Itching, also known as pruritus, can be more than just a minor irritation. For some people, itching all over the body becomes a persistent issue that affects daily life. Whether it’s a symptom of an underlying medical condition or the result of environmental factors, understanding what causes this widespread itching is essential to addressing it effectively. In this article, we’ll dive into the causes, contributing factors, and potential treatments for all-over body itching, supported by data and real medical insights.
Common Causes of Generalized Itching
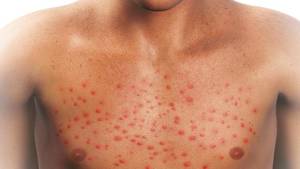
Itching can arise from a variety of sources, and identifying the cause is key to treatment. Here are some common reasons for generalized itching:
- Dry Skin (Xerosis): The most common cause of generalized itching, particularly among older adults. Dry skin is often worsened by cold weather or excessive air conditioning.
- Allergic Reactions: Allergic dermatitis can be triggered by various substances, including soaps, fragrances, and even certain fabrics.
- Systemic Conditions: Conditions such as chronic kidney disease, liver disease, and hyperthyroidism often present itching as a symptom. Research suggests that around 30% of patients with chronic kidney disease experience pruritus.
- Medications: Certain medications can induce itching as a side effect, including opioids, diuretics, and some blood pressure drugs.
- Psychogenic Itching: Stress and anxiety are also common contributors to all-over itching. Studies show that stress can exacerbate existing skin conditions or induce new sensations of itching.
Prevalence and Data
Persistent itching affects a significant proportion of the population. According to a recent study, approximately 8-10% of adults experience chronic generalized itching at some point in their lives. The prevalence increases with age, with around 20% of people over 70 reporting frequent itching episodes.
| Age Group | Percentage of Population Affected |
|---|---|
| Under 30 | 5% |
| 30-50 | 8% |
| 50-70 | 12% |
| Over 70 | 20% |
Medical Example: Itching Due to Systemic Disease
Consider the case of a 65-year-old man experiencing persistent itching for several months. After various topical treatments failed, he was referred to a specialist. Blood tests revealed impaired liver function, which was causing bile salts to accumulate in the bloodstream and contribute to the itching. This case highlights how systemic diseases can often present with skin symptoms, making it critical to address any persistent itching with a healthcare professional.
Health Support: This Vitamin K2 + D3 Complex is essential for bone density, cardiovascular health, and immune function. It’s a highly-rated formula for those looking to maintain optimal nutrient levels. You can find it on Amazon.
Over-the-Counter Treatments and Costs
For those dealing with generalized itching, over-the-counter treatments can be an effective first step:
- Moisturizers: Hydrating lotions, particularly those containing ceramides, can help relieve dryness-related itching. Prices typically range from $10 to $25 per bottle.
- Antihistamines: Oral antihistamines such as loratadine and cetirizine can help reduce itching related to allergies, costing around $15 to $30 per package.
- Topical Corticosteroids: Mild corticosteroid creams can provide relief for inflammation-induced itching. These are generally available for $8 to $20, depending on the brand and potency.
When to See a Doctor
While over-the-counter treatments work for many, persistent itching without an identifiable cause should be addressed by a healthcare professional. It can sometimes indicate an underlying systemic condition, such as:
- Chronic Kidney Disease: Approximately 30% of patients with advanced kidney disease experience pruritus. The itching is often worse at night and can lead to significant discomfort and sleep disruption.
- Liver Disease: Liver dysfunction can cause bile acids to build up, leading to intense itching. This type of pruritus is often resistant to typical anti-itch treatments.
- Thyroid Disorders: Both hyperthyroidism and hypothyroidism can present with itching. An imbalance in thyroid hormones can affect skin health, leading to dryness or rashes.
Modern Trends: Natural Remedies and Lifestyle Changes
There has been a rising interest in natural remedies and lifestyle adjustments for managing itching. Essential oils such as lavender or chamomile are often used topically or in diffusers to help reduce stress-related itching. However, caution is advised, as essential oils can also be allergens for some individuals.
Another trend is colloidal oatmeal baths, which can soothe irritated skin and provide temporary relief for those experiencing widespread itching. A box of colloidal oatmeal costs between $6 and $12 and is an easy, cost-effective way to help manage symptoms.
Health Support: This high-absorption Magnesium Glycinate (200 mg) is gentle on the stomach and supports muscle relaxation, better sleep, and metabolic health. You can find this trusted formula on Amazon.
Advice from Our Editorial Team
If you are experiencing persistent itching all over your body, don’t ignore it. Start with simple remedies—keep your skin moisturized, avoid potential allergens, and consider lifestyle factors like stress management. If the itching persists or significantly affects your quality of life, seek medical advice. A healthcare professional can help identify any underlying conditions and tailor an effective treatment plan. Itching may seem like a small issue, but it can signal important aspects of your overall health, so listening to your body is crucial.