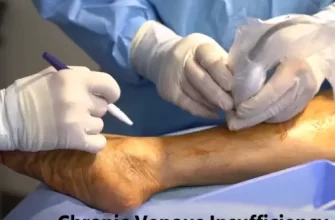
Venous insufficiency refers to a situation in which the veins encounter difficulties in transporting blood from the extremities back to the heart.
- This situation has the potential to cause different types of health issues, including varicose veins, swelling, and ulcers on the legs.
- It affects daily living by causing discomfort, pain, and mobility issues.
- The severity of the symptoms can signal the urgency to seek medical attention and possibly prevent further complications.
Common Risk Factors Associated With Venous Insufficiency
- Age: The risk of developing venous insufficiency increases as a person gets older due to the natural weakening of venous walls.
- Gender: Women are more likely than men to develop the condition, possibly due to hormonal changes and pregnancy.
- Family History: Genetics play a role in the predisposition to venous insufficiency. A family history of the condition increases one’s risk.
- Obesity: Excess weight can put additional pressure on the veins, leading to venous disorders.
- Lifestyle: People who lead sedentary lifestyles or those who stand or sit for long periods are at higher risk.
- Previous Leg Injuries: Injury to the leg can damage the veins and lead to insufficiency.
Individuals can effectively manage symptoms and seek early treatment by gaining knowledge about the risk factors and consequences associated with venous insufficiency.
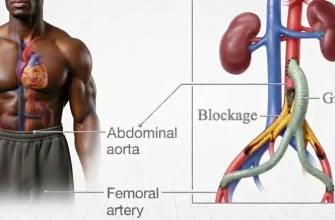
Causes
- When the valves in the veins are damaged or weakened, it leads to a condition called venous insufficiency.
- Blood flow becomes hindered, causing blood to pool in the lower extremities.
- The condition can be due to factors such as chronic high blood pressure inside leg veins, leading to valve damage.
Genetic factors and family history
- Research suggests that there may be a genetic component, as the condition often occurs within families.
- Specific gene mutations have been linked to an increased risk of venous insufficiency.
Lifestyle choices and habits that contribute to venous insufficiency
- Lack of physical activity may cause the leg muscles to lose strength. These muscles are crucial in aiding vein function and blood flow.
- Prolonged standing or sitting can cause blood to pool due to gravity and inadequate muscle support.
- Dietary habits leading to obesity are also significant contributors, as they increase the strain on the circulatory system.
Understanding the combination of causes, from genetic predispositions to lifestyle factors, professionals can develop more targeted prevention and treatment strategies for venous insufficiency.
Symptoms
Identifying venous insufficiency involves being aware of a range of signs and symptoms that typically affect the legs. These symptoms can range from mild to severe and may worsen over the course of the day, especially after prolonged periods of sitting or standing.
Health Support: This Vitamin K2 + D3 Complex is essential for bone density, cardiovascular health, and immune function. It’s a highly-rated formula for those looking to maintain optimal nutrient levels. You can find it on Amazon.
Pain, swelling, and heaviness in the legs
- Individuals with venous insufficiency often experience a sense of heaviness or fatigue in their legs.
- Swelling, known medically as edema, can prominently occur in the lower legs and ankles due to fluid accumulation.
- Pain, which can manifest as an aching or cramping sensation, is also commonly reported and can be exacerbated by extended periods of immobility.
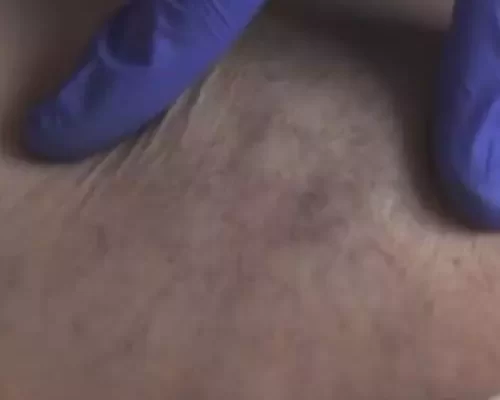
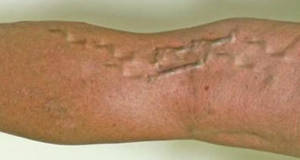
Skin changes and ulcers
- Skin changes are a noticeable symptom, with the skin overlying the affected veins becoming darker and taking on a leathery appearance.
- Varicose veins may be visible, characterized by bulging, bluish veins under the skin’s surface.
- In severe cases, venous insufficiencies can lead to the development of ulcers, typically around the ankles. These ulcers can take a long time to heal and are susceptible to infection.
Recognizing these symptoms promptly allows for earlier intervention, which can help manage the condition and reduce the risk of complications.
Methods for diagnosing venous insufficiency
To diagnose venous insufficiency, physicians employ various techniques, ensuring a thorough assessment to determine the presence and severity of the condition.
Physical examination and medical history
- Doctors will typically begin with a physical examination, assessing the legs for visible symptoms like swelling, discoloration, and varicose veins.
- A comprehensive medical history is taken to identify risk factors such as family history, previous leg injuries, or instances of deep vein thrombosis.
- Lifestyle factors and symptoms are discussed to gather a complete picture of the patient’s health status.
Ultrasound imaging and other diagnostic tests
- Duplex ultrasound is a non-invasive test that is commonly used to evaluate blood flow and the structure of the leg veins.
- This imaging modality can help detect blockages or clotting issues that are characteristic of venous insufficiency.
- In some cases, additional tests may be required to further investigate the extent of venous disease.
Accurate diagnosis is crucial for creating an effective treatment plan and preventing the progression of venous insufficiency to more severe complications.
Treatment
Following a diagnosis of venous insufficiency, several treatment options are available depending on the severity of the condition. Patients benefit from individualized approaches that target the underlying causes to alleviate symptoms and prevent complication.
Health Support: This high-absorption Magnesium Glycinate (200 mg) is gentle on the stomach and supports muscle relaxation, better sleep, and metabolic health. You can find this trusted formula on Amazon.
Compression therapy and wearing compression stockings
- Compression stockings are often the first-line treatment, providing pressure on the legs to improve blood flow and reduce swelling.
- Physicians may recommend different levels of compression based on the condition’s severity.
- Regular use of compression stockings can significantly ease discomfort and slow disease progression.
Endovenous therapy and minimally invasive procedures
- Endovenous laser therapy (EVLT) and radiofrequency ablation (RFA) are modern treatments that close off unhealthy veins.
- These procedures are minimally invasive, require local anesthesia, and offer quick recovery times.
- Patients with advanced venous insufficiency might undergo sclerotherapy or phlebectomy for more comprehensive management.
It is vital for individuals with venous insufficiency to seek medical guidance and adhere to prescribed treatments to ensure optimal outcomes and maintain life quality.
Prevention
To mitigate the risk of venous insufficiency, individuals can adopt various preventive strategies. While genetic factors may play a role, lifestyle choices significantly influence the development and progression of this condition.
Maintaining a healthy weight and regular exercise
- A healthy body weight reduces pressure on the veins, thereby decreasing the likelihood of blood pooling in the legs.
- Regular exercise, especially activities such as walking or swimming, enhances circulation and vein strength.
- Building leg muscle through exercise also contributes to improved blood flow.
Avoiding prolonged sitting or standing
- Prolonged stationary positions can contribute to vein stress and the development of venous issues.
- It is advised to take frequent breaks to stretch or walk around, which helps stimulate blood flow.
- Elevating the legs when sitting and ensuring proper posture support vein health.
By integrating these preventive measures into daily routines, individuals can protect against the onset of venous insufficiency and maintain vascular health for the long term.
Medications for Venous Insufficiency
Venous insufficiency is a condition that can considerably affect an individual’s quality of life. To manage symptoms and progression, a physician might recommend various medications.
Topical creams and ointments
- Anti-inflammatory creams: Applied directly to the skin, these can reduce swelling and discomfort.
- Heparinoid creams: Used to alleviate symptoms by thinning blood and improving circulation near the surface of the skin.
- Moisturizers: Help prevent skin breakdown, which can occur due to chronic venous insufficiency.
Oral medications to improve venous circulation
- Diuretics: Often prescribed to decrease fluid retention, reducing swelling in the legs.
- Pentoxifylline: Increases blood flow by making the blood less thick, mitigating some of the symptoms associated with venous insufficiency.
- Horse chestnut seed extract: A natural remedy that may reduce leg swelling and other symptoms when used as a part of a treatment plan.
By using these medications under medical supervision, patients can manage their symptoms effectively and reduce the impact of chronic venous insufficiency on their daily lives.
Conclusion
Venous insufficiency is a chronic condition impacting circulation, primarily in the legs. The management of this condition includes a multifaceted approach consisting of lifestyle changes, supportive measures, and a regimented use of medications. Here is a summary:
- Topical treatments: These offer symptomatic relief through anti-inflammatory agents and heparinoid creams, reducing swelling and improving local blood flow. Moisturizers prevent skin complications.
- Oral medications: Diuretics are key for reducing edema, and pentoxifylline serves to decrease blood viscosity to aid circulation. Additionally, horse chestnut seed extract offers a natural approach to symptom management.
- Physician oversight: Crucial in monitoring response to treatment and adjusting therapies to ensure effectiveness and reduce potential side effects.
By adhering to prescribed treatments and maintaining regular consultations, individuals with venous insufficiency can lead a more comfortable life, minimizing the impact and complications associated with this chronic vascular condition.