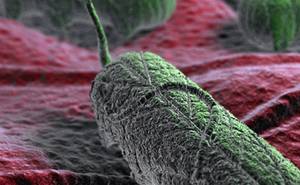
Methicillin-resistant Staphylococcus aureus (MRSA) infection is caused by a type of staph bacteria that’s ended up being resistant to a lot of the antibiotics used to deal with regular staph infections.
Most MRSA infections occur in individuals who’ve been in health centers or other health care settings, such as nursing houses and dialysis centers. When it occurs in these settings, it’s referred to as health care-associated MRSA (HA-MRSA). HA-MRSA infections usually are related to invasive procedures or devices, such as surgical treatments, intravenous tubing or artificial joints.
Another type of MRSA infection has happened in the wider neighborhood – among healthy people. This form, community-associated MRSA (CA-MRSA), often starts as an unpleasant skin boil. It’s spread by skin-to-skin contact. At-risk populations include groups such as wrestlers, childcare employees and people who live in congested conditions.
Health Support: This Vitamin K2 + D3 Complex is essential for bone density, cardiovascular health, and immune function. It’s a highly-rated formula for those looking to maintain optimal nutrient levels. You can find it on Amazon.
Symptoms of Early MRSA Infection
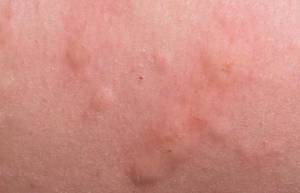
Staph skin infections, consisting of early MRSA, typically begin as inflamed, agonizing red bumps that might appear like pimples or spider bites. The affected area might be:
- Warm to the touch
- Filled with pus or other drainage
- Accompanied by a fever
Early MRSA symptoms and signs can rapidly become deep, unpleasant abscesses that require medical draining. Sometimes the bacteria remain restricted to the skin. However they can also burrow deep into the body, causing possibly deadly infections in bones, joints, medical injuries, the blood stream, heart valves and lungs.
When to see a doctor
Keep an eye on small skin problems – pimples, insect bites, cuts and scrapes – specifically in children. If wounds appear infected or are accompanied by a fever, see your doctor.
Early Stages of MRSA
In the early stages, a MRSA infection might be puzzled with a pimple or a spider bite. Over 24 to 48 hours, the affected area becomes more painful and swollen. Often an abscess or fluid collection will establish underneath the skin and in some cases this abscess starts to drain by itself, states Iytmed.com. While 75 percent of MRSA infections involve the skin, more serious and possibly life-threatening infections can include the heart, spinal cord and brain.
Health Support: This high-absorption Magnesium Glycinate (200 mg) is gentle on the stomach and supports muscle relaxation, better sleep, and metabolic health. You can find this trusted formula on Amazon.
While billions of bacteria live on everybody’s skin, roughly 2.5 percent of children in the United States bring the MRSA bacteria on their skin. These people are at specific risk of developing a MRSA skin infection if they have an abrasion or cut.
The occurrence of MRSA infections has increased drastically over the last 40 years both within the medical facility setting and in the community. In 1972, just 2 percent of infections in American extensive care units were brought on by MRSA. By 1995, this had actually increased to 22 percent, and a decade later on to 64 percent. Another research study revealed that 14 million healthcare gos to associated with staph skin infections were tape-recorded in 2005; most of these infections were brought on by the MRSA bacteria.
Causes of MRSA Infection
Different ranges of Staphylococcus aureus bacteria, commonly called “staph,” exist. Staph bacteria are generally discovered on the skin or in the nose of about one-third of the population. The bacteria are typically harmless unless they get in the body through a cut or other injury, as well as then they typically cause only minor skin problems in healthy people.
According to the Centers for Disease Control and Prevention, less than 2 percent of the population chronically brings the type of staph bacteria known as MRSA.
MRSA and Antibiotic Resistance
MRSA is the result of decades of typically unnecessary antibiotic usage. For several years, antibiotics have actually been prescribed for colds, flu and other viral infections that do not react to these drugs. Even when prescription antibiotics are used properly, they add to the rise of drug-resistant bacteria because they don’t ruin every germ they target. Bacteria survive an evolutionary fast lane, so germs that survive treatment with one antibiotic soon discover how to resist others.
Since medical facility and community stress of MRSA typically happen in different levels, the risk factors for the two strains vary.
Risk factors for HA-MRSA
- Being hospitalized. MRSA remains a concern in health centers, where it can attack those most vulnerable– older adults and individuals with weakened immune systems.
- Having an invasive medical device. Medical tubing– such as intravenous lines or urinary catheters– can offer a path for MRSA to take a trip into your body.
- Residing in a long-lasting care center. MRSA prevails in nursing houses. Providers of MRSA have the ability to spread it, even if they’re not sick themselves.
Risk factors for CA-MRSA
- Participating in contact sports. MRSA can spread out quickly through cuts and abrasions and skin-to-skin contact.
- Residing in crowded or unsanitary conditions. Break outs of MRSA have actually happened in basic training camps, child care centers and prisons.
- Men making love with men. Homosexual men have a higher danger of developing MRSA infections.
Complications
MRSA infections can withstand the effects of numerous common prescription antibiotics, so they are harder to deal with. This can permit the infections to spread and often end up being dangerous.
MRSA infections may influence your:
- Blood stream
- Lungs
- Heart
- Bones
- Joints
Tests and diagnosis
Physicians detect MRSA by inspecting a tissue sample or nasal secretions for signs of drug-resistant bacteria. The sample is sent out to a laboratory where it’s placed in a dish of nutrients that motivate bacterial growth. But since it takes about 48 hours for the bacteria to grow, more recent tests that can discover staph DNA in a matter of hours are now ending up being more widely available.
Treatments for MRSA Infections
Both health care-associated and community-associated strains of early MRSA still react to specific antibiotics. Sometimes, antibiotics may not be essential. For example, physicians might drain a superficial abscess triggered by MRSA instead of treat the infection with drugs.
Diet Tips to Fight with MRSA
- Eat foods that increase your body immune system. ABC Health recommends drinking kefir, a fermented yogurt that contains probiotics – helpful bacteria that enhance your immune system by assisting your body produce white blood cells. Unlike the bacteria in yogurt, which travel through your system, the bacteria in kefir colonize in your digestive tract.
- Add turmeric to your diet. Turmeric contains curcumin, which offers the spice its golden yellow color. Curcumin is an anti-inflammatory with antiseptic properties and may even be used topically with superficial cases of MRSA.
- Eat more garlic, which contains allicin, a powerful anti-oxidant that assists your body detoxify itself. Garlic increases the production of antibodies and stimulates the production of white blood cells that battle infection.
- Follow a well balanced diet that consists of a variety of fruits, vegetables, nuts and seeds. Consuming foods high in vitamin C, such as citrus fruits, strawberries, kiwi and red bell peppers increases the quantity of interferon in your system, the antibody that coats cell surfaces, preventing the entry of damaging bacteria. Vitamins A and E also promote the production of T-cells and support your immune system. Sources of vitamins E and A consist of nuts, seeds, vegetable oils, sweet potatoes and carrots.
- Quit alcohol and avoid refined sugar, both of which reduce immune system function. According to Dr. William Sears, consuming 8 tbsp. of sugar, the amount in two cans of soda, might “decrease the ability of white blood cells to kill bacteria by 40 percent.” Consuming 3 or more glasses of alcohol might minimize your white blood cells’ capability to increase and harm your body immune system.
Preventing HA-MRSA
In the hospital, individuals who are infected or colonized with MRSA typically are positioned in contact precautions as a measure to prevent the spread of MRSA. Visitors and health care workers looking after people in seclusion might be required to wear protective garments and have to follow strict hand health procedures. Infected surfaces and laundry items must be properly decontaminated.
Preventing CA-MRSA
- Wash your hands. Careful hand washing stays your best defense versus germs. Scrub hands quickly for a minimum of 15 seconds, then dry them with a non reusable towel and usage another towel to switch off the faucet.
- Keep injuries covered. Keep cuts and abrasions clean and covered with sterilized, dry bandages until they heal. The pus from infected sores might contain MRSA, and keeping injuries covered will assist avoid the bacteria from dispersing.
- Keep personal products individual. Prevent sharing individual products such as towels, sheets, razors, clothes and athletic equipment. MRSA spreads on infected objects in addition to through direct contact.
- Shower after athletic games or practices. Shower right away after each game or practice. Use soap and water. Don’t share towels.
- Sterilize linens. If you have a cut or sore, wash towels and bed linens in a washing machine set to the hottest water level (with included bleach, if possible) and dry them in a hot clothes dryer. Wash health club and athletic clothes after each using.