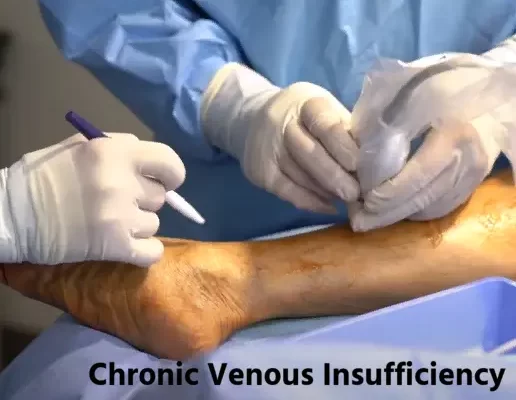
Meet Carlos, a 52-year-old office worker who spends most of his day seated at a desk. Over the last year, he’s noticed that his legs have become increasingly swollen by the end of the day, and there’s a heavy, aching sensation that won’t go away. Eventually, Carlos notices dark patches on his skin around his ankles, and that’s when he decides it’s time to see a doctor. After a thorough evaluation, he learns that he’s suffering from Chronic Venous Insufficiency (CVI).
Symptom Breakdown: What is Chronic Venous Insufficiency?
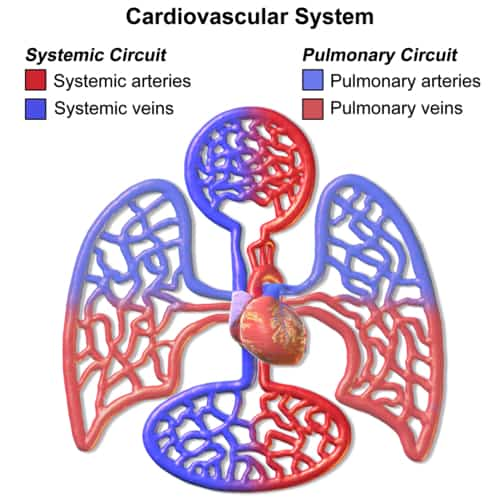
Chronic venous insufficiency is a condition where the veins in your legs have difficulty sending blood back to the heart. When these veins fail, blood pools in the lower extremities, leading to a range of symptoms, including:
- Swelling in the legs (also called edema), especially after long periods of sitting or standing.
- Heaviness and aching in the legs, which can get worse as the day goes on.
- Skin changes, such as darkened patches around the ankles or reddish-brown spots.
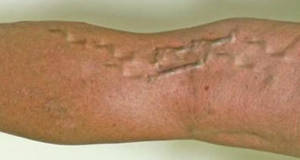
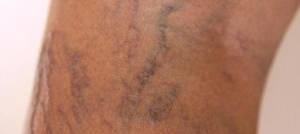
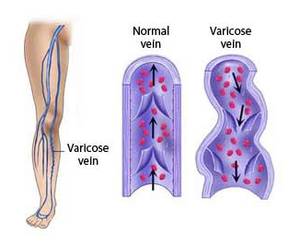
- Varicose veins, which appear swollen and twisted just under the skin.
- Ulcers or open sores on the legs that are slow to heal.
If left untreated, CVI can lead to more serious complications, such as leg ulcers and deep vein thrombosis (DVT).
Diagnostic Path: How Does Chronic Venous Insufficiency Develop?
Chronic venous insufficiency occurs when the valves inside the veins—usually responsible for pushing blood upward toward the heart—become weak or damaged. This leads to blood flowing backward and pooling in the legs. Several factors increase the risk of developing CVI, including:
Health Support: This Vitamin K2 + D3 Complex is essential for bone density, cardiovascular health, and immune function. It’s a highly-rated formula for those looking to maintain optimal nutrient levels. You can find it on Amazon.
- Prolonged Sitting or Standing:
Occupations that require long periods of sitting or standing, such as office work, retail, or factory jobs, can contribute to the weakening of venous valves. - Obesity:
Excess body weight places additional pressure on the veins in the lower extremities, increasing the risk of developing CVI. - Age and Genetics:
As people age, their vein walls and valves naturally weaken, which can lead to CVI. Genetics also play a significant role, as some people are more predisposed to venous conditions due to family history. - Pregnancy:
The increased blood volume and pressure during pregnancy can sometimes lead to chronic venous insufficiency, especially in women who have multiple pregnancies. - Deep Vein Thrombosis (DVT):
A history of DVT, where a blood clot forms in a deep vein, can damage the venous valves and lead to chronic venous insufficiency over time.
Deep Dive: The Importance of Early Diagnosis
Early diagnosis of chronic venous insufficiency is key to preventing further complications. If left untreated, CVI can result in venous ulcers—painful, open sores that develop on the skin and are difficult to heal. These ulcers can significantly affect quality of life, making it harder to walk and perform daily activities.
Doctors typically use duplex ultrasound to assess the blood flow in your veins and to determine how well your venous valves are functioning. Once CVI is confirmed, treatment options are discussed to manage symptoms and improve blood flow.
Treatment Comparison: Managing Chronic Venous Insufficiency
While chronic venous insufficiency cannot always be completely cured, there are effective treatments available that can alleviate symptoms and prevent further damage. Here are the main approaches:
- Compression Therapy:
- Compression stockings are often the first line of defense in managing CVI. These specialized socks help improve circulation by squeezing the legs, allowing the veins to move blood back toward the heart more efficiently.
- Lifestyle Changes:
- Exercise: Regular walking or swimming can strengthen the muscles that support your veins and improve circulation. Aim for activities that get your legs moving but don’t put excessive strain on them.
- Weight Management: Maintaining a healthy weight can reduce the pressure on your legs and help prevent the worsening of CVI.
- Elevating Legs: Elevating your legs above heart level for short periods during the day can help reduce swelling and discomfort.
- Minimally Invasive Procedures:
- Sclerotherapy: A procedure where a chemical is injected into varicose veins, causing them to collapse and fade away over time.
- Endovenous laser treatment (EVLT): A minimally invasive procedure that uses laser energy to close off problematic veins.
- Radiofrequency ablation (RFA): Similar to EVLT, this procedure uses heat to seal off damaged veins.
- Surgical Interventions:
- In more severe cases of chronic venous insufficiency, surgery might be required to remove or tie off damaged veins, improving blood flow and reducing symptoms.
Outcome Story: Finding Relief
Let’s look at another case—Maria, a 47-year-old teacher who spent long hours standing in front of her classroom. Over time, she developed swelling and discoloration in her legs. After consulting her physician, Maria was diagnosed with chronic venous insufficiency. Following her doctor’s advice, she started wearing compression stockings and incorporated daily walking into her routine. Within a few months, Maria noticed significant relief from the aching and swelling in her legs. Her quality of life improved, and she was able to enjoy her daily activities again.
Health Support: This high-absorption Magnesium Glycinate (200 mg) is gentle on the stomach and supports muscle relaxation, better sleep, and metabolic health. You can find this trusted formula on Amazon.
Conclusion: Don’t Ignore the Signs of Chronic Venous Insufficiency
Chronic venous insufficiency is a progressive condition, but with early diagnosis and the right treatment plan, it’s possible to manage the symptoms and prevent further complications. If you’re experiencing signs like leg swelling, varicose veins, or skin changes, don’t wait—speak to a healthcare professional to explore the best course of treatment.
With options ranging from compression therapy to minimally invasive procedures, you can regain comfort and confidence, while protecting your legs from future complications.