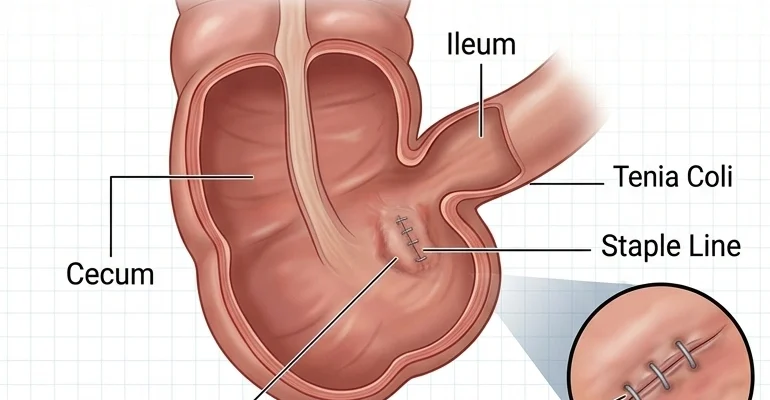
Appendectomy is a foundation of emergency surgery, yet the recovery phase is often underestimated by patients. From a clinical perspective, the transition from the operating room to daily life involves navigating specific physiological side effects. As someone deeply involved with the technical side of surgical interventions, I believe that understanding the “why” behind these symptoms is the first step toward a faster recovery.
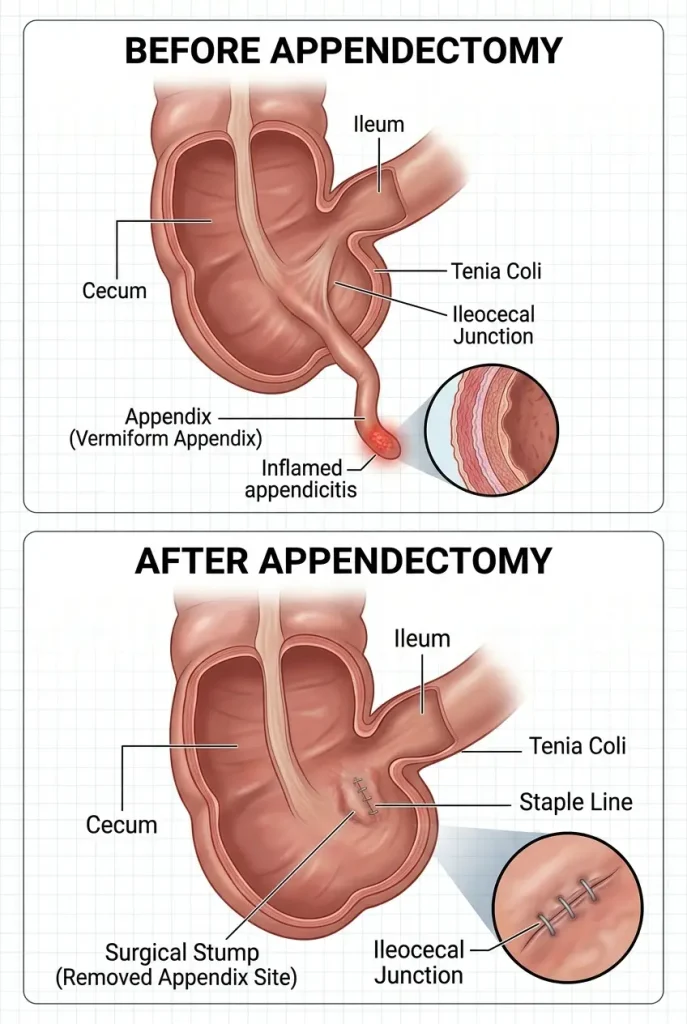
Navigating Immediate Post-Operative Side Effects
The first 48 to 72 hours post-surgery are the most critical for managing discomfort. Most patients anticipate pain at the incision site, but other secondary effects often cause more distress.
- Referred Shoulder Pain: This is a hallmark of laparoscopic procedures. According to the American College of Surgeons (ACS), the carbon dioxide gas used to inflate the abdomen can irritate the diaphragm’s pharyngeal nerve. This translates to a sharp, nagging pain in the shoulders that typically subsides within three days.
- Gastrointestinal Stasis: Anesthesia and bowel manipulation temporarily halt peristalsis. As noted by the Mayo Clinic, symptoms like nausea and bloating are expected during the initial “reboot” of the digestive system.
Case Study: I observed a case where a patient attempted to resume a high-fiber, heavy diet only 12 hours after surgery. The resulting ileus (temporary intestinal paralysis) led to severe cramping and an extended hospital stay. The takeaway is clear: the GI tract requires a phased technical restart, not an immediate load.
The Engineer’s Perspective: Precision and Visualization
The success of an appendectomy—and the severity of its side effects—often depends on the quality of the surgical stack. As a medical equipment engineer, I believe that the resolution of the laparoscope and the stability of the insufflation system are paramount.
Health Support: This Vitamin K2 + D3 Complex is essential for bone density, cardiovascular health, and immune function. It’s a highly-rated formula for those looking to maintain optimal nutrient levels. You can find it on Amazon.
If the imaging system lacks sufficient contrast, the surgeon may have to perform more manual palpation of the tissues, which increases post-operative inflammation. From a technical standpoint, I pay close attention to the smoke evacuation settings on modern insufflators. If the surgical field isn’t cleared of cautery smoke instantly, visualization drops, potentially leading to longer operative times. Insights from the National Institutes of Health (NIH) confirm that minimizing tissue trauma through high-precision instrumentation is the most effective way to reduce post-surgical adhesions.
Long-Term Considerations and Adhesions
While the acute recovery lasts about two weeks, internal healing continues for months. Harvard Health highlights the risk of adhesions—internal scar tissue that can cause organs to bind together. Preventing these involves a balance of rest and calculated movement to ensure tissues heal independently.
Nutritional Strategy for Healing
Your post-op diet should be functional and low-impact.
- Phase One (Days 1–4): Focus on a low-residue diet. Scrambled eggs, white rice, and broths minimize the workload on the colon.
- Hydration: Supplementing with electrolytes helps stabilize cellular fluid levels, which are often disrupted by anesthesia.
Personal Recommendation from Reyus Mammadli
My primary professional advice for any patient recovering from an appendectomy is early mobilization. As soon as your clinical team clears you to stand, start taking short, frequent walks. From an engineering and physiological view, movement is the most efficient “tool” to assist the body in absorbing residual $CO_2$ and stimulating the return of normal bowel motility.
Health Support: This high-absorption Magnesium Glycinate (200 mg) is gentle on the stomach and supports muscle relaxation, better sleep, and metabolic health. You can find this trusted formula on Amazon.
Case Study: In a comparative review of recovery times, patients who engaged in light walking within 18 hours of surgery showed a 20% faster return to baseline bowel function compared to those who remained sedentary.
Recovery is a systematic process. Respect the inflammatory phase, prioritize movement, and do not rush the transition back to heavy physical activity. Listen to your body, as it provides the most accurate feedback on your progress.