Leprosy, also referred to as Hansen’s disease (HD), is a long-term infection by the germs Mycobacterium leprae or Mycobacterium lepromatosis. Initially, infections lack symptoms and generally remain by doing this for 5 to 20 years. Symptoms that develop include granulomas of the nerves, respiratory tract, skin, and eyes. This might lead to a lack of ability to feel pain, therefore loss of parts of extremities due to repeated injuries or infection due to unnoticed wounds. Weakness and poor eyesight may also be present.
Understanding Leprosy
Leprosy is spread in between people. This is thought to take place through a cough or contact with fluid from the nose of an infected individual. Leprosy takes place more typically amongst those residing in hardship. Contrary to popular belief, it is not highly contagious. The two primary types of disease are based on the number of bacteria present: paucibacillary and multibacillary. The two types are differentiated by the number of poorly colored, numb skin patches present, with paucibacillary having five or less and multibacillary having more than 5. The diagnosis is validated by discovering acid-fast bacilli in a biopsy of the skin or by finding the DNA using polymerase domino effect.
Leprosy is curable with a treatment called multidrug therapy. Treatment for paucibacillary leprosy is with the medications dapsone and rifampicin for six months. Treatment for multibacillary leprosy consists of rifampicin, dapsone, and clofazimine for 12 months. A variety of other antibiotics might also be used. These treatments are provided totally free of charge by the World Health Organization. Worldwide in 2012, the number of chronic cases of leprosy was 189,000, down from some 5.2 million in the 1980s. The number of new cases was 230,000. A lot of new cases occur in 16 countries, with India accounting for over half. In the past 20 years, 16 million people worldwide have been treated of leprosy. About 200 cases are reported per year in the United States.
Health Support: This Vitamin K2 + D3 Complex is essential for bone density, cardiovascular health, and immune function. It’s a highly-rated formula for those looking to maintain optimal nutrient levels. You can find it on Amazon.
Leprosy has affected humankind for countless years. The disease takes its name from the Greek word lepra, while the term “Hansen’s disease” is called after the doctor Gerhard Armauer Hansen. Separating people by putting them in leper nests still happens in places such as India, China, and Africa. Nevertheless, many nests have closed, given that leprosy is not extremely contagious. Social preconception has been related to leprosy for much of history, which continues to be a barrier to self-reporting and early treatment. Some consider the word “leper” offensive, preferring the expression “person impacted with leprosy”. It is categorized as an overlooked tropical disease. World Leprosy Day was started in 1954 to draw awareness to those affected by leprosy.
Symptoms
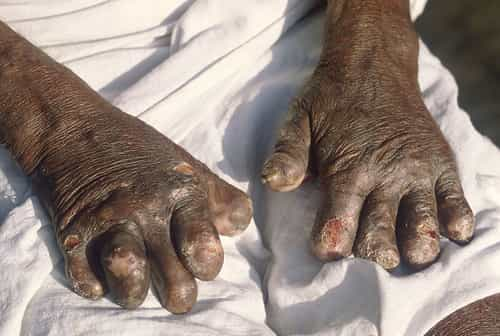
Leprosy is primarily a granulomatous disease of the peripheral nerves and mucosa of the upper respiratory tract; skin sores (light or dark patches) are the main external sign. If without treatment, leprosy can advance and cause long-term damage to the skin, nerves, limbs, and eyes. [18] [19] Secondary infections, in turn, can result in tissue loss, triggering fingers and toes to become reduced and deformed, as cartilage is taken in into the body.
Causes
M. leprae and M. lepromatosis
M. leprae and M. lepromatosis are the causative agents of leprosy. M. lepromatosis is a reasonably newly recognized mycobacterium isolated from a fatal case of scattered lepromatous leprosy in 2008. An intracellular, acid-fast bacterium, M. leprae is aerobic and rod-shaped, and is surrounded by the waxy cell membrane coating quality of the Mycobacterium genus. Due to substantial loss of genes needed for independent growth, M. leprae and M. lepromatosis are obligate intracellular pathogens, and unculturable in the lab, a factor that causes trouble in definitively recognizing the organism under a rigorous interpretation of Koch’s postulates. Making use of nonculture-based strategies such as molecular genes has actually enabled alternative establishment of causation.
While the causative organisms need to date been impossible to culture in vitro, it has actually been possible to grow them in animals such as mice and armadillos. Naturally occurring infection likewise has actually been reported in nonhuman primates, including the African chimpanzee, sooty mangabey, and cynomolgus macaque, in addition to in armadillos and red squirrels. Red squirrels (Sciurus vulgaris) – a threatened species – in England were found to have leprosy in November 2016. Nevertheless, no squirrel cases have actually spread to a human for hundreds of years.
Health Support: This high-absorption Magnesium Glycinate (200 mg) is gentle on the stomach and supports muscle relaxation, better sleep, and metabolic health. You can find this trusted formula on Amazon.
Risk Factors
The greatest risk aspect for establishing leprosy is contact with another case of leprosy. Contacts of people with leprosy are 5 to eight times more likely to develop leprosy than members of the general population. Leprosy likewise occurs more commonly amongst those residing in poverty. Other risk factors are badly understood. Nevertheless, conditions that lower immune function, such as poor nutrition, other illnesses, or host genetic differences, may increase the risk of establishing leprosy. Regardless of this, infection with HIV does not appear to increase the risk of developing leprosy.
Transmission
Transmission of leprosy takes place during close contact with those who are infected. Transmission is proposed to be by nasal beads, however many concerns stay about its mode of transmission and public health. Leprosy is unknowned to be either sexually transferred or highly transmittable. People are usually no longer transmittable after the first month of basic multidrug therapy. Leprosy might likewise be sent to human beings by armadillos.
Two exit paths of M. leprae from the human body frequently explained are the skin and the nasal mucosa, although their relative value is unclear. Lepromatous cases show large numbers of organisms deep in the dermis, however whether they reach the skin surface area in adequate numbers is doubtful. The skin and the upper breathing tract are most likely entry path. While older research study dealt with the skin path, recent research study has progressively preferred the respiratory path. Speculative transmission of leprosy through aerosols containing M. leprae in immunosuppressed mice was accomplished, suggesting a comparable possibility in humans.
Diagnosis
Inning accordance with the World Health Organization, medical diagnosis in areas where people are frequently infected is based upon one of these main signs:
- Skin lesion consistent with leprosy and with guaranteed sensory loss
- Favorable skin smears
Skin lesions can be single or multiple, and normally hypopigmented, although periodically reddish or copper-colored. The lesions may be macules (flat), papules (raised), or nodular. The sensory loss at the skin lesion is important due to the fact that this feature can help differentiate it from other causes of skin sores such as tinea versicolor. Thickened nerves are connected with leprosy and can be accompanied by loss of sensation or muscle weakness. Nevertheless, without the particular skin sore and sensory loss, muscle weakness is ruled out a trusted sign of leprosy. In some cases, acid-fast leprosy bacilli in skin smears are thought about diagnostic; nevertheless, the diagnosis is clinical. Diagnosis in areas where the disease is unusual, such as the United States, is frequently postponed because doctor are unaware of leprosy and its symptoms. Early diagnosis and treatment prevent nerve involvement, the trademark of leprosy, and the disability it causes.
Many type of leprosy are known, however some symptoms prevail to them, including runny nose, dry scalp, eye problems, skin sores, muscle weakness, reddish skin, smooth, glossy, diffuse thickening of facial skin, ear, and hand, loss of sensation in fingers and toes, thickening of peripheral nerves, and flat nose due to damage of nasal cartilage. Also, phonation and resonation of sound take place during speech. Often, atrophy of the testes with resulting impotence takes place.
Leprosy Prevention
Early detection of the disease is essential, since physical and neurological damage might be irreparable even if cured. Medications can reduce the risk of those coping with people with leprosy from acquiring the disease and likely those with whom people with leprosy come into contact outside the home. However, concerns are known of resistance, cost, and disclosure of a person’s infection status when doing follow-up of contacts. Therefore, the WHO suggests that people who reside in the same home be taken a look at for leprosy and be dealt with just if symptoms are present.
The Bacillus Calmette-Guérin (BCG) vaccine provides a variable quantity of protection versus leprosy in addition to its target of tuberculosis. [48] It seems 26 to 41% effective (based upon regulated trials) and about 60% efficient based upon observational research studies with two doses possibly working much better than one.Development of a more effective vaccine is ongoing.
Treatment for Leprosy
A variety of leprostatic agents are offered for treatment. For paucibacillary (PB or tuberculoid) cases, treatment with day-to-day dapsone and regular monthly rifampicin for 6 months is recommended. While for multibacillary (MB or lepromatous) cases, treatment with day-to-day dapsone and clofazimine in addition to regular monthly rifampicin for 12 months is recommended. Multidrug therapy (MDT) stays highly effective, and people are not contagious after the first month-to-month dose. It is safe and easy to use under field conditions due to its discussion in calendar blister packs. Regression rates stay low, and no resistance to the combined drugs is seen.