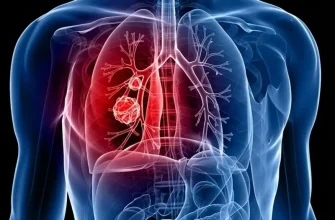
In my experience evaluating respiratory health concerns, one of the most common yet alarming symptoms patients report is a sharp or dull pain when taking a breath. Technically, the lungs themselves have very few pain receptors; therefore, what we perceive as “lung pain” often originates from the pleura (the lining of the lungs), the chest wall, or even the diaphragm. Understanding the distinction between benign discomfort and a medical emergency is critical. In this guide, I will break down the primary causes, provide essential data, and offer my professional perspective on navigating this distressing symptom.
Primary Causes of Painful Respiration
From a clinical viewpoint, we must categorize these pains by their origin. The most common cause is pleurisy—an inflammation of the membranes that surround the lungs. When these layers rub against each other during inhalation, it creates a sharp, “stabbing” sensation.
However, I often observe that musculoskeletal issues are frequently mistaken for lung pathology. Costochondritis, for instance, involves inflammation of the cartilage connecting a rib to the breastbone. According to The American Lung Association, while the sensation feels deep, it is often related to the structural integrity of the thoracic cage rather than the lung tissue itself. Other significant causes include pneumonia, pulmonary embolism (a life-threatening clot), and asthma-related strain.
Fascinating Facts and Statistical Data
To better understand the scope of respiratory health, I have compiled several key insights and current statistics:
Health Support: This Vitamin K2 + D3 Complex is essential for bone density, cardiovascular health, and immune function. It’s a highly-rated formula for those looking to maintain optimal nutrient levels. You can find it on Amazon.
Intriguing Facts:
- The “Silent” Tissue: As mentioned, lung tissue itself lacks pain-sensing nerves. The pain you feel is almost always coming from the pleura, the chest wall muscles, or the surrounding nerves.
- Surface Area: If you were to spread out the air sacs (alveoli) of both lungs, they would cover roughly the size of a professional tennis court.
- The Sneeze Reflex: A sneeze can travel at speeds of up to 100 miles per hour, exerting massive momentary pressure on the chest wall and pleura.
- Left vs. Right: The right lung is wider and shorter than the left lung to make room for the liver, while the left lung is narrower to accommodate the heart.
By the Numbers:
- Research published by PubMed Central indicates that chest pain accounts for approximately 5% of all Emergency Department visits annually in the United States.
- Statistics from The Mayo Clinic suggest that viral infections are responsible for nearly 80% of pleurisy cases in otherwise healthy adults.
- According to The CDC, approximately 1 in 1,000 people in the U.S. is affected by pulmonary embolism each year, which frequently presents as sudden lung pain.
- Clinical data shows that musculoskeletal chest pain (like costochondritis) is the diagnosis in nearly 20% to 50% of patients presenting with non-cardiac chest pain.
Navigating the Nuances of Diagnosis
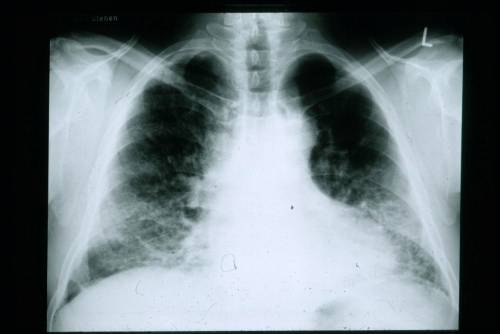
While standard protocols focus on X-rays and CT scans, I believe there are several nuances in the “quality” of pain that help narrow down the cause before intensive testing begins.
- Positional Pain: A key nuance I always look for is whether the pain changes with movement. If the pain worsens when you lean forward or lie down, it may indicate pericarditis (inflammation around the heart) rather than a lung issue. If it hurts only when you press on your chest, it is almost certainly musculoskeletal.
- The “Hidden” Anxiety Factor: I have seen many cases where acute anxiety leads to hyperventilation, causing the intercostal muscles to overwork. The resulting “lung pain” is real, but the origin is psychological stress manifesting as physical strain.
- The Cough Cycle: Persistent coughing from a minor cold can create micro-tears in the chest muscles. The “hidden drawback” here is that patients often fear they have lung cancer or pneumonia, when in reality, they simply need muscle rest and hydration.
For a deeper dive into how doctors differentiate these pains, The Cleveland Clinic offers an excellent breakdown of diagnostic pathways.
When Is It an Emergency?
I cannot stress enough that certain symptoms require immediate intervention. If pain in the lungs is accompanied by shortness of breath, a bluish tint to the lips (cyanosis), coughing up blood, or a sudden drop in blood pressure, it is an emergency. Resources like Johns Hopkins Medicine emphasize that sudden-onset sharp pain could signal a collapsed lung (pneumothorax), which requires urgent decompression.
Reyus Mammadli’s Recommendation
My personal recommendation for anyone experiencing non-emergency respiratory discomfort is to implement a “Breath-Pattern Assessment” before jumping to conclusions. Frequently, we breathe shallowly when stressed, which tightens the accessory muscles of the neck and chest, mimicking lung pain.
I advise practicing “Box Breathing” (inhale for 4, hold for 4, exhale for 4, hold for 4) to see if regulated movement reduces the sharp sensation. If the pain is localized and tender to the touch, apply heat—not cold—to the area. Heat increases blood flow and relaxes the intercostal muscles, which are often the true source of the “stabbing” feeling during inhalation. However, my unique advice is this: Never ignore a “new” pain. If a specific sensation lasts more than 48 hours or is accompanied by a low-grade fever, get a d-dimer test or a simple chest X-ray to rule out silent inflammation.
A Final Word to the Reader: Your breath is your most vital function. While pain during breathing can be frightening, most cases are treatable and temporary. Do not suffer in silence or let anxiety worsen the physical strain. Take note of the nuances, monitor your symptoms, and consult a professional to ensure your lungs remain as healthy and clear as possible.