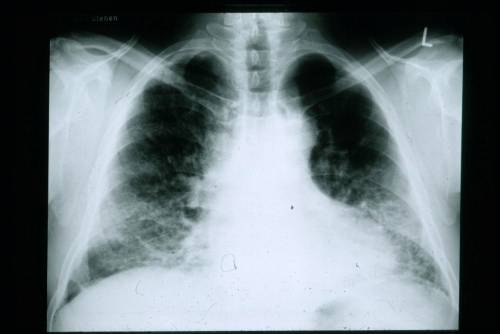
Acute respiratory distress syndrome (ARDS) is a dangerous lung condition that prevents sufficient oxygen from getting to the lungs and into the blood. Infants can also have respiratory distress syndrome.
Causes
ARDS can be brought on by any major direct or indirect injury to the lung. Typical causes consist of:
- Breathing vomit into the lungs (aspiration).
- Inhaling chemicals.
- Lung transplant.
- Pneumonia.
- Septic shock (infection throughout the body).
- Injury.
ARDS leads to a buildup of fluid in the air sacs (alveoli). This fluid avoids enough oxygen from passing into the bloodstream.
Health Support: This Vitamin K2 + D3 Complex is essential for bone density, cardiovascular health, and immune function. It’s a highly-rated formula for those looking to maintain optimal nutrient levels. You can find it on Amazon.
The fluid accumulation also makes the lungs heavy and stiff, which decreases the lungs’ ability to expand. The level of oxygen in the blood can stay precariously low, even if the individual gets oxygen from a breathing machine (ventilator) through a breathing tube (endotracheal tube).
ARDS frequently occurs together with the failure of other organ systems, such as the liver or kidneys. Cigarette smoking and heavy alcohol use might be risk factors.
Symptoms of Acute Respiratory Distress Syndrome
Symptoms normally develop within 24 to 48 hours of the injury or illness. Typically, people with ARDS are so sick they can not experience symptoms. Symptoms can include any of the following:
- Problem breathing.
- Low blood pressure and organ failure.
- Rapid breathing.
- Shortness of breath.
Diagnosis
Listening to the chest with a stethoscope (auscultation) reveals unusual breath sounds, such as crackles, which might be signs of fluid in the lungs. Often, high blood pressure is low. Cyanosis (blue skin, lips, and nails brought on by absence of oxygen to the tissues) is typically seen.
Health Support: This high-absorption Magnesium Glycinate (200 mg) is gentle on the stomach and supports muscle relaxation, better sleep, and metabolic health. You can find this trusted formula on Amazon.
Tests used to diagnose ARDS include:
- Arterial blood gas.
- Blood tests, including CBC and blood chemistries.
- Blood and urine cultures.
- Bronchoscopy in some people.
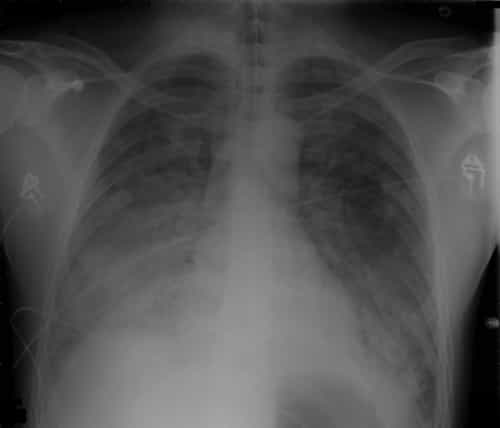
- Chest x-ray.
- Sputum cultures and analysis.
- Tests for possible infections.
An echocardiogram may be had to eliminate heart failure, which can look similar to ARDS on a chest x-ray.
ARDS Treatment
ARDS often has to be dealt with in an intensive care unit (ICU).
The goal of treatment is to offer breathing support and treat the cause of ARDS. This might involve medications to treat infections, reduce inflammation, and remove fluid from the lungs.
A ventilator is used to provide high dosages of oxygen and positive pressure to the harmed lungs. People often need to be deeply sedated with medicines. During treatment, healthcare providers strive to safeguard the lungs from further damage. Treatment is generally helpful until the lungs recover.
ARDS Support Groups
Numerous relative of people with ARDS are under extreme stress. They can often ease this stress by signing up with support groups where members share common experiences and problems.
Can You Die From Acute Respiratory Distress Syndrome?
About one third of people with ARDS die of the disease. Those who live frequently return the majority of their normal lung function, but many people have permanent (usually mild) lung damage.
Many people who survive ARDS have amnesia or other quality-of-life problems after they recuperate. This is because of mental retardation that happened when the lungs were not working effectively and the brain was not getting sufficient oxygen.
Possible Complications
Issues that might result from ARDS or its treatment include:
- Failure of numerous organ systems.
- Lung damage, such as a collapsed lung (also called pneumothorax) due to injury from the breathing machine needed to treat the disease.
- Pulmonary fibrosis (scarring of the lung).
- Ventilator-associated pneumonia.
When to Contact a Medical Professional
ARDS most often takes place during another illness, for which the person is already in the health center. In many cases, a healthy individual has severe pneumonia that worsens and becomes ARDS. If you have problem breathing, call your local emergency number (such as 911) or go to the emergency room.
Alternative names of the disease are: Noncardiogenic pulmonary edema; Increased-permeability lung edema; ARDS; Acute lung injury.