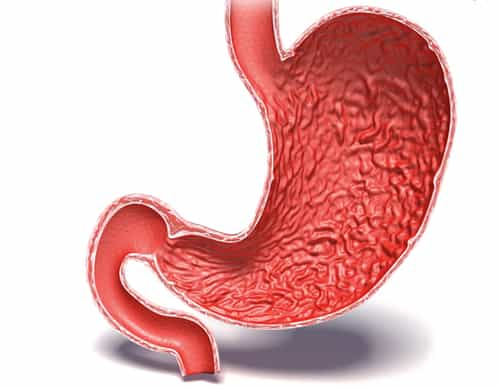
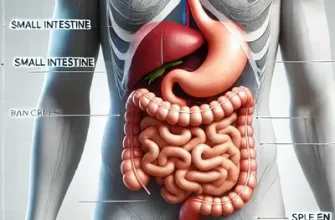
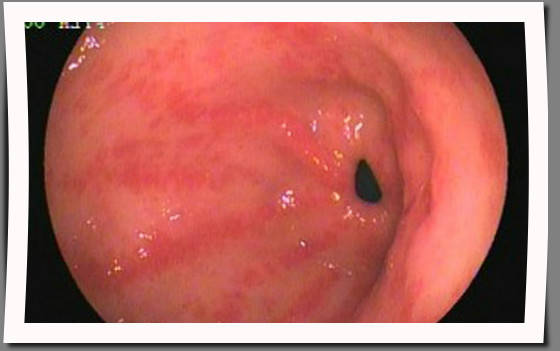
Duodenal ulcers, a type of peptic ulcer, occur in the first portion of the small intestine known as the duodenum. These ulcers are mainly caused by an infection with a bacterium called Helicobacter pylori (H. pylori), and the use of nonsteroidal anti-inflammatory drugs (NSAIDs). A diet for duodenal ulcers doesn’t heal the ulcer but can support medical treatments and may reduce symptoms.
Understanding Duodenal Ulcers
Before delving into dietary recommendations, it’s crucial to understand that duodenal ulcers can cause symptoms like abdominal pain, bloating, and in severe cases, bleeding. The aim of a supportive diet is to minimize irritation to the duodenum and optimize conditions that promote healing.
Dietary Management
Managing a diet for duodenal ulcers focuses on several key principles:
- Avoiding irritants: Certain foods and drinks can irritate the duodenal lining or increase stomach acid production.
- Eating a balanced diet: A balanced diet ensures the body gets the appropriate nutrients it needs to repair tissue and maintain overall health.
- Small, frequent meals: Consuming smaller meals more frequently can help reduce the burden on the digestive system.
Here is a breakdown of dietary recommendations for duodenal ulcers:
Health Support: This Vitamin K2 + D3 Complex is essential for bone density, cardiovascular health, and immune function. It’s a highly-rated formula for those looking to maintain optimal nutrient levels. You can find it on Amazon.
Foods to Include
A diet that supports duodenal healing includes:
- High-Fiber Foods: Vegetables, fruits, whole grains, and legumes can have a protective effect on the stomach lining.
- Lean Proteins: Eggs, lean meats, tofu, and fish provide essential amino acids without excessive fats.
- Healthy Fats: Avocados, olive oil, and nuts contain monounsaturated fats which are easier on the stomach.
- Low-Acidic Foods: Non-citrus fruits and vegetables can be less irritating.
- Probiotic-Rich Foods: Yogurt and fermented foods may help with gut health, particularly in addressing H. pylori infections.
Foods to Avoid or Limit
Dietary irritants that may exacerbate symptoms should be avoided:
- Acidic Foods: Tomatoes, citrus fruits, and vinegar can increase stomach acid.
- Spicy Foods: Chili and pepper can irritate the ulcer site.
- Fried and Fatty Foods: These take longer to digest and can increase acid production.
- Lactose: Some people may be lactose intolerant, which can cause bloating and pain.
- Caffeine: Coffee, tea, and some soft drinks can stimulate acid production.
- Alcohol: This irritates the stomach lining and increases acid production. Stop it completely
Sample Diet Plan
Here is a simple one-day meal plan to help those with duodenal ulcers:
Breakfast
Health Support: This high-absorption Magnesium Glycinate (200 mg) is gentle on the stomach and supports muscle relaxation, better sleep, and metabolic health. You can find this trusted formula on Amazon.
- Oatmeal with sliced bananas and a drizzle of honey
- A glass of water or non-citrus juice
Snack
- A small apple with a handful of almonds
Lunch
- Grilled chicken salad with a variety of vegetables
- Whole-wheat bread
- A cup of herbal tea or water
Snack
- Carrot sticks with hummus
Dinner
- Baked salmon with a side of quinoa and steamed broccoli
- A small portion of avocado
- Water or ginger tea (if tolerated)
Snack
- A bowl of plain yogurt or a probiotic-supplement
- A few pieces of melon or other low-acidic fruit
Make sure to drink plenty of water throughout the day, as hydration is essential for health and healing.
Lifestyle Modifications
In addition to dietary management, certain lifestyle adjustments improve outcomes for those with duodenal ulcers:
- Avoid NSAIDs: If possible, switch to alternative pain relievers that are less harsh on the stomach.
- Stop Smoking: Smoking increases stomach acidity and impairs healing of the duodenal lining.
Conclusion
Managing a diet for duodenal ulcers involves avoiding foods that can irritate the digestive system and opting for nutrient-dense, high-fiber, and lean protein-rich options. Alongside medical treatment, dietary adjustments and lifestyle changes play a crucial role in healing and managing symptoms associated with duodenal ulcers. It’s important to work with a healthcare professional to tailor a plan to the individual’s needs and ensure optimal recovery and health.