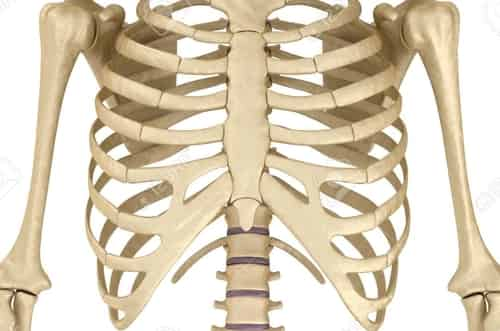
Costochondritis is an inflammation of the cartilage in the chest. The condition typically impacts the cartilage where the upper ribs attach to the breastbone, or breastbone, an area known as the costosternal joint or costosternal junction.
Chest pain caused by costochondritis can vary from moderate to severe. Mild cases might only trigger your chest to feel tender to touch or some pain when you push on the area of your chest cartilage.
Severe cases may cause shooting discomforts down your limbs or excruciating chest pain that hinders your life and does not seem to go away. The condition often goes away within a couple of weeks, but some cases may need treatment.
Health Support: This Vitamin K2 + D3 Complex is essential for bone density, cardiovascular health, and immune function. It’s a highly-rated formula for those looking to maintain optimal nutrient levels. You can find it on Amazon.
Costochondritis Symptoms
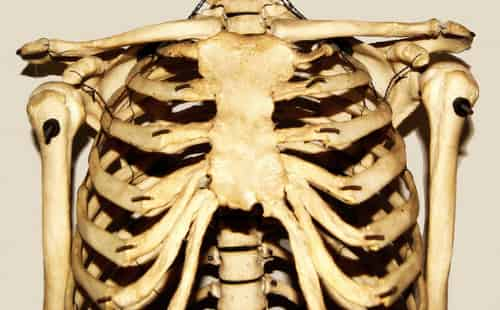
Chest pain associated with costochondritis is generally preceded by exercise, small injury, or an upper respiratory infection.
- The pain, which may be dull, usually will be sharp and situated on your front chest wall. It may radiate to your back or abdominal area and is more common on your left side.
- There can be a pain with a deep breath or a cough.
- The most common websites of pain are your 4th, fifth, and 6th ribs. This pain increases as you move your trunk or take deep breaths. Alternatively, it reduces as your movement stops or with quiet breathing.
- The reproducible inflammation you feel when you continue the rib joints (costochondral junctions) is a continuous function of costochondritis. Without this inflammation, a diagnosis of costochondritis is not likely.
- Tietze syndrome, on the other hand, exhibits swellings at the rib-cartilage junction. Costochondritis has no noticeable swelling. Neither condition includes pus or abscess formation.
- Tietze syndrome usually affects the junctions at the 2nd and third ribs. The swelling may last for several months. The syndrome can develop as a complication of surgery on your sternum months to years after the operation.
- When costochondritis takes place as a result of infection after surgery, you will see inflammation, swelling, or pus discharge at the site of the surgery.
When to Seek Medical Care
Call the medical professional for any of the following symptoms:
- Trouble breathing
- High fever
- Signs of infection such as soreness, pus, and increased swelling at the rib joints
- Continuing or intensifying pain regardless of medication
- Nausea
- Sweating
- Lightheadedness
Go to a health center’s emergency clinic if you have problem breathing or any of the following symptoms happen or getting worse. These symptoms are usually not associated with costochondritis:
- High fever is not reacting to fever-reducers such as acetaminophen (Tylenol) or ibuprofen (Advil).
- Signs of infection at the tender spot, such as pus, inflammation, increased pain, and swelling.
Persistent chest pain of any type related to nausea, sweating, left arm pain, or any generalized chest pain that is not well localized. These might be signs of cardiovascular disease. If you are uncertain what is triggering your condition, continuously go to the emergency clinic.
Health Support: This high-absorption Magnesium Glycinate (200 mg) is gentle on the stomach and supports muscle relaxation, better sleep, and metabolic health. You can find this trusted formula on Amazon.
What Causes Costochondritis?
The triggers of costochondritis in most people is unknown. But conditions that might cause it include:
- injuries to the chest, such as blunt impact from a cars and truck accident or fall
- physical strain from activities, such as heavy lifting and exhausting exercise
- certain viruses or respiratory conditions, such as tuberculosis and syphilis that can cause joint inflammation
- certain types of arthritis
- tumors in the costosternal joint area
Who Is at Risk for Costochondritis?
Costochondritis occurs more frequently in women and people over age 40. You may also be at a higher threat for this condition if you:
- participate in high-impact activities
- carry out manual work
- have allergies and are frequently exposed to irritants
Your risk increases if you have any of the lists below conditions:
- rheumatoid arthritis
- ankylosing spondylitis
- reactive arthritis formerly referred to as Reiter’s syndrome
Improperly managing heavy loads can stress chest muscles. More youthful individuals must raise heavy bags and knapsacks with care. Adults should perform manual labor with caution.
How to Avoid Costochondritis from Getting Worse?
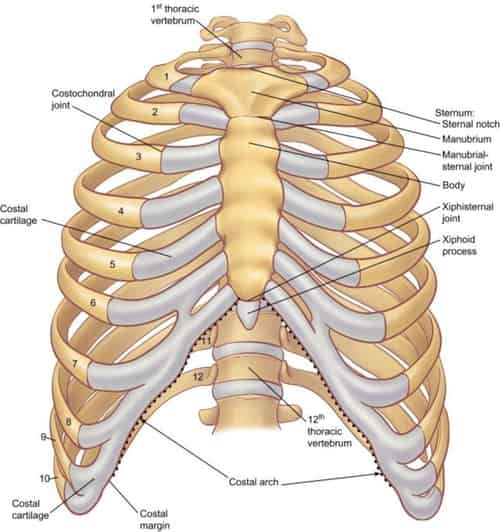
Your doctor may inform you to make a long-term way of life modifications if you have persistent or chronic costochondritis. Some types of exercise can intensify this condition, including running and weightlifting. Manual work can likewise have a negative effect. What makes costochondritis worse? How to prevent it?
Your physician may likewise recommend:
- bed rest
- physical therapy
- hot or cold treatment using a heating pad and ice
Your doctor may use pain levels to examine your reaction to treatment. Once you’ve finished treatment, you can slowly build up to your previous activity levels. Daily stretching can help relieve some pain. Your medical professional can also perform a therapy called transcutaneous electrical nerve stimulation (TENS), which uses small amounts of electrical power to stop your nerves from sending out signals of pain or aching to your brain.
Long-term pain caused by costochondritis can be debilitating if unattended. Typically, treatment of the inflammation and pain triggers costochondritis to disappear on its own ultimately.
If you have chronic costochondritis, the pain may return– even with treatment– when you work out or take part in specific activities. In these cases, you might need to seek long-lasting care to make certain that costochondritis does not affect your quality of life and capability to take part in daily activities.
Discomforts associated with costochondritis can suggest other issues. Chest discomforts can typically imply that you have heart concerns, so see your doctor immediately when you feel pain in your chest to ensure that you’re not having a cardiac arrest or have pneumonia.
The chest pain connected with costochondritis is a common symptom of fibromyalgia. With fibromyalgia, you might experience pain in your chest in addition to:
- pain throughout your body
- fatigue and failure to rest due to pain
- difficulty focusing or focusing
- feelings of anxiety
- headaches
If you experience chest discomforts along with these other symptoms, speak with your doctor about getting tested for fibromyalgia. Understanding this condition can help you deal with the symptoms and ensure that it doesn’t disrupt your daily life.
What Is the Long-lasting Outlook for Costochondritis?
This condition normally isn’t consistent. In most cases, costochondritis disappears on its own. Mild cases of costochondritis may vanish after a couple of days. Chronic cases can last for weeks or more, but a lot of cases don’t last any longer than a year.
To reduce your possibility of consistent and chronic costochondritis, carry and raise heavy loads properly. Try doing less high-impact exercises or manual labor. Call your medical professional instantly if you experience chest pain while carrying out any of these activities.