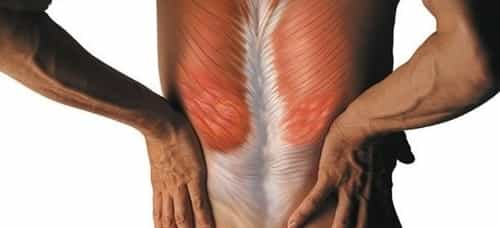
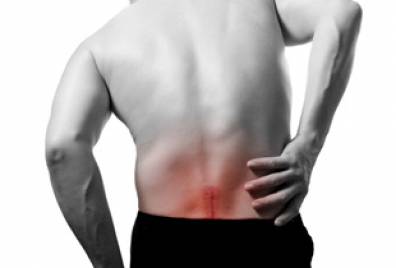
Muscle relaxers, or muscle relaxants, are medications used to treat muscle spasms or muscle spasticity. Muscle spasms or cramps are unexpected, involuntary contractions of a muscle or group of muscles. They can be caused by too much muscle strain and lead to pain. They’re related to conditions such as lower back pain, neck pain, and fibromyalgia.
Muscle spasticity, on the other hand, is a constant muscle spasm that causes tightness, rigidness, or tightness that can disrupt normal walking, talking, or motion. Muscle spasticity is triggered by injury to parts of the brain or spine included with movement. Conditions that can cause muscle spasticity include multiple sclerosis (MS), spastic paralysis, and amyotrophic lateral sclerosis (ALS).
Prescription drugs can help ease the pain and discomfort from muscle spasms or spasticity. In addition, specific over the counter medications might be used to treat aches and pains related to muscle spasms.
Best Muscle Relaxants – Rating of Popular Relaxers in USA
1) Methocarbamol (Robaxin).
Health Support: This Vitamin K2 + D3 Complex is essential for bone density, cardiovascular health, and immune function. It’s a highly-rated formula for those looking to maintain optimal nutrient levels. You can find it on Amazon.
An inexpensive and relatively less sedating choice, methocarbamol has actually been well studied for usage in back pain. In recent studies where it was utilized for as much as eight days, 44% of folks that took methocarbamol had total pain relief (compared with 18% who took nothing) — which lacked any serious side effects.
Taken as needed, 1500 mg every 6 to 8 hours is a low-cost and well-tolerated alternative for patients of acute neck and back pain. Consider attempting this first, as it is less sedating than other options, like cyclobenzaprine and carisoprodol.
2) Cyclobenzaprine (Flexeril).
At the basic dose of 10 mg to 30 mg a day, cyclobenzaprine will make you sleepy. If utilized during the day you’ll want to break your 10 mg tab in half and take 5 mg to lessen the drowsiness. Interestingly, 5 mg 3 times a day has been displayed in research studies to work in addition to 10 mg taken 3 times a day.
Health Support: This high-absorption Magnesium Glycinate (200 mg) is gentle on the stomach and supports muscle relaxation, better sleep, and metabolic health. You can find this trusted formula on Amazon.
Cyclobenzaprine is a reasonable first option since it’s a low-cost generic, but the sedation side effect limits its usage throughout the day. It may also cause more dry mouth, especially in older folks. If this is a concern, think about a better non-sedating alternative.
3) Carisoprodol (Soma).
Carisoprodol is a Schedule IV drug (much like benzodiazepines Ativan, Valium, and Xanax) and has the capacity for being abused. For this factor, it ought to not be utilized if there is a history of compound abuse.
The basic viewpoint is that carisoprodol ought to be phased out as a muscle relaxant in favor of much better choices. If prescribed, carisoprodol needs to only be used for brief durations of 2 to 3 weeks due to lack of proof for effectiveness with longer usage. It may cause sleepiness and lightheadedness, and must not be utilized in folks over 65.
4) Metaxalone (Skelaxin).
Taken as 800 mg tablets three to 4 times a day, metaxalone has actually the fewest reported side effects and most affordable sedation potential of the muscle relaxants based upon clinical studies. Basically, it is the best-tolerated of the muscle relaxants.
Metaxolone is a generic alternative for the brand drug, Skelaxin, however it is still expensive. Having stated that, it works as well as cyclobenzaprine and carisoprodol with fewer side effects and less sedation — so paying money might deserve it.
5) Tizanidine (Zanaflex).
Tizanidine is used more for spasticity in clients with several sclerosis or spastic paralysis. Spasticity is where the muscles go through constant contraction, which causes tightness and stiffness. In head to head studies with Baclofen for those conditions, it has the tendency to have less side effects — however they both work simply as well. This is not a first-line choice for severe neck or back muscle pain though.
6) Baclofen.
Just like tizanidine, Baclofen is mostly used for spasticity in spine injury patients or those with multiple sclerosis. Sleepiness happens in as much as 20% of folks taking it, and there are better alternatives for neck and back muscle pain. Also not a first choice.
7) Oxazepam.
Benzodiazepine medications like oxazepam and diazepam (Valium), are often prescribed as muscle relaxants. However, these truly aren’t suggested because they don’t work well, are sedating, and can be habit-forming. Avoid benzodiazepines for neck and back muscle pain due to the fact that there are far better choices.
8) Chlorzoxazone (Lorzone).
Chlorzoxazone is not well-studied for acute low back and neck pain in adults, and when investigated for pain after spinal column surgery, it wasn’t found to be efficient. Chlorzoxazone has likewise been reported as an unusual cause of intense liver toxicity. Do not select this up until you’ve tired all other options.
9) Orphenadrine (Norflex).
For neck and back pain in adults, the first 4 medications on this list work better than orphenadrine, so save this as another last option in the event the others don’t work. It simply hasn’t been well studied for this function.
Next, we discussed in more detail each of the categories of antispasmodic drugs for the muscles of the body.
Prescription Medications
Prescription medications are divided into two groups: antispasmodics and antispastics. Antispasmodics are used to treat muscle spasms, and antispastics are used to treat muscle spasticity. Some antispasmodics, such as tizanidine, can be used to treat muscle spasticity. Nevertheless, antispastics need to not be used to treat muscle spasms.
Antispasmodics
Centrally acting skeletal muscle relaxants (SMRs). Centrally acting SMRs are used in addition to rest and physical therapy to help relieve muscle spasms. They’re thought to work by triggering a sedative result or by avoiding your nerves from sending out pain signals to your brain.
You need to just use these muscle relaxants for as much as 2 or 3 weeks. The safety of longer-term use is not yet known.
While antispasmodics can be used to treat muscle spasms, they have not been shown to work much better than nonsteroidal anti-inflammatory drugs (NSAIDs) or acetaminophen. In addition, they have more side effects than NSAIDs or acetaminophen.
The more typical side effects of centrally acting SMRs include:
- drowsiness.
- dizziness.
- headache.
- anxiety.
- reddish-purple or orange urine.
- lowered high blood pressure upon standing.
You ought to speak with your doctor about the benefits and risks of these medications for the treatment of your muscle spasms.
List of centrally acting SMRs
| Generic name | Brand name | Form | Generic available |
| carisoprodol | Soma | tablet | yes |
| carisoprodol/aspirin | not available | tablet | yes |
| carisoprodol/aspirin/codeine | not available | tablet | yes |
| chlorzoxazone | Parafon Forte, Lorzone | tablet | yes |
| cyclobenzaprine | Fexmid, Flexeril, Amrix | tablet, extended-release capsule | tablet only |
| metaxalone | Skelaxin, Metaxall | tablet | yes |
| methocarbamol | Robaxin | tablet | yes |
| orphenadrine | Norflex | extended-release tablet | yes |
| tizanidine | Zanaflex | tablet, capsule |
Antispastics
Antispastics are used to treat muscle spasticity. They must not be used to treat muscle spasms. These drugs consist of:
Baclofen: Baclofen (Lioresal) is used to eliminate spasticity caused by MS. It’s not fully comprehended how it works, but it appears to block nerve signals from the spinal cord that cause muscles to spasm. Side effects can include sleepiness, dizziness, weak point, and tiredness.
Dantrolene: Dantrolene (Dantrium) is used to treat muscle spasms triggered by spinal cord injury, stroke, cerebral palsy, or MS. It works by acting directly on the skeletal muscle to unwind the muscle spasm. Side effects can include sleepiness, dizziness, lightheadedness, and tiredness.
Diazepam: Diazepam (Valium) is used to alleviate muscle spasms triggered by inflammation, trauma, or muscle spasticity. It works by increasing the activity of a particular neurotransmitter to reduce the event of muscle spasms. Diazepam is a sedative. Side effects can include drowsiness, fatigue, and muscle weakness.

List of antispastics
| Generic name | Brand name | Form | Generic available |
| baclofen | Lioresal, Gablofen, Lioresal | tablet, injection | yes |
| dantrolene | Dantrium | tablet | yes |
| diazepam | Valium | oral suspension, tablet, injection | yes |
Muscle relaxants such as carisoprodol and diazepam can be habit forming. Make sure to take your medication exactly as recommended by your doctor.
Warnings for Prescription Muscle Relaxants
Muscle relaxants can also cause withdrawal symptoms, such as seizures or hallucinations (noticing things that aren’t genuine). Do not all of a sudden stop taking your medication, particularly if you’ve been taking it for a long period of time.
Also, muscle relaxants depress your central nervous system (CNS), making it difficult to focus or remain awake. While taking a muscle relaxant, prevent activities that need mental alertness or coordination, such as driving or using heavy machinery.
You need to not take muscle relaxants with:
- alcohol (iytmed.com recommend you quit it completely).
- CNS depressant drugs, such as opioids or psychotropics.
- sleeping medications.
- natural supplements such as St. John’s wort.
Talk to your doctor about how you can securely use muscle relaxants if you:
- are older than 65 years.
- have a psychological health issue or brain disorder.
- have liver problems.
Off-label Medications for Spasticity
Medical professionals can use particular medications to treat spasticity even when the drugs are not authorized for that function by the U.S. Food and Drug Association (FDA). This is called off-label drug use. The following drugs are not actually muscle relaxants, however they can still help ease symptoms of spasticity.
Benzodiazepines
Benzodiazepines are sedatives that can assist unwind muscles. They work by increasing the effects of specific neurotransmitters, which are chemicals that relay messages between your brain cells.
Examples of benzodiazepines consist of:
- clonazepam (Klonopin).
- lorazepam (Ativan).
- alprazolam (Xanax).
Side effects of benzodiazepines can consist of sleepiness and problems with balance and memory. These drugs can also be routine forming.
Clonidine
Clonidine (Kapvay) is believed to work by avoiding your nerves from sending out pain signals to your brain or by causing a sedative effect.
Clonidine should not be used with other muscle relaxants. Taking it with similar drugs increases your risk of side effects. For example, taking clonidine with tizanidine can cause really low blood pressure.
Clonidine is offered in brand-name and generic versions.
Gabapentin
Gabapentin (Neurontin) is an anticonvulsant drug normally used to alleviate seizures. It’s not completely known how gabapentin works to relieve muscle spasticity. Gabapentin is readily available in brand-name and generic variations.
Non-prescription alternatives for muscle spasms.
OTC treatment is advised as first-line therapy for muscle spasms caused by conditions such as acute lower back pain or stress headache. This means you should attempt OTC treatments before prescription medications.
OTC treatment choices consist of nonsteroidal anti-inflammatory drugs (NSAIDs), acetaminophen, or a mix of both. Your doctor or pharmacist can assist you select an OTC treatment.
Nonsteroidal anti-inflammatory drugs (NSAIDs)
NSAIDs work by obstructing your body from making certain compounds that cause inflammation and pain. NSAIDs are readily available in generic and brand-name variations. They’re generally offered over-the-counter. More powerful variations are readily available by prescription.
NSAIDs come as oral tablets, capsules, or suspensions. They also come as chewable tablets for children. Side effects of these drugs can consist of indigestion and dizziness.
Examples of NSAIDs include:
- ibuprofen (Advil, Motrin).
- naproxen (Aleve, Naprosyn).
- Acetaminophen.
Acetaminophen (Tylenol) is believed to work by blocking your body from making certain substances that cause pain. Acetaminophen is readily available in generic and brand-name variations. It comes as immediate-release and extended release oral tablets and pills, orally breaking down tablets, chewable tablets, and oral services.
The more typical side effects of acetaminophen can include nausea and upset stomach.
When to call your doctor
You can often handle your muscle spasm or spasticity symptoms by yourself, however in some cases, you may require medical suggestions or care. Make certain to call your doctor if you:
- have spasticity for the first time and do not know the cause.
- observe the spasticity is getting more severe, happening more frequently, or making jobs tough.
- have severe and regular muscle spasms.
- notice defect of the parts of your body affected by muscle spasms.
- have side effects from your muscle relaxant.
- have a “frozen joint” due to contracture that reduces your series of motion or causes pressure sores.
- have increasing pain or discomfort.