Men frequently experience incontinence following prostate surgery, which is characterized by the inability to control their bladder and unintentionally leaking urine. This situation can be distressing and humiliating, significantly affecting an individual’s overall well-being.
The causes of incontinence after prostate surgery
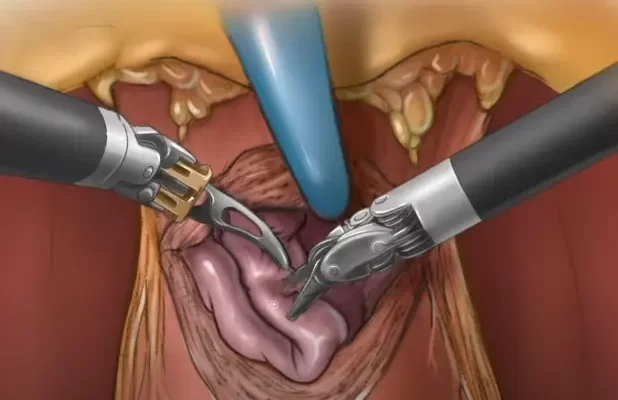
While the procedure can be life-saving and improve quality of life, it can also have some side effects. One of the most common side effects is incontinence, which refers to the loss of bladder control. Incontinence after prostate surgery can be distressing for many men, but understanding the possible causes can help manage and treat this condition effectively. Here are six common causes of incontinence after prostate surgery:
- Damage to the sphincter muscles: During prostate surgery, the delicate sphincter muscles that control urine flow may sustain damage or get weakened. This damage affects their ability to fully close the urethra, leading to bladder leakage.
- Nerve damage: The prostate is in close proximity to important nerves responsible for bladder control. Surgery may accidentally damage these nerves, resulting in temporary or permanent incontinence. This side effect can be minimized if the surgeon takes extra care to preserve these nerves during the procedure.
- Inflammation and swelling: After surgery, the area around the prostate may become inflamed and swollen. This can put pressure on the bladder and affect its normal functioning, leading to temporary incontinence. In most cases, this type of incontinence resolves on its own as the inflammation subsides.
- Overactive bladder: The surgical trauma and changes in the urinary system can sometimes lead to an overactive bladder. This condition makes the bladder contract involuntarily, causing sudden urges to urinate and resulting in episodes of incontinence. Medications and bladder training exercises can often help manage overactive bladder symptoms.
- Post-surgical scarring: Surgery can cause scarring in and around the prostate area, which may affect the proper functioning of the bladder and urethra. Scar tissue can interfere with the closure of the sphincter muscles, leading to urine leakage. Physical therapy and certain surgical interventions can help alleviate this problem.
- Psychological factors: Incontinence after surgery can have a significant psychological impact. Feelings of embarrassment, anxiety, and stress can worsen the condition or even cause it to develop in individuals who did not experience it immediately after surgery.
Managing incontinence after prostate surgery
After prostate surgery, managing incontinence becomes a crucial focus for patients. It involves implementing strategies to regain bladder control and minimize leakage.
While managing incontinence may seem daunting at first, with the right strategies and support, it is possible to maintain an active and fulfilling lifestyle. Here are five essential tips to help you navigate and overcome incontinence after prostate surgery:
- Stay Positive and Seek Support:
Dealing with incontinence can be emotionally distressing, but it’s crucial to stay positive and remember that this is a temporary phase. Seek support from family, friends, or a support group where you can share your experiences, concerns, and triumphs with others going through similar situations. A positive mindset and a strong support network can do wonders in managing day-to-day challenges. - Practice Kegel Exercises:
Kegel exercises are specifically designed to strengthen the pelvic floor muscles and can be highly effective in improving bladder control after prostate surgery. These exercises involve contracting and relaxing the muscles responsible for controlling urine flow. Regularly practicing Kegel exercises can help regain bladder control and reduce instances of leakage. - Adopt a Healthy Lifestyle:
Maintaining a healthy lifestyle plays a crucial role in managing incontinence after prostate surgery. Some dietary modifications, such as avoiding bladder irritants like caffeine, alcohol, and spicy foods, may help reduce bladder urgency and frequency. Additionally, staying hydrated is important, as concentrated urine can irritate the bladder and worsen incontinence symptoms. Aim for a balanced diet rich in fruits, vegetables, and fiber to prevent constipation, as straining to pass stools can put pressure on the pelvic floor. - Use Incontinence Products:
Incontinence products, such as pads or absorbent briefs, provide an extra layer of protection and help manage any unexpected leaks that may occur. Various types of incontinence products are available, ranging from light liners to heavier absorbent pads, allowing you to find the right fit for your needs. It’s essential to experiment with different products to find the most comfortable and effective option for your lifestyle and activity level. - Seek Professional Guidance:
Don’t hesitate to seek professional help from a healthcare provider or a continence specialist who can offer personalized advice and support. In English, the paragraph above can be paraphrased as:Professionals are able to evaluate your unique circumstances, recommend suitable treatment choices, and offer useful tools to assist you in dealing with and conquering incontinence. Depending on the seriousness and root causes of your incontinence, there might be medical interventions accessible, including medications, biofeedback, or surgical remedies.
Rehabilitation for incontinence
Rehabilitation exercises, such as pelvic floor muscle exercises (commonly known as Kegel exercises), are crucial for regaining bladder control after prostate surgery. These exercises involve contracting and relaxing the muscles that support the bladder and control urination.
By strengthening these muscles, individuals can improve their ability to hold urine and reduce leakage. It is advised to perform these exercises regularly and correctly under the guidance of a healthcare professional.
They may also recommend other specific exercises targeting the abdominal and hip muscles to further support bladder control. Consistent practice of rehabilitation exercises can greatly enhance continence recovery post-surgery.
Stories of how men cope with incontinence after prostate surgery
Patient Story 1: John’s Journey
John was a 62-year-old man who underwent a prostate surgery to treat his prostate cancer. While the surgery successfully removed the cancer, it also left him with a new challenge to face – incontinence. At first, John felt frustrated and embarrassed by this unexpected consequence. He found it difficult to cope with the constant worry of leakage and the need to wear protective pads.
However, with the support of his family and medical team, John began to take positive steps towards managing his incontinence. He started doing pelvic floor exercises recommended by his physiotherapist. These exercises helped strengthen his pelvic muscles, gradually improving his bladder control. John also discovered the benefits of using absorbent pads specifically designed for incontinence, which gave him a sense of security and freedom.
Through continuous practice and perseverance, John slowly regained control over his bladder. He discovered that by monitoring his fluid intake and planning bathroom breaks strategically, he could better manage his incontinence. Over time, John’s confidence grew, and he was able to resume his favorite activities, such as playing golf and socializing with friends, without constant worry about leakage.
Patient Story 2: Michael’s Determination
Michael, a 58-year-old man, had always been an active individual. However, after his prostate surgery, he was faced with the challenge of incontinence. Initially, Michael struggled to accept this new reality and felt his quality of life diminishing. However, he was determined not to let incontinence define him.
Michael decided to take a proactive approach to manage his incontinence. He researched different techniques and treatments, such as counseling and biofeedback therapy. This therapy helped him become more aware of his body and refine his pelvic muscle control. With consistent practice and support from his spouse, Michael gradually regained control over his bladder.
In addition to therapy, Michael discovered the benefits of using external devices, like a male urine collection device, which provided him with increased confidence and convenience. This device allowed him to go about his daily routine without having to worry about leaks or constant trips to the bathroom.
Patient Story 3: David’s Support System
David, a 70-year-old retiree, underwent prostate surgery as part of his treatment for prostate enlargement. Like many men in his position, he struggled with incontinence after the surgery. However, David had a strong support system in his wife, who stood by his side throughout the entire journey.
Initially, David found it difficult to adjust to his incontinence. Embarrassment and a sense of isolation began to creep in, affecting his mental well-being. It was his wife’s unwavering support that motivated him to seek help and explore different management options.
David attended support group meetings where he could openly share his challenges and experiences with others who had also undergone prostate surgery. The support and advice he received from fellow group members provided him with immense comfort and guidance. David also found solace in talking to a mental health professional, who helped him cope with the emotional aspects of living with incontinence.
With time, patience, and the support of his wife and the community, David was able to find effective strategies to manage his incontinence. He learned to plan his outings carefully, wear absorbent briefs for added security, and practice relaxation techniques to reduce anxiety. By focusing on the positive aspects of his life and surrounding himself with understanding individuals, David regained his sense of dignity and continued to enjoy his retirement years.
Patient Story 4: Robert’s Adaptive Approach
Robert, a 55-year-old businessman, faced the challenge of incontinence after his prostate surgery. He was determined not to let it hinder his professional and personal life. With his hectic schedule and frequent travel, Robert knew he had to find adaptive solutions to manage his incontinence effectively.
Robert worked closely with his urologist to explore different treatment options. Together, they decided that using an artificial urinary sphincter implant would be the most suitable solution for his lifestyle. This implant provided Robert with better control over his bladder and allowed him to resume his daily activities without interruptions.
In addition to the implant, Robert made alterations to his routine to accommodate his needs. He started carrying a discreet bag with extra supplies, such as absorbent pads, a spare set of clothing, and cleansing wipes, to ensure he was always prepared. He also made sure to plan his meetings and travel arrangements strategically, taking into account his need for frequent bathroom breaks.
Through his adaptive approach and willingness to make necessary adjustments, Robert successfully managed his incontinence while maintaining a fulfilling professional and personal life.