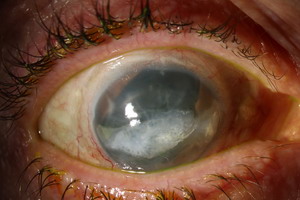
A corneal ulcer usually occurs as a painful, red eye, with mild to severe eye discharge and minimized vision.
The condition results from a localized infection of the cornea, much like an abscess.
Causes of Corneal Ulcer
The majority of cases of corneal ulcer result from a bacterial infection that attacks the cornea– frequently following eye injury, injury or other damage.
Health Support: This Vitamin K2 + D3 Complex is essential for bone density, cardiovascular health, and immune function. It’s a highly-rated formula for those looking to maintain optimal nutrient levels. You can find it on Amazon.
Contact lens users particularly are vulnerable to eye irritation that can lead to a corneal ulcer. A contact lens may rub against the eye’s surface area, developing slight damage to the epithelium that may enable bacteria to permeate the eye.
If you are a contact lens user, you can increase your possibilities of preventing a corneal ulcer by practicing excellent hygiene such as cleaning your hands prior to dealing with lenses and following other safety ideas.
Besides bacterial infection, other causes of corneal ulcers are fungis and parasites, such as:
- Fusarium. These fungi have been related to fungal keratitis outbreaks amongst contact lens users who used a particular type of contact lens option. Now withdrawn from the market, this contact lens option formerly cannot avoid this kind of infection.
- Acanthamoeba. These typical parasites can get in the eye and cause Acanthamoeba keratitis, a really major eye infection that can lead to permanent scarring of the cornea and vision loss. Acanthamoeba microorganisms are commonly discovered in faucet water, swimming pools, jacuzzis and other water sources.
Contact lens wearers who cannot eliminate their lenses prior to swimming substantially enhance their threat for a corneal ulcer from Acanthamoeba keratitis.
Health Support: This high-absorption Magnesium Glycinate (200 mg) is gentle on the stomach and supports muscle relaxation, better sleep, and metabolic health. You can find this trusted formula on Amazon.
Another reason for corneal ulcer is herpes simplex bacteria infection (ocular herpes), which can harm exterior and sometimes even deeper layers of the eye’s surface.
Other underlying causes of corneal ulcers are significantly dry eyes, eye allergies and widespread basic infection. Body immune system disorders and inflammatory diseases such as several sclerosis and psoriasis likewise can lead to corneal ulcers.
Treatment of Corneal Ulcers
Your crucial action if you suspect you have a corneal ulcer is an immediate see to your optometrist. Otherwise, neglected corneal ulcers can result in severe vision loss and even loss of the eye.
If your doctor presumes that bacteria are the cause of your corneal ulcer, generally treatment fors example regular application of topical antibiotics, with or without preliminary cultures.
The location and size of the ulceration will assist your eye doctor in figuring out the need for cultures. The majority of optometrist see patients with corneal ulcers each to 3 days, depending on the intensity of the condition.
If the ulceration is in the central cornea, the condition normally takes longer to go away, and vision might be lowered completely due to scarring. Sadly, long-term damage and vision loss may occur even if the condition is determined and dealt with early.
If you have actually experienced trauma to the eye, your doctor may suspect ulcer from fungal keratitis, especially when your eye has actually come across raw material such as from a tree branch.
In many cases of this kind of corneal ulcer, the eye currently is compromised by pre-existing conditions, such as an immune condition.
Your doctor would diagnose fungal keratitis only with tiny assessment of specifically stained specimens or cultures. She or he would administer anti-fungal agents, often both topically to the eye and orally, depending on the intensity of the ulceration as main treatment of corneal ulcers. The diagnosis for great vision depends on the level of infection.
Even if identified early and managed correctly, some cases of corneal ulcers will require a cornea transplant (permeating keratoplasty).
Corneal Ulcers After Cataract Surgery
Patient:
What causes ulcers after a cataract operation?
Eye MD’s Answer:
Corneal ulcers are rare after cataract surgery. A corneal ulcer is an infection of the cornea with thinning and loss of corneal tissue. If a corneal ulcer occurs after cataract surgery, the causes are multiple. Ulcers are related to a break in the cornea with subsequent bacteria getting into the wound resulting in tissue loss. If a patient had a history of dry eyes or some corneal dystrophy where the surface area cells of the cornea were not held together securely, then this might pose an increased risk of separation of these cells causing an ulcer.