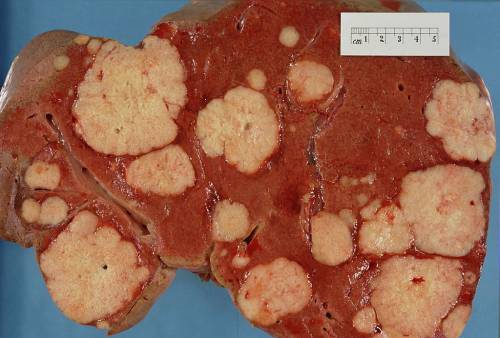
Pancreatic cancer (also known as pancreatitis cancer) starts in the tissues of your pancreas – an organ in your abdomen that lies horizontally behind the lower part of your stomach. Your pancreas releases enzymes that help digestion and hormonal agents that assist handle your blood sugar.
What Is Pancreatic Cancer?
Pancreatic cancer generally spreads out rapidly to close-by organs. It is seldom discovered in its early stages. However for people with pancreatic cysts or a family history of pancreatic cancer, some screening steps might help spot an issue early. One sign of pancreatic cancer is diabetes, specifically when it occurs with weight-loss, jaundice or pain in the upper abdominal area that spreads to the back.
Treatment might consist of surgery, chemotherapy, radiation therapy or a combination of these.
Pancreatic Cancer Symptoms
Signs and symptoms of pancreatic cancer frequently do not happen till the disease is advanced. They might consist of:
Health Support: This Vitamin K2 + D3 Complex is essential for bone density, cardiovascular health, and immune function. It’s a highly-rated formula for those looking to maintain optimal nutrient levels. You can find it on Amazon.
- Pain in the upper abdomen that radiates to your back
- Loss of appetite or unexpected weight-loss
- Anxiety
- New-onset diabetes
- Embolism
- Fatigue
- Yellowing of your skin and the whites of your eyes (jaundice).
When to see a doctor
See your doctor if you experience unexplained weight reduction or if you have persistent fatigue, abdominal pain, jaundice, or other symptoms and signs that bother you. Numerous conditions can cause these symptoms, so your doctor may check for these conditions in addition to for pancreatic cancer.
Pancreatic Cancer Causes
It’s unclear what causes pancreatic cancer most of the times. Doctors have actually determined aspects, such as smoking, that increase your risk of establishing the disease.
Understanding your pancreas
Your pancreas is about 6 inches (15 centimeters) long and looks something like a pear lying on its side. It releases (produces) hormones, consisting of insulin, to help your body procedure sugar in the foods you eat. And it produces digestive juices to assist your body absorb food.
Health Support: This high-absorption Magnesium Glycinate (200 mg) is gentle on the stomach and supports muscle relaxation, better sleep, and metabolic health. You can find this trusted formula on Amazon.
How pancreatic cancer forms
Pancreatic cancer takes place when cells in your pancreas develop anomalies in their DNA. These mutations cause cells to grow uncontrollably and to continue living after normal cells would pass away. These collecting cells can form a growth. Untreated pancreatic cancer spreads to nearby organs and blood vessels.
Many pancreatic cancer starts in the cells that line the ducts of the pancreas. This kind of cancer is called pancreatic adenocarcinoma or pancreatic exocrine cancer. Seldom, cancer can form in the hormone-producing cells or the neuroendocrine cells of the pancreas. These types of cancer are called islet cell tumors, pancreatic endocrine cancer and pancreatic neuroendocrine tumors.
Risk Factors
Aspects that may increase your risk of pancreatic cancer consist of:
- Chronic inflammation of the pancreas (pancreatitis).
- Diabetes.
- Family history of hereditary syndromes that can increase cancer risk, consisting of a BRCA2 gene mutation, Lynch syndrome and familial irregular mole-malignant cancer malignancy (FAMMM) syndrome.
- Family history of pancreatitis cancer.
- Smoking cigarettes.
- Weight problems.
- Older age, as the majority of people are diagnosed after age 65.
A large study showed that the combination of smoking, long-standing diabetes and a poor diet increases the risk of pancreatic cancer beyond the risk of any one of these factors alone.
Pancreatic Cancer Complications
As pancreatic cancer progresses, it can cause complications such as:
Weight-loss. A number of aspects may cause weight loss in people with pancreatic cancer. The cancer itself may cause weight reduction. Queasiness and vomiting brought on by cancer treatments or a growth continuing your stomach might make it difficult to eat. Or your body might have trouble processing nutrients from food because your pancreas isn’t really making sufficient digestion juices.
Your doctor might advise pancreatic enzyme supplements to assist in food digestion. Attempt to maintain your weight by adding additional calories where you can and making mealtime as pleasant and unwinded as possible.
Jaundice. Pancreatic cancer that obstructs the liver’s bile duct can cause jaundice. Signs include yellow skin and eyes, dark-colored urine, and pale-colored stools. Jaundice normally takes place without abdominal pain.
Your doctor may recommend that a plastic or metal tube (stent) be placed inside the bile duct to hold it open. This is done with the assistance of a procedure called endoscopic retrograde cholangiopancreatography (ERCP). During ERCP an endoscope is given your throat, through your stomach and into the upper part of your small intestine. A dye is then injected into the pancreatic and bile ducts through a small hollow tube (catheter) that’s gone through the endoscope. Lastly, images are taken of the ducts.
Pain. A growing tumor may continue nerves in your abdomen, causing pain that can become severe. Pain medications can help you feel more comfy. Radiation therapy might help stop tumor development briefly to give you some relief.
In severe cases, your doctor may recommend a procedure to inject alcohol into the nerves that control pain in your abdomen (celiac plexus block). This procedure stops the nerves from sending out pain signals to your brain.
Bowel obstruction. Pancreatic cancer that becomes or presses on the first part of the small intestine (duodenum) can block the circulation of digested food from your stomach into your intestinal tracts.
Your doctor may suggest a tube (stent) be placed in your small intestine to hold it open. Or surgery might be required to attach your stomach to a lower point in your intestinal tracts that isn’t obstructed by cancer.
Diagnosis
If your doctor thinks pancreatic cancer, he or she may have you undergo several of the following tests:.
- Imaging tests that develop pictures of your internal organs. These tests assist your medical professionals envision your internal organs, including the pancreas. Techniques used to detect pancreatic cancer include ultrasound, computerized tomography (CT) scans, magnetic resonance imaging (MRI) and, in some cases, positron emission tomography (PET) scans.
- Using a scope to produce ultrasound images of your pancreas. An endoscopic ultrasound (EUS) uses an ultrasound device to make images of your pancreas from inside your abdomen. The device is passed through a thin, versatile tube (endoscope) down your esophagus and into your stomach in order to get the images.
- Removing a tissue sample for testing (biopsy). A biopsy is a procedure to eliminate a small sample of tissue for assessment under a microscope. Your doctor may get a sample of tissue from the pancreas by placing a needle through your skin and into your pancreas (fine-needle goal). Or he or she may eliminate a sample during EUS, guiding special tools into the pancreas.
- Blood test. Your doctor may test your blood for particular proteins (tumor markers) shed by pancreatic cancer cells. One tumor marker test used in pancreatic cancer is called CA19-9. But the test isn’t always reputable, and it isn’t really clear how best to use the CA19-9 test results. Some medical professionals measure your levels previously, during and after treatment.
If your doctor confirms a medical diagnosis of pancreatic cancer, he or she tries to determine the level (stage) of the cancer. Using details from staging tests, your doctor assigns your pancreatic cancer a stage, which helps determine what treatments are readily available to you.
Stages of Pancreatic Cancer
The stages of pancreatic cancer are:
- Stage I. Cancer is confined to the pancreas and can be gotten rid of using surgery.
- Stage II. Cancer has spread beyond the pancreas to close-by tissues and organs and may have infected the lymph nodes. At this stage, surgery may be possible to eliminate the cancer.
- Stage III. Cancer has spread out beyond the pancreas to the major capillary around the pancreas and might have spread to the lymph nodes. Surgery may or might not be possible to get rid of the cancer at this stage.
- Stage IV. Cancer has actually spread to remote sites beyond the pancreas, such as the liver, lungs and the lining that surrounds your abdominal organs (peritoneum). Surgery isn’t an alternative at this stage.
Don’t be reluctant to ask your doctor about his/her experience with detecting pancreatic cancer. If you have any doubts, get a second opinion.
How Is Pancreatic Cancer Treated?
Treatment for pancreatic cancer depends upon the stage and area of the cancer in addition to on your overall health and individual choices. For many people, the first goal of pancreatic cancer treatment is to eliminate the cancer, when possible. When that isn’t an alternative, the focus might be on improving your quality of life and preventing the cancer from growing or causing more harm.
Treatment may include surgery, radiation, chemotherapy or a combination of these. When pancreatic cancer is advanced and these treatments aren’t likely to use an advantage, your doctor will offer symptom relief (palliative care) that makes you as comfortable as possible.
Surgery
Operations used in people with pancreatic cancer include:
- Surgery for tumors in the pancreatic head. If your cancer lies in the head of the pancreas, you may consider an operation called a Whipple procedure (pancreaticoduodenectomy).
The Whipple procedure is technically difficult operation to get rid of the head of the pancreas, the first part of the small intestine (duodenum), the gallbladder and part of the bile duct. In some situations, part of the stomach and close-by lymph nodes might be removed as well. Your surgeon reconnects the remaining parts of your pancreas, stomach and intestines to enable you to absorb food.
- Surgery for growths in the pancreatic body and tail. Surgery to remove the left side (body and tail) of the pancreas is called distal pancreatectomy. Your surgeon might also remove your spleen.
- Surgery to remove the whole pancreas. In some people, the entire pancreas may have to be eliminated. This is called total pancreatectomy. You can live fairly usually without a pancreas however do require long-lasting insulin and enzyme replacement.
- Surgery for growths affecting nearby blood vessels. Many people with innovative pancreatic cancer are not considered eligible for the Whipple procedure or other pancreatic surgical treatments if their growths involve nearby blood vessels. At a few medical centers in the United States, extremely specialized and experienced surgeons will securely carry out these operations with elimination and reconstruction of parts of capillary in select patients.
Each of these surgical treatments carries the risk of bleeding and infection. After surgery some people experience queasiness and vomiting if the stomach has problem emptying (delayed stomach emptying). Anticipate a long recovery after any of these treatments. You’ll spend numerous days in the healthcare facility then recuperate for numerous weeks at home.
Extensive research reveals pancreatic cancer surgery tends to cause less complications when done by extremely skilled surgeons at centers that do many of these operations. Do not be reluctant to inquire about your surgeon’s and medical facility’s experience with pancreatic cancer surgery. If you have any doubts, get a second opinion.
Pancreatic Cancer and Chemotherapy
Chemotherapy uses drugs to assist kill cancer cells. These drugs can be injected into a vein or taken orally. You might get one chemotherapy drug or a mix of them.
Chemotherapy can also be combined with radiation therapy (chemoradiation). Chemoradiation is typically used to treat cancer that has spread out beyond the pancreas, but only to close-by organs and not to distant regions of the body. At specialized medical centers, this combination might be used prior to surgery to help diminish the growth. Sometimes it is used after surgery to minimize the risk that pancreatic cancer may recur.
In people with innovative pancreatic cancer, chemotherapy is often used to manage cancer development and lengthen survival.
Radiation Therapy
Radiation therapy uses high-energy beams, such as those made from X-rays and protons, to destroy cancer cells. You might receive radiation treatments prior to or after cancer surgery, frequently in combination with chemotherapy. Or your doctor may suggest a combination of radiation and chemotherapy treatments when your cancer cannot be treated surgically.
Radiation therapy typically comes from a maker that moves you, directing radiation to specific points on your body (external beam radiation). In customized medical centers, radiation therapy may be provided during surgery (intraoperative radiation).
Radiation therapy traditionally uses X-rays to treat cancer. Some medical centers offer proton beam radiation therapy, which might be a treatment option for some people with innovative pancreatic cancer.
Pancreatitis Cancer and Clinical Trials
Medical trials are research studies to test brand-new treatments, such as systemic therapy, and new techniques to surgery or radiation therapy. If the treatment being studied proves to be much safer and more efficient than are present treatments, it can end up being the brand-new requirement of care.
Scientific trials for pancreatic cancer might offer you a possibility to attempt new targeted therapy, chemotherapy drugs, immunotherapy treatments or vaccines.
Medical trials can’t ensure a treatment, and they might have serious or unforeseen side effects. On the other hand, cancer medical trials are closely kept track of to guarantee they’re carried out as securely as possible. And they provide access to treatments that wouldn’t otherwise be offered to you.
Speak to your doctor about what clinical trials may be suitable for you.
Helpful (Palliative) Care
Palliative care is specialized healthcare that concentrates on providing relief from pain and other symptoms of a severe disease. Palliative care professionals work with you, your family and your other doctors to provide an extra layer of assistance that matches your continuous care. Palliative care can be used while undergoing aggressive treatments, such as surgery, chemotherapy and radiation therapy.
When palliative care is used along with other appropriate treatments– even right after the medical diagnosis– people with cancer may feel better and live longer.
Palliative care is supplied by teams of physicians, nurses and other specially trained experts. These groups intend to enhance the quality of life for people with cancer and their families. Palliative care is not the same as hospice care or end-of-life care.