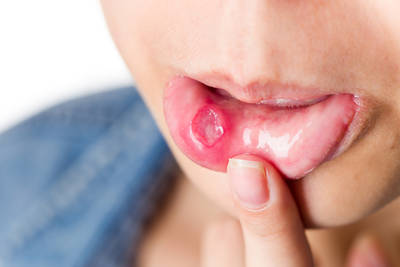
Mouth ulcers hurt round or oval sores that form in the mouth, usually on the inside of the cheeks or lips. They’re generally white, red, yellow or grey in colour and are inflamed (red and inflamed) around the edge.
Although mouth ulcers can be uneasy, particularly when you eat, consume or brush your teeth, they are generally safe.
The majority of mouth ulcers will clear up on their own within a week or more. You just have to see your GP or dental expert if the ulcer worsens or lasts for longer than three weeks, or if you establish ulcers frequently.
How common are mouth ulcers?
Mouth ulcers are typical, especially in ladies and young adults. Many people will have one or two a year.
Health Support: This Vitamin K2 + D3 Complex is essential for bone density, cardiovascular health, and immune function. It’s a highly-rated formula for those looking to maintain optimal nutrient levels. You can find it on Amazon.
However, some individuals have mouth ulcers that return frequently. Recurrent mouth ulcers are estimated to influence about one in every five people in the UK.
What causes mouth ulcers?
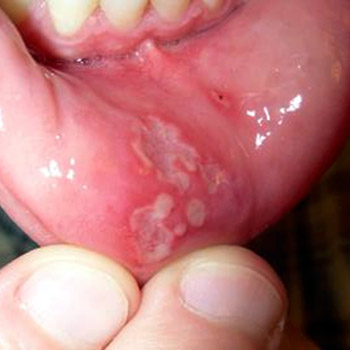
The majority of small, single mouth ulcers are caused by damage to the mouth, for example by inadvertently biting the inside of your cheek while consuming, or from a sharp tooth, food or filling.
The cause of a frequent mouth ulcer is not always clear, but it’s likely to be a combination of aspects including a hereditary vulnerability and a specific trigger. Possible triggers might consist of sensation stressed or distressed, eating particular foods, hormonal modifications and stopping smoking cigarettes.
In some cases, persistent mouth ulcers suggest an underlying health condition, such as iron shortage anaemia or Crohn’s condition.
Health Support: This high-absorption Magnesium Glycinate (200 mg) is gentle on the stomach and supports muscle relaxation, better sleep, and metabolic health. You can find this trusted formula on Amazon.
Mouth ulcers can sometimes be caused by a medication you are taking or treatment you are having, such as:
- non-steroidal anti-inflammatory drugs (NSAIDs) – such as ibuprofen and aspirin
- nicorandil – a medication sometimes made use of to treat angina
- beta-blockers – medicationsused to deal with a variety of conditions that influence the heart and blood flow, such as angina, high blood pressure and abnormal heart rhythms
- chemotherapy and radiotherapy – two common cancer treatments
You may notice that you begin to get mouth ulcers when you begin your treatment, or when your dosage is increased.
Speak to your GP or care group if you believe your treatment is causing your mouth ulcers. You might have the ability to take an alternative medication or you may be offered medication to deal with the ulcers till you finish your course of treatment.
Treatment
How to treat mouth ulcers
Most mouth ulcers don’t need particular treatment, as they will usually recover on their own within 10-14 days.
However, treatment may be needed if your ulcers are severe, uncomfortable or interfere with your daily activities (such as consuming).
If your mouth ulcers are thought to be the result of a hidden condition, you may have to be described a specialist so the condition can be dealt with.
Self-help suggestions
If you have a moderate mouth ulcer, there are some steps you can take yourself to assist your ulcer heal quicker:
- Make use of a soft tooth brush when brushing your teeth.
- Prevent hard, sharp, spicy and acidic foods and drinks till the ulcer heals– stay with soft foods that are easier to chew.
- Prevent things that you believe might be triggering your ulcers, such as particular foods. Read about the causes of mouth ulcers to find out more about potential triggers.
If your ulcer has a particular physical cause, such as a sharp tooth or filling cutting the inside of your cheek, it will usually heal naturally when the cause has been treated. If you suspect that a sharp tooth or filling has caused an ulcer, visit your dentist so that they can fix it.
Medication
If needed, your GP or dental professional can recommend medication that may help alleviate your symptoms.
Some mouth ulcer treatments can likewise be bought without a prescription from your local pharmacy, although you must speak with your pharmacist about which medicine might be best for you. Some treatments aren’t appropriate for youngsters or for ladies who are pregnant, breastfeeding or attempting to get pregnant.
The main treatments for mouth ulcers are explained listed below, although the proof supporting their use is restricted. These treatments likewise won’t stop you establishing brand-new mouth ulcers in the future.
Corticosteroids
- Corticosteroids are a type of medication that minimizes swelling. They can help in reducing pain associated with mouth ulcers and assist them recover much faster.
- Corticosteroids are readily available in many different kinds, including mouthwashes and sprays.
You should talk to your GP for guidance prior to making use of corticosteroid medications for mouth ulcers in youngsters under 12 years of ages.
Antimicrobial mouthwash
Antimicrobial mouthwash helps kill bacteria, viruses or fungi that could contaminate the ulcer, especially if an agonizing mouth ulcer indicates you are not able to brush your teeth appropriately. They may also help accelerate recovery.
Chlorhexidine gluconate is the most typically recommended mouthwash, although numerous gels and sprays are also readily available.
Chlorhexidine gluconate is normally utilized two times a day. After using chlorhexidine gluconate, you might notice that your teeth are covered in a brown stain. This staining is not permanent, and your teeth need to go back to their normal colour once you finish the treatment.
The best way to avoid staining is to brush your teeth before using chlorhexidine gluconate mouthwash. Nevertheless, after brushing your teeth make sure that you completely rinse your mouth out with water prior to utilizing the mouthwash.
Chlorhexidine gluconate mouthwash must not be used by infants under two years of ages.
Painkillers
If your mouth ulcer is very unpleasant, your GP may prescribe a painkiller that you can use straight to your ulcer. These are offered as mouthwashes, sprays, lozenges and gels.
Your GP will normally prescribe benzydamine, which is readily available as a mouthwash or spray. However, the mouthwash is not suitable for youngsters under 12 years of age and should not typically be used for more than seven days in a row.
Benzydamine mouthwashes and sprays might also sting when you first utilize them, but this must decrease as you remain to use them. You may discover it helpful to weaken the mouthwash with an equal amount of money of water prior to using it if stinging is a problem. If the stinging continues, your pharmacist or GP may recommend stopping treatment.
You may also discover that your mouth feels numb when you first use enzydamine mouthwashes and sprays. This is typical and the feeling will quickly go back to your mouth.
Can mouth ulcers be prevented?
As the exact cause of a lot of reoccurring mouth ulcers is unknown, there is no certain way to prevent them. However, the following may help in reducing your threat of establishing mouth ulcers:
- avoid harming the within your mouth by utilizing a soft toothbrush and avoiding hard, fragile or sharp-edged foods
- avoid things you think might be activating your ulcers, such as certain foods
find out some relaxation ideas to relieve tension - ensure you preserve excellent oral health, including brushing your teeth at least twice a day
- have regular check-ups at your dentist– your dentist can find and treat problems, such as sharp teeth or fillings, that could damage your mouth
- eat a healthy, balanced diet rich in vitamins
Mouth ulcers are commonly uncomfortable however they generally clear up by themselves within a couple of weeks.
Could it be mouth cancer?
In a few cases, a lasting mouth ulcer can be a sign of mouth cancer. Ulcers triggered by mouth cancer generally appear on or under the tongue, although they can appear somewhere else in the mouth.
You are more at threat of establishing mouth cancer if you are male, over 45 years of ages and you smoke or drink heavily.
If mouth cancer is spotted early, the opportunities of a full recovery are great. This is why it is always vital to have routine check-ups with your dental professional. They can carry out an extensive evaluation of your teeth and mouth, and will be able to spot any possible signs of mouth cancer.