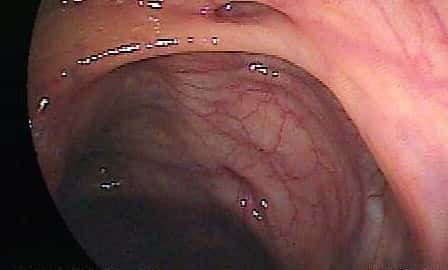
Rectal bleeding may show up as blood in your stool, on the bathroom tissue or in the toilet bowl. Blood that arises from rectal bleeding can vary in color from bright red to dark maroon to a dark, tarry color. There are many possible causes for rectal bleeding and a complete evaluation and early medical diagnosis by your doctor is very important.
Rectal bleeding should constantly be examined with a comprehensive consultation and evaluation by a doctor for a precise diagnosis and treatment plan as it may be a symptom or sign of a severe illness or condition. Causes of of rectal bleeding include:
Anal Fissures
An anal fissure is a little cut or tear in the lining of the rectum. The fracture in the skin causes severe pain and some bright red bleeding during and after bowel movements. At times the fissure is deep enough to expose the muscle tissue beneath. An anal fissure may occur as an outcome of childbirth, straining during defecation, or long bouts of constipation or diarrhea. Anal fissures can also be the outcome of particular medical conditions such as inflammatory bowel disease (IBD), infection, and cancer.
An anal fissure can affect people of any ages, and it’s frequently seen in infants and young kids. Constipation is a typical problem in these age groups. An anal fissure normally isn’t a serious condition. Most of the times, the tear heals by itself within four to 6 weeks. In cases where the fissure persists beyond eight weeks, it’s thought about chronic, or long term.
Health Support: This Vitamin K2 + D3 Complex is essential for bone density, cardiovascular health, and immune function. It’s a highly-rated formula for those looking to maintain optimal nutrient levels. You can find it on Amazon.
To treat anal fissures:
- Apply topical nitroglycerin or calcium channel blockers
- Use stool softeners
- Sitz baths for comfort
- Increase dietary fiber
- Stay hydrated
- Consider pain management
- Seek surgery for chronic cases
Consult a doctor for proper diagnosis and tailored treatment.
Hemorrhoids
Hemorrhoids are very common. Nearly three from 4 adults will have hemorrhoids from time to time. Often they don’t cause symptoms but at other times they cause itching, discomfort and bleeding. They may arise from straining during bowel movements or from the increased pressure on these veins during pregnancy. Hemorrhoids might be located inside the anus (internal hemorrhoids), or they may establish under the skin around the rectum (external hemorrhoids).
Hemorrhoids Treatment Guide
- Use topical treatments: creams, ointments, suppositories
- Take pain relievers: ibuprofen, acetaminophen
- Apply ice packs to reduce swelling
- Soak in a warm bath
- Keep the area clean
- Use moist towelettes instead of dry toilet paper
- Increase fiber intake
- Drink plenty of fluids
- Consider minimally invasive procedures if severe
Anal Cancer
Often anal cancer causes no symptoms at all. But bleeding is typically the first sign of the disease. The bleeding is typically small. In the beginning, most people assume the bleeding is brought on by hemorrhoids (painful, swollen veins in the rectum and anus that might bleed). They are a benign and relatively typical cause of rectal bleeding. Important symptoms of anal cancer consist of: rectal bleeding, rectal itching, a lump or mass at the anal opening, pain or a feeling of fullness in the anal area, etc.
Anal Cancer Treatment
- Consult an Oncologist: For personalized treatment options.
- Surgery: Removes localized tumors.
- Chemotherapy: Uses drugs to destroy cancer cells.
- Radiotherapy: Targets radiation to kill cancerous tissues.
- Follow-up Care: Regular monitoring and supportive therapies.
Seek specialist advice for a tailored approach.
Health Support: This high-absorption Magnesium Glycinate (200 mg) is gentle on the stomach and supports muscle relaxation, better sleep, and metabolic health. You can find this trusted formula on Amazon.
Colon Cancer
Colorectal cancer takes place when the cells that line the colon or the rectum become unusual and grow out of control. Due to the fact that symptoms often do not appear until the cancer has advanced, it is very important to have regular colorectal cancer screenings. Nevertheless, most colorectal cancers are associated with signs or symptoms. Among the early signs of colorectal cancer is bleeding. However, tumors typically bleed only percentages, on and off, so that proof of the blood is discovered only during chemical testing of the stool, which is called a fecal occult blood test.
Treatment Methods for Colon Cancer
To treat colon cancer, a multidisciplinary approach is essential. Treatment options include:
- Surgical resection of the tumor
- Chemotherapy to kill cancer cells
- Radiation therapy to target cancerous areas
- Targeted drug therapy for specific cancer mutations
- Immunotherapy to boost the immune system’s response against cancer cells
Consult an oncologist for a personalized treatment plan.
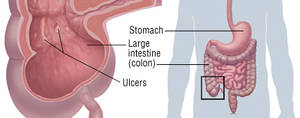
Ulcerative Colitis (Crohn’s Disease)
Crohn disease is an inflammatory bowel disease where chronic inflammation normally includes the lower part of the little intestinal tract, the large intestine, or both and may impact any part of the digestive tract.
Bleeding from the anus is more common in ulcerative colitis than it remains in Crohn’s disease. Ulcerative colitis frequently involves the anus. Because the anus is at the end of the big intestinal tract, blood from this source is rather noticeable in or on the stool. Bleeding likewise accompanies ulcerative colitis due to the fact that this form of IBD attacks the lining of the big intestinal tract.
The ulcers that form in the mucosa of the large intestinal tract have the tendency to bleed. Sometimes, bleeding from ulcerative colitis can result in considerable blood loss. The ultimate objective of treatment will be to soothe the inflammation and stop the bleeding, but dealing with the loss of blood might likewise be necessary.
Treatment Methods for Ulcerative Colitis
- Medication: Aminosalicylates, corticosteroids, and immunosuppressants manage inflammation.
- Biologics: Target specific pathways in the immune system.
- Diet Modification: Low-fiber and lactose-free diets may alleviate symptoms.
- Surgery: Colectomy for severe cases.
- Supportive Care: Hydration and nutritional supplements.
Consult a gastroenterologist for personalized treatment.
Proctitis
Proctitis is a condition in which the lining tissue of the inner rectum becomes inflamed. The anus becomes part of your lower digestive system. It links the last part of your colon to your anus. Stool travels through your anus as it exits your body. Proctitis can be painful and uncomfortable. You might feel a consistent desire to defecate. The condition is typically treated with medications and lifestyle modifications. Surgery isn’t really generally required, other than in the most severe, repeating cases.
Treatment Methods for Proctitis
- Medications:
- Topical corticosteroids: Reduce inflammation and provide symptom relief.
- Oral antibiotics: Treat infections causing proctitis.
- Immunomodulators: Suppress the immune system to manage chronic cases.
- Lifestyle modifications:
- Dietary changes: Avoid trigger foods and increase fiber intake to alleviate symptoms.
- Stress management: Engage in relaxation techniques and seek support to reduce stress-related flare-ups.
- Sitz baths:
- Soaking the affected area in warm water several times a day can promote healing and relieve discomfort.
- Surgery:
- In severe cases, surgical intervention may be necessary to remove damaged tissues or repair rectal complications.
- Complementary therapies:
- Probiotics: Introduce beneficial bacteria to restore gut health.
- Herbal remedies: Aloe vera and chamomile have anti-inflammatory properties.
Solitary Rectal Ulcer
Solitary rectal ulcer syndrome is a condition that takes place when one or more open sores (ulcers) establish in the rectum. The anus is a muscular tube that’s linked to the end of your colon. Stool goes through the rectum on its method out of the body. Singular rectal ulcer syndrome is an unusual and improperly understood disorder that frequently occurs in people with chronic constipation. Singular rectal ulcer syndrome can cause rectal bleeding and straining during defecation. Regardless of its name, often more than one rectal ulcer happens in singular rectal ulcer syndrome.
Treating Solitary Rectal Ulcers
- Consult a healthcare provider for an accurate diagnosis and treatment plan.
- Dietary modifications with increased fiber and fluid intake may alleviate constipation.
- Topical medications, such as steroid creams, can help reduce inflammation.
- Sitz baths and warm compresses can soothe symptoms.
- In severe cases, surgical intervention may be necessary. Regular follow-ups ensure effective management.
Conclusion
Do not hesitate to visit your doctor for proper diagnosis procedure and to get correct treatment for the issue.