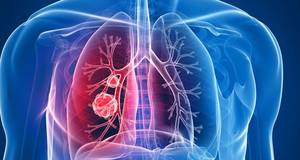
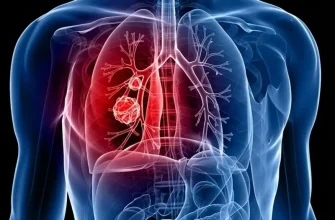
Lung cancer treatment of non-small and small cell types. You and your doctor select a cancer treatment plan based upon a number of elements, such as your general health, the type and stage of your cancer, and your choices.
Non-Small Cell Lung Cancer Treatment
Surgery, radiation, chemotherapy, targeted treatments and immunotherapy– alone or in mix– are utilized to treat lung cancer. Each of these types of treatments might cause different side effects.
Surgery
The majority of stage I and stage II non-small cell lung cancers are treated with surgery to remove the growth. For this procedure, a surgeon gets rid of the lobe, or section, of the lung containing the growth.
Health Support: This Vitamin K2 + D3 Complex is essential for bone density, cardiovascular health, and immune function. It’s a highly-rated formula for those looking to maintain optimal nutrient levels. You can find it on Amazon.
Some cosmetic surgeons use video-assisted thoracoscopic surgery (VATS). For this procedure, the surgeon makes a small cut, or cut, in the chest and inserts a tube called a thoracoscope. The thoracoscope has a light and a tiny electronic camera linked to a video screen so that the cosmetic surgeon can see inside the chest. A lung lobe can then be gotten rid of through the scope, without making a huge incision in the chest.
Chemotherapy and Radiation
For people with non-small cell lung growths that can be surgically eliminated, evidence suggests that chemotherapy after surgery, known as “adjuvant chemotherapy,” might help avoid the cancer from returning. This is especially true for patients with stage II and IIIA disease. Concerns continue to be about whether adjuvant chemotherapy applies to other patients and how much they benefit.
For individuals with stage III lung cancer that can not be removed surgically, physicians generally suggest chemotherapy in mix with conclusive (high-dose) radiation treatments. In stage IV lung cancer, chemotherapy is usually the main treatment. In stage IV patients, radiation is used only for palliation of symptoms.
The chemotherapy treatment plan for lung cancer frequently includes a combination of drugs. Among the drugs most commonly used are cisplatin (Platinol) or carboplatin (Paraplatin) plus docetaxel (Taxotere), gemcitabine (Gemzar), paclitaxel (Taxol and others), vinorelbine (Navelbine and others), or pemetrexed (Alimta).
Health Support: This high-absorption Magnesium Glycinate (200 mg) is gentle on the stomach and supports muscle relaxation, better sleep, and metabolic health. You can find this trusted formula on Amazon.
There are times when these treatments might not work. Or, after these drugs work for a while, the lung cancer might return. In such cases, doctors typically prescribe a 2nd course of drug treatment referred to as second-line chemotherapy.
Recently, the principle of maintenance chemotherapy has been tested in scientific trials, either as a switch to another drug before the cancer advances; or to continue one of the substance abuse at first for a longer amount of time. Both of these strategies have revealed benefits in chosen patients.
Chemotherapy Before Other Treatments (Neoadjuvant Treatment)
Getting chemotherapy prior to radiation or surgery may assist individuals with lung cancer by shrinking the growth enough making it easier to remove with surgery, increasing the effectiveness of radiation and damaging concealed cancer cells at the earliest possible time.
If a growth does not shrink with chemotherapy, the medication can be stopped immediately, permitting the doctor to attempt a various treatment. In addition, research reveals that people with lung cancer are much more able to handle the side effects of chemotherapy when it is given before surgery.
Often, a brief trial period of treatment with the drug shrinks the tumor prior to surgery. If that is the case, then continued treatment with the exact same drug after surgery is most likely to benefit the patient. Due to the fact that many lung cancer specialists all over the world are providing chemotherapy to their patients prior to surgery, patients ought to discuss it with their doctor.
Targeted Treatments
One of the most interesting advancements in lung cancer medication is the intro of targeted treatments. Unlike chemotherapy drugs, which can not tell the distinction between regular cells and cancer cells, targeted treatments are developed specifically to attack cancer cells by attaching to or obstructing targets that appear on the surface areas of those cells. Individuals who have actually advanced lung cancer with particular molecular biomarkers might receive treatment with a targeted drug alone or in combination with chemotherapy. These treatments for lung cancer include:.
Erlotinib (Tarceva and others). A targeted treatment called erlotinib has been shown to benefit some people with non-small cell lung cancer. This drug obstructs a particular kind of receptor on the cell surface area– the epidermal growth factor receptor (EGFR). Receptors such as EGFR function as doorways by permitting substances because they can motivate a cancer cell to grow and spread. Lung cancer cells that have an anomaly on the EGFR are likely to respond to treatment with erlotinib rather of chemotherapy. For patients who have gotten chemotherapy, and are in need of additional treatment, erlotinib can be used even without the presence of the mutation.
Afatinib (Gilotrif). In 2013, the FDA approved afatinib for the initial treatment of metastatic NSCLC in patients with the exact same EGRF gene anomalies or removals as those who can be dealt with successfully with erlotinib.
Gefitinib (Iressa). In 2015, the FDA authorized gefitinib for the first-line treatment of patients with NSCLC whose tumors harbor certain types of EGFR gene mutations, as discovered by an FDA-approved test.
Bevacizumab (Avastin). Similar to normal tissues, growths need a blood supply to endure. Blood vessels grow in numerous ways. One way is through the existence of a compound called vascular endothelial development aspect (VEGF). This drug stimulates capillary to penetrate growths and supply oxygen, minerals, and other nutrients to feed the tumor. When growths spread throughout the body, they launch VEGF to produce new members vessels.
Bevacizumab works by stopping VEGF from promoting the development of new blood vessels. (Because regular tissues have an established blood supply, they are not impacted by the drug.) When integrated with chemotherapy, bevacizumab has actually been shown to improve survival in people with certain kinds of non-small lung cancer, such as adenocarcinoma and big cell carcinoma.
Crizotinib (Xalkori). A treatment that has revealed benefits for people with sophisticated non– small cell lung cancer who have the ALK gene mutation. Crizotinib works by obstructing ALK and stopping the growth of the tumor.
Ceritinib (Zykadia). This was authorized in 2014 for individuals with metastatic ALK-positive lung cancer who can not tolerate crizotinib or whose cancer remained to grow while being treated with crizotinib.
Since the genes of cancer cells can evolve, some growths might become resistant to a targeted treatment. Medications to date those challenges are being studied now in medical trials, which often provide important treatment options for individuals with lung cancer.
Immunotherapy
Immunotherapy has actually recently become a new treatment choice for specific lung cancers. While any cancer treatment can cause side effects, immunotherapy is typically well-tolerated; this remains in part due to its mechanism of action.
Our immune system is constantly working to keep us healthy. It acknowledges and combats against risk, such as infections, viruses, and growing cancer cells. In general terms, immunotherapy utilizes our own immune system as a treatment versus cancer.
In March 2015, the FDA authorized the immunotherapy nivolumab (Opdivo) for the treatment of metastatic squamous NSCLC which was unsuccessfully treated with chemotherapy. Nivolumab works by interfering with a molecular “brake” called PD-1 that avoids the body’s body immune system from assaulting growths.
Added methods to immunotherapy for lung cancer have actually revealed guarantee in early clinical trials and are now in late-phase advancement. Treatments for NSCLC have advanced the outermost; however, a variety of brand-new immune-based treatments for SCLC are also in medical development. These treatments fall into four primary categories:
- Monoclonal antibodies are lab-generated particles that target specific tumor antigens (a drug that the body immune system views as being foreign or dangerous).
- Checkpoint inhibitors target particles that act as checks and balances in the policy of immune responses.
- Restorative vaccines target shared or tumor-specific antigens.
- Adoptive T-cell transfer is a method where T-cells (a type of white blood cell) are removed from the patient, genetically modified or treated with chemicals to improve their activity, and re-introduced into the patient with the objective of enhancing the immune system’s anticancer reaction.
Small Cell Lung Cancer Treatment
Chemotherapy and Radiation Therapy
For individuals with small cell lung cancer, no matter stage, chemotherapy is a necessary part of treatment. Radiation treatment might be utilized also depending on the stage of cancer.
For people with limited-stage small cell lung cancer, mix chemotherapy plus radiation therapy given at the exact same time is the recommended treatment. The most commonly utilized preliminary chemotherapy program is etoposide (Toposar or Vepesid) plus cisplatin (Platinol), known as EP.
For individuals with extensive-stage small cell lung cancer, chemotherapy alone utilizing the EP routine is the conventional treatment. Nevertheless, another regimen that might be utilized is carboplatin (Paraplatin) plus irinotecan (Camptosar).
Radiation therapy of the brain may be put before or after chemotherapy for some individuals whose cancer has actually spread to the brain.
Precautionary Radiation Therapy to the Brain
In majority of individuals with small cell lung cancer, the cancer likewise spreads to the brain. For individuals whose lung cancer has actually responded to chemotherapy, doctors may prescribe radiation therapy to the brain to assist prevent the cancer from infecting the brain. This procedure is referred to as prophylactic cranial irradiation (PCI). This can benefit patient with both limited-stage and extensive-stage small cell lung cancers.
Surgery
An extremely small percentage of individuals who have limited-stage small cell lung cancer and no lymph node tumors may take advantage of surgery, after which adjuvant chemotherapy is provided.