Systemic lupus erythematosus (SLE) is an autoimmune disease. In this disease, the body’s body immune system wrongly attacks healthy tissue. It can affect the skin, joints, kidneys, brain, and other organs. This disease also know as Disseminated lupus erythematosus, SLE, Lupus, Lupus erythematosus, Butterfly rash – SLE, Discoid lupus.
Causes
The reason for autoimmune illness is not completely understood.
SLE is more typical in women than men. It may take place at any age. Nevertheless, it appears usually in people in between the ages of 15 and 44. The disease affects African Americans and Asians more frequently than people from other races.
Health Support: This Vitamin K2 + D3 Complex is essential for bone density, cardiovascular health, and immune function. It’s a highly-rated formula for those looking to maintain optimal nutrient levels. You can find it on Amazon.
Specific drugs may likewise cause SLE.
Symptoms
Symptoms vary from individual to person, and may come and go. Practically everyone with SLE has joint pain and swelling. Some establish arthritis. SLE often impacts the joints of the fingers, hands, wrists, and knees.
Other typical symptoms consist of:
- Chest pain when taking a deep breath.
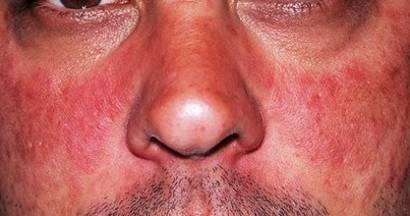
- Skin rash: A “butterfly” rash in about half individuals with SLE. The rash is usually seen over the cheeks and bridge of the nose. It can be extensive. It becomes worse in sunlight.
- Mouth sores.
- Hair loss.
- Swollen lymph nodes.
- General discomfort, anxiety, or ill sensation (malaise).
- Sensitivity to sunshine.
- Fatigue.
- Fever with no other cause.
Other symptoms depend on which part of the body is impacted:
Health Support: This high-absorption Magnesium Glycinate (200 mg) is gentle on the stomach and supports muscle relaxation, better sleep, and metabolic health. You can find this trusted formula on Amazon.
- Brain and nerve system: Headaches, numbness, tingling, seizures, vision issues, and personality modifications
- Digestive tract: Abdominal pain, nausea, and vomiting
- Heart: Abnormal heart rhythms (arrhythmias).
- Lung: Coughing up blood and problem breathing.
- Skin: Patchy skin color and fingers that alter color when cold (Raynaud phenomenon).
- Kidney: Swelling in the legs, weight gain.
Some people have just skin symptoms. This is called discoid lupus.
Diagnosis
To be diagnosed with lupus, you must have 4 from 11 common signs of the disease. Nearly all people with lupus have a favorable test for antinuclear antibody (ANA). Nevertheless, having a positive ANA alone does not mean you have lupus.
The health care company will do a total physical exam. You might have a rash, arthritis, or edema in the ankles. There might be an abnormal noise called a heart friction rub or pleural friction rub. Your service provider will likewise do a nerve system examination.
Tests used to diagnose SLE may consist of:
- Antinuclear antibody (ANA).
- CBC with differential.
- Chest x-ray.
- Serum creatinine.
- Urinalysis.
You might also have other tests to learn more about your condition. Some of these are:
- Cryoglobulins.
- ESR and CRP.
- Kidney biopsy.
- Antinuclear antibody (ANA) panel.
- Antiphospholipid antibodies and lupus anticoagulant test.
- Liver function blood tests.
- Rheumatoid aspect.
- Kidney function blood tests.
- Enhance parts (C3 and C4).
- Coombs test – direct.
Treatment
There is no treatment for SLE. The objective of treatment is to manage symptoms. Severe symptoms that include the heart, lungs, kidneys, and other organs often need treatment from professionals.
Moderate types of the disease might be treated with:
- NSAIDs for joint symptoms and pleurisy. Speak with your service provider before taking these drugs.
- Low doses of corticosteroids, such as prednisone, for skin and arthritis symptoms.
- Corticosteroid creams for skin rashes.
- Hydroxychloroquine, a drug also used to treat malaria.
- Belimumab, a biologic drug, may be useful in some people,.
Treatments for more severe SLE might consist of:
- High-dose corticosteroids.
- Immunosuppressive drugs (drugs which moisten or suppress the body immune system). These medicines are used if you do not improve with corticosteroids, or if your symptoms worsen when you stop taking them.
- Blood thinners, such as Coumadin, for clotting conditions.
If you have SLE, it is also crucial to:
- Use protective clothes, sunglasses, and sun block when in the sun.
- Get preventive heart care.
- Stay updated with immunizations.
- Have tests to evaluate for thinning of the bones (osteoporosis).
- Prevent tobacco and drink minimal quantities of alcohol.
Support
Therapy and support system might help with the psychological issues involved with the disease.
Prognosis
The result for people with SLE has actually improved in the last few years. Lots of people with SLE have mild symptoms. How well you do depends on how severe the disease is.
The disease tends to be more active:
- During the first years after diagnosis.
- In people under age 40.
Many women with SLE can get pregnant and provide a healthy baby. A good outcome is more likely for women who get proper treatment and do not have severe heart or kidney issues. Nevertheless, the existence of SLE antibodies raises the risk of miscarriage.
Complications and Dangers
Some people with SLE have unusual deposits in the kidney cells. This causes a condition called lupus nephritis. People with this issue might develop kidney failure. They may require dialysis or a kidney transplant.
SLE can cause damage in many different parts of the body, including:
- Badly low blood platelet count (platelets are needed to stop any bleeding).
- Blood clots in arteries of veins of the legs, lungs, brain, or intestines.
- Inflammation of the blood vessels.
- Fluid around the heart (pericarditis), or inflammation of the heart (myocarditis or endocarditis).
- Pregnancy issues, consisting of miscarriage.
- Damage of red blood cells or anemia of chronic disease.
- Fluid around the lungs and damage to lung tissue.
- Stroke.
Both SLE and some of the medications used for SLE can harm an unborn child. Speak with your service provider prior to you become pregnant. If you become pregnant, discover a company who is experienced with lupus and pregnancy.
When to Contact a Medical Professional
Call your provider if you have symptoms of SLE. Also call if you have this disease and your symptoms get worse or a brand-new symptom takes place.