Toxic shock syndrome is an unusual, deadly issue of certain types of bacterial infections. Typically toxic shock syndrome arises from toxins produced by Staphylococcus aureus (staph) bacteria, but the condition might also be brought on by toxins produced by group A streptococcus (strep) bacteria.
Toxic shock syndrome has been associated mostly with making use of superabsorbent tampons. However, considering that makers pulled particular types of tampons off the market, the incidence of toxic shock syndrome in menstruating women has declined.
Toxic shock syndrome can impact anyone, including men, children and postmenopausal women. Risk factors for toxic shock syndrome include skin injuries and surgery.
Health Support: This Vitamin K2 + D3 Complex is essential for bone density, cardiovascular health, and immune function. It’s a highly-rated formula for those looking to maintain optimal nutrient levels. You can find it on Amazon.
Toxic Shock Syndrome Symptoms
Possible signs and symptoms of toxic shock syndrome consist of:
- A sudden high fever
- Low high blood pressure (hypotension).
- Vomiting or diarrhea.
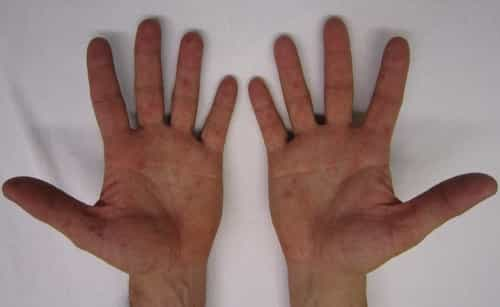
- A rash resembling a sunburn, especially on your palms and soles.
- Confusion.
- Muscle aches.
- Redness of your eyes, mouth and throat.
- Seizures.
- Headaches.
When to see a doctor
Call your doctor right away if you have signs or symptoms of toxic shock syndrome. This is especially important if you’ve recently used tampons or if you have a skin or injury infection.
What Causes Toxic Shock Syndrome
A lot of commonly, Staphylococcus aureus (staph) bacteria cause toxic shock syndrome. The syndrome can likewise be triggered by group A streptococcus (strep) bacteria.
Risk Factors
Toxic shock syndrome can impact anybody. About half the cases of toxic shock syndrome associated with Staphylococci bacteria take place in women of menstruating age; the rest take place in older women, men and children. Streptococcal toxic shock syndrome happens in people of any ages.
Health Support: This high-absorption Magnesium Glycinate (200 mg) is gentle on the stomach and supports muscle relaxation, better sleep, and metabolic health. You can find this trusted formula on Amazon.
Toxic shock syndrome has actually been related to:
- Having cuts or burns on your skin.
- Having actually had recent surgery.
- Using contraceptive sponges, diaphragms or superabsorbent tampons.
- Having a viral infection, such as the flu or chickenpox.
Complications
Toxic shock syndrome can progress quickly. Complications may include:
- Shock.
- Renal failure.
- Death.
Toxic Shock Syndrome Prevention
Producers of tampons sold in the United States no longer use the products or styles that were associated with toxic shock syndrome. Likewise, the Food and Drug Administration needs producers to use standard measurement and labeling for absorbency and to print guidelines on packages.
If you use tampons, checked out the labels and use the most affordable absorbency tampon you can. Change tampons regularly, a minimum of every four to 8 hours. Alternate using tampons and feminine napkins, and use minipads when your flow is light.
Toxic shock syndrome can repeat. People who’ve had it once can get it again. If you’ve had toxic shock syndrome or a previous major staph or strep infection, don’t use tampons.
Diagnosis
There’s nobody test for toxic shock syndrome. You may need to provide blood and urine samples to test for the existence of a staph or strep infection. Your vaginal area, cervix and throat might be swabbed for samples for lab analysis.
Due to the fact that toxic shock syndrome can affect multiple organs, your doctor may order other tests, such as a CT scan, lumbar puncture or chest X-ray, to evaluate the level of your health problem.
Treatment for Toxic Shock Syndrome
If you develop toxic shock syndrome, you’ll likely be hospitalized. In the healthcare facility, you’ll:
- Be treated with antibiotics while doctors seek the infection source.
- Receive medication to support your high blood pressure if it’s low (hypotension) and fluids to treat dehydration.
- Get encouraging care to treat other signs and symptoms.
The toxins produced by the staph or strep bacteria and accompanying hypotension may lead to kidney failure. If your kidneys stop working, you might need dialysis.
Surgery
Surgery may be needed to remove nonliving tissue (debridement) from the site of infection or to drain the infection.