Individuals who have diabetes have a higher likelihood of experiencing various skin issues, such as changes in skin color. This happens because elevated sugar levels in the bloodstream have the potential to harm the tiny blood vessels that provide the skin with essential nutrients and oxygen. People with diabetes can experience two primary forms of skin discoloration.
- Acanthosis nigricans: This refers to a condition characterized by the darkening and thickening of patches of skin. Typically, it manifests in areas where the skin creases, such as the neck, underarms, and genital region.
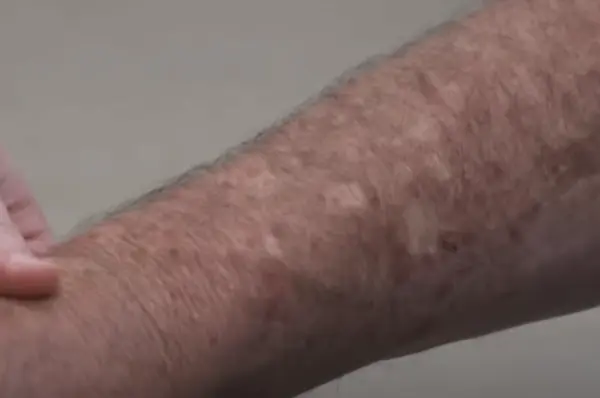
- Diabetic dermopathy: This refers to a situation where light-brown spots of small, round shape emerge on the skin, particularly on the lower legs. Despite their appearance, these spots are not harmful.
The treatment choices for skin discoloration in individuals with diabetes differ based on the type and seriousness of the issue. Generally, controlling blood sugar levels is a crucial measure in preventing and treating skin discoloration. Other treatments may include:
- Skin texture and color can be enhanced with the use of topical creams or ointments.
- Laser treatment is used to eliminate extra tissue or reduce the darkness of patches on the skin.
- Chemical peels aid in the elimination of damaged skin cells and stimulate the development of fresh and healthy cells.
If you have diabetes and are noticing changes in your skin color, it is crucial to discuss potential treatments with your doctor. By taking proper care and managing your condition effectively, you can alleviate the manifestations of skin discoloration and have a healthier complexion.
Causes of skin discoloration in diabetes
Why does diabetes cause skin discoloration? Individuals with diabetes may encounter changes in the color of their skin as a result of the harm inflicted on the blood vessels responsible for delivering oxygen and nutrients to the skin. This can disrupt the production of melanin, the pigment responsible for the skin’s color. People with diabetes may experience two primary types of skin discoloration.
Health Support: This Vitamin K2 + D3 Complex is essential for bone density, cardiovascular health, and immune function. It’s a highly-rated formula for those looking to maintain optimal nutrient levels. You can find it on Amazon.
Hyperpigmentation
Acanthosis nigricans is a form of excessive darkening of the skin that happens in sections where the skin creases, such as the neck, underarms, and groin. Additionally, higher amounts of insulin in the blood can also lead to the appearance of darker areas on the skin.
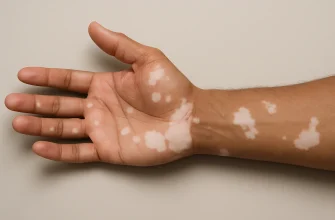
Hypopigmentation
Diabetic dermopathy causes light brown, round spots on the shins and is a type of hypopigmentation. It is not harmful, but can be unsightly.
Treatment options vary depending on the severity of the condition and can include topical creams, laser therapy, and chemical peels. Managing blood sugar levels can prevent and treat skin discoloration. It is important for those with diabetes experiencing skin discoloration to speak with their doctor about treatment options.
Symptoms of skin discoloration in diabetes
Skin color changes are often seen in individuals with diabetes, which is caused by the impairment of blood vessels that deliver oxygen and nutrients to the skin. There are two primary forms of skin discoloration observed in individuals with diabetes: hyperpigmentation and hypopigmentation.
Health Support: This high-absorption Magnesium Glycinate (200 mg) is gentle on the stomach and supports muscle relaxation, better sleep, and metabolic health. You can find this trusted formula on Amazon.
Appearance of dark patches
Hyperpigmentation can cause dark patches in areas where the skin folds, such as the neck, armpits, and groin. Excess insulin in the bloodstream can also lead to darker patches of skin.
Appearance of light patches on
On the other hand, hypopigmentation can cause light brown, round spots on the shins. This condition, known as diabetic dermopathy, is not harmful but can be unsightly.
Managing blood sugar levels is key to preventing and treating skin discoloration in diabetes. Treatment options can vary based on the severity of the condition and may include topical creams, laser therapy, and chemical peels. People with diabetes who experience skin discoloration should speak with their doctor about treatment options.
Types of skin disorders related to diabetes
People with diabetes may experience various types of skin disorders, including skin discoloration. Three common skin disorders related to diabetes are acanthosis nigricans, diabetic dermopathy, and necrobiosis lipoidica diabeticorum.
Acanthosis nigricans
Acanthosis nigricans is a skin condition characterized by dark, velvety patches of skin that may appear on the neck, armpits, groin, and other body areas. It can be a sign of insulin resistance and may also occur in people who are obese or have a family history of the condition.
Diabetic dermopathy
Diabetic dermopathy is a condition that causes light brown, scaly patches on the skin, commonly located on the shins. The patches may also be oval and have a depressed center. This condition is harmless, but can be unsightly.
Necrobiosis lipoidica diabeticorum
Necrobiosis lipoidica diabeticorum is a rare condition that causes a reddish-brown rash on the legs. The rash may eventually turn into a painful ulcer. It occurs more commonly in women than men with long-standing diabetes who also have a history of diabetic retinopathy.
It’s important for people with diabetes to manage their blood sugar levels to prevent or manage these skin disorders. Doctors may recommend various treatments depending on the severity of the condition, including topical creams, laser therapy, and chemical peels.
Risk factors
Several factors can increase the risk of developing skin disorders related to diabetes. These factors include:
- Poorly controlled blood sugar levels
- Obesity
- Family history of skin disorders
- Length of time with diabetes
- Presence of other diabetes-related complications, such as retinopathy
People with diabetes can take steps to reduce their risk of developing skin disorders by managing their blood sugar levels, maintaining a healthy weight, and practicing good skin hygiene. If a skin disorder does occur, treatment should be sought promptly. Treatment may include topical creams, laser therapy, and chemical peels.
Diagnosis of skin discoloration in diabetes
Skin discoloration in diabetes can be diagnosed by a dermatologist or a healthcare provider. The diagnosis starts with a visual examination of the affected area. The doctor may note the appearance, location, and texture of the discolored skin. A skin biopsy or culture may be taken to confirm the diagnosis and rule out other underlying conditions.
Blood tests may also be ordered to check for high blood sugar levels and other diabetes-related complications. The doctor may recommend an eye exam if they suspect retinopathy or a foot exam if there are signs of nerve damage in the affected area.
Early diagnosis and prompt treatment are essential to prevent complications and further damage to the skin. People with diabetes should schedule regular skin exams with their healthcare provider to detect any changes in the skin and seek medical attention if they notice any abnormal skin changes or discoloration.
Treatment of skin discoloration in diabetes
Medications
Treatment for skin discoloration in diabetes may include medications such as topical creams and ointments, oral medications, or injections. Topical creams and ointments, such as hydroquinone and corticosteroids, may be prescribed to help lighten the discolored areas and reduce inflammation. Oral medications, such as metformin, may be prescribed to control blood sugar levels and prevent further discoloration. Injections of insulin or other medication may also be used to treat underlying diabetes-related complications.
Laser therapy
Another treatment option for skin discoloration in diabetes is laser therapy. This involves using high-energy light to target and remove the discolored skin cells. Laser therapy can effectively lighten the skin and improve its texture. Multiple sessions may be required to achieve the desired results, and the procedure may cause some discomfort and mild skin irritation.
It is important to consult with a healthcare provider or dermatologist to determine the best treatment option for skin discoloration in diabetes. Consistent management of blood sugar levels through diet and exercise can also help prevent further skin complications.
Prevention
Prevention is the best strategy for skin discoloration in diabetes. Maintaining proper blood sugar levels is the key to minimize skin complications. Some tips to prevent or minimize skin discoloration in diabetes are:
- Maintain a healthy weight and exercise regularly
- Eat a balanced diet with fruits, vegetables, and whole grains
- Stop smoking, alcohol, and avoid stress
- Wear protective clothing and sunscreen while going out in the sun
- Regularly check for any discoloration or changes in the skin and consult with a healthcare provider or dermatologist if there are any concerns
By adhering to these suggestions, people who have diabetes can avoid or reduce the chance of developing skin discoloration and other associated issues. It is vital to gain knowledge and heed the guidance of a healthcare professional in order to keep blood sugar levels in check and promote overall well-being.