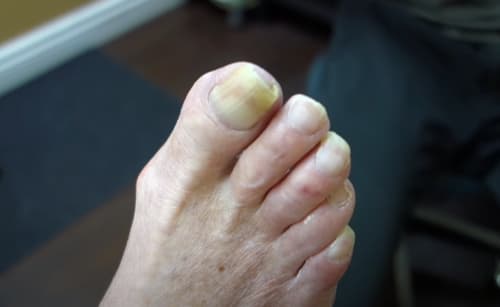
Around 7.4 million people in the United States have psoriasis. This condition triggers your body to produce too many skin cells. The extra cells build up on your skin, forming flaky red or silvery white spots, sores, or blisters.
Psoriasis can take place anywhere on your body, including your:
- chest
- arms
- legs
- trunk
- nails
About 35 percent of individuals with psoriasis and around 80 percent of individuals with psoriatic arthritis, a related joint condition, establish nail modifications. Doctors aren’t sure why this occurs to some people and not others.
In unusual cases, the nails are the only parts of the body that reveal indications of psoriasis. Usually, individuals with psoriasis have a rash on other parts of their body also.
Health Support: This Vitamin K2 + D3 Complex is essential for bone density, cardiovascular health, and immune function. It’s a highly-rated formula for those looking to maintain optimal nutrient levels. You can find it on Amazon.
Symptoms of Nail Psoriasis
Nail psoriasis can cause a number of various symptoms.
Pitting
The nail plate is the tough surface that forms the top of your nails. It’s made of keratin cells.
Nail psoriasis causes your nail plate to lose cells. This results in little pits forming on your fingernails or toenails. The number of pits varies from person to person.
Some individuals may have just a single pit on each nail, while others have lots of pits. The pits can be shallow or deep.
Health Support: This high-absorption Magnesium Glycinate (200 mg) is gentle on the stomach and supports muscle relaxation, better sleep, and metabolic health. You can find this trusted formula on Amazon.
Nail Bed Separation
Sometimes your nail can separate from the nail bed, which is the skin underneath the nail plate. This separation is called onycholysis. It leaves an empty space under your nail.
If you have nail psoriasis, you may first notice a white or yellow spot at the suggestion of a nail. The color will eventually go all the way to the cuticle.
Bacteria can get into the area under the nail and cause infection, which can turn the whole nail a dark color.
Changes in Nail Shape or Thickness
In addition to pitting, you may notice other modifications in the texture of your nails. Psoriasis can trigger lines called Beau’s lines to form throughout your nails.
Weakness of the structures that support nails can trigger your nails to fall apart. Nails can likewise become thicker due to a fungal infection called onychomycosis, which is common in people with psoriasis.
Discolored Nails
The color of your nail may likewise alter. You might see a yellow-red patch in the nail bed. It appears like a drop of oil under your nail plate, which is where it gets its name: oil-drop area.
Your toenails or fingernails can likewise turn a yellow-brown color. Falling apart nails frequently turn white.
Treatments for Nail Psoriasis
Nail psoriasis can be difficult to deal with since psoriasis affects the nail as it grows. Treatment alternatives include:
Topical Medications
Topical corticosteroids are a common nail psoriasis treatment. They’re available as:
- ointments
- creams
- emulsions
- nail polishes
You’ll generally apply them once or twice a day.
Corticosteroid injections can be useful for treating signs like:
- nail thickening
- ridges
- separation
Calcipotriol (Calcitreme), calcipotriene (Dovonex), and calcitriol are man-made versions of vitamin D.
They help reduce inflammation and slow excess skin cell production. These medications can alleviate nail thickness by reducing cell buildup under the nails.
Tazarotene (Tazorac) is a topical retinoid, a medication made from vitamin A. It can aid with:
- nail discoloration
- pitting
- separation
Anthralin is an anti-inflammatory ointment that slows excess skin cell production. When applied to the nail bed once daily, it improves signs like thickening and onycholysis.
Moisturizers don’t treat nail psoriasis, however they can eliminate itching and inflammation and help the skin around your nails heal.
Oral Drugs
Systemic (body-wide) drugs like cyclosporine, methotrexate, apremilast (Otezla), and retinoids are readily available as a liquid or tablet or an injectable medication.
They work throughout the body to clear both the skin and nails and are implied for moderate-to-severe psoriasis.
Biologic drugs like adalimumab (Humira), etanercept (Enbrel), and infliximab (Remicade) moisten the overactive immune action that causes psoriasis.
You get these drugs by infusion or injection. They’re generally scheduled for psoriasis that hasn’t responded to other treatments.
Oral anti-fungal drugs treat fungal infections brought on by nail psoriasis.
Phototherapy
Phototherapy exposes areas of skin affected by psoriasis to:
- ultraviolet (UV) rays from the sun
- a phototherapy system at a center or at home
- a laser
The light slows the growth of skin cells.
For nail psoriasis, the treatment is called PUVA. First, you soak your hands or take a medication called psoralen. Then, you’re exposed to UVA light. This treatment can be practical for treating nail separation and discoloration.
Laser Treatment
Laser treatment may be handy for nail psoriasis. The type of laser utilized in nail psoriasis is called the pulsed color laser (PDL).
It works by targeting blood vessels under the skin with a beam, and it appears to reduce the severity of nail psoriasis.
Home Treatments for Nail Psoriasis
A few natural solutions may relieve psoriasis symptoms, including:
- turmeric
- capsaicin
- Dead Sea salt
- aloe vera
But, for nail psoriasis, the alternative treatment options are more limited.
One natural treatment that’s shown advantage for nail psoriasis is indigo naturalis, a Chinese herbal medicine that originates from the very same plant used to make blue color.
In one small study, an indigo naturalis extract in oil (Lindioil) enhanced nail thickening and onycholysis better than calicootriene.
Tips for Prevention
In addition to medication, attempt these pointers for preventing flares:
- Keep your nails brief to avoid injury or lifting the nail off of its bed. Cutting your nails regularly will likewise prevent buildup from gathering underneath them.
- Don’t bite or pick at your nails or push back your cuticles. Injuries to the skin can set off psoriasis flares. This is called the Koebner phenomenon.
- Use protective gloves when you garden or play sports and when you clean meals or work with your hands in water.
- Keep your nails clean to prevent infection.
- Use a moisturizing cream on your nails and cuticles. This can help avoid split or breakable nails.
- Prevent cleaning your nails with a nail brush or a sharp object. This will assist avoid nail separation.
How to Hide Nail Psoriasis
If you feel uneasy about your nail psoriasis, there are some things you can do to make it less noticeable.
Cosmetic treatments such as nail filing, buffing, and polish can enhance the appearance of your nails while they recover. Just avoid fake nails, which may increase the threat of your nail separating from its bed.
When to See a Doctor
The National Psoriasis Foundation recommends that everybody with psoriasis see a skin doctor for a medical diagnosis and treatment. If you’ve already been identified, make an appointment with your doctor if:
- your symptoms are getting worse or are bothering you
- the treatment you’re on isn’t assisting
- you want to attempt a new treatment or alternative remedy