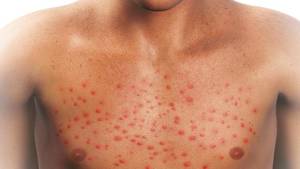
Otitis externa (OE) is an inflammation or infection of the external auditory canal (EAC), the auricle, or both. This condition can be found in all age groups.
Otitis Externa Types
OE may be categorized as follows:
- Intense diffuse OE – Most typical kind of OE, generally seen in swimmers
- Severe localized OE (furunculosis) – Associated with infection of a hair roots
- Persistent OE – Same as intense scattered OE however is of longer duration (> 6 weeks).
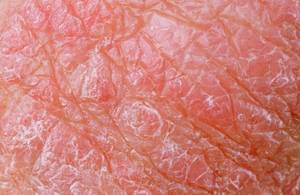
- Eczematous (eczematoid) OE – Encompasses numerous dermatologic conditions (eg, atopic dermatitis, psoriasis, systemic lupus erythematosus, and eczema) that may infect the EAC and cause OE.
- Necrotizing (deadly) OE – Infection that extends into the much deeper tissues surrounding to the EAC; happens mostly in immunocompromised grownups (eg, diabetics, patients with AIDS).
- Otomycosis – Infection of the ear canal from a fungal types (eg, Candida, Aspergillus).
Symptoms of Otitis Externa
The key physical finding of OE is pain upon palpation of the tragus (anterior to ear canal) or application of traction to the pinna (the trademark of OE). Patients may likewise have the following symptoms and signs:
Health Support: This Vitamin K2 + D3 Complex is essential for bone density, cardiovascular health, and immune function. It’s a highly-rated formula for those looking to maintain optimal nutrient levels. You can find it on Amazon.
- Otalgia – Ranges from moderate to severe, usually advancing over 1-2 days.
- Hearing loss.
- Ear fullness or pressure.
- Erythema, edema, and constricting of the EAC.
- Tinnitus.
- Fever (sometimes).
- Itching (specifically in fungal OE or persistent OE).
- Severe deep pain – Immunocompromised patients may have necrotizing (deadly) OE.
- Discharge – Initially, clear; rapidly becomes purulent and foul-smelling.
- Cellulitis of the face or neck or lymphadenopathy of the ipsilateral neck (periodically).
- Bilateral symptoms (uncommon).
- History of exposure to or activities in water (regularly) (eg, swimming, browsing, kayaking).
- History of preceding ear trauma (normally) (eg, strong ear cleaning, usage of cotton swabs, or water in the ear canal).
Diagnosis
The patient’s history and health examination, foring example otoscopy, typically supply adequate info for the clinician to make the diagnosis of OE. Note that a patient who is diabetic or immunocompromised with severe pain in the ear should have necrotizing OE excluded by an otolaryngologist.
Laboratory testing
Usually, lab researches are not searchinged for, but they may be useful if the patient is immunocompromised, if the normal treatment procedures are ineffective, or if a fungal cause is believed. Tests might include the following:
- Gram stain and culture of any discharge from the auditory canal.
- Blood sugar level.
- Urine dipstick.
Imaging research studies
Health Support: This high-absorption Magnesium Glycinate (200 mg) is gentle on the stomach and supports muscle relaxation, better sleep, and metabolic health. You can find this trusted formula on Amazon.
Imaging studies are not needed for most cases of OE. Nevertheless, radiologic examination might be practical if an invasive infection such as necrotizing (malignant) OE is suspected or if the diagnosis of mastoiditis is being thought about.
Imaging techniques may for example the following:
- High-resolution calculated tomography (CT) – Preferred; much better depicts bony disintegration.
- Radionucleotide bone scanning.
- Gallium scanning.
- Magnetic resonance imaging (MRI) – Not used as typically as the other methods; may be considered secondarily or if soft-tissue extension is the primary concern.
Otitis Externa Treatment
Primary treatment of otitis externa (OE) involves management of pain, elimination of debris from the external auditory canal (EAC), administration of topical medications to manage edema and infection, and avoidance of contributing elements.
Most cases can be treated with over-the-counter analgesics and topical eardrops. Commonly utilized eardrops for example acetic acid drops, which alter the pH of the ear canal; anti-bacterial drops, which control bacterial growth; and antifungal prep works. Eczematoid (psoriatic) OE frequently reacts to topical steroid drops however may be persistent or recurrent. The ear might need regular suction debridement under a microscope. If significant canal edema develops, an ear wick may be used to facilitate delivery of topical medications into the medial canal.
In severe cases, oral or intravenous (IV) antibiotic therapy and narcotic analgesics might be required. [18] When it comes to necrotizing (deadly) OE, the patient must be admitted to a health center for IV antibiotic therapy at the discretion of the consulting otorhinolaryngologist. The treatment that is rendered depends on the likely organism, which is best figured out by methods of Gram staining of the affected area.
Many persons with OE are treated empirically. Main treatment involves the following:
- Pain management.
- Elimination of debris from the EAC.
- Administration of topical medications to manage edema and infection.
- Avoidance of contributing aspects.
Pharmacotherapy
- Topical medications (eg, acetic acid in aluminum acetate, hydrocortisone and acetic acid otic solution, alcohol vinegar otic mix).
- Analgesic agents (eg, acetaminophen, acetaminophen and codeine).
- Prescription antibiotics (eg, hydrocortisone/neomycin/polymyxin B, otic ofloxacin, otic ciprofloxacin, otic finafloxacin, gentamicin 0.3 %/ prednisolone 1 % ophthalmic, dexamethasone/tobramycin, otic ciprofloxacin and dexamethasone, otic ciprofloxacin and hydrocortisone suspension).
- Oral prescription antibiotics (eg, ciprofloxacin).
- Antifungal agents (eg, otic clotrimazole 1 % solution, nystatin powder).
Surgery
- Surgical debridement of the ear canal – Usually booked for necrotizing OE or for complications of OE (eg, external canal stenosis); typically required in more severe cases of OE or in cases where a considerable quantity of discharge is present in the ear; essential of treatment for fungal infections.
- Laceration and drain of an abscess.