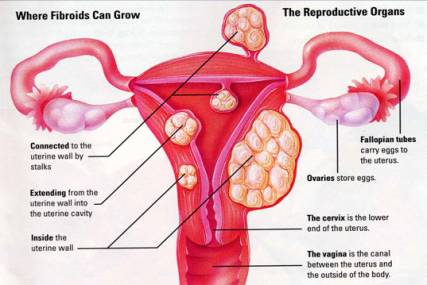
During the childbearing years, non-cancerous growths called uterine fibroids, also referred to as leiomyomas or myomas, appear in the uterus. Although the exact cause is yet to be determined, research has identified numerous factors that may play a role in their formation.
Causes of Fibroid Tumors in the Uterus
The paragraph below provides a carefully selected compilation of possible reasons and factors that may contribute to the formation of fibroid tumors:
- Genetic Changes:
- Research indicates that numerous fibroids have variations in genes that are different from the ones found in regular uterine muscle cells. These genetic modifications could potentially play a role in the development and expansion of fibroids.
- Hormonal Influence:
- Estrogen and progesterone, which are two hormones responsible for the growth of the lining of the uterus during the menstrual cycle, can potentially enhance the growth of fibroids. Fibroids have a higher amount of receptors for estrogen and progesterone compared to regular uterine muscle cells.
- Fibroids have a tendency to reduce in size postmenopause as a result of a decline in hormone production.
- Growth Factors:
- Substances such as insulin-like growth factor, which play a role in maintaining tissue health, might have an influence on the progression of fibroids.
- Extracellular Matrix (ECM):
- The ECM, or extracellular matrix, is a substance that promotes cell adhesion. In comparison to healthy uterine tissue, fibroids contain a higher amount of ECM, potentially causing them to become fibrous and impacting their growth.
- Family History:
- Individuals who have a relative with fibroids have a greater likelihood of developing this condition. If a woman’s mother has fibroids, her chances of having them are about three times higher than the average risk.
- Ethnic Origin:
- Women of African-American descent have a higher likelihood of developing fibroids compared to women belonging to other racial groups. Additionally, they also tend to experience fibroids at a younger age and have a greater number or size of fibroids.
- Obesity:
- Being overweight or obese increases the risk of fibroids. The risk is even higher for women who are severely obese.
- Dietary Factors:
- A diet that consists of a lot of red meat and lacks green vegetables, fruit, and dairy products has been connected to a higher likelihood of developing fibroids. There have been studies indicating a possible connection between a deficiency in vitamin D and an increased risk of fibroids as well.
- Early Menarche:
- Early onset of menstruation may increase the likelihood of developing fibroids.
- Lifestyle Factors:
- Some research indicates that alcohol consumption and hypertension may be associated with an increased risk of fibroid development.
Fibroid Tumors in the Uterus Symptoms
Although certain women may not have any symptoms from uterine fibroids, others may face various signs that can impact their overall well-being. Below is a compilation of the most prevalent indicators related to fibroid growth in the uterus:
- Heavy Menstrual Bleeding:
Menorrhagia, which is excessive menstrual bleeding, is a prominent indicator of fibroids. This can involve periods lasting more than a week and the necessity to frequently change sanitary protection, possibly resulting in anemia. - Menstrual Pain:
Intense cramping or throbbing pain during menstruation, referred to as dysmenorrhea, may be experienced by women with fibroids. The pain can also radiate to the lower back and thighs. - Pelvic Discomfort:
A feeling of fullness or pressure in the lower abdomen is common, which can sometimes be mistaken for weight gain or bloat. - Pelvic Pain:
Fibroids can cause a dull or sharp pain in the pelvis that may be constant or intermittent. It’s usually correlated with the size and location of the fibroids. - Frequent Urination:
Larger fibroids that press on the bladder can cause an increase in the frequency of urination and the urge to urinate, sometimes with little output. - Difficulty Emptying the Bladder:
The pressure exerted by fibroids on the bladder can sometimes result in difficulty emptying it completely, which may lead to a urinary tract infection. - Constipation:
The presence of fibroids pushing on the rectum can cause difficulties with bowel movements, resulting in constipation and unpleasant sensations. - Backache or Leg Pains:
The existence of fibroids may result in pain that spreads to the lower back and even the legs, typically caused by the size and force exerted by the fibroid tumors. - Pain During Intercourse:
Referred to as dyspareunia, certain women with fibroids may feel discomfort during sexual intercourse, and the severity of this symptom depends on the size and location of the fibroid. - Complications During Pregnancy and Labor:
Although fibroids themselves do not directly cause symptoms, they can result in complications while being pregnant such as a higher chance of needing a C-section, delivering the baby prematurely, or having a breech birth. - Reproductive Issues:
In some cases, fibroids can lead to fertility problems or interfere with the ability to carry a pregnancy to term.
Duration and Severity Pattern:
| Symptom | Duration | Severity Pattern |
|---|---|---|
| Heavy Menstrual Bleeding | Typically each period | Can worsen over time |
| Menstrual Pain | During each period | May intensify |
| Pelvic Discomfort | Can be constant | May increase with growth |
| Pelvic Pain | Varies | May escalate |
| Frequent Urination | Persistent | Can worsen with size increase |
| Difficulty Emptying Bladder | Persistent or recurrent | Can worsen over time |
| Constipation | Intermittent | May worsen |
| Backache or Leg Pains | As fibroids grow | Can increase |
| Pain During Intercourse | During intercourse | Varies |
| Reproductive Issues | During attempts at conception or pregnancy | Depends on fibroid position and size |
How fibroid tumors in the uterus are detected
Although most fibroids do not cause symptoms, some women may experience heavy menstrual bleeding, pelvic pain, and reproductive issues. Detecting fibroids early is important for effective management and treatment. We will explore different methods used to detect fibroid tumors in the uterus.
Health Support: This Vitamin K2 + D3 Complex is essential for bone density, cardiovascular health, and immune function. It’s a highly-rated formula for those looking to maintain optimal nutrient levels. You can find it on Amazon.
1. Pelvic Exam: During a pelvic exam, a healthcare provider manually examines the uterus, ovaries, and surrounding areas for any abnormalities. While this method cannot definitively diagnose fibroids, it can indicate the need for further testing.
2. Ultrasound: Transabdominal or transvaginal ultrasound is widely used to detect and diagnose fibroids. These imaging techniques use sound waves to create detailed images of the uterus, allowing healthcare professionals to identify the size, location, and number of fibroids.
3. Magnetic Resonance Imaging (MRI): MRI uses powerful magnets and radio waves to produce detailed images of the uterus. This technique is especially beneficial in determining the dimensions and position of fibroids, even those located deep within the walls of the uterus.
4. Hysteroscopy: In order to examine the uterine cavity and detect any abnormalities such as fibroids, healthcare providers use a hysteroscope – a slender, illuminated tube that is inserted through the cervix into the uterus. This procedure provides direct visualization of the uterus’s interior.
Health Support: This high-absorption Magnesium Glycinate (200 mg) is gentle on the stomach and supports muscle relaxation, better sleep, and metabolic health. You can find this trusted formula on Amazon.
5. Endometrial Biopsy: In this procedure, a small sample of the uterine lining is extracted and analyzed. While an endometrial biopsy is primarily used to diagnose other conditions such as endometrial cancer, it can also help identify fibroids if located near the uterine lining.
6. Blood Tests: Blood tests are not specifically used to diagnose fibroids, but they can help determine any underlying conditions that may cause similar symptoms, such as hormonal imbalances or thyroid issues. These tests can help rule out other potential causes of symptoms.
7. Computed Tomography (CT) Scan: CT scans combine X-ray images taken from different angles to create cross-sectional images of the body. While not as commonly used as ultrasound or MRI, CT scans can provide additional information about the size, location, and spread of fibroids.
8. Saline Infusion Sonography (SIS): This procedure involves injecting sterile saline solution into the uterus while performing an ultrasound exam. The saline helps provide a clearer picture of the uterus and any abnormalities, including fibroids.
9. Laparoscopy: Laparoscopy is a minimally invasive surgical technique used both for diagnosis and treatment. This process entails creating tiny cuts in the belly and inserting a laparoscope to inspect the uterus and nearby structures. Utilizing this technique enables the direct observation of fibroids, aiding in the identification of their size and position.
Effective Treatment Options for Fibroid Tumors in the Uterus
Fibroid tumors, or uterine fibroids, are benign masses that form in the uterus. These growths can vary in size, amount, and where they are located, and they can result in various symptoms such as excessive menstrual bleeding, discomfort in the pelvic area, and fertility issues. If you have received a diagnosis of fibroids, consider these five successful treatment choices to discover the most suitable option for your situation.
- Watchful Waiting:
In cases where women have small fibroids that do not cause major symptoms, doctors might suggest a wait-and-see approach. This entails frequent check-ups to keep an eye on the size and development of the fibroids and observe any changes in symptoms. If the fibroids stay small and the symptoms are manageable, no additional treatment may be necessary. However, if the symptoms worsen or the fibroids grow bigger, alternative treatment options can be explored. - Medications:
Medications, such as hormonal therapy, can help manage the symptoms of fibroids. Commonly prescribed hormonal options include:- Gonadotropin-releasing hormone (GnRH) agonists: These medications cause a temporary menopause-like state by reducing estrogen production. They can shrink fibroids and alleviate symptoms, but they are only a short-term solution due to their side effects and limited usage duration.
- Progestin-releasing intrauterine device (IUD): This small device, inserted into the uterus, releases progestin to reduce heavy bleeding and pain associated with fibroids. While it doesn’t directly shrink fibroids, it can provide relief for some women.
- Tranexamic acid: This oral medication helps control heavy bleeding by promoting blood clotting. It is particularly useful for managing excessive menstrual bleeding caused by fibroids.
- Minimally Invasive Procedures:
If medication on its own is not enough, there are a variety of less invasive procedures that can be used. These choices specifically focus on treating fibroids, while also minimizing the potential risks and shortening the time needed for recovery when compared to traditional surgery. Some notable procedures include:- Uterine artery embolization (UAE): In this process, tiny particles are inserted into the arteries that provide blood to the fibroids, obstructing their blood supply. This absence of blood leads to a reduction in the size of the fibroids. UAE is carried out with the use of local anesthesia and necessitates a shorter period of hospitalization.
- Magnetic resonance imaging-guided focused ultrasound surgery (MRgFUS) is a non-surgical procedure that utilizes targeted ultrasound waves to heat and eliminate fibroid tissue. This treatment does not involve any cuts or anesthesia, although its suitability varies depending on the type and location of fibroids.
- Surgical Options:
If fibroids are causing severe symptoms or if fertility is a concern, different surgical options can be taken into consideration. These include:- Myomectomy: This process entails taking out the fibroids while keeping the uterus intact. It can be done by making a cut in the abdomen or by using less invasive methods like laparoscopic or robotic techniques. Myomectomy is a viable treatment choice for women who plan on having children in the future.
- Hysterectomy: A hysterectomy is a surgical procedure to entirely remove the uterus. It is considered a permanent solution to treat fibroids, as it eradicates any chance of them coming back. Nevertheless, this alternative is suggested only for women who have no intention of becoming pregnant anymore.
- Emerging Treatments:
New therapies for fibroids are continually being researched as the medical industry progresses. These include:- High-intensity focused ultrasound (HIFU): Like MRgFUS, this method utilizes ultrasound waves for the purpose of targeting and eliminating fibroids. However, it is important to note that in certain areas, it is still categorized as experimental and may not be easily accessible to all individuals.
- Radiofrequency ablation: This method utilizes radiofrequency energy’s generated heat to eliminate fibroids. It can be done as an outpatient procedure and allows for a quicker recovery period when compared to conventional surgery.
Essential Prevention Steps to Avoid Fibroid Tumors in the Uterus
By incorporating these precautionary measures into your everyday routine, you have the ability to manage your uterine well-being and potentially steer clear of the challenges linked to fibroids:
- Maintain a Healthy Weight:
Obesity has been associated with a higher likelihood of developing fibroids. By maintaining a healthy weight, you can decrease your risk of developing these growths. Key elements in achieving a healthy weight include engaging in regular physical activity and eating a balanced diet. - Consume a Nutrient-Rich Diet:
Eating a variety of fruits, vegetables, whole grains, and lean proteins can support good health and reduce the chances of developing fibroids. To ensure you’re getting important vitamins, minerals, and antioxidants, include colorful fruits and vegetables such as berries, leafy greens, and cruciferous vegetables in your daily meals. - Quit Alcohol Consumption:
Alcohol intake has been associated with an increased risk of fibroids. To promote uterine health, it’s important to quit an alcohol consumption. - Quit Smoking:
Smoking has detrimental effects on your overall health, and it has also been linked to an increased risk of developing fibroids. Quitting smoking not only reduces your risk of fibroids but also offers numerous other health benefits. - Avoid Hormonal Birth Control Methods:
Long-term use of certain hormonal birth control methods, such as progestin-only contraceptives, can increase the risk of fibroids. Consult with your healthcare provider to explore alternative birth control options that pose a lower risk. - Monitor Hormone Levels:
Imbalances in hormone levels, particularly estrogen dominance, have been associated with fibroid growth. Regularly monitoring your hormone levels and addressing any imbalances promptly can help in avoiding fibroids. - Manage Stress:
Chronic stress may play a role in the development of fibroids. Prioritize stress management techniques, such as exercise, meditation, deep breathing exercises, or engaging in hobbies, to reduce the impact of stress on your body.
Conclusion
Although the development of fibroid tumors in the uterus cannot be entirely prevented, implementing these proactive steps can significantly reduce the risk. By maintaining a healthy lifestyle, including regular exercise, a balanced diet, and stress management, you can take control of your uterine health and potentially avoid the complications associated with fibroids.
Remember, it’s essential to consult with your healthcare provider for personalized advice and guidance regarding fibroid prevention and overall reproductive health.