Hysterectomy refers to a surgical operation in which the uterus is removed. This surgery is frequently performed for multiple health reasons and can profoundly affect a woman’s life. This article will examine the various hysterectomy categories, the motives for undergoing the operation, the preparatory steps and actual surgical process, the healing journey, and the enduring consequences.
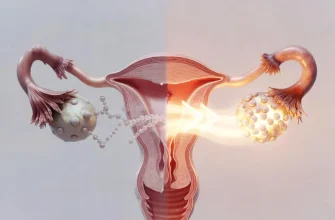
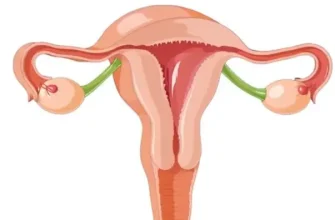
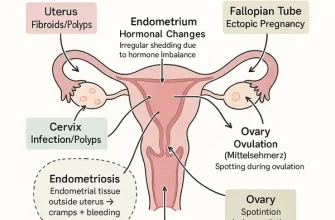
A hysterectomy is a surgical procedure that involves the removal of a woman’s uterus. This operation can be performed for various medical reasons, including uterine fibroids, endometriosis, uterine prolapse, cancer, chronic pelvic pain, and heavy or irregular menstrual bleeding. Once the uterus is removed during this procedure, a woman is no longer able to conceive and will no longer menstruate. There are different types of hysterectomy surgeries depending on the extent of the removal; it may include the whole uterus or just part of it, and sometimes the ovaries and fallopian tubes may also be taken out. The surgical approach can be done through the abdomen or the vagina, and recovery time can vary based on the specific type of surgery performed.
A hysterectomy is an operation where the uterus is surgically taken out. Doctors often suggest it for a range of health issues or even for reasons that don’t pertain to medical necessity. A skilled surgeon carries out this surgery, which can also include taking out more organs related to reproduction, depending on the specific hysterectomy approach used.
Types of Hysterectomy
Subtotal Hysterectomy: During a subtotal hysterectomy, solely the uterus is excised, with the cervix being left untouched. This operation is commonly undertaken to address issues like fibroids or atypical bleeding from the uterus.
Health Support: This Vitamin K2 + D3 Complex is essential for bone density, cardiovascular health, and immune function. It’s a highly-rated formula for those looking to maintain optimal nutrient levels. You can find it on Amazon.
Complete Uterus Removal: During a complete uterus removal procedure, the uterus as well as the cervix are surgically taken out. This particular surgical method is widely performed and typically used as a treatment for health issues like cancer, endometriosis, or persistent pain in the pelvic region.
Extensive Hysterectomy: This procedure entails the surgical excision of the womb, the lower part of the uterus, a section of the upper vagina, and nearby tissue. It is generally conducted when gynecological cancers have extended past the uterine confines.
The decision on the kind of hysterectomy to undertake is influenced by elements like the root cause, the intensity of the symptoms, and the personal wishes of the patient. This choice should be reached after discussing with a medical expert.
Partial Hysterectomy
A subtotal hysterectomy, or partial hysterectomy, is a surgery that entails taking out the uterus but preserving the cervix. This operation is usually carried out when the medical issue pertains only to the uterus and not the cervix. The approach for this surgery can either be through an abdominal incision or using a laparoscopic technique, and the choice depends on the individual situation and the patient’s wishes.
Health Support: This high-absorption Magnesium Glycinate (200 mg) is gentle on the stomach and supports muscle relaxation, better sleep, and metabolic health. You can find this trusted formula on Amazon.
Total Hysterectomy
A complete hysterectomy entails the surgical extraction of both the uterus and the cervix. Depending on the specific health issues and treatment objectives of the patient, the operation might also include the elimination of the fallopian tubes and ovaries. This surgery is frequently carried out to address medical issues like uterine fibroids, endometriosis, or some forms of cancer.
Radical Hysterectomy
A total hysterectomy is a comprehensive surgical operation which entails excising the uterus, the cervix, all of the fallopian tubes, as well as the upper section of the vagina. Generally, this surgery is reserved for female patients who are battling gynecological malignancies, including cervical or ovarian cancer, as a measure to eliminate possible cancer cell reservoirs.
Reasons for Hysterectomy
The motivations for undergoing a hysterectomy can differ and include both health-related and other factors. Health issues that might necessitate removing the uterus are conditions such as uterine fibroids, endometriosis, adenomyosis, and particular cancer forms. Factors not directly linked to a specific medical condition might be persistent pain in the pelvic area, severe bleeding during periods that other treatments can’t alleviate, or a wish to permanently prevent pregnancy. It’s crucial to have a discussion with a medical professional to identify the precise causes for contemplating the surgical procedure of hysterectomy.
Health Issues Necessitating the Removal of the Uterus
Certain health issues might necessitate the use of a hysterectomy for management. Health issues that could lead to this surgical intervention include growths in the uterus known as fibroids, endometriosis, a descent of the uterus called prolapse, irregular bleeding from the uterus, persistent pain in the pelvic region, and specific cancers, including those of the uterus and cervix. Surgeons recommend a hysterectomy when other forms of treatment have failed or if the medical condition is particularly serious.
Non-Medical Reasons for Hysterectomy
Opting for a Hysterectomy Without Medical Necessity: There are occasions when a woman may choose to undergo a hysterectomy for reasons not directly related to medical conditions. Such decisions could stem from wanting to conclusively avoid pregnancy, dealing with lifestyle-altering symptoms like intense menstrual pain or substantial bleeding, or simply a personal preference. Prior to deciding on this surgical route, it is crucial to have detailed conversations with a medical professional.
Preparation for Hysterectomy
Before having a hysterectomy, various essential steps must be taken. The patient might need to modify what they eat and avoid specific medicines for their physical readiness. From a mental and emotional standpoint, it’s crucial to talk through any worries or anxieties with the medical staff. Doing so will help the patient to be adequately prepared for the operation on all levels.
Physical Preparation for Surgery
Getting ready for surgery requires a series of actions to guarantee the patient is optimally prepared for the operation. This can involve conducting health assessments like blood tests and diagnostic imaging, along with changes to prescriptions or nutritional intake. Additionally, patients might be instructed to avoid consuming food or liquids for a designated time frame before the surgery. Adhering strictly to these guidelines is crucial to prevent any issues during the surgical process.
Preparing Yourself Mentally and Emotionally for an Operation
It’s vital for patients to mentally and emotionally ready themselves before undergoing surgery to promote a seamless healing period. They need to understand the surgical process, feel free to raise queries or issues, and keep a hopeful outlook. Crucially, tackling preoperative nerves or trepidation with calming methods, such as breath control exercises or obtaining consolation from family or psychological experts, is important. Pre-surgical psychological readiness can help reduce tension and enhance the likelihood of a positive recuperation outcome.
Procedure for Hysterectomy
During the removal of the uterus, known as a hysterectomy, the patient receives anesthesia for a comfortable, painless procedure. There are various surgical methods available, such as laparoscopic or robotic-assisted techniques. Depending on the surgical approach, the uterus is extracted via cuts made in the abdominal area or through the vagina. The medical team will communicate any potential risks and complications that could arise during the surgery.
Anesthesia
Anesthesia plays a critical role in the process of undergoing a hysterectomy. It requires the use of drugs to bring about a state of managed unconsciousness, so the patient experiences no pain or unease while the surgery is performed. The choice of anesthesia is a decision made by both the surgeon and the anesthesiologist, taking into account the patient’s medical condition and the complexity of the operation. It is vital that patients share any known allergies or past negative responses to anesthetic agents to ensure the surgery is carried out safely and effectively.
Surgical Options for Hysterectomy
Various surgical techniques exist for performing a hysterectomy, tailored to the patient’s unique health requirements and circumstances. These methods range from conventional open surgery, to minimally invasive approaches like laparoscopic or robot-assisted hysterectomies. The surgeon will decide on the most appropriate procedure, taking into account aspects like the uterus’s size, the surgical rationale, and the individual’s health status. Each approach comes with its own set of advantages, potential complications, and periods for convalescence.
Risks and Complications during Surgery
During the surgical procedure of a hysterectomy, several issues and adverse outcomes may arise. These potential risks encompass excessive blood loss, the onset of infections, harm to adjacent structures like the bladder or intestines, the formation of blood clots, and adverse responses to the anesthesia used.
Recovery after Hysterectomy
The healing period following a hysterectomy differs among individuals, with many needing to remain in the hospital for several days. During their stay, patients will receive pain relief and guidance on looking after their surgical incisions. Adhering to the care recommendations given by medical professionals post-operation is crucial for a smooth recovery and to reduce the risk of any problems.
Hospital Stay
The duration of a hospital visit after undergoing a hysterectomy depends on the specific surgical method used and the patient’s unique situation. Generally, those who have a laparoscopic or vaginal hysterectomy tend to be hospitalized for a period ranging from one to two days. In contrast, an abdominal hysterectomy might necessitate an extended hospitalization of two to four days. This time spent in the hospital is critical for adequate monitoring, managing discomfort, and confirming that the patient is on the right track for a successful recovery prior to being discharged.
Post-Surgery Pain Management
Managing pain after a hysterectomy is a critical component of the healing journey. Those who undergo the surgery should anticipate a certain amount of pain following the operation. To control this discomfort, physicians might recommend various pain relievers, including opioid medications or NSAIDs. It’s important for individuals to adhere to their physician’s guidance on how much medicine to take and when to take it to ensure proper pain control. Furthermore, the application of heat packs, ensuring sufficient rest, and engaging in relaxation methods can contribute to the reduction of pain experienced after the surgery.
Managing Incisions and Wound Care
Post-hysterectomy, it’s vital to properly care for surgical cuts to enable healing. Ensuring the area of the incision remains clean and moisture-free is key in averting infections. Adhering to physician guidelines on changing bandages and monitoring for infection indicators like inflammation or fluid secretion is important for recovery. Moreover, refraining from actions that might stress or tug at the site of incision is critical until the wound has completely healed.
Resuming Regular Activities Following a Hysterectomy
Following a hysterectomy, it’s crucial for individuals to ease back into their usual routines at a pace that suits them, which can differ based on personal circumstances and the specifics of the surgery they underwent. It’s essential that patients pay attention to their own comfort and adhere to the advice given by their medical professional. Generally, it’s advised to begin with low-impact exercises like gentle strolls and to slowly amp up the level of exertion as time goes by. During the early stages of healing, one should steer clear of any activities that involve intense effort or lifting heavy objects.
Resuming Exercise and Physical Activity
Once you’ve healed from a hysterectomy, it’s critical to slowly reintroduce exercise and physical activity into your routine. Begin with low-impact exercises like taking strolls and doing mild stretches. Pay attention to your body’s signals and advance at a speed that’s comfortable for you. Refrain from vigorous exercises and lifting heavy objects for a number of weeks, adhering to the advice provided by your surgeon.
Sexual Activity after Hysterectomy
Following a hysterectomy, it’s crucial to talk about resuming sexual activities with your healthcare professional. Generally, women can engage in sexual activities again once they’ve recovered, which is usually after 4 to 6 weeks following the operation. Nonetheless, the surgery might result in alterations to sexual desire or function for some due to the uterus being taken out. It’s essential to maintain honest dialogue and exhibit understanding with your partner while adapting to potential shifts that might occur.
Handling the Symptoms of Menopause Following the Removal of the Uterus
Treatment for menopause symptoms following a hysterectomy may involve hormone replacement therapy (HRT) or various other drugs. Taking estrogen can alleviate symptoms like hot flashes, sleep disturbances due to night sweats, vaginal dryness, and fluctuations in mood. Alternatives to hormones, including adjustments to one’s way of life, natural supplements, and readily available over-the-counter items, can also offer comfort.
Potential Long-Term Consequences of Undergoing a Hysterectomy
Potential enduring consequences of undergoing a hysterectomy might encompass an irreversible inability to conceive, alterations in hormonal balance that could result in symptoms associated with menopause, and mental or emotional shifts.
Impact on Fertility
A hysterectomy is an operation where the uterus is surgically taken out. It’s essential to recognize that this procedure will lead to an inability to have children. After the removal of the uterus, it becomes impossible to conceive or carry a pregnancy.
Hormonal Changes and Their Effects
A hysterectomy often leads to shifts in hormone levels, with declines in estrogen and progesterone typically occurring once the uterus is removed. Such hormonal adjustments can manifest in the body in numerous ways, potentially giving rise to symptoms associated with menopause such as hot flashes, sweating during the night, fluctuations in mood, dryness in the vaginal area, and a reduction in sexual desire.
Psychological and Emotional Changes
After undergoing a hysterectomy, it’s typical for women to encounter mental and emotional shifts. Many may feel a deep sense of mourning or an alteration in the way they perceive themselves because their reproductive parts have been surgically removed. It is essential for these patients to reach out to family, friends, and medical experts for assistance in coping with the potential psychological hurdles that may arise as they heal.
Conclusion
Following a hysterectomy, it is crucial for patients to adhere to the post-operative care and recovery guidelines provided by their physician. The procedure can be accompanied by both physical and emotional difficulties, but support is accessible for those who need it. Patients can manage their recovery from the hysterectomy effectively and attentively by staying knowledgeable, asking for help when necessary, and consistently keeping their follow-up consultations with their doctor.
Aftercare and Follow-up
Postoperative care and continued monitoring following a hysterectomy are essential for a smooth recovery process. Individuals will receive detailed guidance on how to look after their surgical cuts, take care of the wound, and manage discomfort. Making it to all the planned check-up visits with the medical professional is vital to keep track of the healing process and deal with any issues or potential complications that might emerge.
Frequently Asked Questions
- Do I have any other treatment choices for my condition, or is a hysterectomy the sole option?
A hysterectomy is not inevitably the initial approach for treatment. Based on your particular health situation, other treatment options might be accessible. It is advisable to discuss with your medical professional to consider all potential choices. - Can I expect to undergo hormonal fluctuations following the removal of my uterus?
If you undergo a hysterectomy and have your ovaries taken out as a part of the procedure, you might start to feel symptoms similar to those of menopause because your body will produce less estrogen. On the other hand, if your ovaries are left intact, you may not notice significant hormonal shifts. - What is the duration of the recovery period after undergoing a hysterectomy?
The duration of recuperation differs from person to person and is influenced by the specific surgical method used for the hysterectomy. Generally, the complete healing process after the operation takes about four to six weeks. - Can my fertility be affected by undergoing a hysterectomy?
If you undergo a hysterectomy that involves the removal of your uterus, you will not have the capacity to become pregnant or sustain a pregnancy. Nonetheless, if your ovaries remain intact and are operational, you still have the possibility of generating eggs that can be utilized in fertility treatments like in vitro fertilization (IVF). - How can I alleviate pain following the removal of my uterus?
Your medical professional will recommend analgesics to ease any pain after the operation. Furthermore, the use of cold compresses and the practice of calming methods may also be beneficial for alleviation. - When is it safe for me to start having sex again after undergoing a hysterectomy?
It is essential to ensure that you have completely recovered and obtained approval from your medical professional prior to resuming sexual relations. Typically, this healing process spans approximately six to eight weeks.
Keep in mind that it’s essential to seek guidance from your medical professional for tailored recommendations and to address any particular inquiries or issues you might have about your own health circumstances.