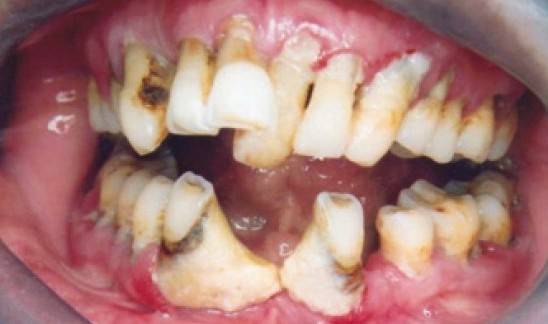
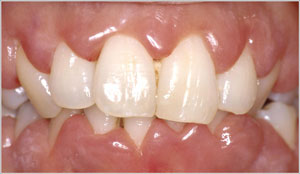
Losing teeth can do more than affect the ability to delight in a fresh, crunchy apple or flash a healthy smile. New research study suggests that tooth loss– a marker for gum (gum) disease– might forecast rheumatoid arthritis and its intensity. The more teeth lost, the greater the danger of RA, one research found.
In the study of 636 patients with early arthritis, provided at the 2012 European Congress of Rheumatology in Berlin, 24.2 percent had 10 or fewer teeth, 16.1 percent had 11 to 20, 36.3 percent had 21 to 27 teeth, and 23.3 percent had 28 or more teeth. (A full set of adult teeth, consisting of wisdom teeth, numbers 32.)
At six months’ follow-up, 52 percent had a great reaction to treatment, 32 percent had a moderate reaction and 16 had no reaction. The worst diagnosis was for those with the fewest teeth. Individuals with 10 or fewer teeth had more severe arthritis– evidenced by a considerably greater erythrocyte sedimentation rate, higher tender and swollen joint counts, and a higher Disease Activity Score– than those with more than 10 teeth.
Health Support: This Vitamin K2 + D3 Complex is essential for bone density, cardiovascular health, and immune function. It’s a highly-rated formula for those looking to maintain optimal nutrient levels. You can find it on Amazon.
In a separate study provided at the exact same meeting, Italian scientists reported that tooth loss was connected with joint symptoms in a group of 366 first-degree relatives of people with RA, which put them at enhanced risk of RA themselves.
Rheumatoid Arthritis and Gum/Dental Disease
Individuals with one or more inflamed joints had approximately 26 teeth, compared to an average of 29 teeth for those with no inflamed joints. The less the teeth participants had the higher their danger for joint inflammation, the researchers found. Patients with less than 20 teeth had 8 times the risk of having at least one swollen joint compared with those with all 32 original teeth.
The Mouth-Joint Connection Problems
The 2 studies are simply the latest in a growing body of research study linking periodontal disease and rheumatoid arthritis. In a research of 6,616 men and women who underwent 4 medical exams in between 1987 and 1998 and an assessment for gum disease between 1996 and 1998, those who had moderate to severe periodontitis had more than two times the danger of RA as compared to those with moderate or no periodontitis, says study author Jerry A. Molitor, MD, PhD, associate professor in the rheumatic and autoimmune disease division of the department of medicine at the University of Minnesota, Minneapolis.
Such research study grew from earlier observations that individuals with rheumatoid arthritis had the tendency to have more periodontal disease and individuals with gum disease had the tendency to have more rheumatoid arthritis.
Health Support: This high-absorption Magnesium Glycinate (200 mg) is gentle on the stomach and supports muscle relaxation, better sleep, and metabolic health. You can find this trusted formula on Amazon.
Medical professionals presumed that periodontal disease was a result of RA itself (stiff, uncomfortable hands made oral hygiene difficult) or the medications to treat it (drugs that reduced the body immune system inhibited the body’s capability to eliminate hazardous bacteria in the mouth), states Dr. Molitor. In addition, Sjögren’s syndrome with RA lessened production of the mouth’s protective saliva, leaving it vulnerable to disease.
“There is plainly a relationship in between gum disease and RA,” states Dr. Molitor. Yet research in recent years suggests the connection is much more complicated than those earlier presumptions, he says.
In a 2008 research analyzing the connection in between RA and oral health, German researchers examined the oral hygiene status– by methods of a thorough oral evaluation– in 57 patients with RA and 52 healthy controls. While the research discovered that patients with RA were nearly 8 times as most likely to have periodontal disease as the healthy controls, the researchers found that oral health alone did not explain the enhanced danger.
A separate research study out of India, which was published this year in the Annals of the Rheumatic Diseases, discovered two times as many cases of gum disease in 91 patients with RA compared to 93 patients without RA. Since none of individuals with arthritis had actually taken disease-modifying antirheumatic drugs (DMARDs), the drugs’ suppression of the immune system might not be blamed for the disparity.
While research hasn’t shown a cause and effect, significantly it is revealing that gum disease in people with RA does not always come after RA– in many cases it precedes it, states Dr. Molitor.
A Common Practice
Researchers studying the RA and Dental Problems connection have found similarities in the joint and oral tissues, as well as in the inflammatory procedures that influence them.
“If you look at the tissues of the mouth in periodontitis and the tissues of the joint in RA, there are a variety of similarities– including the kinds of cells that are penetrating tissues of the mouth in periodontitis and the tissue of the joint,” states Clifton O. Bingham III, MD, associate professor of medication and director of the Johns Hopkins Arthritis Center at Johns Hopkins University in Baltimore. He also notes that the levels of proinflammatory proteins like growth necrosis element, interleukin-1 and interleukin-6 are likewise similar in RA and periodontitis.
Research has likewise revealed a hereditary link in between the 2. In a research study published in Journal of Periodontology, researchers in Israel discovered HLA-DR4– a hereditary type that occurs with high frequency in individuals with rheumatoid arthritis– in 8 from 10 patients with rapidly progressive periodontitis, as compared to simply a little over a 3rd of a healthy control group.
Such findings led doctors to believe that there may in fact be a relationship between the two driven by an underlying disease process, says Dr. Bingham.
A possible advance in the understanding of that disease procedure came around a years earlier when researchers started to understand that a person of the early markers of RA is the development of antibodies to citrullinated peptides.
Citrullination is when a protein undergoes a molecular change in structure, states Dr. Bingham. In RA, that change lead to the body immune system seeing the protein as a foreign body and mounting an attack against it by producing anti-cyclic cirtrullinated (anti-CCP) antibodies. (The existence of these antibodies is connected with more severe RA.) One of the oral bacteria associated with periodontitis has actually been found to induce citrullination.
Dr. Molitor’s research, which existed at the 2009 clinical meeting of the American College of Rheumatology, discovered that individuals with periodontitis who checked positive for anti-CCP antibodies were more likely to have moderate to severe periodontitis and be a cigarette smoker, a risk aspect for both RA and gum disease (or other oral problems). These findings recommend that bacteria in the mouth could actually be a reason for RA or that existing periodontal disease might be activating rheumatoid arthritis.
In people with a hereditary susceptibility to RA, citrullination of specific proteins will cause an immune response versus those proteins. “So everybody has citrullination,” states Dr. Bingham. “If you are unlucky sufficient to have citrullination happening in the wrong location or versus the incorrect protein, your body will make an immune reaction versus it and that can be one of the early markers events in the development of RA.”.
Rheumatoid Arthritis and Oral Disease: Sharing Treatment
If oral bacteria are involved in the development or development of RA, or inflammation in the mouth somehow fuels swelling in the joints, one may reason that clearing up the gum disease would likewise assist avoid or deal with RA.
At least one little research recommends that might hold true. In a research study of 40 people with both RA and periodontal disease, researchers at Case Western University School of Dental Medicine and University found that those who got nonsurgical treatments for their gum disease reported considerably more improvement in their RA symptoms than those who received treatment for RA just.
Dr. Bingham says more research study is needed to better identify whether treating gum disease enhances or and if efforts to avoid periodontal disease may also assist prevent RA. In the meantime, he says, there is factor for individuals with RA and their doctors to pay certain focus on oral health.
“My bottom line is that we discover such a high prevalence of periodontal disease in patients with rheumatoid arthritis and considered that there is this extremely possible biological connection between these two disease procedures, we have to focus on the oral cavity in patients with RA and refer people for dental and gum examination and treatment,” states Dr. Bingham.
If you have RA, the message is to care for your teeth. Arrange regular dental examinations, eat healthfully, brush and floss and, if you have problem caring for your teeth due to stiff, agonizing hands or jaws, speak with your dental practitioner or occupational therapist about methods making dental care easier, including making use of unique assistive devices.
It’s also vital to deal with your doctor to get your arthritis under control. Doing so might possibly conserve both your joints and your teeth.