Pregnant women are susceptible to the same illnesses as other people at different times in their lives. They also suffer from colds, seasonal and perennial allergies, and viral illnesses. The statistics are disappointing: almost no one manages to avoid the common cold during pregnancy.
Carrying a child requires a tremendous effort from the body – as a result, it becomes more susceptible to any disease. Colds, viral diseases, seasonal or perennial rhinitis can take a more severe form and require intensive treatment.
| Trimester | Incidence of Rhinitis |
|---|---|
| First | 20-30% |
| Second | 30-40% |
| Third | 40-50% |
According to recent research, rhinitis is a common affliction during pregnancy, affecting an estimated 20-30% of women during the first trimester. This incidence increases to 30-40% during the second trimester and up to 50% during the third trimester.
IYTMed.com
Characteristics of rhinitis in pregnant women
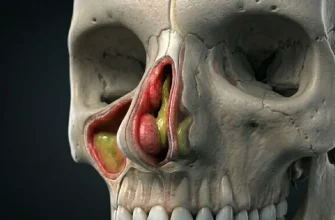
In addition to the general causes of runny nose, there are changes that occur in the body during pregnancy. First of all, there is a decrease in immunity, a change in hormonal balance and toxicosis, which causes edema of the mucous membranes. We can distinguish several types of rhinitis that can occur in pregnant women: allergic, infectious, vasomotor, hormonal.
Health Support: This Vitamin K2 + D3 Complex is essential for bone density, cardiovascular health, and immune function. It’s a highly-rated formula for those looking to maintain optimal nutrient levels. You can find it on Amazon.
Allergic
In pregnant women, the symptoms of allergic rhinitis are the same as in other people:
- Sneezing;
- Itching in the nasal cavity;
- swelling, nasal congestion;
- tearing and nasal discharge.
During pregnancy, specific skin allergy tests for diagnosis are contraindicated. Therefore, the diagnosis is made on the basis of complaints and allergic history. Determination of the level of specific antibodies to allergens in serum may be used.
Infectious
During pregnancy, there are significant changes in the maternal immune system, making pregnant women extremely susceptible to acute respiratory and bacterial infections. The mucosa reacts to the appearance of viruses in the nasal cavity – there is edema, more actively produced mucus, which leads to a violation of nasal breathing.
A distinguishing feature of acute infectious rhinitis is the connection with hypothermia or contact with a sick person, as well as the variability of symptoms during the disease: first dryness, burning in the nasal cavity, sneezing, then congestion and abundant clear nasal discharge for 3-5 days. After that, the nasal discharge may become thick and change color from yellow to greenish. The illness passes within 7-14 days.
Health Support: This high-absorption Magnesium Glycinate (200 mg) is gentle on the stomach and supports muscle relaxation, better sleep, and metabolic health. You can find this trusted formula on Amazon.
In pregnant women, rhinorrhea associated with acute respiratory viral infections often has a prolonged course, responds poorly to conventional therapeutic measures, and may be complicated by purulent rhinosinusitis.
Chronic rhinitis
This disease is caused by a violation of the tone of the vessels of the nasal cavity. Predisposing factors are heredity, anatomical features of the structure of the nasopharynx, as well as hormonal changes, the presence of gastroesophageal reflux, which is often observed in pregnancy.
Chronic vasomotor rhinitis is characterized by both local and general symptoms. Under the influence of various provoking factors (exhaust fumes, nicotine inhalation, temperature changes, consumption of spicy food), as well as against the background of stress, there is a constant or periodic nasal congestion and mucous discharge, an unpleasant feeling of mucus flowing down the nasopharynx. The congestion occurs on one side or the other and increases in the supine position.
General symptoms include manifestations of vegetovascular dystonia: sweating, low body temperature, decreased blood pressure, drowsiness, and others. There are two types of vasomotor rhinitis: medicamentous and hormonal. Medicated runny nose is associated with prolonged use of vasoconstrictive drops and habituation to them.
What is hormonal rhinitis of pregnancy? This is a special form of vasomotor rhinitis that occurs only during pregnancy. Although it affects 20-30% of all women, the mechanism of the disease is not fully understood. Among the many changes in the body at this time – increased blood flow in the tissues.
The main cause is believed to be the increased level of female sex hormones during this period. Estrogens cause blood vessels to dilate, and progesterone causes fluid retention. The nasal mucosa is particularly affected. Its swelling causes breathing difficulties and nasal congestion.
How can you tell the difference between rhinitis in pregnancy and an infectious runny nose? Pregnancy rhinitis usually begins at the end of the first trimester, when the level of female sex hormones increases significantly. It is characterized by nasal congestion and discharge of clear mucus, frequent sneezing.
Despite the unpleasant symptoms, hormonal rhinorrhea tends to go away on its own when a woman has a baby. However, it is very important not to confuse it with “real” illnesses. If snot, congestion, and sneezing are accompanied by fever, sore throat, or a dry or wet cough, you may have a cold or an acute respiratory infection.
How to treat the common rhinitis during pregnancy
To prevent complications and the development of chronic forms of rhinitis in pregnancy, you need to be especially attentive to the first signs and at their appearance urgently consult a doctor – he will diagnose and prescribe treatment.
It is often difficult for the doctor to decide how to treat rhinitis in pregnant women: the choice of drugs for expectant mothers is limited. It is necessary to exclude those that may cause harm to the mother or child in the short or long term. If possible, the use of any medication in pregnant women in the early stages should be avoided. Therefore, non-drug therapies come to the fore.
Here are some tips to help fight or reduce a runny nose during pregnancy.
- Sleep in a semi-recumbent position with your upper body at about a 40-degree angle.
- Rinse the nasal passages with a homemade saline solution or its pharmacy equivalent.
- Drink more fluids.
- Use nasal heat if you do not have a fever or sinus infection.
If prescribed by a doctor, you may use medications. Nasal lavage is used to treat acute infectious rhinitis in pregnant women. If the situation is complicated by inflammation of the paranasal sinuses – sinusitis, then the doctor can prescribe an antibiotic. Therapy should be carried out with drugs in the lowest possible doses and a short course.
When prescribing the drug, the doctor takes into account:
- The woman’s general health;
- Possible interactions with other medications;
- Avoidance of habituation, development of vasomotor or drug-induced rhinitis;
- safety for placental development and fetal health.
The treatment of allergic rhinitis in pregnancy is particularly difficult. When treating this type of rhinitis in pregnant women, the main role is played by eliminatory measures – measures aimed at removing the allergen from the space where the future mother lives and from the surface of the mucosa.
To maximize the elimination of provoking factors is necessary to control dust (ventilation of the room, wet cleaning, getting rid of carpets, heavy curtains, down pillows), separation from the animal to which there is an allergy, the elimination of contact with pollen, for example, during the flowering season to travel to regions where there are no plants that cause allergies. The use of air purifiers and humidifiers will be useful.
Nasal rinsing with isotonic saline solutions based on ocean or sea water is of great importance. This will help reduce the severity of allergic irritation. If symptoms persist, topical glucocorticosteroids and vasoconstrictors may be used as prescribed by a physician. Low-dose, short-term use of these agents does not harm the developing fetus.
The first thing to do when a pregnant woman has a hormonal rhinorrhoea should be to avoid smoking, spicy foods and other provocative factors. Heartburn can also provoke vasomotor rhinitis, which often develops during pregnancy. Some drugs for its elimination are approved for pregnant women.
Besides, there is a safe, simple and yet effective way to treat hormonal rhinitis during pregnancy – nasal rinsing with saltwater solutions. The procedure should be done 2-4 times a day and more frequently. In severe cases, topical glucocorticosteroids are prescribed. It is absolutely necessary to consult a doctor when choosing medication.